Image: ShutterStock
Neural tube defects such as anencephaly and spina bifida affect approximately one in 1,000 babies (1). Experts claim taking supplements of folic acid in pregnancy is effective in significantly lowering the risk of these congenital anomalies. Therefore, folic acid or folate is recommended for consumption before and after a woman conceives. Read this post as we discuss the importance of folic acid during pregnancy, the amount you need, its sources, and when to avoid taking it.
Key Pointers
- Folic acid promotes the production of red blood cells, prevents neural tube defects, protects the baby’s hearing, and protects expectant mothers.
- Health professionals advise taking 400mcg of folic acid daily before and during pregnancy, in addition to prenatal vitamins.
- In high-risk cases, it is recommended to take folic acid at least three months before conception and throughout pregnancy.
- Folic acid deficiency can lead to pregnancy anemia and increase the risk of birth abnormalities.
- Spinach, asparagus, Brussels sprouts, avocado, mushrooms, nuts, eggs, zucchini, and oranges are some foods that are good sources of folate.
What Is Folic Acid?
Folic acid is a synthetic form of vitamin B9 found in fortified foods and other supplements. It is usually utilized by the body to promote new cell growth and nucleic acid (which is a form of genetic material). It is essential for the healthy growth and development of the baby and helps in carrying out specific functions such as producing red blood cells, protecting the child’s ability to hear and supporting the baby’s organ development (2).
Experts recommend taking 400mcg of folic acid along with prenatal vitamins every day before and during pregnancy (3).

Why Should You Take Folic Acid When Pregnant?
Here is why you need to increase your folic acid intake if you are pregnant or are trying to get pregnant.
1. Prevents neural tube defects
Folic acid helps in the neural and brain development of the fetus. The neural tube of your fetus, which later grows into the brain and spinal cord of your baby, is protected by folic acid to prevent any prenatal defects during the early formation of the central nervous system (2).
According to a study by the Centers for Disease Control and Prevention, the fortification of folic acid at 100–220 µg per 100 g of the product can increase the blood concentration of folate by 1.47 times and reduce the rate of onset of neural tube defects by 78%.
2. Produces red blood cells
Folate enhances the production of red blood cells in your body. This is vital during pregnancy when anemia (iron deficiency) is a common complaint. Folic acid ensures that the red blood cell (RBC) count in your body is normal even when you take iron supplements that could replenish the mineral (4).
3. Protects the baby from several complications
Folic acid lowers the baby’s risk of cleft lip and palateiA congenital condition that causes a gap or opening on the lip or the roof of the mouth due to improper development of the fetus. . It also reduces the risk of premature birth, miscarriage, poor baby growth in your womb and low birth weight problems (2).
4. Protects expectant mom
Adequate intake of folic acid everyday is known to prevent preeclampsiaiA pregnancy disorder characterized by high blood pressure, water retention, and protein content in urine. , heart stroke, heart disease, cancers, and Alzheimer’s diseaseiA progressive form of dementia in which the brain cells shrink gradually and die, leading to gradual memory and personality loss. (5).
5. Other essential functions

Folic acid is required for the production, repair, and functioning of DNA. It is also important for the quick growth of the placenta and developing baby (6).
Given its importance, folic acid needs to be taken even before you get pregnant. It is an important nutrient which is required during DNA synthesis.
When Should You Start Taking Folic Acid?
Your doctor will advise you to start taking folic acid and other necessary maternal nutrition when you plan to conceive. Considering that most birth defects could develop in the first trimester, consuming folate-rich foods even before you conceive can be extremely helpful.
Consult your healthcare provider before picking your prenatal vitamins and make sure that it has the recommended amounts of folate you need.
How Much Folic Acid Do You Need?
The standard breakup of recommended folic acid consumption before, after and during pregnancy is as follows (7):
- Before conceiving: 400mcg
- First trimester of pregnancy: 400mcg
- Second and third trimesters of pregnancy: 600mcg
- Breastfeeding stage: 500mcg

Consult your doctor to understand how much folic acid you should consume, considering your personal, past, and family history. You should also inform them about the supplements you are taking and the vitamin deficiencies if you have any. Your folic acid recommendation when pregnant may differ if you have a family history of neural tube defects. Also, folic acid supplementation (0.2 to 15 mg/d) could help lower homocysteine levels.
 Quick fact
Quick factHow Long Do You Need To Take Folic Acid During Pregnancy?
You can start taking folic acid at least three months before pregnancy and all through the pregnancy in high risk cases to lower the risk of birth defects (7).
What Are The Effects Of Folic Acid Deficiency During Pregnancy?
Deficiency of folic acid will lead to pregnancy anemia with symptoms such as decreased appetite, pale skin, lack of energy, diarrhea, headache, and irritability (8). In the case of a moderate deficiency, you may not experience any symptoms but will lack the necessary amount of folate needed for the baby’s embryonic development.
Folic Acid Food Sources
Folate is found in several foods but is water-soluble and easily destroyed or eliminated when cooked. Therefore, the best way is to cook them just a little bit or eat raw if possible. Steaming or cooking by microwave is also good.
A well-balanced diet chart for pregnant women should contain several folic acid foods from different food groups and also those that provide essential vitamins, minerals, and other nutrients. Here’s a list of folic acid-rich foods you should include in your prenatal diet (9).
Folate per half cup of serving:
- Cooked spinach: 131mcg
- Fortified breakfast cereals: 100mcg
- Black-eyed peas: 101mcg
- Asparagus: 89mcg
- White rice: 90mcg
- Brussel sprouts: 78mcg

- Spaghetti: 83mcg
- Romaine lettuce: 64mcg
- Avocado: 59mcg
- Raw spinach: 58mcg
Some other good sources of folate are cabbage, green beans, mushrooms, sweet corn, zucchini, grapefruit, orange, legumes, juices, nuts, and eggs.
 Point to consider
Point to considerWhen Should You Stop Taking Folic Acid?
You can stop taking folic acid once you reach 12 weeks of pregnancy since the baby’s spine will be well developed by then
. However, you can continue taking folate post the 12th week, as it will not harm you or your baby in any way (10).
Keep reading for answers to more questions about folic acid intake during pregnancy.
Frequently Asked Questions
1. Which folic acid tablets are good to take before or during pregnancy?
Some of the most commonly used folic acid supplements are from the brands such as Nature’s Blend, Now Foods and Nature’s Bounty.
2. How does folic acid help when I am trying to get pregnant?
Folic acid can improve your chances of becoming pregnant, as it boosts fertility and also improves RBC production besides providing other health benefits.
3. Are folic acid and prenatal vitamins the same?
Folic acid is already present in the prenatal vitamin formulas. If there is any need for extra folate, your doctor may prescribe additional folic acid supplements.
4. How much folic acid is required for twin pregnancy?
Women carrying twins need about 1,000mcg of folate per day (11).
5. Can folic acid intake during pregnancy cause diarrhea?
Folic acid deficiency can cause diarrhea. In such a case, make sure to have enough water to avoid dehydration and seek the doctor’s help to control diarrhea.
6. Can folic acid cause multiple pregnancies?
No, folic acid supplementation before pregnancy will not increase the likelihood of multiple pregnancies (12).
7. Is too much folic acid bad for pregnancy?
Yes, too much folic acid can increase your baby’s risk of developing autism, obesity, insulin resistance and cognitive impairment (13).
The deficiency of folic acid in pregnancy may cause pregnancy anemia. Symptoms such as headache, diarrhea, or fatigue may go unnoticed in mild cases, but they may still be harmful to the fetus. Folic acid, or the synthetic form of vitamin B9, is essential during pregnancy as it helps in forming the neural tube and red blood cells. It reduces the risk of several congenital disabilities and prevents preeclampsia in pregnant women. It is indeed beneficial for women to take folic acid for pregnancy. Experts also recommend that women planning a pregnancy may start taking folic acid three months before conceiving. However, one may get it prescribed by a doctor to avoid an overdose.
Infographic: What Are The Benefits Of Taking Folic Acid When Pregnant?
Even before conception, your doctor would advise you to take folic acid supplements and enriched foods, such as spinach, peas, and sprouts. This requirement would increase as you become pregnant. Check out the infographic below to learn the various advantages of folic acid for pregnant women and their babies.
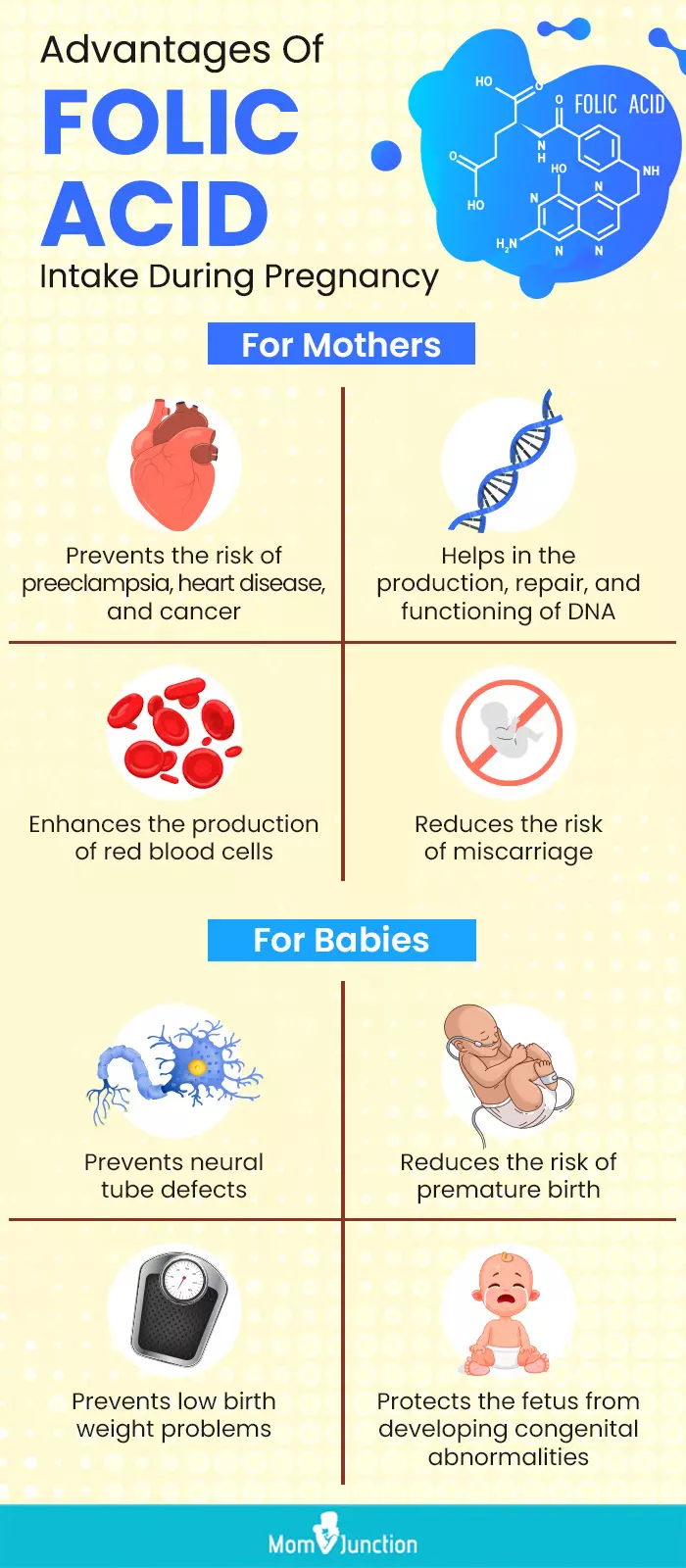
Illustration: Momjunction Design Team
References
- Henk J. Blom et al.; (2006); Neural tube defects and folate: case far from closed.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2970514/ - James A. Greenberg et al,; (2011); Folic acid supplementation and pregnancy: more than just neural tube defect prevention.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3218540/ - About Folic Acid, CDC.
https://www.cdc.gov/folic-acid/about/ - Folic acid, OASH, Office on Women’s health.
https://womenshealth.gov/a-z-topics/folic-acid - Folate, Oregon State University.
https://lpi.oregonstate.edu/book/export/html/71 - Reyna Penailillo et al.; (2015); Folic Acid Supplementation during Pregnancy Induces Sex-Specific Changes in Methylation and Expression of Placental 11β-Hydroxysteroid Dehydrogenase 2 in Rats.
https://pmc.ncbi.nlm.nih.gov/articles/PMC4368185/ - Nutrition during pregnancy, ACOG.
https://www.acog.org/womens-health/faqs/nutrition-during-pregnancy - Folate-Deficiency Anemia, University of Rochester Medical Center.
https://www.urmc.rochester.edu/encyclopedia/content?ContentTypeID=85&ContentID=P00089 - Folate (Folic acid)-Vitamin B9, Harvard.
https://nutritionsource.hsph.harvard.edu/folic-acid/ - Breige McNulty et al.; (2013); Impact of continuing folic acid after the first trimester of pregnancy: findings of a randomized trial of Folic Acid Supplementation in the Second and Third Trimesters.
https://www.sciencedirect.com/science/article/pii/S0002916523051365 - Getting enough folic acid (folate), University of Michigan Health.
https://www.uofmhealth.org/health-library/ue2418 - Tali Levy and Issac Blickstein;(2006); Does the use of folic acid increase the risk of twinning?
https://pubmed.ncbi.nlm.nih.gov/17039857/ - Too much folate in pregnant women increases autism risk, study suggests, John Hopkins University.
https://hub.jhu.edu/2016/05/12/too-much-folate-pregnant-autism/ - Folic acid in pregnancy
https://www.tommys.org/pregnancy-information/im-pregnant/nutrition-in-pregnancy/folic-acid-pregnancy - B vitamins and folic acid
https://www.nhs.uk/conditions/vitamins-and-minerals/vitamin-b/
It’s important to keep taking your folic acid supplements right from the time you get pregnant and even before you’ve conceived. But keep the intake within the recommended portion. Watch this video to find out why!
Community Experiences
Join the conversation and become a part of our nurturing community! Share your stories, experiences, and insights to connect with fellow parents.
Read full bio of Dr. Shashwat Jani
Read full bio of Rebecca Malachi
Read full bio of Swati Patwal
Read full bio of Dr. Joyani Das