Image: iStock
A C-section is a surgical form of delivery, preferred when there are potential risks for a vaginal delivery. It is also known as a cesarean birth or cesarean section. The surgical method is planned during emergencies when a continuous vaginal delivery is arrested or life-threatening complications occur in the mother and fetus. It can also be pre-planned if the potential risks are known in prenatal care.
The World Health Organization (WHO) states that cesarean section is the cause of 21% of all childbirths (one in five). Furthermore, according to WHO, there is a prediction that the number may rise in the next decade. Indeed, according to the National Vital Statistics Reports, the cesarean delivery rate in the US rose to 32.1% in 2026, marking a 1% increase from the previous year’s rate of 31.8% in 2026. But, a cesarean is mostly a last resort of delivery and is not a recommended procedure due to the associated risks and complications(1).
Read on to know more about the types, indications, risks, and complications, along with tips to prepare for a cesarean birth procedure.
Key Pointers
- An abnormal fetal heart rate or multiple gestations could require a C-section delivery.
- Excessive bleeding or iatrogenic damage may lead to complications during the procedure.
- Taking the prescribed medications and following a balanced diet can aid in fast recovery.
- Avoiding solid foods before the procedure, discussing pain management, and other tips to prepare for a c-section as you scroll through.
Types Of C-Section Delivery
C-sections can be of two types based on the skin incision (2).
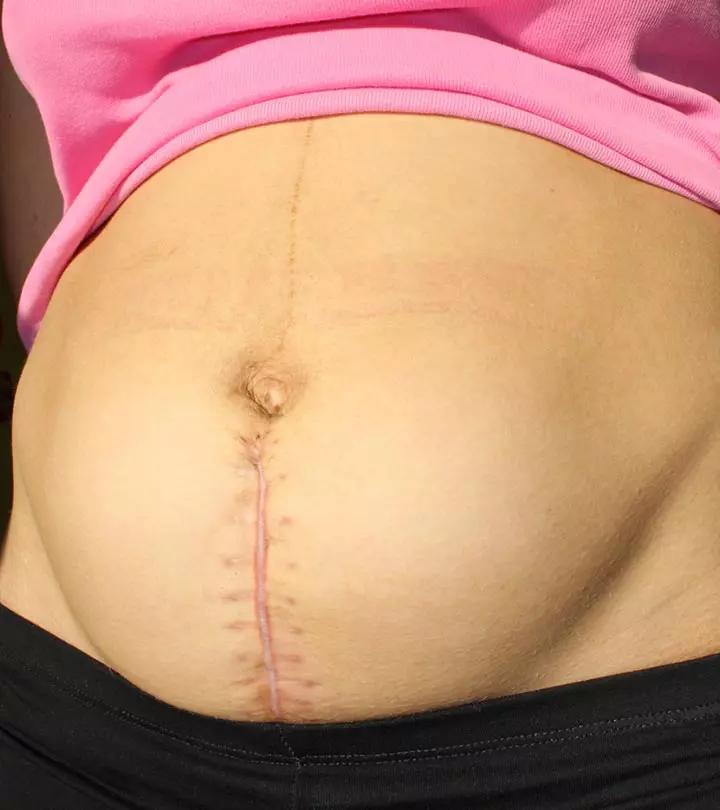
- Horizontal or side-to-side C-section (bikini cut) is when the incision is made across the pubic hairline. This type is more frequently done since it heals well and bleeding is less compared to other types.
- Vertical or up-and-down C-section is where an incision is made from the belly button to the pubic hairline. This is often done in emergencies.
Vertical or horizontal incisions are made based on maternal and fetal health factors; horizontal incisions are cosmetically better.
Indications For C-Section Delivery
C-section delivery is indicated if there is a risk to the mother or the baby during vaginal delivery. Your doctor may discuss the risks and benefits and choose the better method of delivery for you. The following conditions could be the reason for cesarean delivery (2)(3)(4).
- Labor dystocia is a condition when the labor fails to progress. Abnormally slow or protracted labor during the first stage of labor (from contractions until cervical dilation) and the second stage (from complete cervical dilationiThe opening process of the cervix during the initial stage of labor to let the baby slide into the birth canal. until childbirth) are common reasons for emergency C-section deliveries.
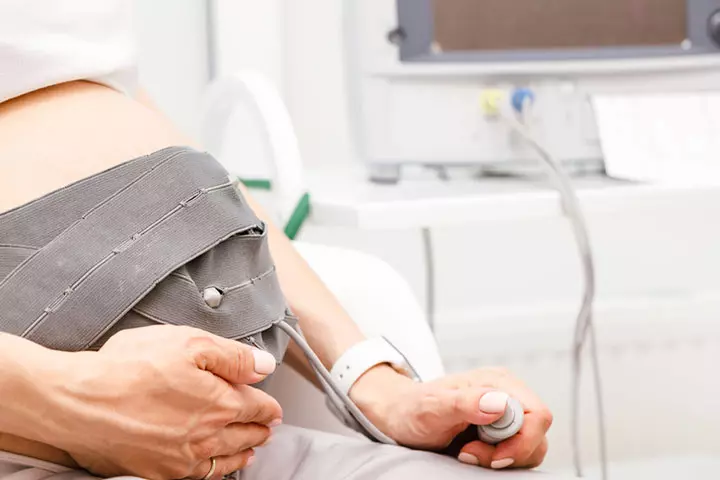
- Indeterminate or abnormal (non-reassuring) fetal heart rate tracing is an indication to do C-section delivery. Fetal heart rate during labor indicates how well the fetus is doing, and the normal rates may vary between 120 to 160 beats per minute. If the heart rate is low, or there is an issue, doctors may try giving IV fluids and oxygen to the mother or change the mother’s position to improve it. Emergency cesarean delivery is indicated if the abnormal fetal heart rate is not improved.
- Fetal macrosomia is a condition in which the baby is too large for gestational age. C-section is suggested in cases of suspected fetal macrosomia since cephalopelvic disproportions (CPD) can cause problems in vaginal delivery. CPD is when there is a size mismatch between the mother’s pelvis and the baby’s head.
- Fetal malpresentation or abnormal position such as breech presentation of the fetus could require cesarean section since vaginal delivery can be difficult in abnormal presentations.
- Multiple gestations with twins or other multiples can indicate C-section delivery since the vaginal delivery for multiple births may need more time, and there is a risk of malpresentation after one delivery.
- Placental conditions that could risk the baby’s or mother’s life and prevent vaginal delivery. Placenta previa is a condition in which the placenta completely or partially blocks the uterus neck. This may interfere with normal vaginal delivery, so a C-section is indicated. Premature detachment of the placenta, such as abruption cases, may also need C-section delivery.
- Previous classical uterine incisions or C-sections can be a contraindication for vaginal delivery since the uterine scars from a previous incision have an increased risk of rupture during uterine contractions.
- Active herpes sores in the cervix or vagina and other maternal conditions such as diabetes, high myopiaiAn eye condition in which a person can see near objects but has difficulty seeing far objects. with risk for retinal retinal detachmentiA condition where the inner layer of the retina gets separated from the back of the eye. , HIV infection, heart problems, high blood pressure, and preeclampsiaiA condition of high blood pressure and protein in the urine during pregnancy. are also indications for cesarean sections based on individual risk and benefits.
- Fetal conditions, such as alloimmune thrombocytopenia, may make it necessary to have a C-section. Alloimmune thrombocytopenia is a condition where there is a maternal-fetal plateletiThe tiny blood cells that prevent and stop bleeding by forming clots. incompatibility, and maternal antibodies destroy fetal platelets, leading to severe internal bleeding in the baby. Although a C-section has a better outcome, it is not mandatory in this condition. It may often be treated during prenatal care.
- Maternal contraindications to vaginal delivery such as inflammatory bowel disease, cervical leiomyomaiMuscle tumor in the uterus near the cervix causing vaginal discharge and bleeding. that could prevent vaginal delivery, large lower-uterine segment, or perineal or rectal fistula could make C-section delivery the appropriate option.
In addition to this, cesarean section deliveries can also be performed if the mother requests. Mothers may choose the most suitable delivery method after counseling with their doctor and understanding the benefits and risks of the procedure.
A 2026 study on the US population observed that the cesarean delivery rate differs for different races. As depicted in the graph below, out of all the live cesarean births, the cesarean delivery rates were highest in black infants (36.0%), followed by Asian/Pacific Islanders (32.7%), Whites (31.0%) and American Indian/Alaska Natives (29.0%).

Total cesarean deliveries in the US population by race
Source: Delivery Method; March Of Dimes/National Center for Health Statistics/final natality dataRisk And Complications Of C-Section Delivery

C-section is usually a safe surgical procedure. However, like any other surgery, this also has a risk of causing certain complications. The likelihood of having C-section risk may vary based on whether it is a planned or emergency procedure and maternal health status. Usually, doctors or midwives may discuss the risk and complications before the procedure.
Common maternal complications and risks of C-section delivery may include the following (5).
- Wound infection, causing pain, redness, swelling, and discharge from the incision wound.
- Excess bleeding, which may require blood transfusion or other surgical procedures to stop bleeding.
 Quick fact
Quick fact- Uterine lining infection (endometritis) causes abdominal pain, heavy vaginal bleeding, fever, and abnormal vaginal discharge.
- Latrogenic damages (damages during a medical procedure) of the bladder, kidneys, or fallopian tube may rarely occur, requiring further surgeries.
- Deep vein thrombosis (DVT) is a blood clot after birth in the leg, causing pain and swelling. It is a rare complication of a C-section. Although it is rare, it is dangerous since the clot can move to the lungs and result in life-threatening pulmonary embolism.
Giving antibiotics before surgery to reduce infections, compression stockings, adequate mobility to prevent clots, and surgery by experienced professionals may reduce a mother’s risks of experiencing complications.
C-sections may pose the following risks to newborns (5).
- Breathing issues, especially if born before 39 weeks of gestation. However, the breathing issues usually improve within a few days in most babies, and they are closely monitored in the hospital during this period.
- Skin cuts may happen accidently while opening the uterus. This is usually minor and heals without complications.
 Things to know
Things to knowRisks To Future Pregnancies
Most women who undergo C-sections may not have problems in future pregnancies. Some women can also safely have a vaginal delivery for their next pregnancy; it is known as vaginal birth after cesarean (VBAC). However, some women may need C-sections for their next delivery too.
Although rare, C-sections may pose the following risks to future pregnancies (5).
- Abnormal attachment of the placenta to the uterus walls, causing trouble delivering the placenta
- Previous C-section scar opening-up
- Stillbirth in rare cases
Risks and complications of C-section to mother, baby, and future pregnancy may vary depending on individual factors. You may talk to your obstetrician and gynecologist to plan future pregnancies accordingly.
Is C-Section Delivery Better Than Vaginal Delivery?

Pregnancy is a physiological process and naturally ends with vaginal delivery. Hormones and other changes prepare a mother’s body for vaginal birth. If there are no risks, opting for vaginal delivery is recommended by most healthcare providers. Cesarean sections are indicated only when there is a risk to the maternal or baby’s health or life during the vaginal delivery.
Dr. Ian Askew, Director of Department of Sexual and Reproductive Health and Research, World Health Organization (WHO), says that “Caesarean sections are critical for saving a life if the vaginal delivery poses risks. Therefore, health systems should ensure timely access for all women when required.“
Cesarean section can also be associated with slower recovery after childbirth, delays skin-to-skin contact and breastfeeding, and causes risk for future pregnancies. “However, not all cesarean sections are done at the moment due to medical reasons. Unnecessary procedures can be harmful to the mother and her baby,” Dr. Askew adds (1).
Vaginal delivery can be painful, but there are also epidural pain management options during the delivery. During a C-section, you may feel pressure such as pull and push during the procedure under spinal anesthesia, but you cannot feel pain. However, the recovery can be long and often requires pain medications while recovering from a C-section. That being said, C-section has its place and is often the safest option in certain scenarios. Rachel Spurrier, a mother, shares her experience of undergoing a C-section after hours of labor. She says, “One of the last clear memories I have of my daughter’s birth is when my Obstetrical Consult made a recommendation: I needed a cesarean section (c-section). Despite my best efforts and six hours of pushing, my baby wasn’t any closer to being born. I consented to the procedure, and all the urgent energy of pushing fell away to the calm of surgery prep. I was wheeled into the OR, and at 10:26 AM, my daughter was born.
“Five months later, as I look back on my c-section, I feel like I was unprepared. In my childbirth classes, c-sections were given a cursory overview. Having gone through one, I don’t regret my c-section…Multiple professionals, including my Doula and Midwife, assured me that the surgery saved both my and my daughter’s lives. I am here today because of modern medicine (i).”
Tips To Prepare For Your C-Section
Preparing for a C-section involves understanding the procedure, discussing anesthesia, and arranging for support. Robyn Horsager-Boehrer, M.D., Chief of Obstetrics and Gynecology at UT Southwestern Medical Center’s William P. Clements Jr. University Hospital, suggests the following tips for pregnant mothers to prepare for their C-section (6).
- Avoid solid food eight hours before the C-section
Restricting food intake before surgery reduces the likelihood of vomiting and aspiration. In earlier days, food and liquids were restricted before the procedure. However, recognizing the need for food or drink while physically and emotionally taxing events such as childbirth, pregnant mothers can drink water, juice, and sports drinks before surgery. Follow your doctor’s instructions since the intake of food beyond the recommended time may delay the procedure.
- Avoid shaving the abdomen or pubic area
Although many women may think shaving the abdomen or pubic area before surgery can be helpful, it is not. Razors can create minor cuts, small abrasions, or scrapes on the skin. This may increase the risk of infection after delivery. If hair removal is needed, nurses will take care of it with clippers on the surgery day.
- Shower using antiseptic soap

You may shower or bathe with special soaps, such as antibiotic soap, in the night or morning before you go for a C-section. You may purchase this soap from drug stores, or some hospitals may provide you during the pre-surgical visits. These soaps help kill the bacteria on your skin and reduce the risk of infection.
- Discuss about the incision closure
Various methods such as staples, glue, and stitches are available to close the skin incision of the C-section. You may discuss with your surgeon to know the best ways for you depending on the body characteristics. You may also ask the doctor about skin closure methods with better cosmetic results.
- Discuss pain management
Various possibilities of pain management after surgery can be discussed while planning the surgery itself. Immediately after surgery, pain medications are given through the epidural catheter (spinal pump) or IV (intravenous) route. When you begin to eat after surgery, doctors may switch to medications by mouth. Discussing the available medications for pain management earlier can keep everyone on the same page.
How Is A Cesarean Delivery Performed?
If there are indications for C-section delivery, doctors conduct pre-surgical and pre-anesthetic evaluations and plan the date for surgery. Sometimes, C-sections are done in emergencies if there are sudden complications, or the vaginal delivery is not progressing as expected.
Doctors may often ask not to consume food or drink a few hours before surgery and take a shower using antiseptic soap. Usually, pregnant mothers are asked to reach the hospital three to four hours before the surgery time. However, this may vary based on the healthcare setting policies and individual factors.
The following steps are included in the preparation and the procedure of a planned (elective) C-section delivery (7) (8).
- Doctors obtain an informed consent signed by you before the procedure after informing you about the procedure, alternatives, risks, and complications. You have the right to ask any concerns and queries to the healthcare provider during this time.
- Change to a hospital scrub and check for your vitals such as heart rate, blood pressure, and baby’s heartbeat.
- IV (intravenous) line is placed on the arm to deliver medicines and fluid as per requirement.
- An antacid injection is given to neutralize stomach acid.
- Pregnant mothers are taken to the operating room approximately half an hour before the operation. ECG leads from the chest and pulse oximeter from the fingers are connected to monitors.
- DVT pump or DVT stockings are put on legs to prevent blood clot formation.
- Spinal (regional/local) anesthesia is given in a sitting or side-lying position, and you may lay down after the anesthesia. General anesthesia is rarely given in specific situations. You may feel tingling or warmness on the legs and soon feel numb below chest level.
- A screen is placed on chest level from you to maintain the operating area’s sterility and avoid seeing the procedure.
- Oxygen mask is placed to increase the oxygen supply to the body.
- Intravenous antibiotics are given to avoid infections.
- A foley catheter (tube) is placed in the urinary tract to drain urine.
- The abdomen and pelvic area will be sterilized with antiseptic, and the incision is made on the skin and then uterus, and the baby is delivered.
- The umbilical cord is clamped, and the placenta is delivered, and the incisions are closed.
While the obstetric surgeon is closing the incision, neonatologists evaluate the APGAR score of the newborn. If the baby is stable, neonatologists place your baby on your chest for skin-to-skin contact and breastfeeding. Otherwise, they shift the baby to NICU for further evaluation and treatment, ensuring adequate neonatal care.
Duration And Recovery Of C-Section Procedure
The C-section procedure may last about 45 minutes. Delivery of the baby can take as little as five to 15 minutes from the time incision is made. However, more time is needed to close the incision on the uterus and abdomen after the baby is delivered. Although C-section delivery is done quickly during emergencies, additional time is still needed to close the incisions (8).
After the procedure, the mother and baby are shifted to the post-operative area for observation. Most women are shifted to their room in two to three hours. Doctors may restrict food or drinks by mouth up to six to 12 hours after a C-section, and you may receive intravenous fluids as needed. Doctors may ask you to drink fluid and have soft foods after this time (8).
The urinary catheter is removed after 12 hours, and women are encouraged to move at this time. Most women can walk with support the next day. However, you may have to stay in hospital for three days after a C-section. It may take up to four to six weeks to recover completely after a C-section, and doctors prescribe medications for pain management during healing.
C-Section Recovery Tips

The following tips may help you recover from C-section delivery (9).
- Take pain medications as prescribed.
- Keep the incision area clean and dry. You may wash the incision area with soapy water, and pat dry it during the shower.
- Avoid using cleaning products on the incision site since this may slow down the healing process.
- If the incision is covered with tape strips, let it fall on its own.
- Physical activity such as walking or moving a little can be beneficial. However, you may avoid lifting heavy objects and tiring activities until you recover completely.
- Do not use tampons or douche until recommended by the doctor.
- Take showers to clean up. Avoid soaking in baths or using public hot baths or pools until the incision is healed and the postpartum bleeding ceases.
- Delay intercourse until recommended by the doctor.
- Consume a well-balanced, fiber-rich meal and plenty of water to cope with nutritional requirements for recovery and breastfeeding. Take the supplements as prescribed. Avoid crash diets to reduce weight immediately after delivery. You will lose weight eventually due to breastfeeding and the right diet.
Seek medical care if you have any physical symptoms such as fever, breathing issues, or incision site pain after returning home. In addition, emotional changes, such as troubling thoughts and depression, may also require medical attention in the postpartum phase.
Frequently Asked Questions
1. How many C-sections can a woman have?
A woman can have a maximum number of three C-sections (10). According to experts, the more C-sections you have, the higher chances of complications in the subsequent deliveries (11). However, every case is unique, and the safest number of C-sections a woman can have might vary.
2. Which week does cesarean delivery usually occur?
Planned cesarean is usually done from the 39th week of pregnancy (5). However, in cases such as placenta previa, your doctor may plan a C-section as early as 36 or 37 weeks of pregnancy to avoid excessive bleeding (12).
3. Can a planned cesarean section provide a sense of control or reduce anxiety for some women?
The childbirth experience is unique for every woman, and anxiety over childbirth can happen in any pregnancy. Studies show that anxiety levels were the highest before a C-section but decreased significantly after admission to post-operation (17).
4. How does a cesarean section help in cases where the baby is at risk of umbilical cord prolapse?
A cesarean section, also known as a C-section, can be performed in cases where the baby is at risk of umbilical cord prolapse to ensure the safety of both the baby and the mother. Umbilical cord prolapse is a labor complication that occurs shortly before or during childbirth. This condition occurs when the umbilical cord, which connects the baby to the placenta, slips out (prolapses) from its usual position and emerges through the cervix before the baby does. This can compress or occlude the cord, cutting off the baby’s oxygen supply and often necessitating prompt delivery. The most secure and expeditious delivery method typically involves a cesarean section (18).
5. What are the possible advantages of a cesarean section in preventing birth injuries, such as shoulder dystocia?
Shoulder dystocia occurs when the baby’s shoulder gets stuck behind the mother’s pubic bone during vaginal delivery. By opting for a C-section, the risk of shoulder dystocia can be significantly reduced as the baby bypasses the birth canal altogether. If you have diabetes or your baby is significantly large, your obstetrician may suggest planning a C-section(19).
6. Are there any benefits of choosing a planned cesarean section for women with a history of perineal tears or pelvic floor dysfunction?
Perineal tears can occur during vaginal childbirth, particularly in women with a history of perineal trauma or pelvic floor dysfunction. If you have experienced a third- or fourth-degree tear during previous childbirth, there is a possibility of facing a tear again during future vaginal deliveries. In certain situations, your healthcare provider might recommend a Cesarean section (C-section) as a preventive measure against tearing (20).
A C-section is the ideal childbirth your doctor might suggest for your child’s safety in case of some risks from vaginal delivery. Failure in labor progression, fetal distress, abnormal fetal heart rate, fetal macrosomia, and previous classical c-section are some contraindications of vaginal delivery that require a C-section. Thus, carefully discuss the procedure with your doctor and follow before and after-surgery instructions to protect yourself and the baby from any surgical complications. Eating a well-balanced diet, taking medicines as prescribed, and ensuring proper rest are essential to hasten postpartum recovery after a C-section.
Infographic: What Causes Pregnant Women To Have A Cesarean Section?
The rate of cesarean births has been increasing, which can be horizontal or vertical C-sections depending on maternal and fetal factors. However, what factors influence a cesarean birth? The conditions listed in the infographic below indicate when a doctor might advise a cesarean delivery to ensure the baby’s and mother’s safety.
Some thing wrong with infographic shortcode. please verify shortcode syntaxIllustration: When Is C Section (Cesarean Section) Done? Its Types & Risks
_done_its_types__risks_illustration.jpg.webp)
Image: Stable Diffusion/MomJunction Design Team
“Watch this video to learn about Cesarean Section, a surgical procedure to deliver a baby. Discover the risks factors and benefits of this procedure.”
Personal Experience: Source
MomJunction articles include first-hand experiences to provide you with better insights through real-life narratives. Here are the sources of personal accounts referenced in this article.
i. My C-section experience: What I wish I had known.https://medium.com/@rachelk.spurrier/my-c-section-experience-what-i-wish-i-had-known-9860f7941fd0
References
- Caesarean section rates continue to rise amid growing inequalities in access: WHO.
https://www.who.int/news/item/16-06-2026-caesarean-section-rates-continue-to-rise-amid-growing-inequalities-in-access - Cesarean Section.
https://www.stanfordchildrens.org/en/topic/default?id=cesarean-section-92-P07768 - Malpresentation.
https://www.sciencedirect.com/topics/nursing-and-health-professions/malpresentation - Safe Prevention of the Primary Cesarean Delivery.
https://www.acog.org/clinical/withdrawn-document?utm_source=redirect&utm_medium=web&utm_campaign=int - Cesarean Section.
https://www.nhs.uk/conditions/caesarean-section/risks/ - Having a C-section? What pregnant women should know.
https://utswmed.org/medblog/c-section-what-to-know/ - Dr Frances Hills; Caesarean section: step by step.
https://www.ogmagazine.org.au/18/4-18/caesarean-section-step-step/ - Cesarean Birth (C-Section).
https://my.clevelandclinic.org/health/treatments/7246-cesarean-birth-c-section - The Do’s and Don’ts of Healing from a C-Section.
https://intermountainhealthcare.org/blogs/the-dos-and-donts-of-healing-from-a-csection - YOU ASKED: HOW MANY C-SECTIONS CAN A WOMAN HAVE?.
https://vitalrecord.tamu.edu/asked-many-c-sections-can-woman/ - MEDICAL REASONS FOR A C-SECTION.
https://www.marchofdimes.org/find-support/topics/birth/medical-reasons-c-section - 4 Questions to Ask if Your Doctor Suggests a Scheduled C-Section
https://healthtalk.unchealthcare.org/4-questions-to-ask-if-your-doctor-suggests-a-scheduled-c-section/ - Postpartum Hemorrhage.
https://www.urmc.rochester.edu/encyclopedia/content?ContentTypeID=90&ContentID=P02486# - Some Moms Want to Give Their C-Section Babies a ‘Bacterial Baptism’ But Experts Advise Caution.
https://health.clevelandclinic.org/why-some-moms-are-giving-their-c-section-babies-a-bacterial-baptism-and-why-experts-urge-caution - Breastfeeding After Cesarean Delivery.
https://www.healthychildren.org/English/ages-stages/baby/breastfeeding/Pages/Breastfeeding-After-Cesarean-Delivery.aspx - Breastfeeding After Cesarean Birth.
https://llli.org/breastfeeding-info/breastfeeding-cesarean-birth/ - Measuring the course of anxiety in women giving birth by Cesarean section; A prospective study
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4870728/#:~:text=Planned%20post%2Dhoc%20paired%2Dsamplelevels%20significantly%20decreased%20(p%20%3C%20. - Umbilical cord prolapse.
https://my.clevelandclinic.org/health/diseases/12345-umbilical-cord-prolapse - Shoulder Dystocia.
https://my.clevelandclinic.org/health/diseases/22311-shoulder-dystocia - Vaginal tears during childbirth.
https://my.clevelandclinic.org/health/diseases/21212-vaginal-tears-during-childbirth
Community Experiences
Join the conversation and become a part of our nurturing community! Share your stories, experiences, and insights to connect with fellow parents.
Read full bio of Dr. Shashwat Jani
Read full bio of Dr Bisny T. Joseph
Read full bio of Rebecca Malachi
Read full bio of Reshmi Das