Image: ShutterStock
Symptoms of most viral and bacterial infections in babies may look similar, but the treatments vary. So it is recommended to seek pediatric consultation to identify and treat the exact causes. Giving over-the-counter medications and antibiotics for viral infection may not be helpful, and it also causes resistance to drugs later. It is also essential to determine the dose and duration of the medications to prevent recurrence and resistance. Knowing the risks associated with bacterial infections in infants can help you provide prompt treatment and avert serious complications and long-term developmental issues.
Bacterial infection can occur in newborns and older infants and is often accompanied by fever and other symptoms. Although many pathogenic or disease-causing bacteria lead to infections, some good bacteria in the gut microbiome, such as lactobacillus, promote good gut health and digestion (1). Read on to know more about common bacterial infections in babies
Key Pointers
- Although the signs of viral and bacterial infections in infants can be similar, the treatments differ.
- Bacterial infections include listeriosis, pneumonia, conjunctivitis, urinary tract infections, streptococcal diseases, and impetigo.
- Common signs of a bacterial infection include poor appetite, labored breathing, skin rashes, sore eyes, diarrhea, drowsiness, and lethargy.
- Bacterial infections can be diagnosed via a urine test, blood test, blood cultures, and imaging tests.
- Treatment for mild bacterial infections in babies includes antibiotics, antipyretics, and oral rehydration.
What Are The Signs And Symptoms Of Bacterial Infections?
Babies infected with bacterial infections can exhibit any of the following symptoms (2).
- Fever, cough, rhinitis or runny nose

Image: IStock
- Poor appetite and feeding
- Labored breathing
- High pitch crying
- Diarrhea
- Vomiting
- Drowsiness
- Lethargy
- Cranky mood
- Skin rashes
- A swollen or bulging fontanelle (soft spot on the head), vomiting, fever, abnormal reflexes, and poor feeding are some symptoms unique to meningitis (3).
- Mottling of skin might be seen in babies who have sepsis (4).
- Coughing is seen in babies with pneumonia.
- Granulomatosis infantiseptica, a characteristic skin rash with widespread small, pale nodules on the skin is a unique symptom of listeriosis (5)
- Teary, itchy, puffy, and sore eyes are seen in conjunctivitis. Occasional green or yellow discharge is also seen at the corner of the eyes (6).
Contact a healthcare provider if your baby is unwell, and you suspect an infection.
 Be watchful
Be watchfulCommon Bacterial Infections In Babies
There are several bacterial infections that can affect babies. Below is a list of the common ones (7).
1. Group B streptococcal diseases
A. Meningitis
B. Sepsis
C. Pneumonia

Image: Shutterstock
2. Listeriosis
3. Conjunctivitis
4. Urinary tract infections
5. Gastrointestinal infections
6. Impetigo
There can be several causes behind each of these bacterial infections in babies.
Causes Of Bacterial Infection In Babies
1. Group B streptococcal diseases
Group B streptococcus (GBS) bacteria are commonly found in the digestive tract, urinary tract, and genital areas of adults (2).
About one in four pregnant women has GBS in their rectum or vagina. A baby can get it from the mother during vaginal birth (8). Most babies show symptoms of GBS after a few hours or days after birth (9).
A. Meningitis
- Meningitis is the inflammation of the membranes that surround and protect the brain and spinal cord.
- Early signs and symptoms can appear similar to those of flu or stomach infection.
- Newborns can pick up one of these pathogens from the mother during birth or from their surroundings.
- Infants with meningitis are usually hospitalized for monitoring and intensive care.
B. Sepsis
- Septicemia is an infection that may travel to different organs through the bloodstream.
- It is an emergency condition and needs immediate medical attention.
- Early-onset neonatal sepsis appears between the time of birth and six days of life. It is most commonly seen within 24 hours of birth. The babies are infected during pregnancy or at the time of delivery.
- Babies with late-onset neonatal sepsis are infected after delivery. It is usually seen seven days after birth up to the age of seven months.
- Babies born prematurely are at a higher risk of getting this infection (4).
C. Pneumonia
- Pneumonia is an infection of the lungs.
- The air sacs in the lungs might be filled with fluid, mucus, or pus, which causes labored breathing in babies.
- The condition prevents enough oxygen from reaching the blood and other organs of the body.
- Pneumonia is generally more common in children younger than five years old (10). Furthermore, according to the World Health Organization (WHO) statistics, pneumonia accounted for 14% of all deaths among children aged zero to five in 2019.
2. Listeriosis
- Listeriosis is a rare but serious infection caused due to the consumption of contaminated food. The infection is caused by the Listeria monocytogenes bacterium.
- Though rare, it can affect newborns (5).
- Neonatal listeriosis occurs in approximately 8.6/100,000 of live births (11).
3. Conjunctivitis
Conjunctivitis is an inflammation of the conjunctiva, which is a lining that covers the white part of the eye and inside of the eyelids. This infection is commonly known as “pink eye”since it changes the color of the white part of the eye to red or dark pink.
Staphylococcus aureus, Haemophilus influenzae, and Streptococcus pneumonia are some of the common bacteria that could cause pink eye in babies (6).
4. Urinary tract infections (UTI)
UTIs are bacterial infections that affect the kidneys, urinary bladder, urethra, or the ureters.
Babies have a fever. As they cannot communicate the common complaints of UTI like burning or pain during urination, they might exhibit unexplained crying while urinating (12).
5. Gastrointestinal infections

Image: IStock
Gastrointestinal infections are among the common bacterial infections during infancy (13).
The World Health Organization (WHO) states that each year, diarrhea fatally affects about 525,000 children under the age of five years (14). (most of the deaths are due to dehydration rather than infection itself). Escherichia coli (E.coli), campylobacter, and salmonella are common bacterial causes of gastroenteritis.
Babies under six months of age might get quickly dehydrated due to gastrointestinal infections.
Profuse oral rehydration is recommended with ORS solution, and intravenous fluid replenishment might be needed in severe cases(15).
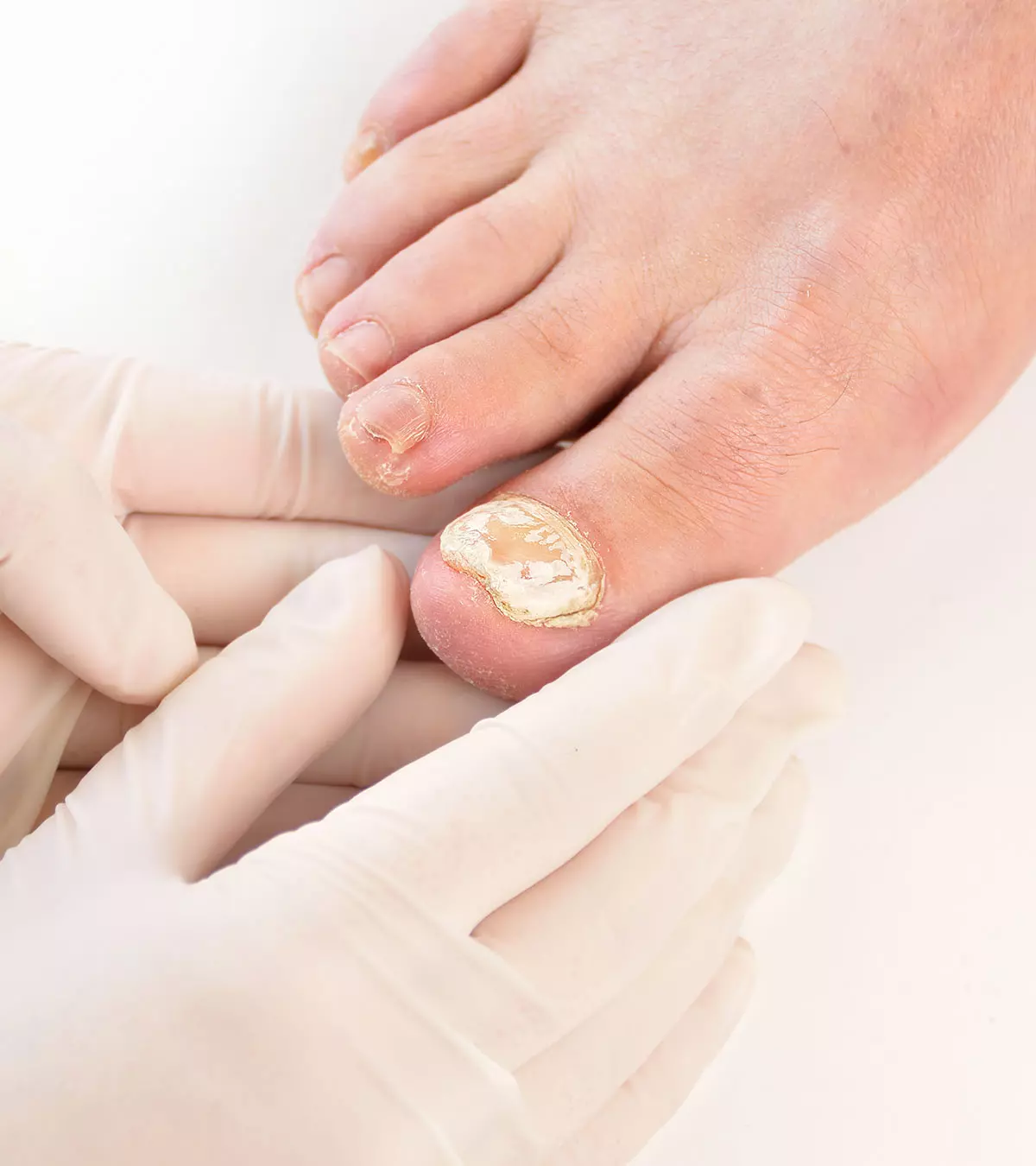
6. Impetigo
It is a contagious skin infection commonly caused by bacteria such as Staphylococcus aureus or Streptococcus pyogenes. It is characterized by small vesicles (blisters or sores) seen on the surface of the skin.
Impetigo is broadly classified into two types (16):
- Non-bullous impetigo
Vesicles grow up to two centimeters and are filled with pus. They persist for several days. The enlargement of lymph nodes is usually not seen.
Some bacterial infections can also hamper a baby’s hearing ability, such as in the case of otitis media. Therefore, always consult a doctor at the earliest if you suspect any bacterial infection in your babies as bacterial infections might spread quickly and worsen the condition.
- Bullous impetigo
Vesicles grow up to two centimeters and are filled with pus. They persist for several days. The enlargement of lymph nodes is usually not seen.
Always consult a doctor at the earliest if you suspect any bacterial infection in your babies as bacterial infections might spread quickly and worsen the condition.
Diagnosis Of Bacterial Infection

Image: Shutterstock
Bacterial infections are most often diagnosed through the observation of symptoms. The following are some of the common diagnostic tests used to determine the type of bacterial infection (17).
- Physical examination: For diseases like impetigo, the doctor usually identifies the disease based on the appearance of the rash (16).
- Blood tests: White blood cells count, and platelet count can help indicate the presence of an infection.
- Blood cultures: Blood samples are cultured for bacterial growth. This method can help identify precise bacterium.
- Urine tests: Urine samples are checked under a microscope or cultured to confirm the presence of bacteria.
- X-ray: A chest x-ray might be needed when the baby is suspected of having pneumonia.
- CT scans or MRI: These scans help show the inflammation in the membranes that cover the brain and the spinal cord (18).
- Spinal tap or lumbar puncture: A small quantity of cerebrospinal fluid is collected through a needle inserted into the spinal column. The invasive procedure is usually done as a last resort. It is an accurate way to diagnose sepsis and meningitis (19).
- Culture of other samples: In a few cases, the doctor might collect gastric juices, meconium (first stool of the baby), and infected tissue through a biopsy to determine the type of bacteria (20).
Laboratory culture of samples often takes 24-48 hours to yield results (21).
Meanwhile, the infants might be started on empirical antibiotic therapy (preferably after taking the blood sample for culture and sensitivity), which means antibiotics against the most suspected causative bacteria.
Common Treatment Options For Bacterial Infections
There are some specific treatment criteria for bacterial infections. It is essential to identify the bacteria that caused the infection and plan the treatment accordingly. The following are the common treatment procedures used in the treatment of bacterial infections in babies (7) (10).
- Antibiotics: It includes both oral and intravenous antibiotics. The exact type of antibiotic and mode of administration depends on the type of bacteria diagnosed, age of the baby, and severity of the illness.
- Antipyretics: Medicines like acetaminophen/ paracetamol might be given to babies to reduce the fever that happens because of bacterial infections.
- Rehydration: Oral rehydration is recommended by doctors when the babies are dehydrated due to vomiting or diarrhea. In very young infants, the doctors might recommend IV rehydration.
- Nasogastric tubes or gavage tube: For babies who do not feed adequately, a pipe might be inserted through the mouth or the nose in a way that milk drips into their stomachs. It prevents malnourishment and helps keep the immune system strong.
- Corticosteroids: These medicines help reduce swelling and relieve the pressure that might occur in the brain due to bacterial meningitis.
- Blood and plasma transfusions: It might be needed in babies who have developed severe sepsis.
Your baby’s pediatrician will make the best treatment choice according to the progression and severity of the infection. It is vital to consult with a healthcare professional before giving any medications, as improper use of antibiotics can lead to resistance and complications. It is also important to complete the entire course of antibiotics as suggested by your baby’s doctor.
 Things to know
Things to knowHow Do You Prevent Bacterial Infection In Babies?
Most bacterial infections are contagious. While not all bacterial infections can be prevented, taking some precautions may lower the risk of contracting the infection (22).
- Maintain good hygiene around the baby. Wash their hands after returning from outdoors. If you or some family member has a cold or other infection, then wash hands before holding the baby and their belongings. It is good to wear a mask while handling the baby to prevent the transmission of bacteria through cough or sneezes.

Image: Shutterstock
- Always dispose of soiled diapers into a dustbin or diaper pail to prevent bacteria from transferring to the surroundings.
- Promptly clean any open wounds with baby-safe disinfectant and see the doctor for the further dressing of the wound and medication.
- Vaccinate your child against common childhood diseases. The American Academy of Family Physicians recommends immunizing all babies unless contraindicated. Some types of pneumonia in babies can be prevented with vaccines (23).
- Prevent exposure to tobacco smoke. Exposure to second-hand smoke increases a baby’s risk of developing pneumonia.
- Only serve cooked food or sealed ready-to-eat infant food (homemade food). Never feed the baby anything raw since it can expose the little one to bacteria. Store uncooked food away from cooked and ready-to-eat food meant for the baby (24).
- For the prevention of neonatal conjunctivitis, the state law requires most hospitals to administer antibiotic eye drops that contain erythromycin to the baby after birth (25).
According to the WHO, adequate nutrition is essential to improve a baby’s immunity. They strongly recommend exclusive breastfeeding for the first six months of life. It helps reduce the length of illness (26).
Frequently Asked Questions
1. Are there any home remedies for bacterial infection in babies?
There is no research-based evidence on any effective home remedies for bacterial infections in babies. Bacterial infections spread quickly and might lead to complications if left unattended. You should seek a doctor or infant immunology expert’s advice if you suspect an infection in your baby.
2. How long does bacterial infection last in babies?
The longevity of the disease depends on several factors such as age, weight, the severity of the disease, and the general health and immunity of the baby.
3. How do you know if it’s a bacterial or viral infection?
Viral and bacterial infections exhibit several similar symptoms. Therefore, it can be difficult to tell the cause through the symptoms alone. But generally speaking, in viral infection the child does not look to be sick and temp is also low grade while in bacterial infection the child looks sick and toxic with high grade fever. You should take your baby to a pediatrician for the right diagnosis. Blood and urine tests can help determine the exact pathogen that has caused the infection.
4. How often do babies get bacterial infections?
Babies are born with immature immune systems that begin developing defenses after birth. As a result, children often get infected with bacterial and viral infections, the frequency of which may range between four and eight conditions per year (27).
5. Are bacterial infections more contagious than viral infections?
No, bacterial infections are less contagious and respond better to medications such as antibiotics than viral infections (28).
Fever, lack of appetite, and crying are common symptoms of bacterial infections in babies. However, it is recommended to visit the pediatrician to diagnose the cause of infections since bacterial and viral infection symptoms can be similar. Pneumonia, group B streptococcal disease, sepsis, and meningitis are common bacterial infections in babies. Symptomatic treatments such as fever medications and antibiotics are also prescribed to manage bacterial infections. Giving vaccinations as per the schedule and maintaining good hand hygiene while handling a baby may help to prevent most bacterial infections.
Infographic: What Are The Common Bacterial Infections In Infants?
Babies are prone to infections due to their underdeveloped immune system. However, differentiating between a viral and bacterial infection is crucial since they have different treatment options. The infographic below includes some typical bacterial infections a baby may develop. Knowing about them can help parents opt for medical care as early as possible.
Some thing wrong with infographic shortcode. please verify shortcode syntaxIllustration: Signs Of Bacterial Infections Causes Diagnosis & Treatment

Image: Stable Diffusion/MomJunction Design Team
Expand your knowledge of the causes and prevention of bacterial infections through this informative video.
References
1. Bacterial Infections; Journal of Bacteriology and Parasitology
2. Group B Streptococcus Infection in Babies; Cedars Sinai
3. Bacterial Meningitis; Centers for Disease Control and Prevention
4. Group B streptococcal septicemia of the newborn; US National Library of Medicine
5. Listeriosis; National Organization for rare Disorders
6. Conjunctivitis in Children; Stanford Children’s Health
7. Neonatal Infections; John Hopkins Medicine
8. Group B Streptococcus Infection in Babies; University of Rochester Medical Center
9. GBS infection in babies;; Group B Strep Support
10. Pneumonia in Children; Stanford Children’s Health
11. Ronald F. Lamont et al, Listeriosis in Human Pregnancy: a systematic review; The Journal of Perinatal Medicine
12. Urinary Tract Infection (UTI) in Children; MSD manuals
13. Alter SJ et al, Common childhood bacterial infections..; US National Library of Medicine
14. Diarrhoeal disease; World Health Organization
15. Gastroenteritis in children; Victoria State Government
16. Patty Ghazviniet al, Impetigo in the Pediatric Population; Journal of Dermatology and Clinical Research
17. Detecting bacterial infections in newborns; US Department of Health and Human Services
18. Meningitis in Children; Stanford Children’s Health
19. Sepsis in Newborns; MSD Manual
20. Neonatal Listeriosis; MSD Manual
21. Overview of Bacterial Infections in Childhood; MSD Manual
22. Repeated infections in children; The Family Doctor Organization
23. Hib (Haemophilusinfluenzae type b); Immunization Action Coalition
24. Bacterial Diarrhea (Infant/Toddler); Fairview Organization
25. Conjunctivitis (Pink Eye) in Newborns; Centers for Disease Control and Prevention
26. Pneumonia; World Health Organization
27. Why do children get repeated infections?; Family Doctor (org)
28. Viral illnesses vs. Bacterial infection; Pediatric Association of Richmond
Community Experiences
Join the conversation and become a part of our nurturing community! Share your stories, experiences, and insights to connect with fellow parents.
Read full bio of Dr. Atiqur Rahman Khan
Read full bio of Dr. Ritika Shah
Read full bio of Rebecca Malachi
Read full bio of Ghazia Shah