Image: Shutterstock
Rubella in children is usually a mild condition but could lead to complications if not managed properly. Rubella, often referred to as German measles, is a contagious viral infection marked by a red rash and flu-like symptoms. It is caused by the rubella virus, which spreads mainly through respiratory droplets when an infected person coughs or sneezes. The red rashes caused by the infection are the most noticeable of its signs.
Read on to learn about the signs and symptoms of rubella in kids as well as treatment options and preventative strategies.
Key Pointers
- Rubella is a mild form of skin infection in babies.
- Mild fever, nausea, and inflammation of the joints are common symptoms.
- If rubella is left untreated in a pregnant woman, it can lead to complications.
- Babies born with CRS are prone to having congenital disabilities such as anemia and low birth weight.
Symptoms Of Rubella
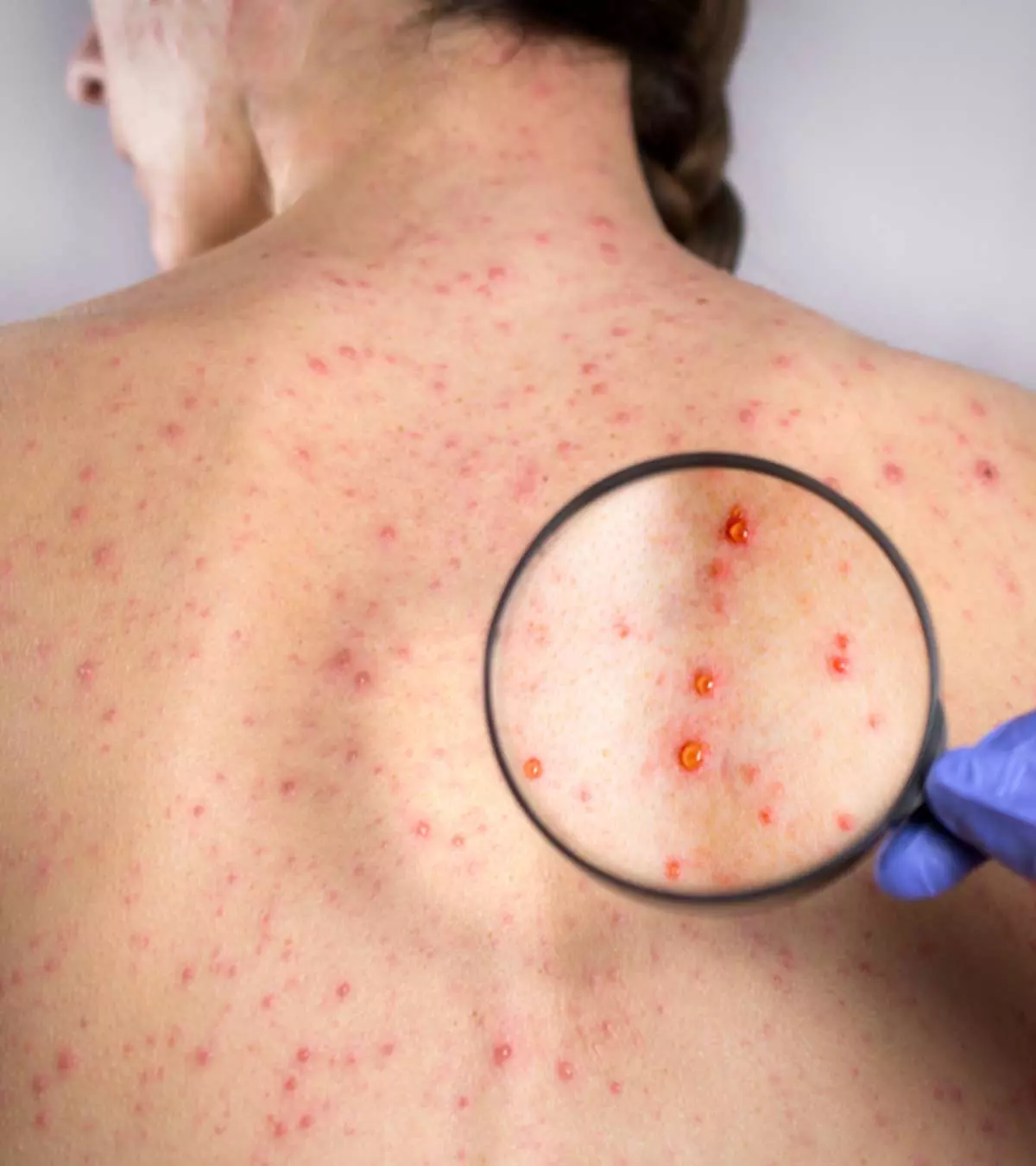
The symptoms of pediatric rubella infection are usually mild; the rash appears two to three weeks after exposure to the virus. According to the World Health Organization (WHO), this rash is observed in approximately 50 to 80 percent of affected children and typically endures for one to three days. Some common symptoms of rubella in children include (1) (2):
- Red-colored spotty rash that start on the face and neck and progress downward (rashes last for one to three days)
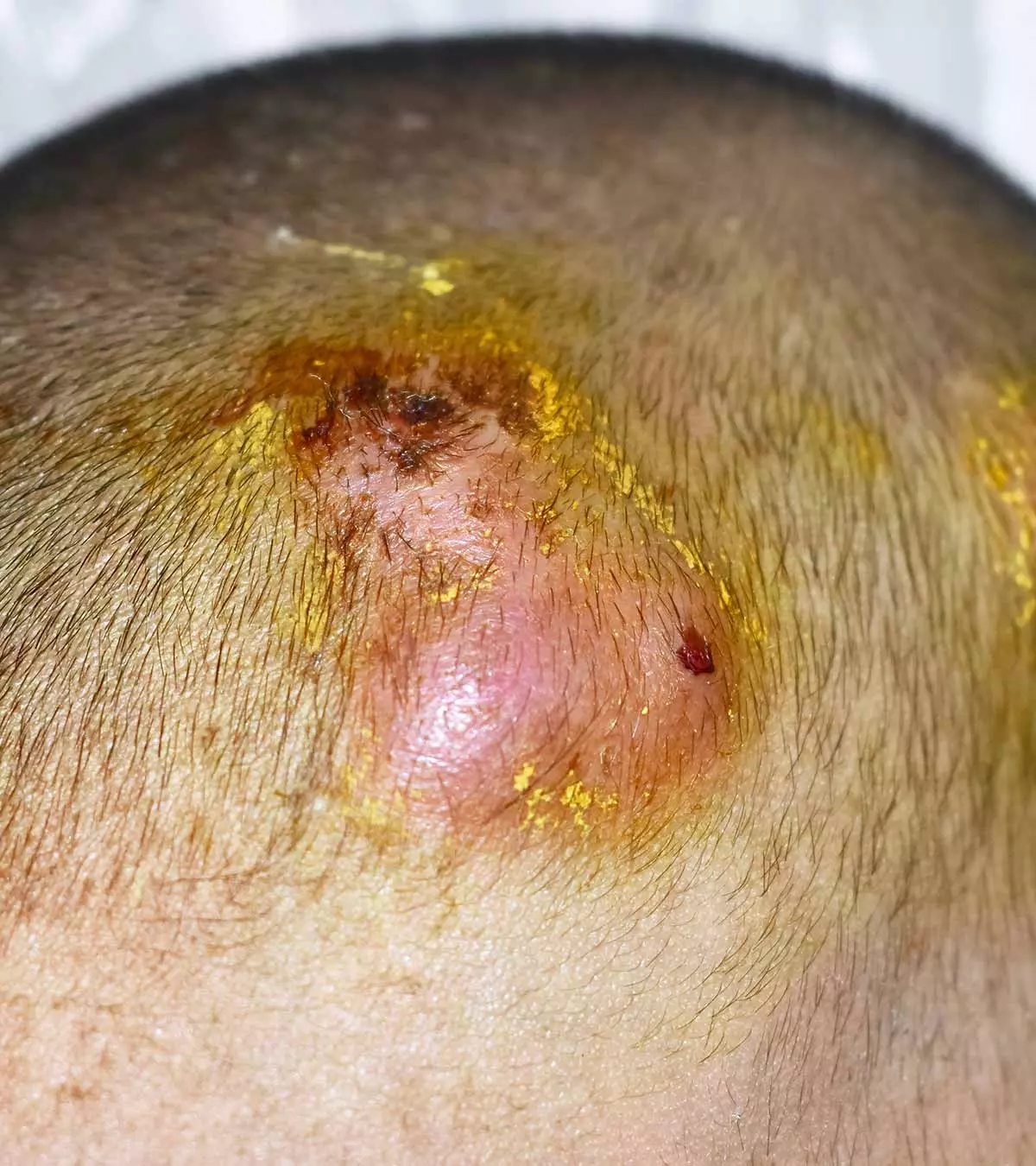
- Swollen lymph glands behind the ears and in the neck
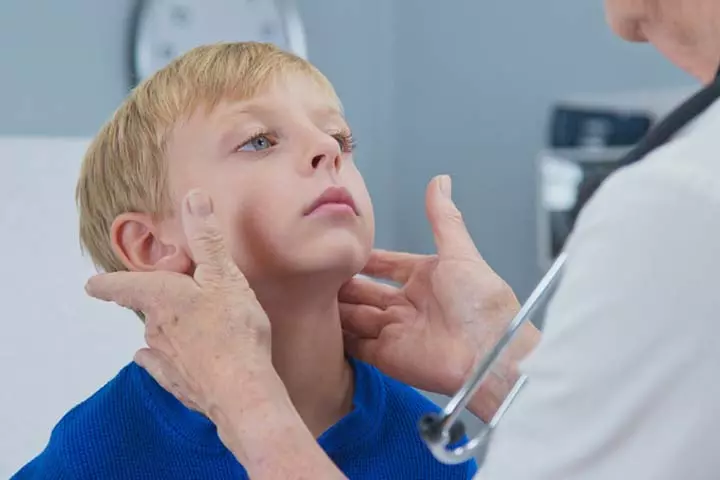
Image: Shutterstock
- Low fever with a body temperature of less than 39℃
- Nausea and mild conjunctivitisiInflammation of the transparent membrane that covers the inner region of eyelids and the outer part of the eyeball
- Soreness and inflammation of joints (more common in older children and adolescents)
Once a child is infected, the virus spreads through the body in five to seven days. The child may spread the virus one week before the onset of rash and remain contagious up to seven days after the rash appears. However, the Centers for Disease Control and Prevention states that 25% to 50% of people do not develop a rash or any symptoms (3).
A woman infected with rubella during early pregnancy (before 10 weeks are completed) has a 90% chance of passing the virus to the fetus. The virus may cause a miscarriage, or the fetus may develop congenital rubella syndrome (CRS) (1). Anyone with rubella or exposure to a known case of rubella should not come in direct contact with a pregnant woman.
 Things to know
Things to knowCongenital Rubella Syndrome
Babies born with CRS suffer from many congenital disabilities. Some common disabilities associated with this congenital syndrome include the classical triad of cataract, heart defects, and deafness. The following are usually seen in neonatal period and are transient (1) (2) (4):
- Low birth weight
Image: Shutterstock
- Low platelets
- Anemia
- Enlargement of liver and spleen
- Inflammation of brain and meningesiTri-layered membranes that protect the central nervous system (the brain and spinal cord)
Longer lasting or permanent manifestations include:
- Hearing impairments
- Eye defects such as cataract, glaucomaiAn eye condition where optic nerves are damaged due to increased pressure on the eyes, leading to gradual vision loss , retinal damage, small eye
- Heart defects such as patent ductus arteriosusiA congenital condition in which the opening between two crucial blood vessels of the heart fails to close and pulmonary hypertension
- Autism
- Diabetes mellitusiA metabolic disease characterized by high sugar levels in the blood
- Thyroid dysfunction
- Mental retardation
- Delayed growth
As some of these impairments are lifelong and require therapies and surgeries, women of childbearing age are advised to take the measles mumps rubella (MMR) vaccination. However, it is not advisable to vaccinate pregnant women. The vaccine should be taken at least four weeks before planning a pregnancy.
Who Is At A Higher Risk For Rubella?
Anyone who does not have immunity against rubella is at risk of developing rubella. However, according to the World Health Organization (WHO), the highest risk of CRS is in women of childbearing age who do not have immunity to the disease (1).
Diagnosis And Treatment For Rubella

Image: Shutterstock
Your child’s doctor might diagnose rubella based on physical examination and the child’s medical history. The pediatric specialist might further recommend blood or urine tests to confirm the diagnosis (5).
Since rubella is a viral infection, there is no cure for it. It is best to vaccinate children and women in child bearing age beforehand. If your child is infected with the rubella virus, your doctor might recommend the following.
- Increased intake of fluids
- Adequate rest
- Isolation to prevent the spread of the virus
- Over-the-counter medications to reduce the severity of the symptoms (5)
Children might recover from rubella within a week.
The caretaker should always wash and disinfect the infected child’s clothes and dry them under the sun. It is important to teach children to cover their nose and mouth when sneezing or coughing. Such precautions should be taken to prevent the spread of the infection.
Prevention Of Rubella
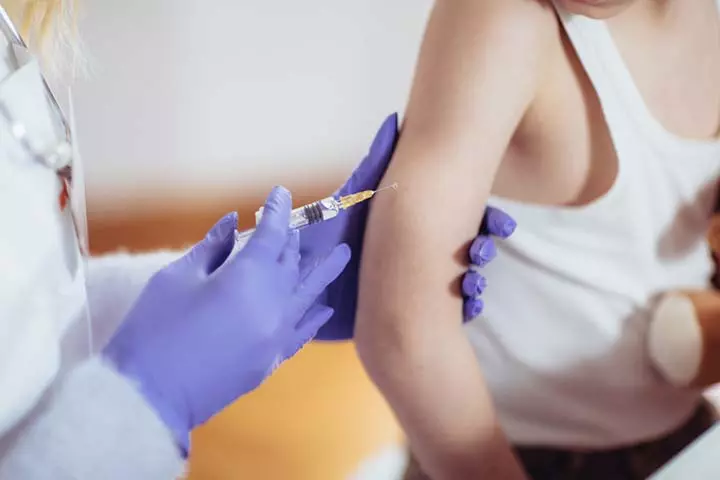
Image: Shutterstock
The best way to prevent the infection is through vaccination. The vaccine for rubella is a live attenuated strain, and a single dose can give long-lasting immunity to more than 95% of children (6). The vaccine is available in monovalent (single vaccine for rubella) form and is also administered in combination with other vaccines, such as the measles, mumps, and rubella (MMR) vaccine. However, in rare cases, children can get rubella even if they had been vaccinated or had a previous rubella infection (7).
According to the CDC, all children should get two doses of the MMR vaccine. The first dose should be given at 12–15 months of age, and the second dose at 4–6 years of age. Children can also receive the second dose 28 days after the first dose (8). In India, the first dose is given at 9 months and second at 15 months. It has recently been added to the national immunization schedule and is to be given in combination with measles vaccine.
 Quick fact
Quick factPossible Side Effects Of The Vaccine

Image: Shutterstock
There may be mild adverse reactions after the vaccination, including pain and redness at the injection area, low-grade fever, rash, and muscle aches (1).
However, children with the following conditions should consider vaccination only after consulting a doctor (8).
- Children with life-threatening allergies and a weak immune system due to HIV or cancer and children undergoing medical treatments such as radiation, immunotherapy, steroids, or chemotherapy
- Children with a family history of immune system problems
- Children who had a condition that makes them bleed or bruise easily
- Children who have tuberculosis or had other live vaccines in the past four weeks
- Children who are ill
Frequently Asked Questions
1. How long is rubella contagious?
Yes. Rubella is contagious when the rashes start to appear. This could be seven days before to seven days after the symptoms are seen. Rubella is the most contagious when the rashes erupt (9).
2. How long does it take to recover from rubella?
Children with rubella may usually recover from the infection within seven to ten days. The symptoms might go away in a few days, but the glands may remain swollen a few weeks after the infection (10).
3. Are mumps and rubella the same?
No, mumps or rubella are different viral infections. Mumps in children mainly causes inflammation of the salivary gland. On the other hand, rubella causes mild fever and skin rashes in children. Although these viral infections are different, they can be prevented through the MMR vaccine, which also protects against measles (11).
Rubella in children is a benign viral infection, but it can have serious consequences if a woman is infected during pregnancy. Infected children may develop symptoms such as a reddish-brown spotty rash, swollen lymph glandsiTube-like structures that are part of a system (lymphatic system) of the body that plays a role in providing immunity against diseases behind the ears and in the neck, low body temperature, and so on, and can spread the infection for up to seven days. Rubella has no known cure, but immunization is the most effective way to prevent it. If your child has been diagnosed with rubella, keep them away from the other children and family members and take all necessary precautions to prevent the spread of the disease.
Infographic: More About Signs And Prevention Of Rubella
Rubella is an infectious condition whose spread can be controlled using simple safety measures. If your child is exposed to the infection-causing pathogens and exhibits these signs, get them evaluated and follow these steps to prevent further disease transmission.
Some thing wrong with infographic shortcode. please verify shortcode syntax
Illustration: Symptoms Of Rubella In Children Treatment And Prevention
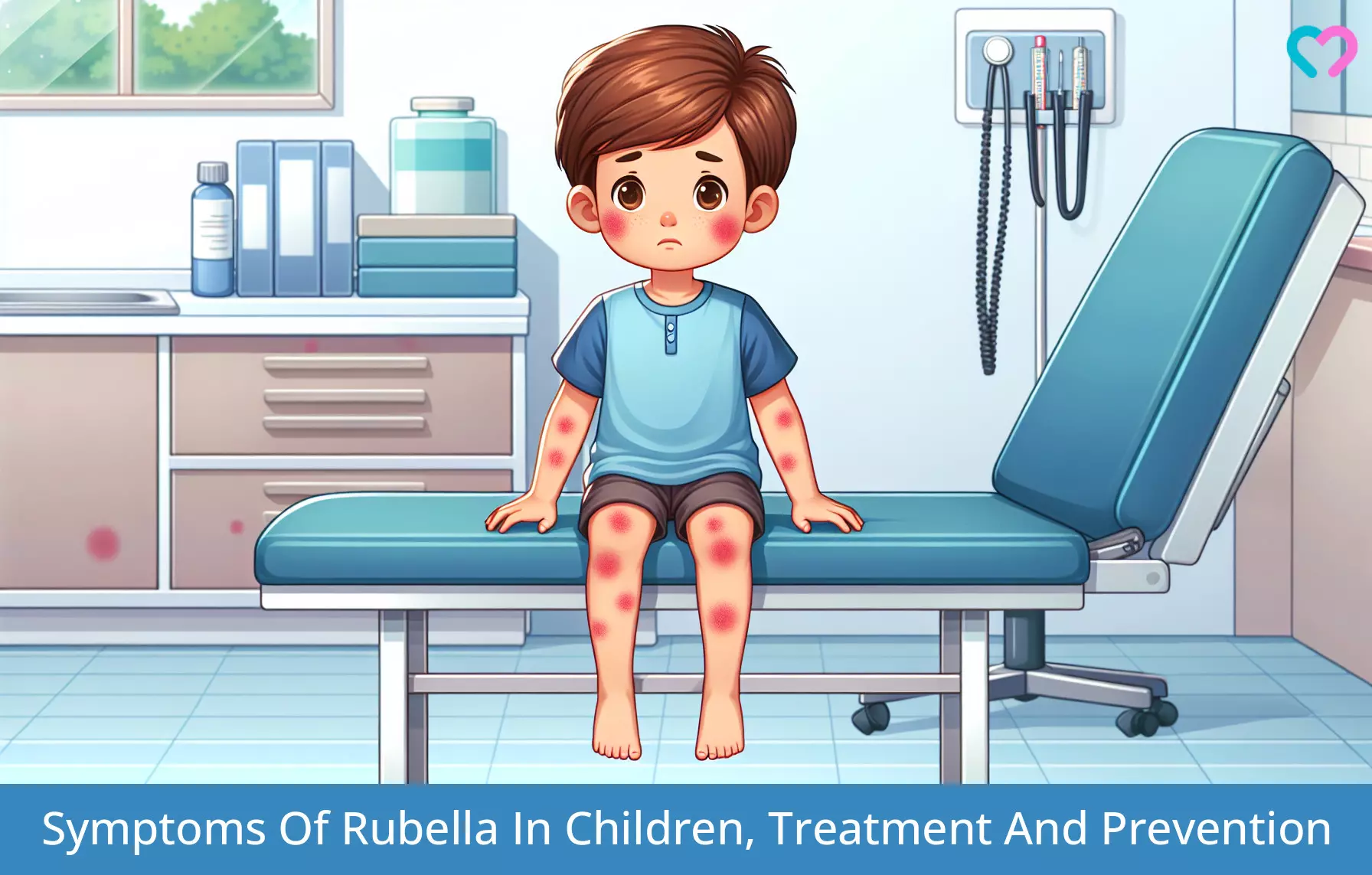
Image: Dall·E/MomJunction Design Team
Rubella is a contagious condition in children. This video gives valuable insight into the causes, symptoms, diagnosis, and treatment.
References
1. Rubella; World Health Organization
2. Rubella Symptoms & Causes; Boston Children’s Hospital
3. About Rubella; CDC
4. Manual for the Surveillance of Vaccine-Preventable Diseases – Chapter 15: Congenital Rubella Syndrome; CDC
5. Testing & Diagnosis for Rubella in Children; Boston Children’s Hospital
6. Jan Hendriks and Stuart Blume; Measles Vaccination Before the Measles-Mumps-Rubella Vaccine; American Journal of Public Health (2013).
7. Rubella; Better Health Channel – State of Victoria
8. Vaccines and Preventable Diseases – Measles, Mumps, and Rubella (MMR) Vaccination: What Everyone Should Know; CDC
9. Clinical Overview of Rubella; CDC
10. Rubella; NHS Inform
11. Measles, Mumps, and Rubella (MMR) Vaccine; Stanford Children’s Health
Community Experiences
Join the conversation and become a part of our nurturing community! Share your stories, experiences, and insights to connect with fellow parents.
Read full bio of Dr. Pooja Parikh
Read full bio of Swati Patwal
Read full bio of Rohit Garoo
Read full bio of Shinta Liz Sunny