Image: ShutterStock
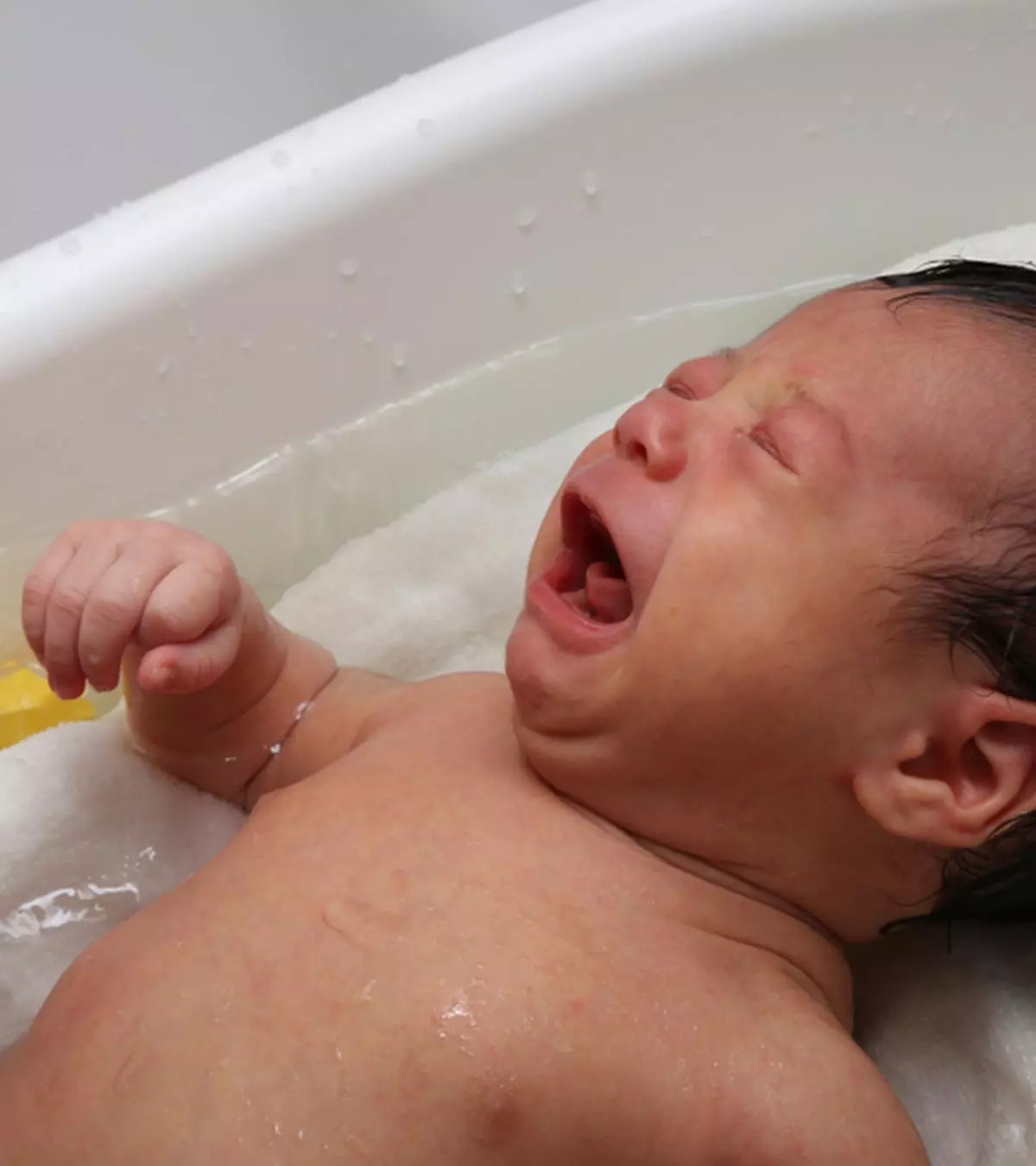
Human immunodeficiency virus (HIV) gives rise to AIDS (acquired immunodeficiency syndrome). HIV in babies or Pediatric HIV is also known as congenital HIV or neonatal HIV. The virus may cause opportunistic infections in babies by attacking and weakening their immune system (1) (2).
Babies acquire congenital HIV from their mothers during pregnancy, labor, or breastfeeding. The spread of the disease is called vertical transmission or perinatal transmission of the disease. Most HIV infections in babies are caused by vertical transmission (3).
Read this post to learn about signs, causes, diagnosis, management, and prevention of HIV in babies.
Key Pointers
- Babies infected with HIV usually have no symptoms for the first two to three months.
- Lack of energy, weight loss, persistent fevers, etc., are a few early signs of HIV infection in babies.
- Babies with HIV need antiretroviral therapy (ART) for their entire life.
Signs Of HIV Infection In Babies
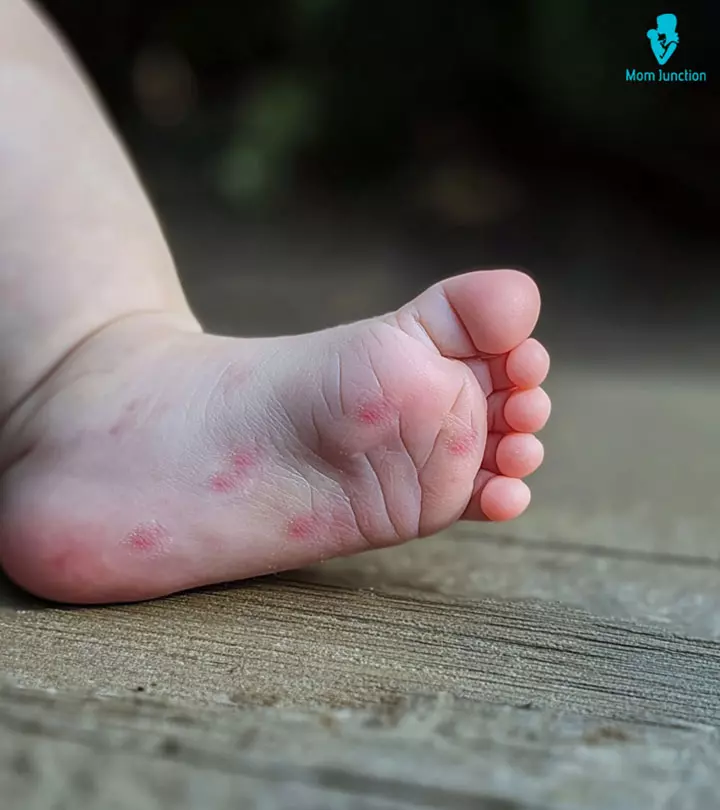
Infants infected with HIV most often do not have symptoms for the initial two to three months. Once the symptoms develop, the way they manifest varies from one baby to the other. Early signs of HIV in babies may include the following (1) (2).
- Lack of energy
- Weight loss and failure to grow
- Frequent and long lasting fevers

- Sweats
- Repeated or persistent yeast infection (candidaiA yeast genus capable of causing fungal infections in babies ) in the mouth
- Inflamed lymph nodes
- Inflamed salivary glands
- Enlarged liver
- Enlarged spleen
- Repeated ear infections
- Repeated sinusitisiA condition in which the tissues that line the sinus (hollow, air-filled spaces in the skull) get swollen or inflamed
- Repeated upper respiratory tract infections
- Developmental delays
- Diarrhea
- Recurrent herpesiViral infection marked by the formation of sores and blisters in and around the mouth and genital regions infections
- Recurrent bacterial infections
 Quick fact
Quick factDiagnosis Of HIV In Babies
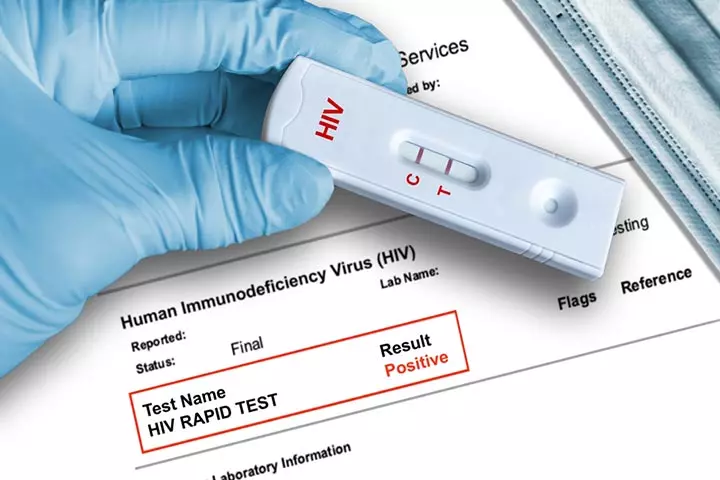
Babies born to HIV-infected mothers always have a positive antibody test at birth because the HIV antibody passively transfers across the placenta. Virological testingiA screening test used to identify HIV infection in infants is essential to confirm the diagnosis. Viral testing for HIV is done in babies at the following ages.
- 14 to 21 days
- One month
- Four months
If two tests come back negative, the infant does not have an HIV infection, and if two tests show positive results, the baby has an HIV infection. Babies who fall under the high-risk category for HIV transmission might be tested before the infant is 48 hours old, followed by testing at the requisite ages (1) (4).
Prevention And Medications For HIV In Babies
Dr. Anthony Puopolo, California-based chief medical officer at LifeMD and founder of Integrated Medical Wellness Group, says, “Vertical transmission of HIV can be prevented through maternal testing, effective control of the maternal infection, prenatal antiviral therapy as well as treating the mother and infant during labor and the neonatal period, and avoiding breastfeeding.”
Treatment for pregnant women identified as HIV-positive can prevent the transmission of infection to their babies. The treatment plan for HIV-positive pregnant women may consist of the following modalities (1).
- Antiretroviral therapyiA treatment modality for HIV which uses a combination of medications to inhibit replication of the virus (ART) is the choice of treatment for HIV/AIDS.
- If a woman tests HIV-positive during pregnancy, a three-drug regimen of ART will be given.
- ART drugs are low-risk for the baby in the womb. However, the pregnant woman may have an ultrasound in the second trimester to assess the baby’s development.
- If a woman is diagnosed with HIV infection at a time close to her labor, intravenous ART drugs are administered immediately. This can reduce the risk of transmission by 10%.

A C-section may be advised to reduce the risk of transmission from the birth canal (4). The following treatment plan is followed for babies born to HIV-positive babies (1).
- Infants born to HIV-infected mothers are administered ART drugs within six to 12 hours after birth.
- The doctor may prescribe one or more antiretroviral drugs for six weeks after birth.
 Quick fact
Quick factHIV-positive women should refrain from breastfeeding their babies. In addition, mothers who are taking HIV medicines should also avoid breastfeeding (1).
According to the Centers for Disease Control and Prevention, all women trying to conceive should get themselves and their partners tested for HIV to ensure maternal health and fetal health. If either of the partners has HIV, the infected partner should take the HIV medicine daily to prevent transmission and stay healthy (5). Today, there are many medical treatments available that slow down the progression of the disease and the rate at which HIV weakens the immune system (4).
Long-Term Outlook For HIV-Positive Infants
Early diagnosis and neonatal care are critical for babies with HIV infection. Babies with HIV infection will need ART for their entire life. ART drugs do not cure the infection but slow down HIV replication, making it easier for the immune system to suppress the virus. The medicines should be taken as prescribed for them to work well. Parents must work closely with healthcare providers to monitor and adjust treatment as needed, as consistent care can help most babies with HIV/AIDS lead a normal lifespan.
 Point to consider
Point to consider
Frequently Asked Questions
1. How long can a person born with HIV live?
With proper treatment, people with HIV may not develop AIDS-related complications and may live a near-normal lifespan (7).
2. What is nevirapine used for in babies?
Nevirapine is an antiretroviral drug used to treat HIV infection. It helps reduce mother-to-child transmission of HIV during pregnancy (8).
3. Why do all babies born to HIV-positive mothers initially test positive?
Babies are usually tested thrice, from birth to 14 days; 1 to 2 months, and; 3 to 6 months of age. Babies get maternal antibodies during pregnancy, and the initial HIV test may react to those HIV antibodies. A second test may be required for confirmatory results (9).
If you are HIV-positive, it is important to take your doctor’s advice before getting pregnant. HIV-positive mothers may transmit the infection to their babies during pregnancy, delivery, or breastfeeding. This infection could gradually progress into AIDS. Preventing viral transmission of HIV infection could protect the babies. In case of any doubt, it is better to consult your doctor and get the much-required guidance on the vaccines and other aspects related to HIV in babies. It is also important to take the best care of yourself after delivery for your baby’s well-being.
Infographic: Symptoms Of HIV Infection In Babies
Neonatal HIV infection causes the immune system to malfunction, making the infant susceptible to opportunistic infections. However, it is important to note early signs and symptoms as it improves the success rate of available treatments. The infographic below summarizes such manifestations.
Some thing wrong with infographic shortcode. please verify shortcode syntaxAn HIV-positive baby from Mississippi has achieved freedom from infection! Witness the incredible tale of optimism and strength in this captivating video.
References
1. HIV/AIDS in pregnant women and infants; U.S. National Library of Medicine
2. Congenital HIV; Nicklaus Children’s Hospital
3. Congenital HIV Symptoms & Causes; Boston Children’s Hospital
4. AIDS/HIV in Children; Stanford Children’s Health
5. Preventing HIV; Centers for Disease Control and Prevention
6. Evaluation and Management of the Infant Exposed to HIV in the United States; American Academy of Pediatrics
7. HIV and AIDS; National Health Service, UK
8. Nevirapine use to reduce mother-to-child transmission of HIV in Canada; National Library of Medicine
9. Testing HIV Positive During Pregnancy; DC Health
10. Neonatal HIV; U.S. National Library of Medicine
11. HIV Home Care; Stanford Children’s Health
Community Experiences
Join the conversation and become a part of our nurturing community! Share your stories, experiences, and insights to connect with fellow parents.
Read full bio of Dr. Ashraf Kasem
Read full bio of Dr. Ritika Shah
Read full bio of Rohit Garoo
Read full bio of Vidya Tadapatri