Image: ShutterStock
An amniocentesis test helps assess fetal health and detects any potential problems in a high-risk pregnancy. In addition, it offers high accuracy of up to 99% compared to the other invasive prenatal tests (1). If you come under the high-risk category, your doctor may suggest this diagnostic test. Keep reading as we bring you the information you need to know about the amniocentesis test in this post.
What Is Amniocentesis?
Image: Shutterstock
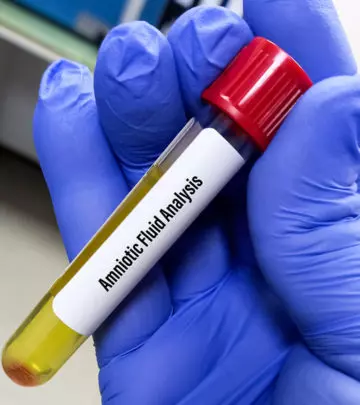
Amniocentesis is a prenatal diagnostic test to check the amniotic fluidiXClear, yellowish liquid surrounding and protecting the developing fetus during pregnancy. that surrounds the fetus in the uterus. This fluid contains cells and substances that indicate the status of the baby’s health.
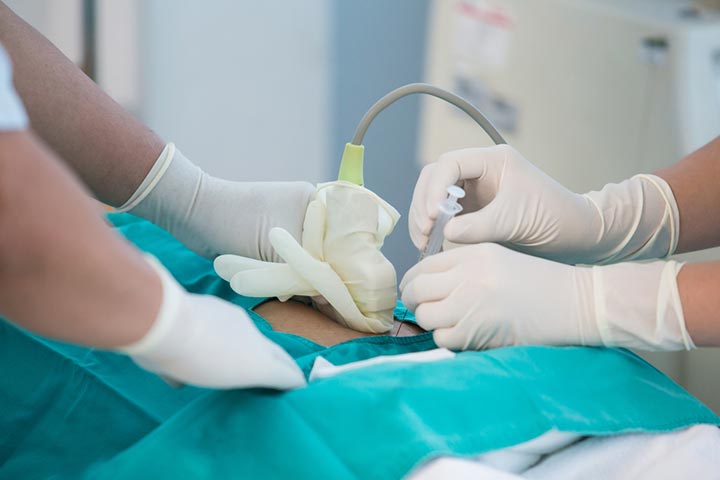
For this test, the gynecologist inserts a long, thin needle (of gauge size 0.9mm) into the uterus to collect a small amount of amniotic fluid. Usually, the procedure is done under ultrasound guidance. The fluid is then tested for specific genetic disorders such as Down syndrome, spina bifidaiXA birth condition characterized by spinal cord defects, identified by its protruded tissue requiring surgery. , and cystic fibrosisiXA genetic disorder affecting the lungs, pancreas, and digestive system by blocking the airways and organ ducts with mucus. (2).
The test results help determine whether or not to continue the pregnancy or deliver early to prevent further complications. This is done at a specific time during pregnancy.
When Is Amniocentesis Done?
Amniocentesis is usually done between the weeks 15 and 20, which is during your second trimester. Some doctors may recommend the test as early as 11 weeks. Amniocentesis done before 14 weeks has higher complication rates (fetal loss, fetal talipesiXA congenital abnormality that causes the feet to turn inward inwards, facing each other. and respiratory morbidity) and it should be avoided before ten weeks. In some cases, an amniocentesis is done even during the third trimester (3).
Amniocentesis has many uses, besides understanding the baby’s health status.
Why Do You Need Amniocentesis?
You may require amniocentesis for the below reasons.
- The results from prenatal screening tests are abnormal
- You had a child with a birth defect or any abnormality
- You are 35 years or above, so to rule out the possibility of your baby having chromosomal abnormalities such as Down syndrome
- You or your partner is a carrier of genetic disorder such as cystic fibrosis
- Your doctor suspects any infection or anemia in the fetus
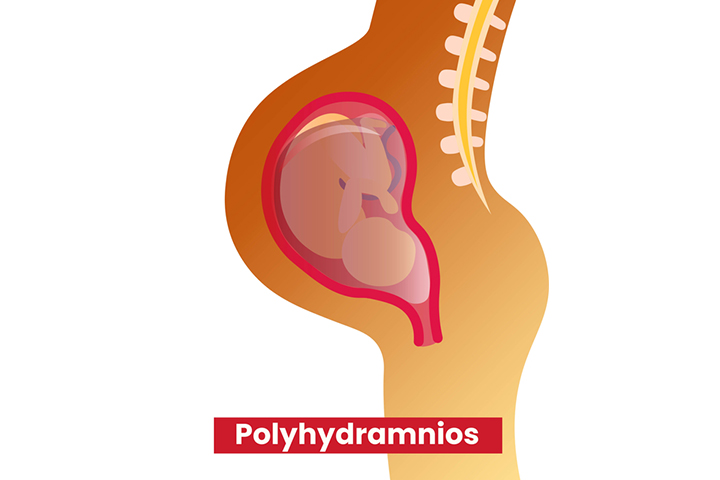
- There is too much amniotic fluid, a condition known as polyhydramnios where amniocentesis is done to relieve pressure effect due to excessive fluid.
Emma Springer reflects on the reasons that led her to undergo amniocentesis during her pregnancy. She recounts, “During my 20-week ultrasound, my doctor identified a couple of markers that prompted her to refer me to a high-risk specialist. The high-risk doctor observed additional concerns on the ultrasound and conducted lab testing, including genetic and carrier screening —tests we had initially opted out of. Concurrently, she recommended consulting a cardiologist. The lab results indicated a significant risk for trisomy 18. Consequently, she scheduled an amniocentesis to definitively confirm or rule out any genetic issues. It is why the amniocentesis was deemed necessary in my case (i).”
Image: Shutterstock
Now, let’s understand the process of amniocentesis.
What Happens During Amniocentesis Procedure?
Image: IStock
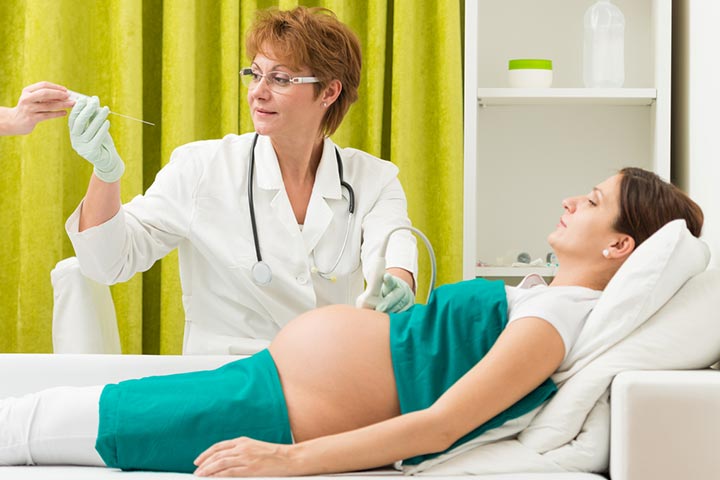
Amniocentesis is an outpatient procedure, meaning you do not have to stay in the hospital.
- Firstly, the doctor performs an ultrasound of your abdomen to check the exact fetal status, liquor volume, placental location, and to map the location where the needle is to be inserted.
- A special gel is applied, and a small device known as an ultrasound transducer is used to get the baby’s image on the monitor (4).
- Post ultrasound, the doctor applies a numbing medication to that belly region.
- The results from ultrasound give an idea of where to insert the needle. He then inserts a hollow needle into the womb through your belly, withdrawing a sample of amniotic fluid.
- The amount withdrawn depends upon the week of pregnancy. You may feel a stinging sensation as the needle enters into the skin and have slight cramps as the needle penetrates into the uterus.
- Your practitioner will continue to use the ultrasound to monitor the baby’s heart rate. You will also experience mild pelvic pain and cramping after amniocentesis.
The pain and cramps should not worry you as you can overcome them with a proper rest schedule as advised by your doctor.
 Quick fact
Quick factHow Long To Rest After The Amniocentesis?
You can go back home and rest for about two hours. You may resume your routine after 72 hours. Your doctor gives you detailed instructions on what to do after an amniocentesis (5).
Amniocentesis recovery speeds up when limiting specific activities, such as:
- lifting above 15 pounds for at least a day
- strenuous work or exercises for 72 hours
- Traveling in air for 72 hours
- Sex for 72 hours
Contact your practitioner if you experience any of the following signs of infection after amniocentesis:
- Fever
- Severe uterine cramps that last for more than a few hours
- Vaginal fluid leakage or bleeding
- Unusual or lack of fetal movement
- Inflammation or redness at the area of insertion (6)
The test results could take a few days to come in. Depending on the results, your doctor would advise you on a few things.
What Do The Amniocentesis Test Results Mean?
Some results would take a few days while some take up to four weeks. Your obstetrician or a genetic counselor will explain the findings.
- Normal amniotic fluid is clear with a light yellow hue. It will not contain any harmful bacteria, and the cells are tested for problems.
- The fetal cells are examined carefully and checked for chromosomal number and arrangement that show genetic disorders. There should be 46 chromosomes in 23 pairs. Any defect in them would lead to genetic abnormalities.
- In the case of genetic amniocentesis, test results will help diagnose or rule out various genetic disorders, neural tube defectsiXCongenital disabilities of the brain, spine, or spinal cord caused when the neural tube doesn’t close completely. , and chromosomal abnormalities. The probability of detecting the problems is high, but it does not measure the severity of the birth defects.
- In the case of fetal lung maturity amniocentesis, normal results assure your baby will survive and is, therefore, ready for birth.
Abnormal results in any of the above cases mean your baby has a chromosomal condition or genetic disorder. However, a few things may affect the results of the test.
What Factors Affect Amniocentesis Test Results?
The amnio results will not be helpful for some reasons, such as:
- Fetal blood in the amniotic fluid will falsely increase the Alpha-fetoprotein (AFP) and Acetylcholinesterase (AChE) substance levels that test for neural tube defects (7).
- Amniotic fluid, when exposed to light, can falsely show lower bilirubiniXA byproduct of old broken down red blood cells, found in the liver, that is excreted from the body. levels.
- Blood or meconiumiXThe first stool of a newborn baby. in the amniotic fluid leads to a false result on the maturity levels of the baby’s lungs.
If none of the factors has influenced the test, and the result has indicated a problem, then you need to decide on the future course of action.
What Happens If Your Baby Is Found To Have A Problem?
Image: Shutterstock
In such cases, you undergo genetic counseling sessions that provide you with more information. Based on the information, some women opt to continue the pregnancy while some decide to terminate it.
Whatever you decide, you will require further support or counseling. Some may find help from support groups while a few require individual counseling.
What Are The Reasons To Take And Not To Take The Amniocentesis Test?
Your reasons for taking up the test or not may vary.
Undergoing the test and confirming the diagnosis will provide you with the following benefits:
- Opt for a medical intervention (if it exists) to correct the abnormality
- Start planning your life to have a child with special needs
- Get ready to make lifestyle changes after the child is born
- Get in touch with support groups and resources to help deal with your unique situation
Some may not prefer to take up the test for the following reasons:
- You are perfectly okay whether or not your baby has a chromosomal defect
- You decide against amniocentesis because of the possible harm it may have on the baby
- Your personal, religious, or moral beliefs prevent you from terminating your pregnancy or seeking medical intervention
If you decide to go ahead with the procedure, you must be aware of the possible complications it could have.
What Are The Complications Associated With Amniocentesis?
It is a tough decision for any woman to opt for amniocentesis. You need to weigh the pros and cons of the procedure before you decide. As you already know the benefits of amniocentesis, let us take a look at the risks involved in the procedure (8).
- Leaking of amniotic fluid: Sometimes, amniocentesis causes amniotic fluid to leak from the vagina. Usually, the loss is minimal and stops in a week’s time, and the leak will not hurt your pregnancy.
- Miscarriage: Based on the available statistics, the risk of miscarriage with amniocentesis in the second trimester is about 0.6%. On the other hand, the likelihood of miscarriage increases if the procedure is performed before 14 weeks of pregnancy. Most miscarriages occur within 72 hours of the procedure, but sometimes, it may occur after two weeks.
- Rh disease: In rare cases, the procedure may cause the fetal blood cells to enter your bloodstream. This causes your body to produce antibodies, which can damage the red blood cells of your baby. To prevent this from occurring, the doctor will give you an injection of Rh immune globulin. This prevents your blood from creating antibodies that may otherwise cross placenta and damage the baby’s red blood cells.
- Needle injury to the baby: During amniocentesis, if the baby moves and gets in the way of the needle, there is the risk of the baby’s arm or leg getting pierced by the needle. However, serious injuries due to needles are quite rare.
- Uterine infection: Although rare, you can contract a uterine infection when bacteria manages to enter the amniotic sac. This will cause high-grade fever, abdominal contractions, and tenderness in your abdomen. Uterine infection requires immediate medical intervention. However, the risk of infection due to amniocentesis is less than one in 1,000.
Image: Shutterstock
- Transmission of infection: Amniocentesis carries a risk of transmitting severe infections to your baby. If you have HIV/AIDS, hepatitis C, or toxoplasmosisiXAn infection caused by the Toxoplasma gondii parasite, typically found in undercooked meat, animal feces, and contaminated soil. , the likelihood of your baby contracting the disease during the procedure increases.
- Clubfoot: Research shows early amniocentesis is linked to higher chances of clubfoot. Also, known as talipes, clubfoot is a congenital deformity of the baby’s foot and ankle. Since there is an increased risk of this congenital defect, most doctors will not perform amniocentesis before 15 weeks of pregnancy (9).
Note that genetic amniocentesis is done only if the test results will have a significant impact on managing the pregnancy. However, the decision is up to you.
 Point to consider
Point to considerAre There Ways To Reduce Amniocentesis Risks?
- Speak to your OB/GYN to recommend a specialist, who has good experience in performing the amniocentesis.
- Don’t hesitate to check on the success rate of the professional who is performing it.
- Make sure the doctor uses a qualified and registered medical sonographer during the procedure. The sonographer provides constant ultrasound guidance, and this increases the likelihood of the doctor drawing a sufficient amount of fluid in the first attempt and that too without harming the fetus.
Below, we have answered a few common questions that you may still have on the procedure.
Frequently Asked Questions
1. What is the difference between amniocentesis and chorionic villus sampling (CVS)?
Both CVS and amniocentesis help find genetic abnormalities before birth. CVS is done earlier than amniocentesis and gives results sooner.
The CVS is accurate in detecting genetic abnormalities but does not recognize neural tube defects, birth defects, and Rh incompatibility, which amniocentesis does.
The CVS can give you results in your first trimester itself whereas amnio cannot give until the second trimester. However, the risks of the CVS are slightly higher than amniocentesis (10).
2. Can amniocentesis detect autism?
Yes, amniocentesis can detect autism. It is based on a finding that high levels of testosterone in the amniotic fluid are linked with autistic traits in children, such as lack of verbal skills and sociability. As amniocentesis detects the testosterone levels and screens autism (11).
3. What is FISH amniocentesis?
FISH (Fluorescence In Situ Hybridisation) is a rapid test that specifically detects some chromosomes such as 21, 18, 13, X, and Y. It is performed on uncultured amniocentesis or CVS samples for quicker results. It holds about 98% accuracy rate in predicting chromosomal disorders and determines the sex of the unborn. This test is performed only under special circumstances upon discussion with your doctor (12).
4. Is amniocentesis procedure painful?
Amniocentesis is not painful, but you may feel uncomfortable while undergoing the procedure (13).
5. Do you need a full bladder for amniocentesis?
Yes. The doctor may sometimes advise you to have a full bladder as it makes the procedure easier (13).
Amniocentesis is not a regular test done for every pregnant woman. Your doctor recommends it if they suspect genetic disorders in the fetus, based on your family history and the regular ultrasound and other tests. Whether or not to get it done needs to be decided after a thorough discussion with your doctor and a careful analysis of its pros and cons.
Infographic: Vital Prenatal Care After Amniocentesis
Your gynecologist may recommend amniocentesis during your prenatal visit between weeks 15 and 20 if you have a high-risk pregnancy. Since this procedure is invasive, your doctor would also recommend certain instructions after amniocentesis, some of which are mentioned in the infographic below.
Illustration: Momjunction Design Team
Key Pointers
- Testing the fetus’s health through amniocentesis occurs between weeks 15 and 20 of pregnancy.
- Amniocentesis can detect genetic disorders such as Down syndrome, spina bifida, and cystic fibrosis.
- Seek medical attention in case of fever, severe uterine cramps, vaginal bleeding, lack of fetal movement, or inflammation of the needle inserted area.
- The test results may be affected by fetal blood, meconium, or exposed amniotic fluids.
- Complications include amniotic fluid leakage, miscarriage, Rh disease, uterine infection, clubfoot, infection transmission, and needle injury to the fetus.
Image: Dalle E/MomJunction Design Team
Learn about amniocentesis, a prenatal test to detect genetic disorders. Understand its process, risks, and benefits. Discover the signs, symptoms, and conditions prompting this diagnostic procedure and available treatments.
Personal Experience: Source
MomJunction articles include first-hand experiences to provide you with better insights through real-life narratives. Here are the sources of personal accounts referenced in this article.
i. My amniocentesis experience.https://youtu.be/PreTgkGiQmQ
References
- Errol R Norwitz; Noninvasive Prenatal Testing: The Future Is Now.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3893900/ - Amniocentesis.
https://www.urmc.rochester.edu/encyclopedia/content.aspx?contenttypeid=92&contentid=p07762 - B R Elejalde et al; Prospective study of amniocentesis performed between weeks 9 and 16 of gestation: its feasibility risks complications and use in early genetic prenatal diagnosis.
https://pubmed.ncbi.nlm.nih.gov/2309757/ - Amniocentesis.
https://medlineplus.gov/ency/article/003921.htm - Amniocentesis.
https://www.hopkinsmedicine.org/health/treatment-tests-and-therapies/amniocentesis - Amniocentesis.
https://myhealth.ucsd.edu/Library/TestsProcedures/Gynecology/92P07762 - Diagnosis of Birth Defects.
https://www.cdc.gov/ncbddd/birthdefects/diagnosis.html - Munawar Hayat et al; A very unusual complication of amniocentesis.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4498839/ - S Farrell et al; Club foot an adverse outcome of early amniocentesis: disruption or deformation?.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC1734259/ - Zarko Alfirevic et al; Amniocentesis and chorionic villus sampling for prenatal diagnosis.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4171981/ - The Path to Diagnosis: A Case Study of Two Children with Autism.
https://fisherpub.sjf.edu/cgi/viewcontent.cgi?referer=https://www.google.co.in/&httpsredir=1&article=1254&context=education_ETD_masters - Ashish Fauzdar et al; Rapid-prenatal diagnosis through fluorescence in situ hybridization for preventing aneuploidy related birth defects.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3722628/ - Amniocentesis.
https://www.nhs.uk/conditions/amniocentesis/what-happens/