Image: Shutterstock
Erythema toxicum in newborns, also called erythema toxicum neonatorum or erythema toxicum, is a benign, transient, and self-limited skin eruption in newborns.
Approximately 48% to 72% of term infants develop this skin irritation condition (1). The condition does not cause other signs of systemic toxicityiToxic effects seen on different parts of the body rather than specific or single organs. such as fever, low temperature, irritability, or lethargy.
Read this post to know about the symptoms, causes, diagnosis, and treatment of toxic erythema of the newborn.
Key Pointers
- Erythema toxicum is a common, non-concerning skin condition seen in newborns and appears as rashes of different types.
- These lesions can result from factors such as an allergic reaction or the action of microbes near the hair follicles.
- The doctors can identify the condition from its significant rashes and usually let them heal on their own within the normal 14-day period.
Symptoms And Signs Of Erythema Toxicum Of The Newborn

Image: Shutterstock
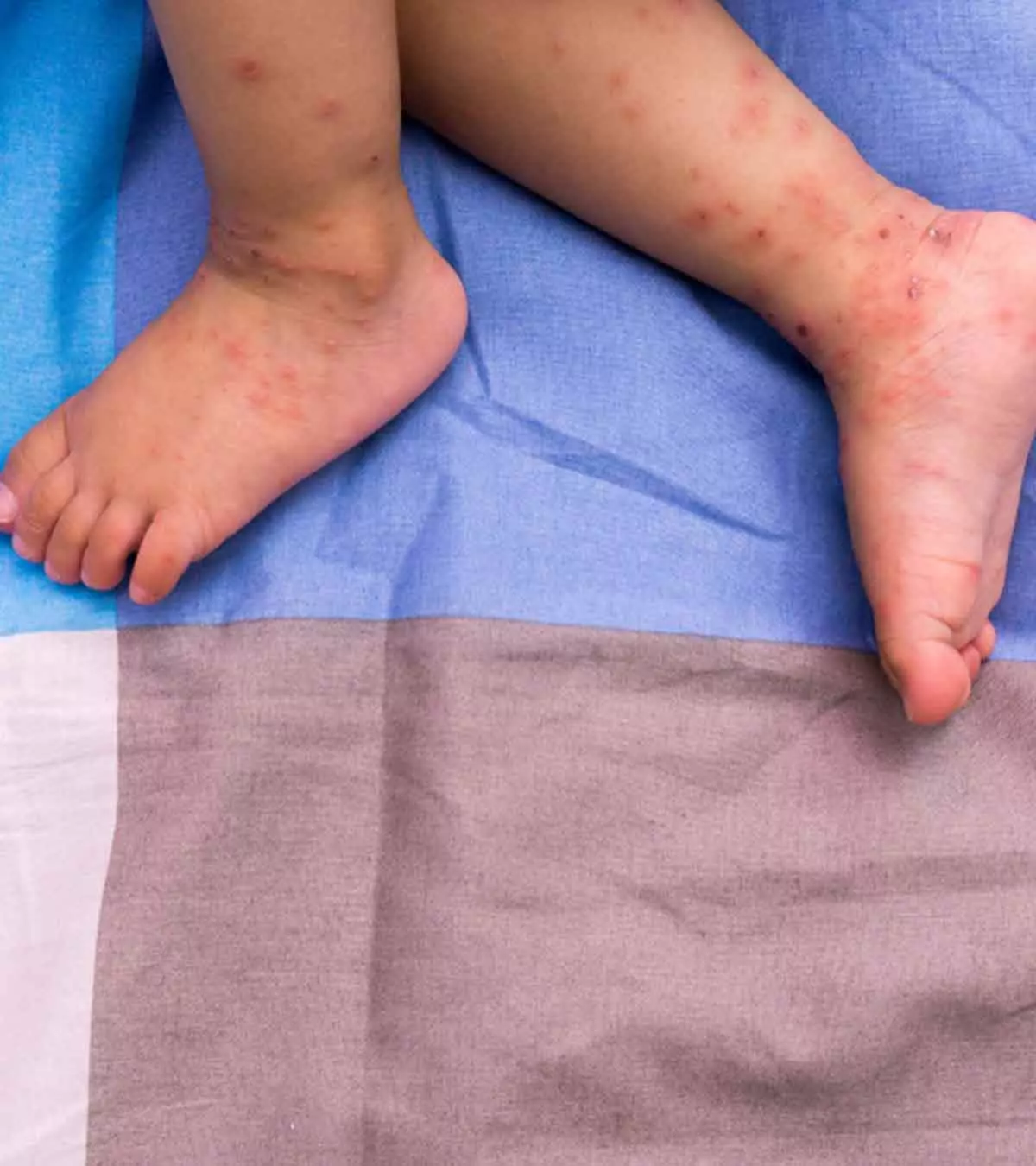
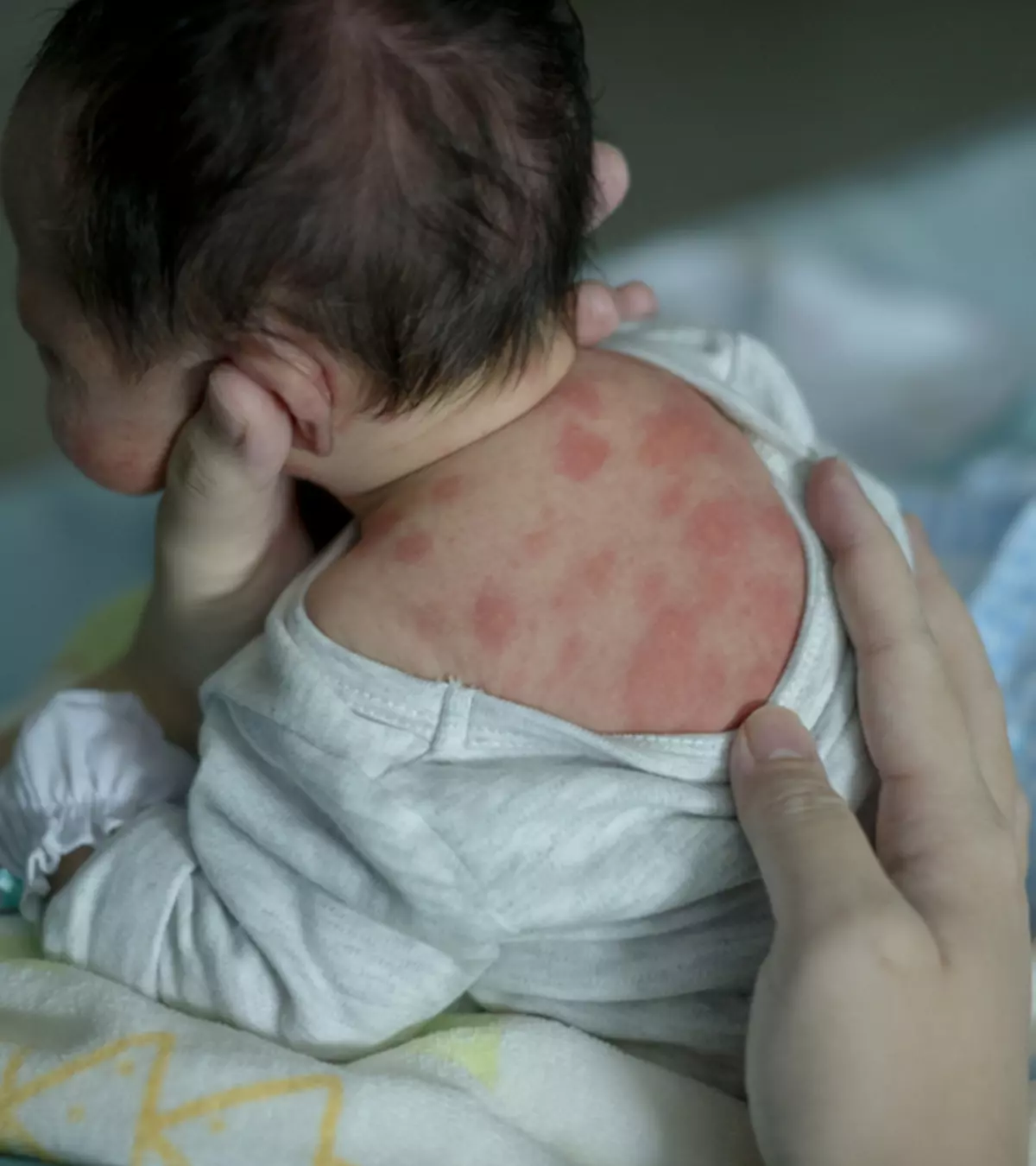
Erythema toxicum of the newborn may usually begin within the first six days of life. However, some babies may have late onset of the condition at up to two weeks of age. Erythema rash is rarely seen at birth (2). The skin redness and rashes may start on the face and spread to the torso and limbs. Palms and soles are usually spared. In most cases, babies appear well other than the skin rashes.
You may notice any of the following types of skin rashes in toxic erythema of the newborn (3).
- Erythematous macules are red flat skin patches
- Papules are small bumps on the skin
- Pustules are small skin bumps filled with pus or fluid
An irregular reddish wheal can surround yellow pustules and papules
. These skin eruptions can wax and wane over several days. It means they may increase or decrease in number, size, or severity over days.
How Long Does It Take For Erythema Toxicum To Go Away?
Most skin lesionsiThe parts of the skin that look different than the skin around them. in toxic erythema are transient or temporary. It may often disappear within a few hours and reappear on other parts of the body other than the soles and palms. Erythema toxicum may resolve within seven to fourteen days from the first day of their appearance. The skin eruptions fade away without leaving any scars.
Ruth Sameke, a mom of a baby girl, shares her experience on her blog of when her little girl suffered from Erythema toxicum, “I had been told that rashes are common in babies and that the rash that will appear on baby May’s cheeks and forehead, but no one told me about the one that would cover her entire face. So imagine the scare I got when I woke up one morning to find baby May’s face covered in blotchy bumps. What broke out on baby May’s face is called Erythema Toxicum Neonatorum. It is mostly common in full-term babies (40/40 weeks). She didn’t scratch or even seem bothered by it; however, it hurt to watch. Within two weeks, it was gone, you would have never known it was once there (ⅰ).’’
Causes Of Toxic Erythema Of The Newborn
The exact cause of toxic erythema of the newborn is unknown. It is considered to be an allergic response since the skin lesions display significant eosinophilic infiltrationiThe build-up of eosinophils (white blood cells) in a tissue or organ that may lead to inflammation or destruction of the tissue. . Eosinophils are a type of white blood cells. It was suggested that the skin allergies could be due to the maternal lymphocytes (a type of white blood cell). However, recent studies have failed to prove the presence of maternal cells in skin lesions.
The absence of skin lesions on non-hair-bearing areas, such as palms and soles, suggests that erythema toxicum could be a response to skin inflammation caused by microbes penetrating the hair follicles. However, more studies are needed to identify the microbes and the mechanism for the development of erythema toxicum neonatorum (1).

Image: Shutterstock
There is no genetic or gender prediction known for erythema toxicum. Premature infants tend to be less likely affected by the condition for unknown reasons.
Diagnosis Of Toxic Erythema Of The Newborn
Differential diagnosis is crucial to distinguish erythema toxicum from other similar rashes and ensure appropriate care. Doctors can diagnose erythema toxicum based on the clinical features. Characteristics of a neonatal rash and no associated symptoms are key to diagnosis. Skin biopsy could show infiltration of neutrophils and eosinophils in the upper skin. Pustules and papules may also contain these inflammatory cells and are usually located around the hair follicles.
Clinical diagnosis is sufficient in most cases, and no laboratory analysis is ordered. Doctors may often order some tests to rule out similar conditions. Differential diagnosis to toxic erythema of the newborn may include the following conditions (4).
- PyodermaiA rare skin disorder that causes severe ulceration (wounds) of the skin, usually on the legs.
- Congenital candidiasisiA rare condition in newborns usually caused by intrauterine candida infection that leads to rashes, respiratory disorders, and sepsis.
- Staphylococcal folliculitisifolliculitis: A bacterial infection of the hair follicle that resembles acne and causes itching and discomfort.
- Neonatal SepsisiBlood infection occurring in newborns and babies less than 90 days old.
- Acne neonatorum (baby acne)
- Neonatal varicellaiAbnormalities in the newborn due to the mother getting chickenpox during early pregnancy.
- Miliaria (baby heat rash)
- HerpesiA skin condition leading to sores and painful blisters on different parts of the body.
- Transient neonatal pustular melanosis (TNPM)iA benign skin disorder occurring in newborns in which they have pus-filled pustules at birth which burst later.
- Incontinentia pigmentiiA disorder that affects skin, hair, teeth, nails, eyes, and the central nervous system and is characterized by skin lesions in babies.
- Infantile acropustulosisiA condition in which there is a recurrence of itchy pustules on the extremities.
 Quick fact
Quick factTreatment For Erythema Toxicum

Image: Shutterstock
Erythema toxicum of the newborn does not require any treatment since it fades away within days or weeks without any complications. Doctors may educate the parents about the natural course of this condition and advise them not to apply any OTC creams or other remedies.
Primary care physicians may often refer to pediatric dermatologists to rule out other diagnosis (3). Antifungals and antibacterial creams are only effective in treating rashes in babies caused by fungal infections and bacterial infections.
 Quick tip
Quick tipFrequently Asked Questions
1. Can erythema toxicum spread?
Erythema toxicum in babies usually starts on the face and may spread to the arms, legs, and torso. However, the condition is not contagious and does not spread from one person to another (5).
2. Are there any long-term effects of erythema toxicum in newborns?
Erythema toxicum has been found to have a good prognosis and no long-term complications in the child. However, a link between erythema toxicum and eosinophilic esophagitis (allergic condition of the esophagus) may be present (1).
3. Can erythema toxicum rash be prevented in newborns?
There are no known methods to prevent erythema toxicum rash in newborn babies (6). Since this is a self-limiting condition, following the doctor’s advice and avoiding touching the bumps may help with the healing process.
4. Is erythema toxicum rash painful for newborns?
No, erythema toxicum rash isn’t painful for newborns (6). However, avoid overwashing and scrubbing to prevent dryness and itchiness.
5. What is the difference between baby acne and erythema toxicum?
Erythema toxicum in newborns is a self-limiting condition that could appear from the first six days of life to two weeks after birth. The precise cause of this skin condition is unknown. However, it is considered a skin allergy in babies with undetermined etiology. Most babies get transient rashes and are generally well otherwise. Experts advise letting the condition run its course as the rashes usually self-heal without causing skin damage or scars. Nonetheless, consulting a doctor for all skin problems during the neonatal period is vital to ensure the baby is safe and healthy!
Infographic: Conditions Requiring Medical Attention In Erythema Toxicum Neonatorum
Erythema toxicum neonatorum (ETN) affects newborns during their first two weeks of life and is usually mild. However, contact a pediatrician if you observe any symptoms mentioned in the infographic below. As several skin conditions may have symptoms similar to ETN, early diagnosis can help prevent potential complications.
Some thing wrong with infographic shortcode. please verify shortcode syntaxIllustration: Erythema Toxicum Neonatorum In Newborns: Symptoms & Treatment

Image: Stable Diffusion/MomJunction Design Team
Personal Experience: Source
MomJunction articles include first-hand experiences to provide you with better insights through real-life narratives. Here are the sources of personal accounts referenced in this article.
i. Baby’s Skin: Delicate, Sometimes Irritated, Plus The Two Complexions.https://mumandmay101.wordpress.com/2026/04/17/babys-skin-delicate-sometimes-irritated-plus-the-two-complexions/
References
1. Erythema Toxicum; U.S. National Library of Medicine
2. Etiology of Toxic Erythema; Erythema Toxicum Neonatorum; JAMA Pediatrics; JAMA Network
3. Toxic Erythema of the Newborn; DermNet NZ
4. Newborn Skin: Part I, Common Rashes; American Academy of Family Physicians
5. Erythema toxicum; Raining Children, Australia
6. Erythema Toxicum Neonatorum; Cleveland Clinic
Community Experiences
Join the conversation and become a part of our nurturing community! Share your stories, experiences, and insights to connect with fellow parents.
Read full bio of Dr. Neema Shrestha
Read full bio of Dr Bisny T. Joseph
Read full bio of Rohit Garoo
Read full bio of Shinta Liz Sunny