Image: ShutterStock
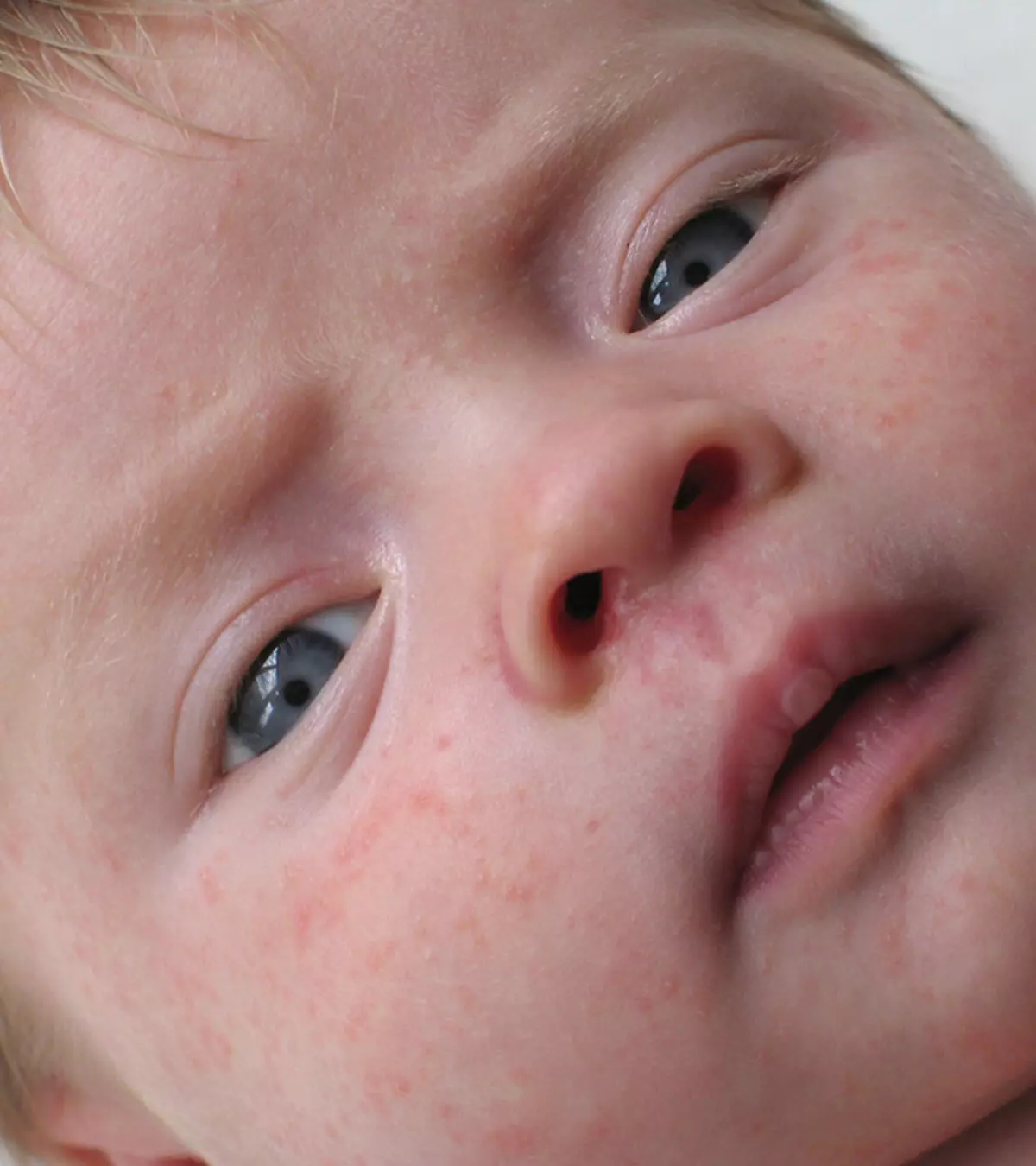
An allergy is defined as a chronic skin condition that occurs due to the immune system’s abnormal response to an allergen or an unknown substance. Skin allergies in babies might be caused due to food, bites, stings, or adverse reactions to medicines (1). The common areas where allergies occur include the nose, skin, eyes, and digestive tract. In newborns, skin allergies usually manifest in the form of rashes, swelling, and itching of the skin (2). Read on to know more about the common skin allergies that can be seen in babies, their causes, symptoms, treatment, and prevention techniques.
Key Pointers
- Eczema is a skin allergy that causes rashes and itching in babies.
- Hives, or urticaria, are skin swellings that can occur anywhere on the body.
- Insect bites cause papular urticaria, which appears as itchy, wheal-like papules.
- Allergic contact dermatitis is a skin response caused by allergen exposure.
- Angioedema is a swelling of deep skin tissues, usually around the eyes or mouth.
- Treatment of skin allergies in babies depends on the specific condition and involves topical creams, medications, and avoiding triggers.
- For prolonged or severe skin allergies, it is best to consult a pediatrician for proper diagnosis and management.
Common Skin Allergies In Babies
Here we have listed some of the common types of skin allergies seen in babies.
- Eczema or atopic dermatitis
- Hives or urticaria
- Papular urticaria
- Contact dermatitis
- Angioedema
Each type of skin allergy has its own causes, medical management, and home remedies. Allergies may not always have a treatment, but there are ways to reduce the symptoms. Recognizing the signs of skin allergies is important for timely and proper intervention.
1. Atopic dermatitis or eczema

This chronic and relapsing inflammatory condition leads to itching and risks of skin infections. The most common parts of the skin to display the condition are the face and skin folds. Eczema affects about 10-20% of children in the US and Western Europe (3).
Symptoms
- Itchiness
- Rashes
- Tiny red bumps on the face, forehead, scalp, and later on the torso (4)
- Dry skin
- Red bumps on the forearm, knees, and ankles in infants who crawl (5)
Causes
- Inhalant allergens: Some allergens are house dust (the most common allergen), grass pollen, and animal dander from pets.
- Skin irritants: A few common skin irritants that trigger allergies are woolens, nylon, acrylic material, excess soap in bubble baths, and heavily perfumed soaps, lotions, etc. (5)
- Food allergens: Less than 10% of babies exhibit a food item as a cause for eczema.
Medical management
The treatment of eczema focuses on the effective management of the condition and avoiding potential triggers. Do not provide any medicine to the baby without consulting the pediatrician.
- Topical corticosteroidsiA group of steroid hormones produced in the adrenal cortex that are used for treatments in synthetic form to reduce inflammation. of different types could be used for the management of eczema.
- Topical immunosuppressantsiDrugs that reduce and control the body's immune response and prevent it from attacking its cells or tissues. could help address the symptoms of eczema, although more research is needed to prove efficacy (6).
- AntihistaminesiMedications that relieve allergic symptoms. at bedtime are commonly prescribed for their sedative action to help relieve itching. More studies are needed to establish the safety and efficacy of antihistamines in babies (5).
- Identifying and eliminating potential food allergens may help reduce eczema symptoms.
However, the use of thick lubricant skin creams (non-medicated) may be useful. Also, avoiding rubbing the skin with a towel to dry it, touching it instead to absorb the water is quite useful.
Pediatrician and neonatologist Dr. Neema Shrestha says, “Regular use of moisturizers to maintain the skin barrier, minimizing hot and long showers, and avoiding exposure to the allergens that exacerbate the condition can help keep the symptoms under control. In case of eczema flares, visit the doctor to assess the need for a topical corticosteroid therapy and antihistamines.”
 Quick fact
Quick fact2. Hives
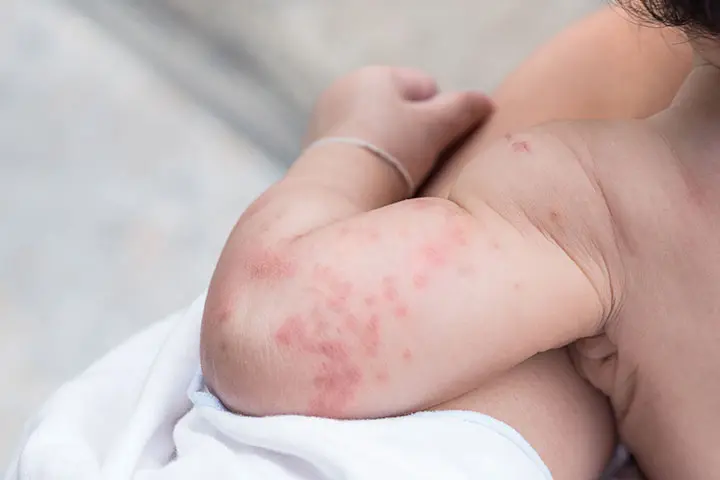
Urticaria, also known as hives, is a type of allergic rash triggered by the release of histamineiA chemical that is released by the immune system to signal between cells and IgE in the body that happens in response to an allergic reaction (7). Hives on baby feature a superficial swelling that can appear on any part of the body.
Symptoms
- Development of lesions, which are bumpy, red, warm, and swollen. These lesions are also called wheals (7).
- Lesions might have a pink or red outline with a pale center (8).
- They might range in size from the diameter of half an inch to several inches.
- They are generally very itchy (9).
Causes
Allergy to one or more of the following items could lead to hives (28).
- Milk
- Shellfish
- Dust mites
- Mold
- Pollen
- Mildew
- Certain foods
- Natural rubber latex
- Pets (pet dander and droppings)
- Medicines such as penicilliniA group of antibiotics that target and destroy infectious bacteria in the body , sulfa drugs, ibuprofen, aspirin, antacidsiMedications for indigestion and heartburn. , eye and ear drops, laxatives, etc. (10)
- Certain viruses might causes hives as well
- Extreme temperatures
- In some cases, there is no clear cause of hives
May, a stay-at-home mom of two, shares her account of her son’s hives outbreak, “Our boy started showing signs of food allergy when he turned ten months old. He came home one day from Grandpa’s with a bad hives breakout. For someone who loves food like he does, the need to be selective on his intake is almost a tragedy. The newest ingredient added to his porridge that day was anchovies, aka Ikan Bilis. We immediately accused these tiny common salt-water forage fish as the culprit.
“We removed anchovies in his diet and continued feeding him his usual Threadfin, which he had been consuming since month eight, by the way. Threadfin was his daily protein consumption, and he enjoyed it, too. Yet, after this episode, he couldn’t stomach Threadfin anymore. Only then did we find out that Threadfin was the guilty party for this awful allergic breakout (i).”
Treatment
Hives are usually self-limiting and do not need extensive medical intervention. The symptoms usually heal by themselves. However, the itch may diminish by exposing the skin to lukewarm water through a bath. Your pediatrician might prescribe topical calamine lotion or oral antihistamines, if necessary.
3. Papular Urticaria
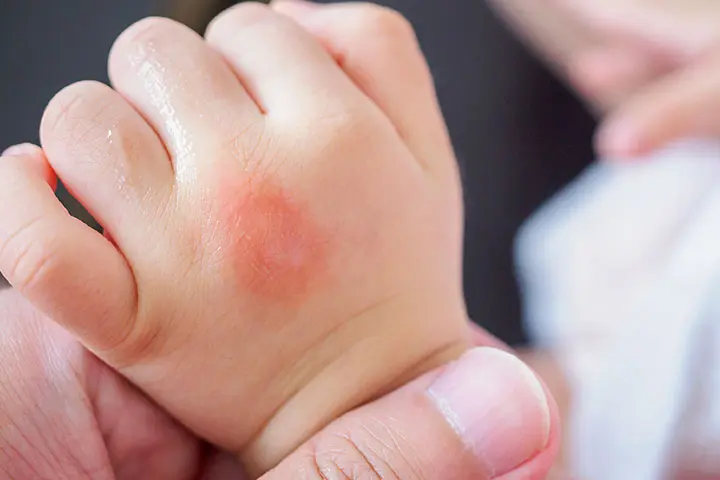
It is a chronic inflammatory disease caused due to insect bites (11). Some common insects whose bites could cause papular urticaria are fleas, bedbugs, flies, mites, and ticks (12). According to the Asthma and Allergy Foundation of America, 5% of the US population is affected by insect allergies, and about 100 people in the US succumb to insect sting anaphylaxis annually.
Symptoms
- Itchy and wheal-like papules on the skin.
- The bumps might usually appear in clusters in a specific area.
- They might be filled with fluid (13).
- Lesions usually disappear in a few minutes or a few hours but, in some cases, may be chronic and recurrent.
Causes
The main cause for the papular urticaria is the body’s hypersensitive reaction to insect bites (13). Checking the baby’s room and crib for potential pests like bedbugs and mites could help identify the insect. In some instances, the use of an appropriate insect repellent (safe for babies) may be useful.
Treatment
Papular urticaria is generally a self-limiting disease, and the symptoms subside eventually. Babies outgrow the disease. For severe itchiness, the doctor might prescribe topical corticosteroids or antihistamines.
4. Allergic contact dermatitis

It is a type of eczema that is triggered by skin contact with an allergen. Its prevalence is highest among babies up to the age of three years (14). Allergic contact dermatitis was earlier uncommon in babies, but there has been an increase in cases due to increased exposure to allergens at a young age (15).
Symptoms
- Mild to severe itchiness at the affected site.
- Red, dry, and scaly skin with visible borders.
- Fluid-filled sacs could also appear (16).
Causes
- Contact with metals like nickel, aluminum, cobalt, mercury, etc. Nickel is the most commonly identified metallic allergen.
- Rubber gloves used by the baby’s doctor or caretaker, while cleaning or examining the baby might also elicit an allergic response (17).
- Fragrances and dyes used in baby products might also be potential allergens.
 Quick fact
Quick factTreatment
- Identification and removal of the allergen.
- Use of a moisturizer.
- Cool water soaks.
- Topical corticosteroids and antihistamines prescribed by a doctor for acute cases with intense irritation (18).
5. Angioedema
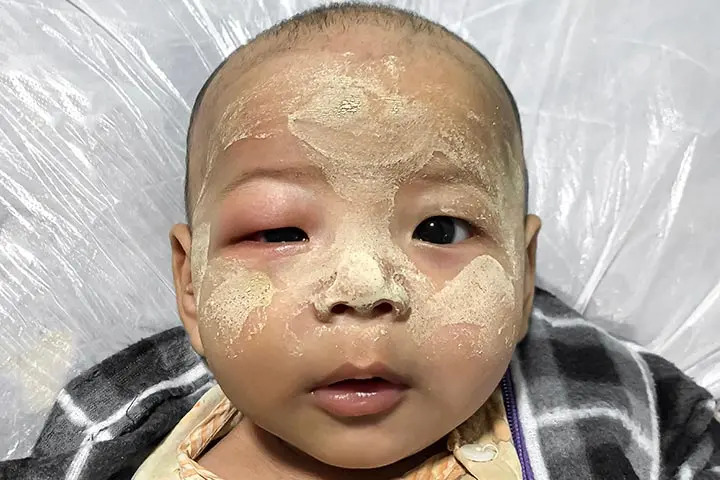
It is an allergic reaction that causes inflammation of deeper layers of the skin. It might occur along with hives or might manifest by itself (19).
Symptoms
- Inflammation can happen anywhere but is most prevalent around eyes, hands, feet, and mouth.
- Stomach cramps might occur.
- Severe cases might cause difficulty in breathing and swallowing due to the swelling of tissues.
Causes
Allergic reactions to one or more of the following might cause angioedema.
- Mold
- Food
- Dandler
- Pollen
- Drugs
- Insect bites
Very rarely, hereditary angioedema (HAE) is also seen. It might cause recurrent and severe allergic reactions, requiring immediate medical intervention. (20)
Management
- Identification and removal of the allergen.
- Regularly changing and washing the baby’s bed sheets, pillow covers, and blankets to get rid of dust.
- Severe cases might require medicines like antihistamines and corticosteroids prescribed by the doctor.
- Home remedies like oatmeal baths and barrier creams containing lanoliniAn oily material derived from sheep's wool possessing antimicrobial properties. or cetomacrogoliA non-greasy moisturizing agent used to heal dry skin problems such as eczema. might help. Consult a doctor before trying any home remedies.
Tips To Prevent Skin Allergies
The following are some ways to avoid skin allergies in babies (21) (27) (28).
- Identify and avoid the allergen to prevent recurrent infections.
- It is also recommended to avoid exposure to foods that have a high potential for allergy in babies. It is good to consult a doctor before introducing foods such as eggs, fish, soy, etc.
- Managing food allergies in babies requires careful monitoring of their reactions. If the baby is confirmed to be allergic to a particular food, then a breastfeeding mother may consider avoiding the food.
- Keep pets and carpets clean to avoid allergies due to fleas and bed bugs.
- Avoid the baby’s exposure to metals like nickel, to avoid allergic contact dermatitis.
- Keep a food diary to track any allergic reactions and identify potential food allergens.
- Clean your home regularly to maintain a dust-free environment.
- Wash your baby’s clothes with hypoallergenic detergents to prevent irritation.
- Discuss with the pediatrician if you can keep any emergency medicines at home as a response to allergic reactions.
- Change your baby’s diapers frequently and keep the area dry to prevent rashes from wetness. Also, frequently apply a zinc-oxide-based ointment or petroleum jelly to the baby’s skin.
- Bathe the baby in warm water and moisturize to prevent skin dryness and sensitivity to infections.
- Avoid using perfumed soaps, shampoos, oils, and other products on the baby’s skin.
- Keep the child in a less humid and cooler environment.
- Avoid using talc or heavy creams that may block the baby’s pores.
- Cut the baby’s nails regularly to keep them from scratching their rashes.
- Observe care with public accessories such as high chairs at restaurants, shopping carts, and hotel bedding as these may have traces of potential allergens.
In this context, a mother Irene C shares about the precautions she takes for preventing eczema and writes, “We avoided giving Ryken any dairy or any new major allergens. After months of being careful, I had realized that dairy is everywhere — in all sorts of processed foods and also in little tikes’ hands (as milk, cheese, crackers) as they played, sat for storytimes, or accompanied their parents on errands. Ryken would sometimes develop random hives on his face while we were out shopping or in another public place. I became very careful about pre-wiping the surfaces for shopping carts, restaurant tabletops, and public play areas to minimize possible reactions (ii).”
When To See A Doctor
It is good to see a doctor when you notice symptoms, and you suspect the baby has a skin allergy. The doctor may recommend an epinephrine auto-injector to keep handy for anaphylactic shock, a condition where the baby has a severe allergic reaction.
 Point to consider
Point to considerCertain allergies, like hives, might be mild and occasional, seldom requiring prompt medical attention. However, if the condition occurs repeatedly or sustains for more than six weeks, then you must take the baby to a doctor (9).
Frequently Asked Questions
1. How long do allergic rashes last in babies?
Allergic rashes in babies, such as hives (urticaria), last for a short time and can be treated with anti-allergy medicines (anti-histamines) (22). Mild cases of allergic contact dermatitis usually self-resolve in a few days or weeks (23).
2. Is petroleum jelly (Vaseline) good for allergic rash in babies?
You may use petroleum jelly to soothe dry, itchy rashes in skin allergy cases, such as atopic dermatitis or diaper dermatitis (baby diaper rash) (24). However, do consult the doctor first since petroleum jelly may not be suitable for all types of allergic rashes.
3. How can I tell the difference between eczema and allergies in babies?
Dr. Shrestha opines, “Allergy is a broad term used to define an immune response by the body to any substance (allergen) that is usually harmless to other people. The allergens may be the substances found regularly in the environment, such as dust, pollen, ticks/mites, pets, and certain food items. Eczema or atopic dermatitis is an inflammatory skin condition characterized by redness, pruritus, and oozing rash that comes and goes, resulting in dry and sensitive skin.”
Skin allergies in babies are not uncommon but may require medical attention if their frequency or severity increases. Allergies such as eczema, hives, papular urticaria, contact dermatitis, or angioedema may be triggered if the baby comes in contact with allergens such as dust, pollen, pet dander, insect bites, some metals, baby-care products, food, or even clothes. Babies may show reduced signs of allergy as they grow. Until then, identifying the allergen may help prevent subsequent episodes of allergy. However, you should see a doctor before treating your baby with over-the-counter topical or oral anti-allergy medications.
Infographic: Reducing Allergens At Home
You can reduce your child’s risk of developing allergies by allergy-proofing your house. Save this infographic to know the steps you can take to have an allergen-free abode. Illustration: Momjunction Design Team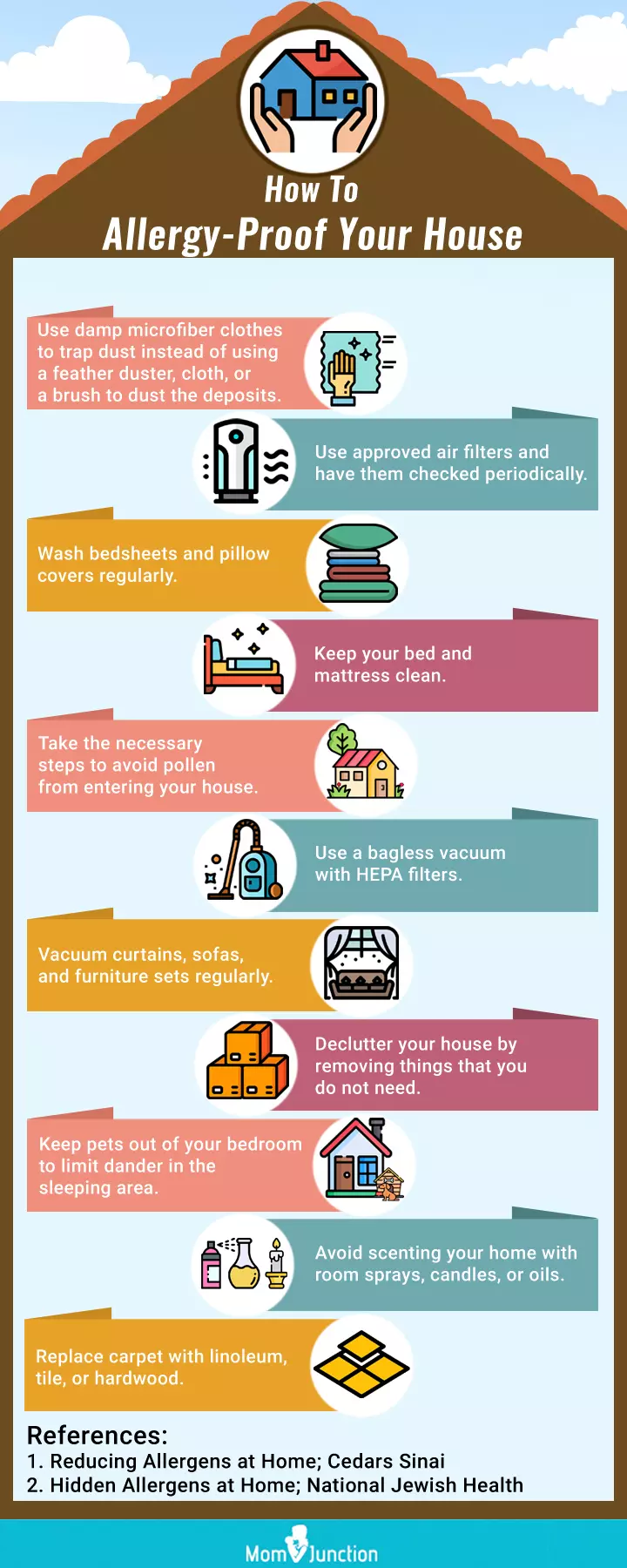
Illustration: Types Of Skin Allergies In Babies Treatment & Prevention

Image: Dall·E/MomJunction Design Team
Personal Experience: Source
MomJunction articles include first-hand experiences to provide you with better insights through real-life narratives. Here are the sources of personal accounts referenced in this article.
i. Away with swells and hives.https://mmlittlee.blogspot.com/2013/10/away-with-swells-and-hives.html
ii. Raising food allergic kids in a mostly non-allergic world, Ryken.
https://getallergywise.blogspot.com/2011/02/when-ryken-was-first-born-my-husband_03.html
References
1. Allergies in Children; Cedars Sinai
2. Skin Allergies; Asthma and Allergy Foundation of America
3. Megan A. Moreno,Atopic Diseases in Children; Journal of JAMA Pediatrics
4. Jocelyn M. Biagini and Gurjit K. Khurana Hershey,Eczema in early life: Genetics, the skin barrier, and lessons learned from birth cohort studies; The Journal of Pediatrics.
5. Ross St C Barnetson and Maureen Rogers; Childhood atopic eczema; The BMJ.
6. Alan B. Fleischer Jr.,Treatment of atopic dermatitis: Role of tacrolimus ointment as a topical noncorticosteroidal therapy; The Journal Of Allergy and Clinical Immunology.
7. Meeyong Shin and Sooyoung Lee,Prevalence and Causes of Childhood Urticaria; Allergy, Asthma and Immunology Research.
8. Hives; American Academy of Pediatrics
9. S J Deacock,An approach to the patient with urticaria; Clinical and experimental Immunology.
10. Hives, Children’s Hospital of Philadelphia
11. Evelyne Halpertet al.,Prevalence of papularurticaria caused by flea bites and associated factors in children 1–6 years of age in Bogotá, D.C.;The World Allergy Organization Journal
12. Sanjay Singh and Baldeep Kaur Mann; Insect bite reactions; Indian Journal of Dermatology, Venereology and Leprology
13. Papular Urticaria; Primary Care Dermatology Society
14. Paolo Pigattoet al.; Contact dermatitis in children; Italian Journal of Pediatrics
15. Yasmeen JabeenBhat, Saniya Akhtar, and Iffat Hassan,Contact dermatitis in pediatric age group: Indian scenario; Indian Journal of Pediatric Dermatology
16. Richard P. Usatineand Marcela Riojas; Diagnosis and Management of Contact Dermatitis; American Family Physician
17. Taru Garget al.,Allergic contact dermatitis in children: Culpable factors, diagnosis and management; Gale Academic OneFile
18. Patrick B. Murphy et al.,Allergic Contact Dermatitis; National Center for Biotechnology Information
19. Hives and Swelling; Riley Children’s Health
20. Giuliana Ferranteet al.,The care pathway for children with urticaria, angioedema, mastocytosis; The World Allergy Organization Journal
21. Zave Chad,Allergies in children; NiDirect
22. Skin rashes in babies; Journal of Pediatrics Child Health
23. Red, Itchy Rash?; National Institute Of Health
24. Atopic dermatitis; Mount Sinai
25. HOW TO TREAT ECZEMA IN BABIES; American Academy of Dermatology Association
26. Contact Dermatitis in Children; Stanford Medicine
27. Hives; Seattle Children’s
28. Urticaria (Hives) in Children; Cedars Sinai
Community Experiences
Join the conversation and become a part of our nurturing community! Share your stories, experiences, and insights to connect with fellow parents.
Read full bio of Dr. Miguel Ángel Guagnelli Martínez
- Dr. Neema Shrestha is a pediatrician with a special interest in the field of neonatology. She completed her graduation in medicine at Kasturba Medical College, Diploma in Child Health at D.Y. Patil University, post graduation in Pediatrics at Nepal Medical College and Fellowship in Neonatology at Sir Ganga Ram Hospital, New Delhi. Dr. Shrestha has an overall experience of five years and currently works at NICU in Grande International Hospital, Kathmandu, Nepal.
 Dr. Neema Shrestha is a pediatrician with a special interest in the field of neonatology. She completed her graduation in medicine at Kasturba Medical College, Diploma in Child Health at D.Y. Patil University, post graduation in Pediatrics at Nepal Medical College and Fellowship in Neonatology at Sir Ganga Ram Hospital, New Delhi. Dr. Shrestha has an overall experience of five years and currently works at NICU in Grande International Hospital, Kathmandu, Nepal.
Dr. Neema Shrestha is a pediatrician with a special interest in the field of neonatology. She completed her graduation in medicine at Kasturba Medical College, Diploma in Child Health at D.Y. Patil University, post graduation in Pediatrics at Nepal Medical College and Fellowship in Neonatology at Sir Ganga Ram Hospital, New Delhi. Dr. Shrestha has an overall experience of five years and currently works at NICU in Grande International Hospital, Kathmandu, Nepal.
Read full bio of Dr. Ritika Shah
Read full bio of Rohit Garoo
Read full bio of Shinta Liz Sunny