Image: Shutterstock
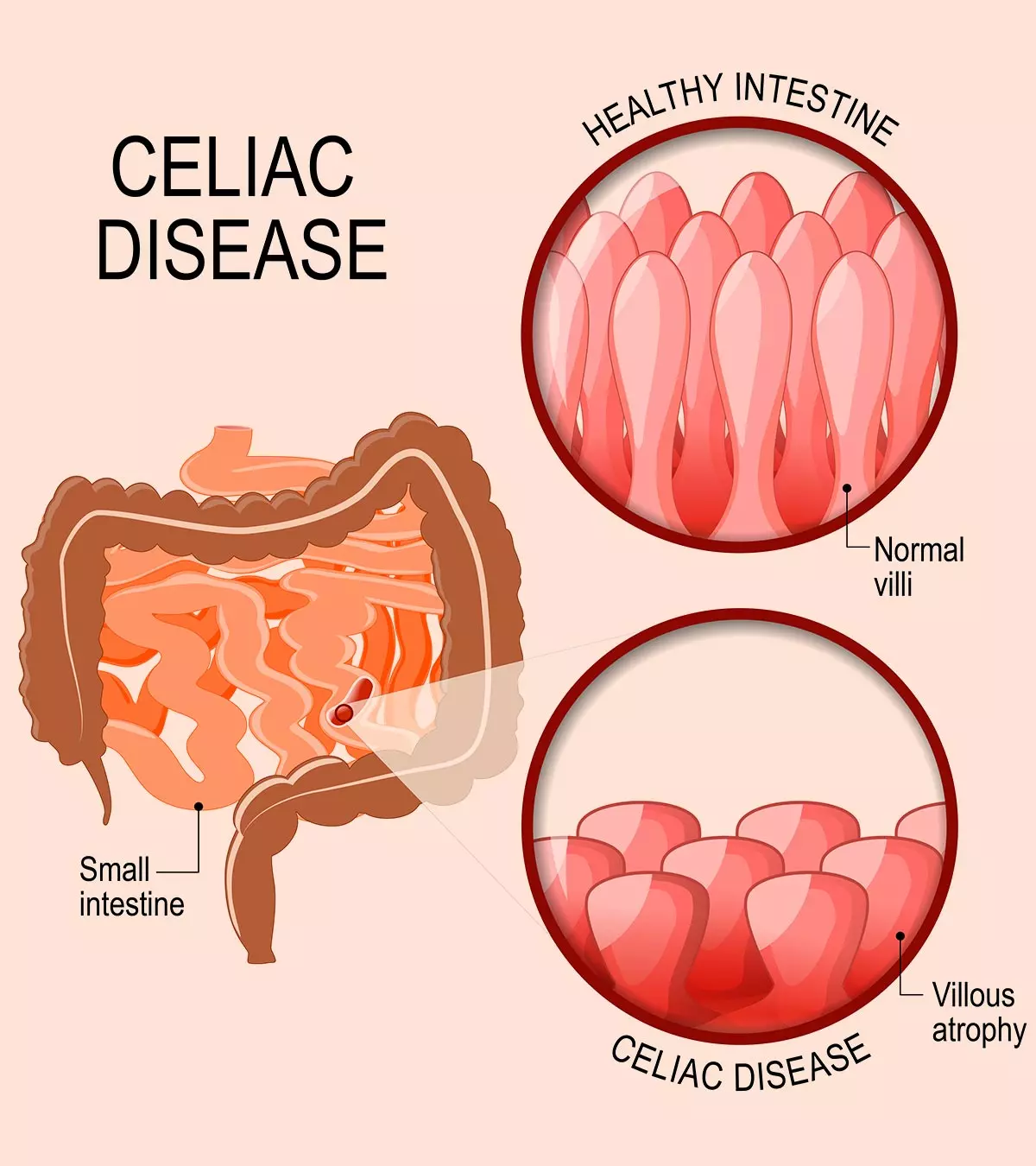
Celiac disease in teens can cause abdominal pain, constipation, and vomiting. In addition, delayed growth in adolescence and short stature requires diagnosis tests in teens. Celiac disease is also called celiac sprue or gluten-sensitive enteropathy. It causes an immune reaction to the gluten protein found in rye, wheat, and barley and damages the intestinal lining. It can occur at any age in people with a genetic predisposition to this disorder. If left untreated, this may result in malnutrition and anemia with poor growth in children and teens (1).
Read on to learn more about signs, symptoms, causes, high-risk groups, and treatment of celiac disease in teens and gluten-free diet, including the best food choices for teens.
Key Pointers
- Celiac disease damages the intestinal lining due to an immune reaction to gluten in wheat, barley, and rye.
- Symptoms of celiac disease include chronic diarrhea, constipation, abdominal pain, weight loss, and anemia.
- Risk factors for celiac disease include autoimmune thyroid diseases, Down syndrome, positive family history, and Diabetes Mellitus type I.
- Gluten sensitivity is a food allergy to gluten with symptoms like abdominal pain, diarrhea, and bloating, but normal test results.
- Untreated celiac disease can lead to complications such as malnutrition, anemia, and poor growth in children and teens.
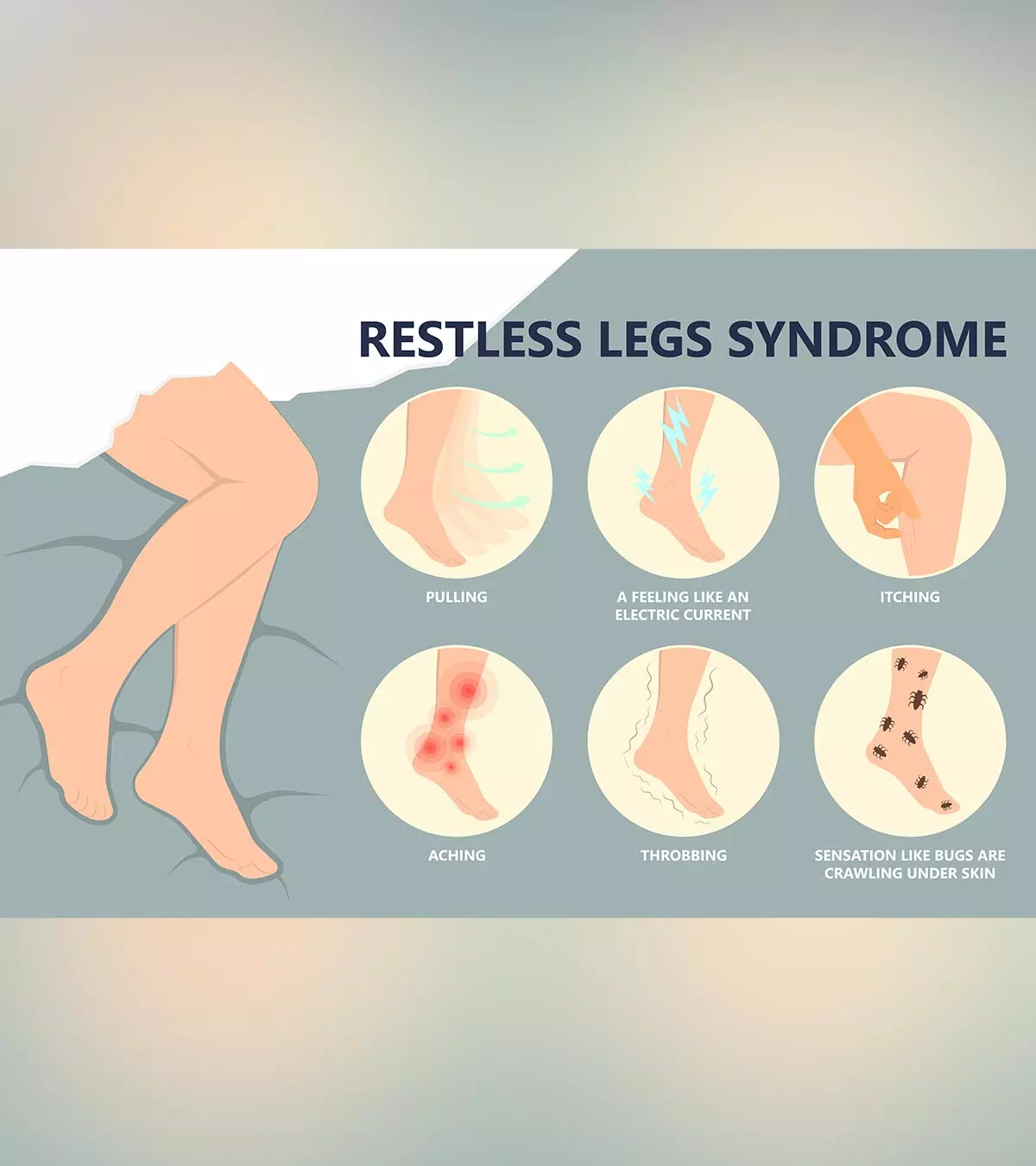
Signs And Symptoms Of Celiac Disease In Teens

Symptoms and signs of celiac disease may vary in each person. They may include both intestinal (digestive) and extraintestinal symptoms. Extraintestinal manifestations can be due to malabsorption of essential nutrients. Children tend to have more digestive manifestations compared to celiac sprue signs in adults.
The common symptoms and signs of celiac disease may include (2):
- Chronic diarrhea
- Nausea
- Vomiting
- Constipation
- Abdominal pain
- Flatulence and bloating (intestinal gas)
- Pale, foul-smelling, and greasy stools
- Tooth enamel damage
- Weight loss
- Headaches
- Anemia (iron deficiency anemia)
- Delayed puberty
- Short stature compared to parents’ height
- Learning difficulties
- Fatigue
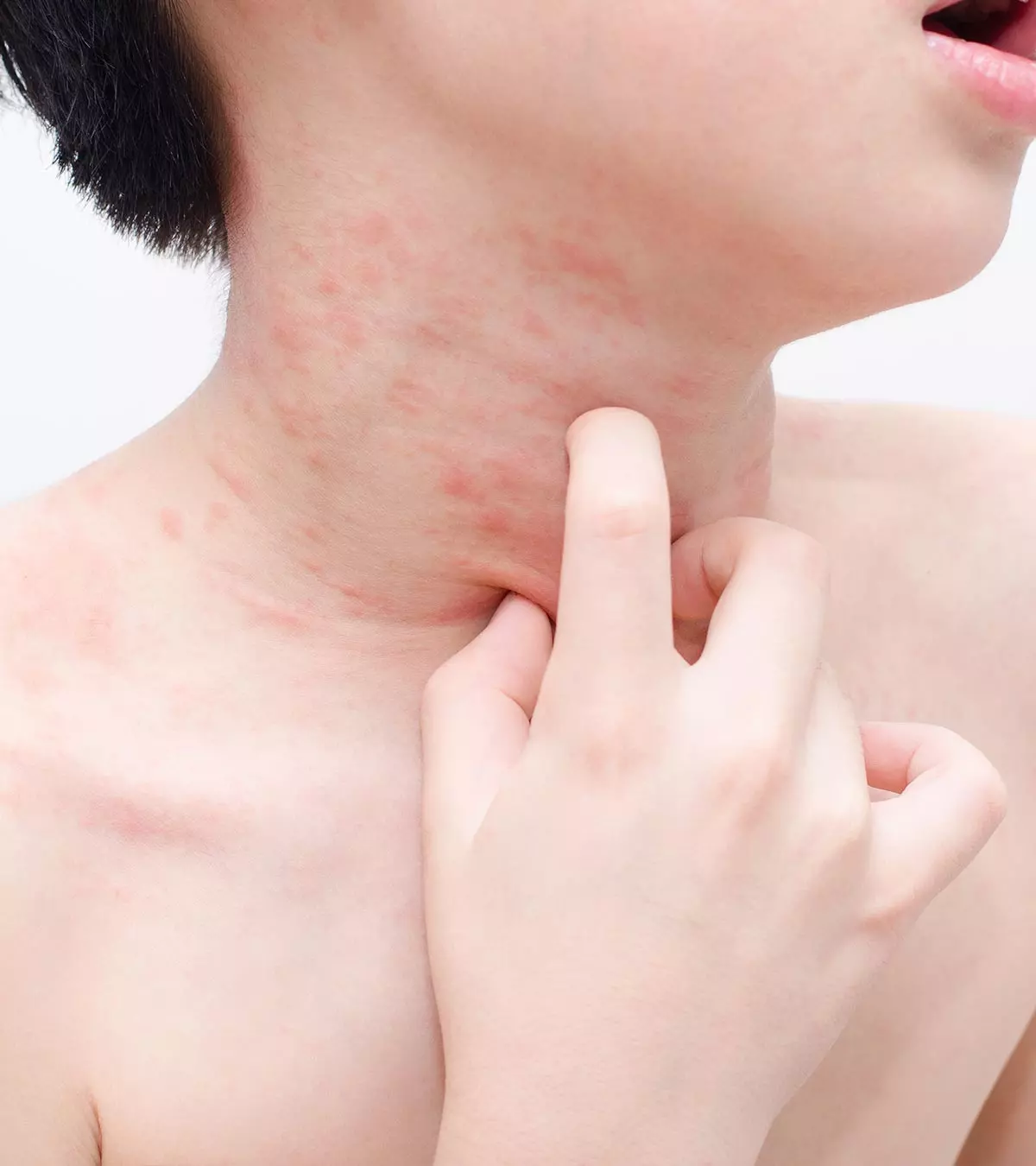
- Skin rash
- Mouth ulcers
These symptoms and signs are not specific to celiac disease, so your teen requires medical assessment for diagnosis.
 Quick fact
Quick factWhat Does The Celiac Rash Look Like?
Cutaneous manifestation of celiac disease is evident as skin rashes that are known as dermatitis herpetiformis. They manifest as incredibly pruritic (itchy) skin lesions often on elbows, scalp, buttocks, knees, and torso (3).
According to the National Institutes of Health (NIH), two to three percent of children and 10 to 20 percent of adults with untreated celiac disease have dermatitis herpetiformis. Also, some individuals may have the rash and no other symptoms.
Rashes similar to dermatitis herpetiformis are also seen in certain other autoimmune disorders and skin diseases. Therefore, it is best to let the doctor take a look to make a diagnosis.
Causes Of Celiac Disease In Teens
Celiac disease is caused by an abnormal response of the immune system to gluten, a protein found in barley, wheat, and rye. It leads to an immune-mediated inflammation of the small intestine. This gluten sensitivity is caused by a problematic HLA DQ protein-coding gene located on chromosome number six. This gene can be inherited (hereditary), which means the condition can run in families. One in ten teens with close relatives or family members with celiac disease could develop the condition (4).
If a person with celiac disease eats gluten or gliadin-containing foods, then it triggers an immune response, which could damage the small intestine leading to inadequate nutrient intake or nutritional deficiencies (5).
Gluten Sensitivity Vs. Celiac Disease

Celiac disease is an autoimmune disorder. It causes damage to the intestine from the immune system’s response to gluten, whereas gluten sensitivity is more like a food allergy to gluten.
Gluten sensitivity is intolerance to a gluten-containing diet, which may often result in symptoms such as abdominal pain, diarrhea, bloating, and gasses. This condition is called non-celiac gluten sensitivity (NCGS) or gluten intolerance (5).
The symptoms usually improve with a gluten-free diet and recur with the consumption of gluten. However, blood tests and endoscopic imaging show normal results in gluten sensitivity.
Celiac disease is an autoimmune disorder that affects the digestive system. If a person with celiac disease eats gluten-containing foods, then it triggers an immune response, which could lead to small intestine damage. Over time, this damage can result in nutrient malabsorption, causing nutrient deficiencies (6).
Risk Factors For Celiac Disease

The following conditions may increase the risk of developing celiac disease (7).
- Autoimmune thyroid diseases
- Down syndromeiA chromosomal disorder caused by the presence of an extra copy of chromosome 21, resulting in intellectual impairment and short stature
- Turner syndromeiA chromosomal condition in which a female is born with only one sex chromosome and Williams syndromeiAn uncommon genetic condition that affects physical appearance, cognitive development, and cardiovascular health
- Positive family history of dermatitis herpetiformis or gluten intolerance
- Diabetes mellitus type IiA lifelong condition caused by less or no insulin production leading to high blood sugar levels in the blood
- Selective IgA deficiency
- Addison's diseaseiA condition due to an insufficiency of cortisol and aldosterone
- Microscopic colitis also known as collagenous colitis or lymphocytic colitis
When To See A Doctor
You may consult a doctor if your teen has any concerning signs and symptoms of celiac disease. Also, see a doctor in the following scenarios.
- Digestive disorders, such as diarrhea, abdominal pain, or any other gastrointestinal problems, lasting longer than two weeks.
- If you have a close relative or family member with celiac disease. You can mention it to your teen’s doctor during regular visits. They can make early assessments and prevent its complications.
Trying a gluten-free diet before diagnosis may give false-negative results
. Therefore, seek consultation when your teen is on a regular diet that includes gluten for an exact diagnosis.
Diagnosis Of Celiac Disease
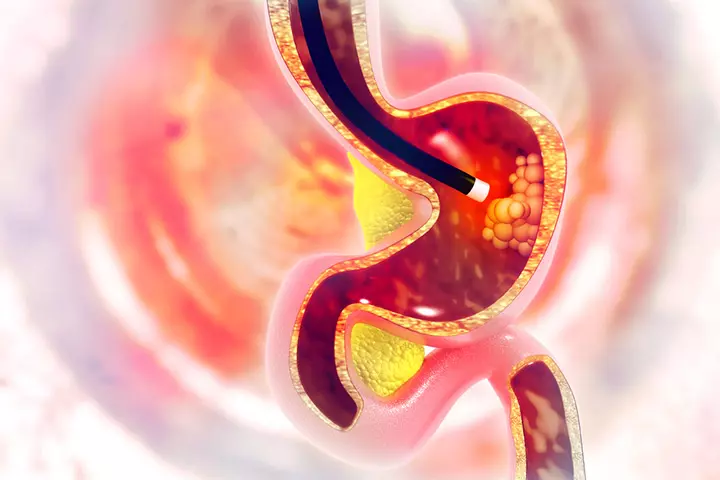
If the signs and symptoms are suggestive of celiac disease or if there is a positive family history, then your teen’s doctor may order the following tests (8).
- SerologyiA branch of medicine that studies the presence of substances in the blood sample testing looks for antibodies against gluten, which are produced during an immune reaction.
- Genetic tests help identify defective genes that point towards celiac disease.
If the results from serologic and genetic tests are positive, then your teen may have to undergo the following tests to visualize the intestines (8).
- Endoscopy uses a tiny flexible tube with a camera to visualize the digestive tract.
- Capsule endoscopy uses a tiny wireless camera to look for intestinal damages.
- Skin tissue is collected for skin biopsy if dermatitis herpetiformis is seen.
Nonresponsive And Refractory Celiac Disease
The following cases of celiac disease may require special care for a longer duration (9) (10).
- Nonresponsive celiac disease: This is a complex autoimmune disease where the person continues to display symptoms of celiac disease and intestinal damage despite following a gluten-free diet for six months to a year. People with this condition may show improvement initially, but then experience a relapse of symptoms.
- Refractory celiac disease (RCD) or refractory sprue: This is a rare and severe form of celiac disease and affects no more than 4% of individuals with celiac disease. It is marked by persistent symptoms and intestinal damage (villous atrophy) despite having a gluten-free diet.
The above conditions may require an additional examination to exclude the following diseases (11):
- Pancreatic insufficiency
- Bacterial overgrowth
- Microscopic colitis
- Irritable bowel syndrome
- Lactose intolerance
- Fructose intolerance
Unresolved celiac disease can also indicate contamination of diet with gluten. In such scenarios, your teen may require help from specialized dieticians.
Treating Celiac Disease In Teens

The initial management plan for celiac disease is a gluten-free diet. Sometimes medications are required to control intestinal inflammation. They include (11):
- Steroid medications to relieve symptoms of refractory celiac disease and if your teen has severe damage of the intestinal wall.
- Immunosuppressive medicinesiMedicines that reduce or inhibit the body’s immune response , such as Entocort EC or Uceris (budesonide) and Azasan or Imuran (azathioprine), to help relieve the symptoms.
- Oral intake of the antibiotic dapsone with a gluten-free diet to heal celiac skin rash. Your teen may require regular blood tests to assess the side effects of dapsone therapy.
- Vitamins and mineral supplements for nutritional deficiencies and anemia due to malabsorption. Oral supplementations are given for most teens. Intravenous supplementation may be considered in cases of severe malabsorption.
During the treatment period, you may have to follow up with tests, including blood tests, to assess the effectiveness of treatment and gluten-free diet. It can take months for intestines to heal. Your doctor may order an endoscopy if symptoms persist.
Foods And Ingredients To Avoid
The best way to manage celiac disease and control dermatitis herpetiformis is to consume an entirely gluten-free diet for the entire life. The gluten-containing foods are (12):
- Wheat
- Rye
- Barley
- Malt
- Semolina
- Farina
- Durum
- Graham flour
- Triticale
The following ingredients or products may contain gluten and often go unnoticed (13).
- Food preservatives
- Food stabilizers
- Modified food starch
- Supplements of essential nutrients
- Medications
- Lipstick
- Toothpaste
- Mouthwash
- Communion wafers
- Beer
- Malt vinegar
- Candies
- Sauces such as soy sauce
- Salad dressings
- Pasta
- Cereals
- Baked items
Processed, marinated, coated, and imitation meat, poultry, or seafood can also be contaminated with gluten through cross-contamination. You may also avoid seasoned snacks and packed foods. Celiac patients can eat pure oats and oats products. However, oats have a higher chance of contamination with wheat during processing. Always make a habit of reading food labels to find gluten content.
Avoiding gluten in diet may reduce small intestinal inflammation and damage. You need to educate the teen about the importance of avoiding a gluten diet.
 Quick tip
Quick tipGluten-Free Foods
The following food items, among various others, can be included in the diet (14).
- Fruits
- Vegetables
- Fresh meat and poultry
- Eggs
- Fish
- Lentils
- Dairy products
- Nuts
- Corn and cornmeal
- Rice
- Buckwheat
- Amaranth
- Gram flour
- Quinoa
- Tapioca
Dairy products should be taken after consultation with the doctor. If your teen has lactose intolerance due to intestinal damage, then dairy products might worsen the condition. Distilled alcohol and wine are gluten-free alcoholic beverages.
Sharing her experience dealing with celiac disease during her college days, Casey Cromwell recounts, “I needed more than just a gluten-free diet to heal from my celiac complications. I cut out dairy when I noticed how much it bothered my stomach. I eventually discovered the low FODMAP diet and pinpointed several foods, like garlic, onion, and mango, that turn my tummy into a time bomb. I avoided (even the gluten-free) foods my stomach didn’t seem to tolerate at the time. I also ate to my appetite, even when my hunger was insatiable (i).”
Cromwell discovered that her condition required more than just avoiding gluten, highlighting the importance of individualized dietary adjustments in managing celiac disease.
 Quick tip
Quick tipComplications Of Celiac Disease In Teens
The following complications may occur if celiac disease is left untreated (11) (15).
- Malnutrition can occur due to malabsorption of essential nutrients from the small intestine. This may cause weight loss, short stature, growth delay, and anemia in teens.
- Long term malabsorption of vitamin D and calcium may result in weakening of the bones. Children may have rickets or softening of bones (osteomalacia) and may develop osteoporosis as adults.
- Malabsorption may also affect reproduction in the future by causing conditions such as miscarriage or infertility.
- Untreated gluten enteropathy may pose an increased risk of small bowel cancer and intestinal lymphoma.
- Seizures and peripheral neuropathy in nerves of hands and feet are often seen in some cases.
- Intestinal wall damage may cause lactose intolerance, resulting in gas, diarrhea, and abdominal pain in teens on the consumption of dairy products.
Frequently Asked Questions
1. What happens if I have celiac and eat gluten?
If you have celiac and accidentally eat gluten, you may experience typical symptoms such as vomiting, diarrhea, and abdominal pain. But it mostly isn’t a long-term reaction, and consulting a doctor to alleviate the symptoms can help manage the situation (16).
2. Can I grow out of celiac disease?
No, celiac is a lifelong autoimmune disorder, and a person with the disease cannot grow out of it (17).
3. Is one born with celiac, or does it develop later?
Celiac is genetic or hereditary, i.e., a person with the condition will carry the genetic variant of the disorder from birth that may get activated or triggered after consuming gluten (18).
4. Does celiac disease affect puberty in teens?
Yes, celiac disease may affect puberty. In girls, it delays the onset of puberty or menarche. In boys, there are hormonal imbalances (19).
5. At what age does celiac disease appear?
Celiac disease can appear any time after introducing gluten to your child’s diet, typically after 6-9 months. It is unknown why it shows early in some children and late in others (20).
6. How long can celiac disease go undetected?
Celiac disease can go undetected for years, even decades, as many of its symptoms, including gastrointestinal symptoms, are similar to other common gastrointestinal conditions. In addition, some people may not experience any symptoms at all. On average, it takes about 6 to 10 years from the onset of symptoms to receive a correct diagnosis. Regular check-ups and screening tests can help detect the condition earlier (21) (22).
7. How long does a celiac flare-up last?
Celiac flare-ups can last anywhere from a few hours to several days, depending on the severity of your condition and the amount of gluten ingested (23).
Celiac disease in teens can significantly impact their quality of life. This autoimmune disorder occurs when the immune system reacts abnormally to gluten, causing damage to the small intestine and leading to nutritional deficiencies. Teens may experience vomiting, weight loss, headaches, and constipation. Treatment involves steroid medications, nutritional supplements, and diet changes. Doctors may recommend a gluten-free diet for your teenagers. However, following this diet may be challenging for you and your child. Seek your doctor’s advice to choose suitable food options and support your teenager in their journey.
Infographic: Treating Celiac Disease In Teens
The treatment for celiac disease in teens involves following a strict gluten-free diet to manage symptoms and prevent further damage to the small intestine. In addition to dietary changes, some teens may also need to take medications to help control their symptoms and manage the underlying autoimmune process. This infographic explains the different treatment methods commonly used for celiac disease. Illustration: Momjunction Design Team
Illustration: Common Signs And Symptoms Of Celiac Disease In Teens

Image: Dall·E/MomJunction Design Team
Celiac disease is an autoimmune condition. This video provides valuable insights into the causes, symptoms, management, and treatment.
Personal Experience: Source
MomJunction articles include first-hand experiences to provide you with better insights through real-life narratives. Here are the sources of personal accounts referenced in this article.
i. I have celiac disease, but a gluten-free diet wasn’t enough;https://caseythecollegeceliac.blogspot.com/2017/06/i-have-celiac-disease-gluten-free-diet-not-enough.html
References
1. Santiago Vivas et al., Age-related differences in celiac disease: Specific characteristics of adult presentation; The United States National Library of Medicine
2. Symptoms & Causes of Celiac Disease; The National Institute of Diabetes and Digestive and Kidney Diseases
3. Dermatitis Herpetiformis (For Health Care Professionals); The National Institute of Diabetes and Digestive and Kidney Diseases
4. What is Celiac Disease?; Celiac Disease Foundation
5. Celiac Disease, Non-Celiac Gluten Sensitivity or Wheat Allergy: What is the Difference?; Gluten Intolerance Group
6. Celiac Disease; MSD Manual
7. Coeliac disease; National Health Service
8. Diagnosis; Celiac Disease Center; The University of Chicago Medicine
9. Non responsive and refractory coeliac disease; Coeliac UK; Livewell
10. Carol Semrad, What is nonresponsive celiac disease?; The University of Chicago Medicine
11. Abdulbaqi Al-Toma et al., European Society for the Study of Coeliac Disease (ESsCD) guideline for coeliac disease and other gluten-related disorders; United European Gastroenterology Journal
12. Eating, Diet, & Nutrition for Celiac Disease; The National Institute of Diabetes and Digestive and Kidney Diseases
13. Sources of Gluten; Celiac Disease Foundation
14. Gluten free diet for coeliac disease; My Nutrition; The Queensland Government
15. C J R Goddard and H R Gillett; Complications of coeliac disease: are all patients at risk?; The United States National Library of Medicine
16. What happens if someone with coeliac disease eats gluten by mistake?; Coeliac UK
17. Center for Celiac Research: Celiac Disease FAQ; Massachusetts General Hospital
18. Celiac Answer Bank; National Library of Medicine
19. Mechanisms of abnormal puberty in coeliac disease; National Library of Medicine20. Celiac Disease in Children; Celiac Disease Foundation
21. Symptoms of Celiac Disease; Celiac Disease Foundation
22. 20 Things You Might Not Know About Celiac Disease; Celiac Disease Foundation
23. Coeliac disease symptoms; Coeliac UK
Community Experiences
Join the conversation and become a part of our nurturing community! Share your stories, experiences, and insights to connect with fellow parents.
Read full bio of Dr. Elna Gibson
Read full bio of Dr Bisny T. Joseph
Read full bio of Swati Patwal
Read full bio of Anindita Ghatak