Image: Shutterstock
An anomaly scan, also known as an anatomy scan, level 2 ultrasound, or 20-week ultrasound, looks for anatomic structures of the fetus, placenta, and maternal organs. Routine prenatal checkups and diagnostic assessments are necessary, as they show the baby’s health status. Some prenatal tests can be challenging, while a few, such as seeing your baby on-screen or listening to their heartbeat, can be unforgettable experiences.

Read on to know when the anomaly scan is performed and its significance in prenatal care.
Key Pointers
- A 20th-week or mid-pregnancy scan, commonly known as an abnormality scan, is a complete morphological ultrasound study.
- The objective of an anomaly scan is to detect any anomalies in fetal development or congenital defects.
- If the scan was unclear due to the unfavorable fetal position or the mother’s thick skin tissue, a repeat scan around the 23rd week could be done.
What Is Anomaly Scan?

The Anomaly scan is a detailed morphology ultrasound scan, also known as 20th-week scan or mid-pregnancy scan, and is carried out between the 18th and 21st weeks of pregnancy (1). In some cases, it is also done after you are 21 weeks pregnant. It checks if the fetus is growing normally and has any congenital abnormalitiesiA wide variety of birth defects with prenatal roots that affect body structure or function . That said, it cannot detect every problem (2).
The primary purpose is to monitor fetal development.
Is It Necessary To Have An Anomaly Scan?
All women, irrespective of their age, carry a little risk of delivering babies with physical and mental anomalies. The anomaly scan helps to find or rule out such abnormalities (3).
What Does It Look For?

Just like the pregnancy ultrasound scan, the anomaly scan determines the following (4):
- Size, growth, maturity and general health of the baby
- Examines all the fetal organs, stomach, and abdominal wall
- Gestational age
It may also be helpful in screening congenital abnormalities including (5):
- Anencephaly
- Cleft lipiA separation in the upper lip of a baby caused due to improper development of the fetus during early pregnancy or palate
- Spina bifida
- Congenital heart disease
- Down syndrome
- Edward’s syndrome
- Patau’s syndrome
Cardiac abnormalities could be missed around the 20th week, but a repeat scan for fetal echocardiographyiA type of ultrasound examination done during the second trimester to detect heart problems in the baby before birth around the 24th week determines the cardiac structures in detail
.
Most of the time, the scan shows normal development of the baby, and only a sonographer can detect the problem if any.
 Point to consider
Point to considerHow To Prepare For An Anomaly Scan?

The anomaly scan is a normal procedure that requires no special preparations. Some tips could make the scan comfortable, quick, and efficient for you.
- Relax before the scan and reach the diagnostics center early to make yourself comfortable.
- You should have a full bladder as the scan cannot give accurate results when performed on an empty bladder. Wait until the bladder is full.
- During the scan, you will need to expose your abdomen from the navel to pubic bone. Therefore, wear some loose clothing that is easily adjustable.
- Do not wear any ornaments or accessories on your body during the scan.
- Take all your reports and medical records while going to the diagnostic center.
- Consider bringing a partner or support person for comfort and to ease anxiety.
Keep reading to know the exact procedure.
How Is The Anomaly Scan Done?
It is carried out by a specially trained sonographer in a dimly lit room to get good images of the baby (5).
- The sonographer will apply a water-based gel on your abdomen to begin the procedure.
- A handheld probe is run over the tummy to examine the fetal body. The probe collects the sound waves and creates a sonogram (or image) of your baby on the ultrasound screen.
- The sonographer may apply a little pressure on the tummy for the best view of the baby. It might be a bit uncomfortable, but it will not hurt the baby.
- The scan takes around 30 minutes, and the sonographer will show you and talk to you about the different parts of the baby as well as the baby’s heartbeat.
Sometimes you may not get a clear picture if the fetus is lying in an awkward position or moving around a lot, or if your body tissue is dense or you are obese.
What Does The Anomaly Scan Show?
The main purpose of the scan is to check if the baby is developing without any abnormalities. The sonographer will look for the following (6):
- Shape and structure of the baby’s head and brain. At this stage, severe brain problems are identified.
- Face, to spot cleft lip although it is difficult to see it clearly.
- The spine, along its length and cross-section, to check if the bones are aligned properly and if the skin is covering the back properly.
- Abdominal wall to check if all the internal organs are covered in the front.
- Heart, if its top two chambers (atria) and bottom two chambers (ventricles) are equal in size, the major veins and arteries that carry blood, vales that open and close with each heartbeat.
- Stomach, as baby consumes some amniotic fluid. The scan shows it as a black bubble.
- Kidneys, to check if there are two, and urine freely flows through the bladder. Even if the baby’s bladder is empty, it fills up as you take water before the scan, and the little one urinates every half an hour around this period.
- Hands, arms, legs, and feet along with fingers and toes.
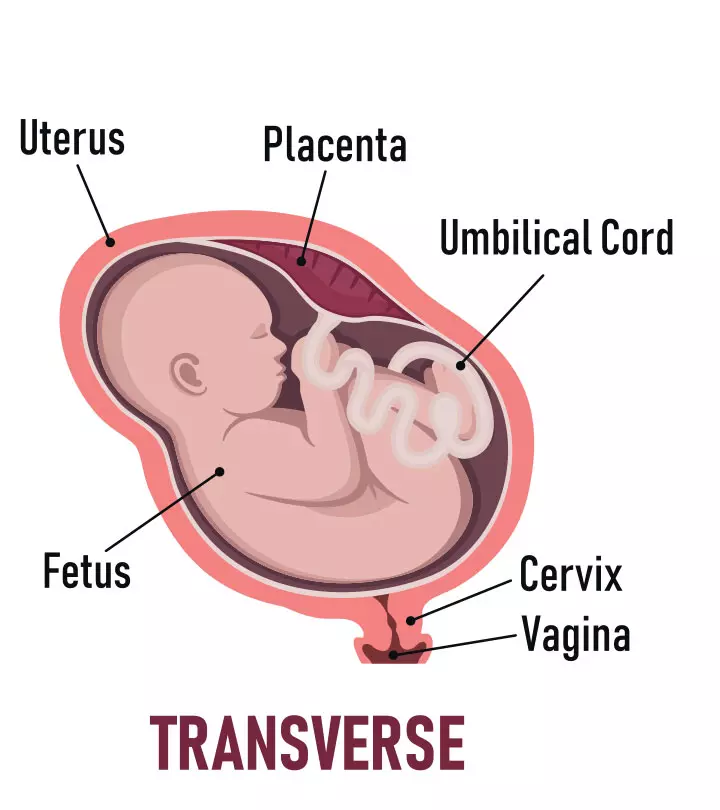
- The position of the placenta.
- Blood vessels of the umbilical cord to check if enough blood is flowing through it.
- If there is enough amniotic fluid for the baby to move freely.
The sonographer also takes anomaly scan measurements to determine the:
- Head circumference (HC)
- Abdominal circumference (AC)
- Length of the humerus or arm bone
- Length of the femur or thigh bone
The measurements should be similar to what is expected for your baby around that week. It also depends on the due date that is established as per the dating scan. In case it is your first scan, it is also helpful in determining the due date. In addition to this, the scan may also be able to detect some anomalies. If abnormalities are found during the scan, your healthcare provider may suggest further testing or consultations with specialists.
 Quick fact
Quick factWhat Abnormalities Can Be Detected In The Anomaly Scan?
The sonographer will observe the sonograms for a wide range of fetal abnormalities, some of which are normal and treatable. Some others may be severe and also fatal for the baby.
Following is the list of conditions that can be seen in the scan and their chances of detection (7) (8):
- Anencephaly (absence of the head top) – 99%
- Cleft lip or palate
- Hydrocephalus (extra fluid in the brain) – 60%
- Gastroschisis (defect of the abdominal wall in which the intestines protrude) – 90%
- Exomphalos (defect of the abdominal wall in which liver and bowel protrude) – 90%
- Spina bifida (open spinal cord) – 90%
- Lethal dysplasia (missing or short limbs) – 90%
- Missing or abnormal kidneys – 85%
- Diaphragmatic hernia (protrusion of abdominal content in the thorax via a hole in the muscle dividing the chest and abdomen) – 60%
- Heart problems such as defects in the chambers, vessels, and valves – 25%
- Down syndrome – 40%
- Patau’s or Edward’s syndromes (chromosomal abnormalities)
Some conditions, including heart defects and bowel obstructions, are not detected until late pregnancy. Anomaly scan will rule out or detect all the above conditions in time and allow the doctor to plan the further course of action.
An anonymous mother recalls her 20th-week anomaly scan detected fetal anomalies such as mongoloid features, absent nasal structure, and low-set ears in her child. She says, “The sonologist instructed me to lie down and put the cold gel on my tummy… She then said that she could see the nostrils but not the nose… She pointed to one of her assistants and asked her to confirm that what she saw were ears and then said that it was lower than where they were supposed to be by that age.”
After a few days, the mother went to see her OB to get her anomaly scan reports checked. She adds, “When it was our turn, we handed the result to her (the OB) and waited for her to check it… She said these were just soft signs, and there wasn’t any assurance whether the baby has DS until the day he comes out. The whole reason for the CAS is that we could prepare ourselves if something is wrong. She tried to make me feel better and suggested that if we wanted, we could have a 3D ultrasound on my 7th month to have a better look at our baby (i).”
What Happens If The Anomaly Scan Is Not Normal?

Know that the anomaly scan result is not always 100% accurate, and observations may sometimes go incorrect. If any problem is spotted, your doctor might give you advice on how to deal with the condition.
- Some problems may need a repeat scan. This is in case the sonographer has not seen everything in detail because of the unfavorable fetal position, or the mother’s dense skin tissue hindering the view. In this case, the scan is repeated around the 23rd week.
- If a problem is suspected, you will be given an appointment with a fetal medicine specialist.
- If your baby is suspected of having a heart problem, you will be taken to a fetal echo scan for a detailed look at the heart.
- If a severe problem is detected, the doctor gives all the needed support and guides you through the options. Some issues may require surgery or treatment while the baby is still in the womb and some after birth.
 Point to consider
Point to considerEven the thought of the baby having a problem can be overwhelming. But know that not all babies have a congenital problem. If there is a concern, a chain of obstetricians, midwives, pediatricians, and other specialists will support you through it.
Next, we address a few commonly raised queries about this scan.
Frequently Asked Questions
1. Can I have a photo of my scan?
Most diagnostic centers will give the picture of your scan but check with the doctor before the appointment. They may also charge for the picture that is probably printed on thermal paper and is sensitive to heat.
2. When will I get the results of the scan?
The sonographer will tell you about the visible problems immediately during the scan. However, it depends upon the hospital when to produce the results.
3. Is anomaly scan painful?
No, scans are not painful. But you may feel uncomfortable sometimes as the sonographer may apply a little pressure on your abdomen and pelvic area to have a good view of the fetus (9).
4. Can I eat before an anomaly scan?
You can eat and drink normally before an anomaly scan. No fasting is required, and there is no need for you to go on an empty stomach (10).
5. Can I know the sex of my baby in the anomaly scan report?
You may know the baby’s gender in the anomaly scan report since the external genitalia are developed by 20 weeks. However, the identification of the sex also depends on the position of your baby. If the baby does not cooperate, the sonographer may not get a clear picture of the genitalia, making the identification difficult (11).
An anomaly scan is usually done to check the proper growth and development of the fetus and rule out any abnormalities. This scan does not pose any threat to the baby. So get this scan done during your pregnancy to determine any conditions present in the fetus. This will help respond promptly and reduce the chances of any complications in the future.
Infographic: Benefits Of An Anomaly Scan
Although having an anomaly scan is optional, doctors recommend it to every pregnant woman because of its multiple benefits. This infographic highlights those benefits and helps you understand the importance of this scan.
Some thing wrong with infographic shortcode. please verify shortcode syntax
Illustration: What Is Anomaly Scan During Pregnancy And Why Is It Done?

Image: Dall·E/MomJunction Design Team
Personal Experience: Source
MomJunction articles include first-hand experiences to provide you with better insights through real-life narratives. Here are the sources of personal accounts referenced in this article.
i. The congenital anomaly scan;https://thedailyducs.wordpress.com/2014/11/29/the-congenital-anomaly-scan/
References
1. Women’s Health Care; The Aga Khan University Hospital
2. Dr Mary Moran; Fetal Anomaly Scan Guidelines; The British Medical Ultrasound Society (BMUS)
3. Antenatal care critical in detecting and correcting foetal abnormalities during pregnancy; Aga Khan University Hospital (2018)
4. Charles H. Rodeck and Martin J. Whittle; Fetal Medicine: Basic Science and Clinical Practice; Page 266
5. 20-week anomaly scan; NHS (2018)
6. Yvonne Cargill and Lucie Morin; Content of a Complete Routine Second Trimester Obstetrical Ultrasound Examination and Report; SOGC CLINICAL PRACTICE GUIDELINE (2009)
7. Checking for structural anomalies St George’s Hospital; NHS
8. Dr Hon Sook Kit; Detailed Fetal Anomaly Scan; Regency Specialist Hospital (2017)
9. How an Anomaly Scan Helps & Why You Need It; Sitaram Bhartia
10. Dr Hon Sook Kit; Ultrasound scan—your 18 to 20 week scan; Mater Mothers’ Hospital
11. Dr Hon Sook Kit; 20-Week Ultrasound (Anatomy Scan); Cleveland Clinic
Community Experiences
Join the conversation and become a part of our nurturing community! Share your stories, experiences, and insights to connect with fellow parents.
Read full bio of Dr. Neha Singh
Read full bio of Rebecca Malachi
Read full bio of Dr. Ritika Shah
Read full bio of Reshmi Das