Image: Shutterstock
Meningitis is a neurological disease that causes inflammation in the membrane covering the brain and spinal cord. Meningitis in toddlers can be caused by viruses, bacteria, fungi, or parasites. If this condition is not treated on time, it could result in alarming symptoms and long-lasting complications.

Therefore, early detection of the symptoms is important to begin the treatment promptly. Moreover, you should follow preventive measures to keep your children safe from this disease.
Read the post for more information on meningitis, including its causes, symptoms, complications, diagnosis, and treatment options.
Key Pointers
- Meningitis is the inflammation of the meninges membrane that encloses the brain and spinal cord.
- The condition is caused by different types of pathogens such as viral, bacterial, fungal, and parasitic.
- Toddlers can contract meningitis by inhaling droplets from an infected person, touching contaminated surfaces, or sharing utensils with an infected person.
- Meningitis in toddlers can also be caused by certain drug reactions, brain injury, brain surgery, cancer, and autoimmune diseases.
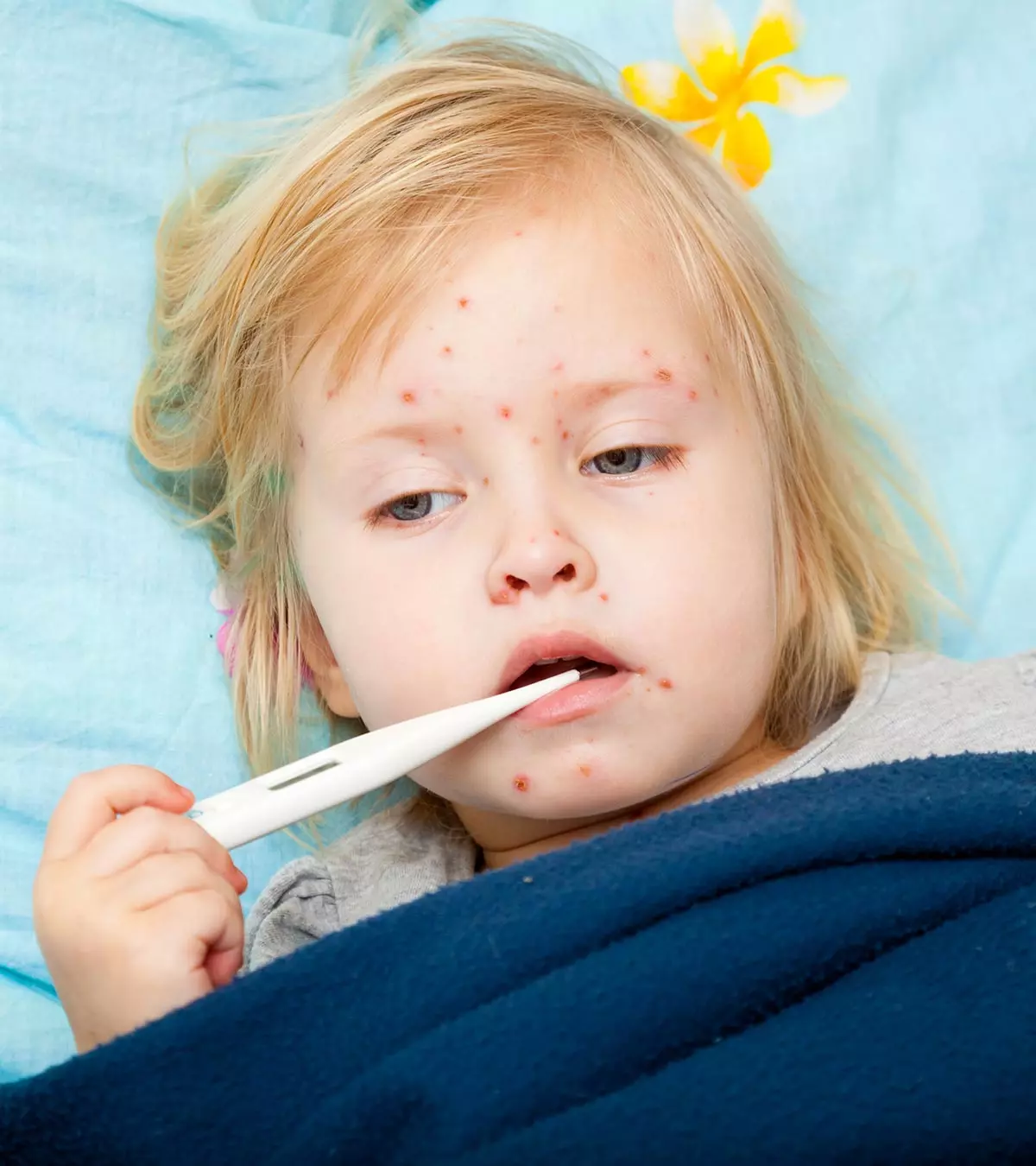
- Symptoms of meningitis in toddlers include high fever, vomiting, bulging soft spot, lack of appetite/thirst, sleepiness, stiff neck, and rash.
What Is Meningitis?
Meningitis is the acute inflammation (swelling) of the membrane called meninges that covers the brain and the spinal cord. The swelling results from an infection caused by a pathogen, which affects the meninges. The swollen meninges interfere with the functions of the brain and spinal cord, making meningitis a central nervous system disease (1). Let’s take a look at the causes of meningitis.
What Causes Meningitis In Toddlers?
There is no single cause for the disease, and there are many pathogens that can lead to it. Meningitis can be classified based on the cause of the condition.
1. Viral meningitis
It is the leading cause of meningitis among toddlers, but less severe than bacterial meningitis. Milder forms of viral meningitis resolve without treatment, and there are several viruses that infect meninges, causing the problem. Following are the most common ones (2):
- Non-polio enteroviruses
- Herpes virus
- Varicella-zoster virus (chickenpox and shingles virus)
- Mumps virus
- Influenza virus
- Measles virus
- West Nile virus
- Lymphocytic choriomeningitis virus
2. Bacterial meningitis
Bacterial meningitis is less common than viral meningitis, but is more severe and disabling. A severe central nervous system infection could be fatal or cause damage to certain parts of the brain among those who survive. The most common bacteria that cause bacterial meningitis are (3):
- Streptococcus pneumoniae (pneumonia bacteria)
- Neisseria meningitidis causing meningococcal disease (also called meningococcus) According to the Centers for Disease Contol and Prevention, Serogroups B Neisseria meningitides is the most common cause of meningococcus in the US, with a prevalence rate of 60% among children and young adults who are under 24.
- Group B Streptococcus (strep bacteria)
- Type B Haemophilus influenzae (causes meningitis type b)
- Listeria monocytogenes (also causes gastroenteritis)
3. Fungal meningitis
It is caused by fungus, which spreads from the bloodstream into the cerebrospinal fluid or brain/spinal cord tissue. The fungus enters the bloodstream through a cut in the body. This happens when the toddler already suffers from a fungal infection such as that of the skin. Fungal meningitis is rare and most common in toddlers with a suppressed immune system such as those suffering from cancers and HIV. This form of meningitis is non-contagious (4). Some of the common fungi that cause fungal meningitis are:
- Cryptococcus (most common cause of fungal meningitis)
- Candida (yeast fungus)
- Histoplasma (found in bird and bat droppings)
- Blastomyces (found in decaying organic matter)
- Coccidioides (naturally found in soil)
4. Parasitic meningitis
Some parasites cause meningitis as a collateral effect of their invasion of the central nervous system. Parasitic meningitis is highly incidental and only occurs when a person ingests the parasite, its eggs, or active larvae. Just three parasites have been associated with meningitis (5):
- Angiostrongylus cantonensis (a type of roundworm)
- Gnathostoma spinigerum (a parasite common in tropical climate)
- Baylisascaris procyonis (also called raccoon roundworm)
5. Non-infectious meningitis
When meningitis happens as an indirect result of a condition, then it is called non-infectious meningitis. The following cases have been associated with this type of meningitis (6):
- Drug reaction
- Brain injury
- Brain surgery
- Cancer
- Autoimmune diseases
Non-infectious meningitis can be chronic, which means it can come and go regardless of treatment (7). These cases can go on for a long duration, ranging from months to years.
How Does A Toddler Get Meningitis?
A toddler can get meningitis if he contracts a bacteria, virus, or parasite. The pathogen’s primary target could be another organ, such as lungs in pneumonia, but it would eventually find its way into the nervous system (generally through the blood stream) causing meningitis. Following are the scenarios that can lead to meningitis in toddlers (8):
- Sneeze and cough of an infected person releases hundreds of tiny droplets of mucus and saliva into the air. Inhaling these droplets can spread the bacteria and virus to the bloodstream and then to the brain. The pathogens cause meningitis.
- Touching any contaminated surfaces such as doorknobs, toilet seats, toys, and floor can transfer the microbes from these surfaces to the toddler. Poor personal hygiene can exacerbate the contraction of the pathogen from inanimate objects.

- Sharing utensils with an infected person while eating and drinking can spread infections. Toddlers can be susceptible to it at playschools and daycare where preschoolers could eat snacks from the same plate.
- Eating contaminated food transmits bacteria, virus, and parasites, which are potential agents for meningitis infection.
- Breathing contaminated dust with fecal matter of bats and birds may contain spores of fungi that could cause meningitis.
- Overall poor hygiene, such as not washing hands, playing in contaminated soil, and not covering the mouth while coughing and sneezing increase the risk of developing meningitis.

- Head injury, cancers, autoimmune diseases such as allergies, certain types of tumors in the brain, can all cause inflammation of the meninges.
While any toddler can be at risk of getting meningitis, some are more susceptible than others.
 Be watchful
Be watchfulWhat Are The Risk Factors For Contracting Meningitis?
The following conditions can increase the risk of meningitis among toddlers (9) (10):
- Immunodeficient toddlers, who suffer from diseases such as cancers, HIV, sickle cell anemia or immunoglobulin deficiency are at a higher risk of meningitis due to the weak immune system.
- Toddlers who have deformities and defects in the nervous system, and those who develop spontaneous defects such as a cerebrospinal fluid leak are at a higher risk.
- Recurrent sinus infections increase the risk of meningitis. It is not known what exactly causes it, but it could be due to the proximity of the sinuses to the eye from where the bacteria can travel upwards to the brain through the optic nerve.
- Brain injury and skull fracture or open concussion expose the brain to pathogens that can cause meningitis.
- Toddlers who undergo brain surgery, or toddlers with cochlear implants for hearing and shunt insertioniA surgical procedure where a small tube (shunt) is placed in the brain to drain excess cerebrospinal fluid in the brain are at a greater risk since such devices are prone to accidental bacterial contamination.
- Toddlers in overcrowded setups, such as in playschools, daycare or other similar environments, are at a higher risk of contracting meningitis.
These risks can evolve into complications and may bring other problems in the toddler’s health.
What Are The Complications Of Meningitis In Toddlers?
Untreated meningitis can lead to the following complications in toddlers (10).
- Neurological complications, such as cerebral palsy and repeated fits
- Intellectual problems such as having low IQ, attention deficit and hyperactivity disorder (ADHD)iA chronic condition of childhood characterized by inattentiveness, hyperactivity, and impulsive behaviors , and limited cognitive abilities.
- Chronic weakness, fatigue, and lethargy
- Problems ranging from a permanent blurred vision to blindness in one eye
- Hearing problems
- Acute headache, with bouts of dull and sharp pain in the head like a migraine
- Poor limb coordination that hampers precision in movements like those needed during running or walking. It hampers the toddler’s ability to participate in sports or vigorous outdoor activities.
- Sepsis, also called septicemia and blood poisoning, is an overwhelming immune response to bacteria that causes meningitis (11). Sepsis also multiplies the intensity of meningitis’ symptoms. The complication is most likely to occur in younger toddlers and those suffering from a severe infection. The condition is fatal with 50% of meningitis-induced sepsis cases leading to death (12)
Around one in five people with bacterial meningitis may develop long-lasting side-effects (13). Viral meningitis survivors fare better and suffer only from a chronic headache and weakness. Nevertheless, the condition can be spotted for immediate treatment.
What Are The Symptoms Of Meningitis In Toddlers?
A toddler with meningitis will display the following symptoms (14):
- The toddler has a fever with a body temperature higher than 100.4°F (38°C) (15)
- The toddler’s cries become abnormally high-pitched in their tone with grunts in between. A high-pitched cry, along with a fever, is among the early signs of meningitis in toddlers.
- Repeated bouts of vomiting are accompanied by a constant sensation of nausea.
- Younger toddlers display a bulge in the fontanelle, which is a soft spot right at the center of the top section of the skull.
- The toddler’s appetite is affected with a general disinterest in food. They will also refuse to drink water due to diminished thirst.
- The baby will be excessively fussy and irritated.
- The toddler will have a constant pain that radiates across the head.
- The toddler lacks energy, feels excessively lazy, and sleeps a lot more than usual. Sleepiness would be so acute that it may be difficult to wake the baby up.
- Neck muscles would tighten, leaving the toddler with a stiff neck so much that the neck does not flex at all. Younger toddlers tend to have stiffness in other body muscles, especially those of limbs.
- Red blisters and patches form on parts of the body. However, this symptom is limited to bacterial meningitis in toddlers.
- Sensitivity to light, also called photophobia, is a general irritability towards light including natural sunlight. The toddler with meningitis would prefer the windows curtained and lights turned off.
- The toddler seems visibly delirious and has limited levels of consciousness. In severe cases, the toddler would be in a state of absolute unresponsiveness.
- Toddlers may also have fits and seizures as a symptom of meningitis.
Parents may not relate meningitis to these symptoms as they could overlap with several other conditions. Therefore, taking the toddler to a doctor immediately is imperative when you spot any of the above symptoms.
How Is Meningitis In Toddlers Diagnosed?
Neck rigidity (Kernig’s sign) is one of the diagnostic signs. The doctor uses one or more of the following methods (8):
- Blood test determines the presence of infectious meningitis pathogens in the blood.
- Stool and urine samples are collected to detect the presence of a pathogen. A stool test is especially useful in identifying parasitic meningitis.
- Computed tomography scan or CT scan uses multiple X-rays of the head to detect inflammation. Magnetic resonance imaging or MRI may also be used to determine the extent of infection in the meninges accurately.
- Lumbar tap, also called spinal tap, is a cerebrospinal fluid analysis; in the test, the fluid is extracted from the lower section of the spinal cord. The fluid is sent for laboratory analysis to check for anomalies. Lumbar tap is quite invasive and could be preferred when other tests do not yield a conclusive diagnosis. It is useful in cases where there is a suspicion of sepsis (16). Spinal tap also helps in identifying the pathogen responsible for causing meningitis.
The treatment methods are based on the final analysis and could vary as per the severity of the condition.
How Is Meningitis In Toddlers Treated?
The treatment is determined by the type of meningitis. Most forms of viral meningitis have no specific treatment, and the infection usually resolves in ten days. The only exception is herpes virus related meningitis, which is treated with acyclovir injections. The other kinds of meningitis do require extensive therapy through medication (8):
- Bacterial meningitis is treated with a combination of several antibiotics, including those administered intravenously. The doctor prescribes a treatment course, and the toddler must attend all the IV therapy sessions. Oral antibiotic therapy is prescribed for taking at home.
 Quick tip
Quick tip- High concentration antifungal and antiparasitic medicines treat fungal and parasitic meningitis respectively. These drugs are directly diffused into the bloodstream through intravenous administration.
- Antiviral medicines are needed in cases of viral meningitis caused by herpes and influenza virus since they cannot be overpowered by the immune system alone.
- Corticosteroids are prescribed to reduce the inflammation of the meninges. Anti-epileptic drugs are given when the toddler suffers from seizures and fits as a result of meningitis (15).
- Antihistamine treatment is useful in non-infectious meningitis caused by autoimmune diseasesiA group of medical conditions where the body’s immune system erroneously attacks healthy cells such as allergies (16).Despite complete recovery, a toddler may have to visit a doctor for any remnant effects of meningitis.
Are There Any After-Effects Of Meningitis?
The effects of meningitis may take time to taper away after treatment. As a result, the toddler may display mild after-effects (17):
- Lethargy and tiredness
- Frequent headaches
- Problems in concentration
- Brief short-term memory loss
- Difficulties in body balance and general clumsiness
- Hearing problems
- Mood swings and sudden tantrums
- Paralysis of the limbs or hemiplegia
- Vision difficulties
Therefore, follow-up care is essential after treating meningitis in toddlers to monitor their recovery. A pediatrician will frequently review the condition of the toddler to ensure these after-effects do not hinder healthy growth.
 Point to consider
Point to considerHow To Prevent Meningitis In Toddlers?
Despite being a critical illness, meningitis can be easily prevented through some simple preventive measures (8):
- The US Center for Disease Control & Prevention (CDC) and the American Academy of Paediatrics (AAP) recommend immunization against bacterial infections. Vaccines against meningitis bacteria are type b Haemophilus influenzae (causes type b meningitis), Streptococcus pneumoniae (pneumonia bacteria), and Neisseria meningitidis (also called meningococcus) (18) (19) (20). Vaccinations can protect against a dozen and more strains of bacteria. Each vaccine has its dosage and immunization schedule, which is determined by the doctor after considering the toddler’s age. Parents need to stick to the schedule to ensure complete immunity.
- Washing hands is a single personal hygiene measure to prevent a host of diseases including meningitis. Teach the toddler the good habit of washing hands before eating, after using the toilet, and returning from outdoors.
- Never share utensils as that spreads bacteria from one person to another. Parents and other caretakers may tend to feed toddlers from the same plate but do not do that! The toddler may invariably come in contact with bacteria that would be dormant in adults but may have adverse effects in toddlers.
- Consuming hygienically-prepared, well-cooked food prevents the spread of parasites that can lead to parasitic meningitis.

- Avoid dusty environments. Fungal meningitis often occurs due to inhalation of soil and dust particles contaminated with bird droppings. Hence, it is best for the toddler to stay indoors when the air outside is excessively dusty.
Frequently Asked Questions
1. What does the onset of meningitis look like?
According to the Meningitis Research Foundation, fever, headache, vomiting, and nausea are the first symptoms of meningitis (14). However, the early symptoms may vary from one child to another. Thus, you should pay close attention to the symptoms and act promptly.
2. How quickly does meningitis progress?
Meningitis in children has different types based on which its progress varies. For instance, the onset of bacterial meningitis is fast, and the symptoms may appear within 24 hours. On the other hand, viral meningitis progresses gradually, and the symptoms usually appear three to six days after the baby is exposed to the virus (21) (22).
3. Can toddlers recover from meningitis?
According to the WHO, “meningitis is a devastating disease with a high case fatality rate and leading to serious long-term complications (9).” However, with early diagnosis and prompt treatment of pediatric meningitis, babies or toddlers have a reasonable chance of recovery (9).
4. How often should toddlers be vaccinated against meningitis?
There are various types of meningitis vaccines that target the specific causes. The vaccine recommended would depend on the prevalent vaccine in your country or the one recommended by your toddler’s pediatrician. These vaccines are administered to babies and toddlers across various doses. The first dose may be administered as early as when the baby is six weeks old, with a second dose when the baby is older. A booster shot is often administered when the child is at least a year old (23).
Meningitis in toddlers can either be caused due to a virus, bacteria, or fungi. Toddlers are usually affected by this disease after coming in contact with contaminated surfaces or food. Although immunodeficient toddlers are at a higher risk of contracting this disease, maintaining proper hygiene and immunization can help prevent the chances of contracting it. Antifungal or antiparasitic medications are the most common treatment measures used to treat this condition. Contact your healthcare provider immediately if you notice signs of complications such as chronic weakness, poor coordination between hands and limbs, or hearing problems.
Infographic: Differential Diagnosis Of Meningococcal Meningitis
Meningococcal meningitis is a form of bacterial meningitis which commonly affects infants and children. However, its symptoms may be similar to some other conditions too. Read this infographic to learn more about these conditions. Illustration: Momjunction Design Team
Illustration: Symptoms Of Meningitis In Toddlers Risks And Treatment

Image: Dall·E/MomJunction Design Team
In this insightful video, you will gain valuable information about identifying meningitis in kids. Explore the distinctive symptoms and understand the vital measures for swiftly seeking proper medical help.
References
- Meningitis.
https://kidshealth.org/en/parents/meningitis.html - About Viral Meningitis.
https://www.cdc.gov/meningitis/about/viral-meningitis.html?CDC_AAref_Val=https://www.cdc.gov/meningitis/viral.html - About Bacterial Meningitis.
https://www.cdc.gov/meningitis/about/bacterial-meningitis.html?CDC_AAref_Val=https://www.cdc.gov/meningitis/bacterial.html - Fungal meningitis.
https://www.meningitis.org/fungal-meningitis#:~:text=This%20is%20the%20fungus%20which - About Parasitic Meningitis.
https://www.cdc.gov/meningitis/about/parasitic-meningitis.html?CDC_AAref_Val=https://www.cdc.gov/meningitis/parasitic.html - Meningitis.
https://my.clevelandclinic.org/health/diseases/14600-meningitis - P.K. Coyle; (1999); OVERVIEW OF ACUTE AND CHRONIC MENINGITIS.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7132757/ - Meningitis in Children.
https://www.stanfordchildrens.org/en/topic/default?id=meningitis-in-children-90-P02528 - Meningitis in Infants and Children.
https://www.healthychildren.org/English/health-issues/conditions/head-neck-nervous-system/Pages/Meningitis.aspx - Bacterial Meningitis.
https://pedclerk.uchicago.edu/ - Meningitis.
https://www.sepsis.org/sepsisand/meningitis/ - Septicemia.
https://www.hopkinsmedicine.org/health/conditions-and-diseases/septicemia - Meningitis.
https://www.who.int/news-room/fact-sheets/detail/meningitis - Meningitis and septicaemia – higher risk for young children.
https://www.meningitis.org/meningitis/check-symptoms/toddlers - Signs and Symptoms of Fever.
https://www.healthychildren.org/English/health-issues/conditions/fever/Pages/Signs-and-Symptoms-of-Fever.aspx - Lumbar Puncture.
https://www.hopkinsmedicine.org/health/treatment-tests-and-therapies/lumbar-puncture - Meningitis.
https://www.rch.org.au/kidsinfo/fact_sheets/Meningitis/ - Haemophilus Influenzae Type B (Hib) Vaccine: What You Need to Know.
https://www.healthychildren.org/english/safety-prevention/immunizations/pages/Haemophilus-Influenzae-TypeB-Hib-Vaccine-What-You-Need-to-Know.aspx - Pneumococcal Conjugate Vaccine: What You Need to Know.
https://www.healthychildren.org/english/safety-prevention/immunizations/pages/Pneumococcal-Conjugate-Vaccine-What-You-Need-to-Know.aspx - Meningococcal ACWY Vaccines: What You Need to Know (VIS).
https://www.healthychildren.org/English/safety-prevention/immunizations/Pages/Meningococcal-Vaccines-What-You-Need-to-Know.aspx - Bacterial Meningitis.
https://my.clevelandclinic.org/health/diseases/11039-bacterial-meningitis - Viral Meningitis- FAQ.
https://oeps.wv.gov/aseptic_meningitis/documents/community/aseptic_meningitis_faq_public.pdf - Vaccination. Meningitis.
https://www.nhs.uk/conditions/meningitis/vaccination/
Community Experiences
Join the conversation and become a part of our nurturing community! Share your stories, experiences, and insights to connect with fellow parents.
Read full bio of Dr. Mubina Agboatwalla
Read full bio of Rohit Garoo
Read full bio of Dr. Ritika Shah
Read full bio of Vidya Tadapatri