
Image: ShutterStock
Gray baby syndrome (GBS) is a rare disorder that is caused due to the presence of high levels of chloramphenicol in babies born prematurely
. Chloramphenicol is an antibiotic that is used in the treatment of bacterial infections such as meningitisiThe inflammation of the meninges or membranes around the brain and spinal cord due to an infection. , cholera, and typhoid fever. The common symptoms of this disease include graying of the baby’s skin, cardiac issues, and swelling up of the abdomen (also known as abdominal distension). Although the complications caused due to this syndrome can be severe, they can be prevented. Read on to know more about the causes, signs, treatment, diagnosis, and prevention of this syndrome.
Key Pointers
- High levels of chloramphenicol cause Gray baby syndrome, a rare medical condition that results in circulatory collapse and gray skin color.
- The newborn’s liver and kidneys are inefficient in eliminating chloramphenicol, leading to its accumulation in the body.
- Symptoms include low body temperature, respiratory distress, cyanosis, hypotension, abdominal distention, pale appearance, and ashen-gray skin color.
- Complications include hepatic and renal failure, vision problems, peripheral neuritis, aplastic anemia, cardiovascular issues, and brain damage.
- Treatment involves intensive support therapy with the withdrawal of chloramphenicol using activated charcoal hemoperfusion and exchange transfusion.
Causes Of Gray Baby Syndrome
The primary cause is the accumulation of the antibiotic chloramphenicol in the blood serumiThe liquid part of the blood left after the blood cells and clotting materials are removed. of an infant. Blood serum levels of chloramphenicol higher than 50mcg/mL is associated with gray baby syndrome. Toxic levels of chloramphenicol may cause a circulatory collapse that leads to mottling (smears of color) of the skin in ashen-gray color (1). This disease is named after the appearance of gray-colored skin in newborn babies.
Gray baby syndrome can be due to the following deficiencies in neonates (1).
- The immature liver may not be able to metabolize the chloramphenicol.
- Newborn’s kidneys are not efficient enough to excrete chloramphenicol and its metabolic products from the body.
A well-functioning liver and kidneys can metabolize and excrete the chloramphenicol
. However, it may not be the case in babies. This could be a reason that premature neonates are more vulnerable to gray baby syndrome than healthy and full-term infants.
 Quick fact
Quick factNote: A research study published by the CDC suggests that newborns getting this syndrome in utero due to maternal exposure to chloramphenicol is extremely low (2).
Risk Factors Of Gray Baby Syndrome
The following risk factors may play a vital role in the development of gray baby syndrome during the neonatal period.
- Reduced liver (hepatic) function
- Reduced kidney (renal) function
- High dose of chloramphenicol
- Longer duration of chloramphenicol treatment
- Maternal use may cause chloramphenicol to reach the baby through breast milk
- Underweight and malnourished children

Image: Shutterstock
Pediatricians decide chloramphenicol dose based on weight. This weight-based dosage may vary among newborns until the first 15 days. There may also be variations in dosage in babies up to four weeks old and those older than a month.
Note: Although there is a lack of quality evidence, NHS reports suggest that chloramphenicol is contraindicated in breastfeeding mothers due to infant toxicity (3). It is also a category C drug that may cause complications in pregnant women (4).
Symptoms Of Gray Baby Syndrome
Gray baby syndrome may occur after two to nine days of chloramphenicol treatment
. The onset and severity may vary based on drug levels and hepatorenal functions.
Gray baby syndrome symptoms may include (5) (6):
- Fussiness
- Poor feeding
- Weakness
- Vomiting
- Changes in mental status such as lethargy and less alertness (obtundation)
- Pale appearance (pallor)
- Ashen-gray color of the skin
- Abdominal tenderness
- Abdominal distention
- Hypotension (low blood pressure)
- Cyanosis causing blue lips, blue nails and bluish skin
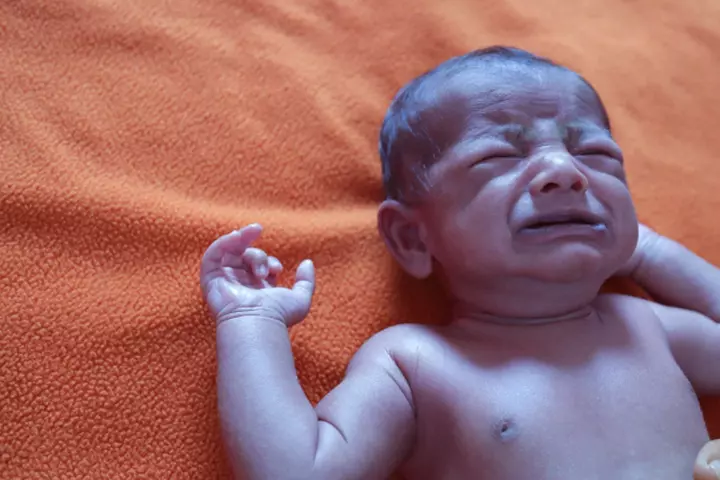
Image: Shutterstock
- Respiratory distress
- Low body temperature
Seek medical advice if you notice any signs and symptoms of toxicity in newborns due to direct or maternal intake of chloramphenicol antibiotics.
Complications Of Gray Baby Syndrome
The following complications can be associated with chloramphenicol toxicity (1) (7):
- Bleeding
- Liver failure
- Renal failure
- Aplastic anemiaiA rare blood disorder in which the body does not produce enough new blood cells due to bone marrow damage. due to bone marrow toxicity (8)
- Inflammation of the optic nerve (optic neuritis) and vision problems
- Problems with peripheral nerves (Peripheral neuritisiNumbness and tingling in the extremities due to nerve damage. )
- Cardiovascular collapse or shock
- Infection
- Brain damage
Chloramphenicol could displace bilirubin (formed by the breakdown of red blood cells) from albumin (main blood protein). Free or non-albumin bound bilirubin may cause newborn jaundice (yellow skin and eyes) and permanent brain damage known as kernicterus (1)
Diagnosis Of Gray Baby Syndrome
Diagnosis of gray baby syndrome can be made from the ashen-gray appearance of the skin along with the history of exposure to chloramphenicol in babies. Neonatologists or pediatricians may also look for signs of toxicity during physical examination.
The following tests are ordered to confirm the diagnosis of the gray baby syndrome (1):
- Blood tests could show the levels of chloramphenicol in the blood. Cardiac biomarkers, arterial blood gasiA test that measures the levels of oxygen and carbon dioxide in the blood to examine the working of the lungs. , metabolic profileiA set of blood tests to check the levels of different blood components and gain information about metabolism and chemical balance. , etc., are based on blood tests to identify or exclude conditions that can be present with neonatal cyanosis.
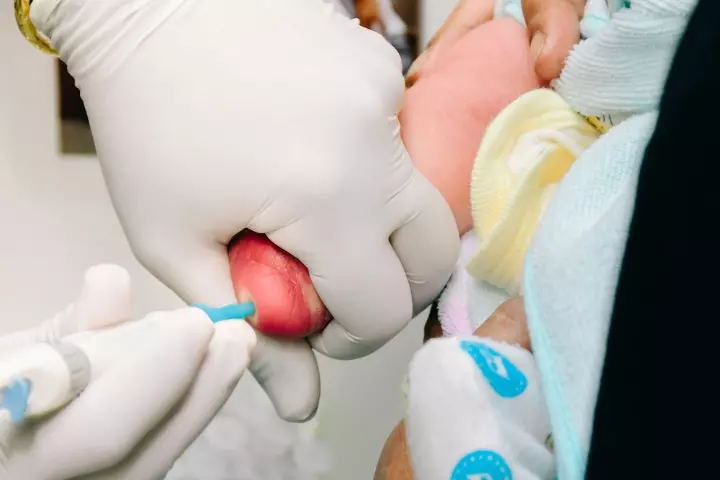
Image: Shutterstock
- CT scan, abdominal X-rays, or abdominal ultrasound are conducted depending on the symptoms.
- Electrocardiography (ECG) and echocardiography are often done to exclude cardiac causes of circulatory collapse and skin discoloration.
Your doctor may perform these tests to look for neonatal sepsisiBlood infection in babies less than 90 days old. , trauma, volvulusiA condition in which the intestine twists around itself and its mesentery to create a bowel obstruction. , heart diseases, and metabolic syndromes to make a differential diagnosis, since these conditions may also cause cyanosis in babies.
Treatment For Gray Baby Syndrome
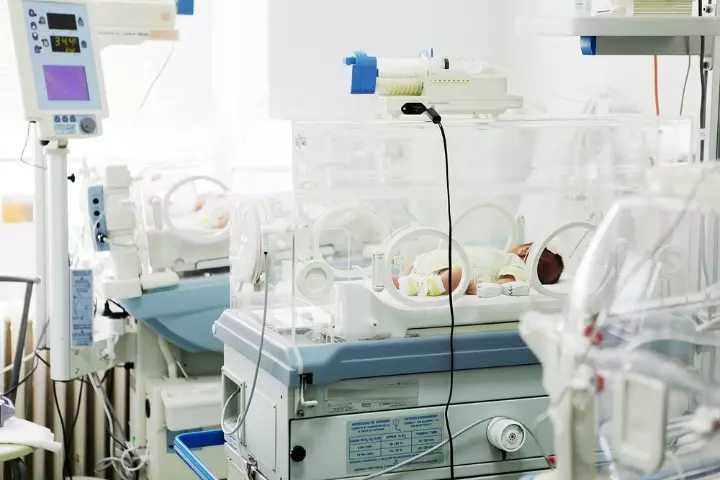
Image: Shutterstock
The treatment for gray baby syndrome is intensive support therapy with the withdrawal of chloramphenicol. Babies with problems in the blood and circulatory system receive aggressive resuscitation in intensive care units. They may receive appropriate oxygen therapy, ventilation, and early intubation, depending on the requirement.
If the baby develops hypothermiaiThe inability of the body to produce heat faster than it loses, leading to a severe drop in body temperature. , then they will require rewarming. HypoglycemiaiA condition in which there is an excessive drop in blood sugar levels. will require glucose correction.
The direct removal of antibiotic chloramphenicol molecules from the blood can be achieved by the following treatments (6).
- Activated charcoal hemoperfusion: This is an extracorporeal (outside the body) method to filter the toxin from the body.
- Exchange transfusion: This life-saving procedure involves the replacement of a patient’s blood with fresh donor plasma or blood.
Third-generation cephalosporin and phenobarbital medications are also used for treating gray syndrome (5).
Prognosis Of Gray Baby Syndrome
The prognosis or outcomes are good if the gray baby syndrome is diagnosed earlier, and the chloramphenicol treatment is discontinued
. However, if the baby has developed organ failure before diagnosis, then there is a high risk of worse prognosis.
Prevention Of Gray Baby Syndrome
Avoiding chloramphenicol exposure is a way to prevent gray baby syndrome. This can be achieved by practicing the following steps.
- Pediatricians and infectious disease experts try to give other safer antibiotics instead of chloramphenicol to babies.
- Expecting mothers and nursing mothers should go for treatment with newer antibiotics instead of chloramphenicol since it may cause birth defects in unborn babies and neonatal toxicity.
 Health fact
Health factHealthy babies and premature infants are carefully monitored for drug levels in the blood if they are treated with chloramphenicol antibiotics.
Long-term therapy with oral or intravenous chloramphenicol may result in gray baby syndrome. You may also seek a healthcare provider’s advice before using chloramphenicol eye drops for bacterial conjunctivitisibacterial infection causing the inflammation of the membrane that covers the eyelids and the eyeball. in infants and children since this may also result in toxicity (9). Pediatric drug therapy with chloramphenicol is only considered when it is an absolute requirement.
Frequently Asked Questions
1. Does tetracycline cause gray baby syndrome?
Tetracycline is a bacteriostatic antibiotic that should not be used during pregnancy (10). The drug, in high doses, can suppress bone growth and cause tooth discoloration. However, its association with the gray baby syndrome is not well established.
2. Which enzyme is deficient in gray baby syndrome?
Infants, particularly preterm infants, have immature livers that cannot produce and recycle UDP-glucuronyl transferase enzymes that help metabolize chloramphenicol. A shortage of these enzymes leads to increased serum levels of chloramphenicol, leading to the gray syndrome (11).
3. What age is Gray baby syndrome?
Gray Baby syndrome is a rare but dangerous disease that has been most frequently observed in newborn babies or neonates. It has also been observed to occur in babies up to the age of two years (12).
Gray baby syndrome is an adverse drug reaction to antibiotic chloramphenicol. The use of chloramphenicol in babies is limited, considering the risk for this reaction. It was often used in topical ointments and eye drops in the past. Currently, doctors may recommend chloramphenicol for treating specific infections such as typhoid fever or tick-based rickettsiaiBacteria caused by ticks leading to spotted fever and typhus. infections. However, knowing the risks, healthcare providers often consider alternate drugs. Chloramphenicol is not prescribed for pregnant mothers since it has the potential to cause congenital disabilities in babies. However, lower doses are considered in unavoidable cases.
Infographic: Use Of Chloramphenicol In Lactating Mothers
If you are nursing your newborn, you must be aware of certain crucial factors regarding the use of chloramphenicol during breastfeeding. This infographic shares some critical points about using chloramphenicol while breastfeeding. Illustration: Momjunction Design Team
References
- Earl D. Cummings and Mary Ann Edens; Gray Baby Syndrome; The United States National Library of Medicine (NLM)
https://www.ncbi.nlm.nih.gov/books/NBK448133/ - Christina A. Nelson et al.(2026) Antimicrobial Treatment and Prophylaxis of Plague: Recommendations for Naturally Acquired Infections and Bioterrorism Response; Centers for Disease Control and Prevention
https://www.cdc.gov/mmwr/volumes/70/rr/rr7003a1.htm - Chloramphenicol: is it safe in breastfeeding? NHS Evidence website.
http://www.midlandsmedicines.nhs.uk/filestore/QA263_ChloramphenicolBM.pdf - Chloramphenicol; Drugs and Lactation Database (LactMed); The United States National Library of Medicine (NLM)
https://pubmed.ncbi.nlm.nih.gov/30000554/ - Mahendra Kumar BJ et al. Drug Induced Syndromes: An Overview; Indian Journal of Pharmacy Practice;
https://ijopp.org/files/IndJPharmPract-5-3-13.pdf - Gray baby syndrome; Sciencedirect
https://www.sciencedirect.com/topics/pharmacology-toxicology-and-pharmaceutical-science/gray-baby-syndrome - WHO Food Additives Series: 53; Chloramphenicol; International Programme On Chemical Safety (IPCS)
https://www.inchem.org/documents/jecfa/jecmono/v53je03.htm - Chloramphenicol-Induced Bone-Marrow Aplasia; The New England Journal of Medicine
https://www.nejm.org/doi/full/10.1056/NEJM196711092771912 - Tim Lancaster et al. Risk of serious haematological toxicity with use of chloramphenicol eye drops in a British general practice database; The British Medical Journal
https://www.bmj.com/content/bmj/316/7132/667.1.full.pdf - Teratogenic Medications.
https://www.ncbi.nlm.nih.gov/books/NBK553086/ - Gray baby syndrome; National Library Of Medicine
https://www.ncbi.nlm.nih.gov/books/NBK448133/ - A Note on Gray Baby Syndrome; Endocrinology and Metabolic Syndrome
https://www.longdom.org/open-access-pdfs/a-note-on-gray-baby-syndrome.pdf
Community Experiences
Join the conversation and become a part of our nurturing community! Share your stories, experiences, and insights to connect with fellow parents.
Read full bio of Dr. Wayne Hough
Read full bio of Dr Bisny T. Joseph
Read full bio of Rohit Garoo
Read full bio of Shinta Liz Sunny
















