Image: iStock
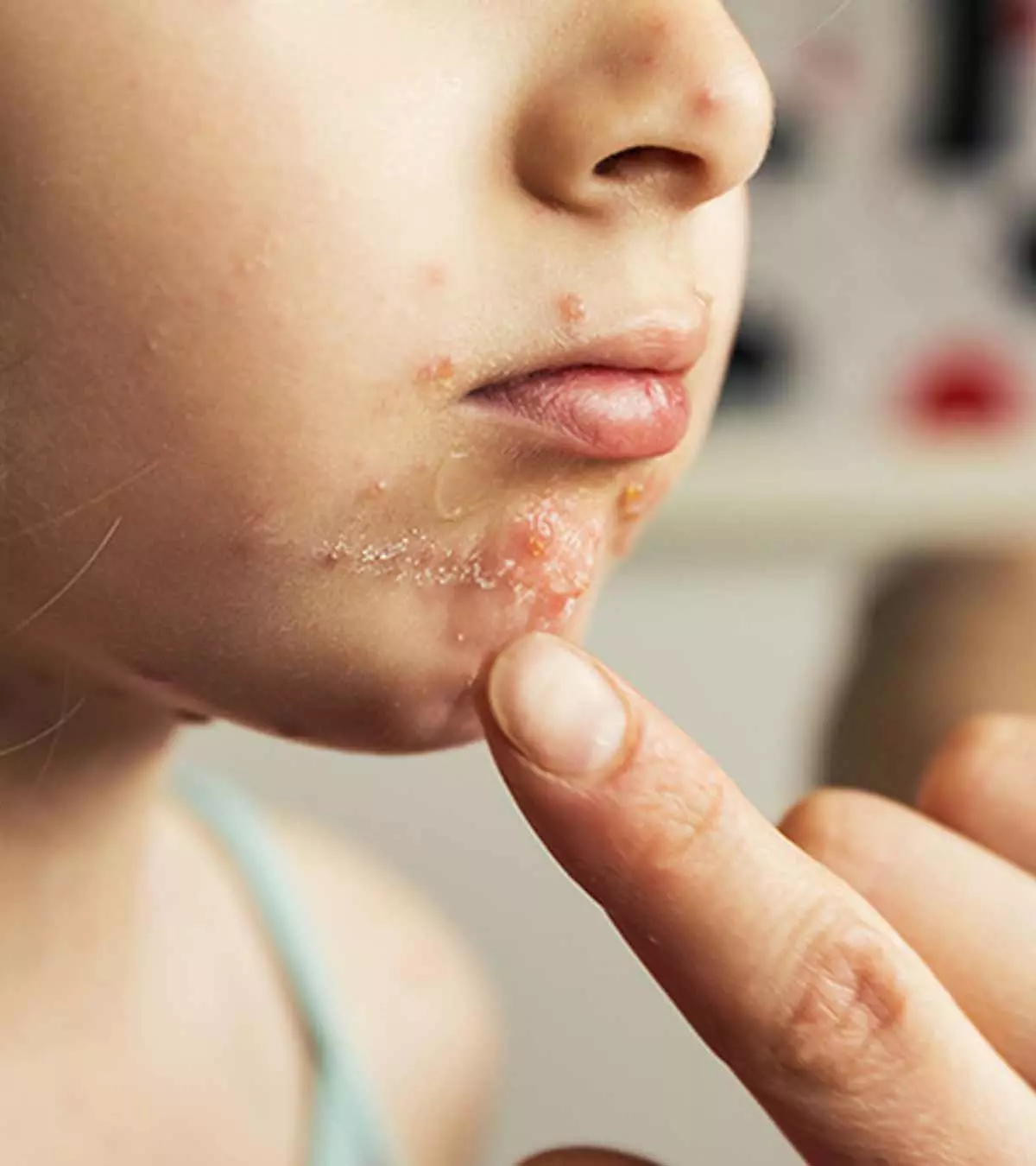
Hand, foot, and mouth disease in children is a highly transmissible viral infection, particularly in young ones. Fever is the first symptom, followed by rashes on the lips, hands, and feet. You may also be concerned that the rashes will spread from one part of the body to another.
Although hand, foot, and mouth disease (HFMD) is not a life-threatening infection, it can make your child uncomfortable, especially when drinking and swallowing food. It is particularly prevalent in childcare and educational institutions. Thus, it is crucial for parents and caregivers to know the symptoms and routes of transmission to provide prompt treatment and prevent further spread among children.
Read on to learn more about HFMD in children, including treatment options and home remedies, as well as how it can be prevented.
Key Pointers
- HFMD is a contagious viral infection that affects children during summer or fall, causing symptoms such as fever, fatigue, loss of appetite, and rash on hands, feet, and mouth.
- Contamination through contact with saliva, contaminated objects, soiled surfaces, or skin contact with an infected person can cause HFMD in kids.
- Seek medical attention if symptoms persist beyond ten days or if there is severe dehydration.
- Dealing with HFMD requires proper clinical diagnosis and treatment, hydration, consumption of cold and soft foods, and gargling with warm water.
What Is Hand, Foot, And Mouth Disease?
Hand, foot, and mouth disease is one of the contagious viral infections in children, usually affecting children younger than five years of age. However, it can happen in adults as well.
The disease is characterized by sores in the mouth and a rash on the hands and feet, and occurs mostly during the summer and fall (1).
It is generally mild, self-limiting, and goes away in a few days.
 Quick fact
Quick factWhat Causes HFMD In Children?
Hand, foot, and mouth disease is caused by the coxsackievirus, mostly coxsackievirus A16.
Coxsackievirus belongs to a group of viruses called enteroviruses.
Other types of enteroviruses can also cause HFMD. But Coxsackievirus A16 and Enterovirus 71 have been mostly associated with HFMD outbreaks in children (2).
HFMD is highly contagious and spreads easily from person to person. Your child may contract hand, foot, and mouth disease by coming in touch with an infected person’s:
- Saliva. It can directly transmit the virus to your child. Even sharing the same cup or plate, stationary, towel can make it contagious.
- Respiratory droplets such as a sneeze or cough. If your kid comes in contact with an infected person’s cough or sneeze, or breathes in the same air, they can get infected.
- Fluids from the blisters. Your child can contract the disease when they touch or come in skin contact with the fluid discharge from blisters on another child.
- Feces. HFMD virus can also transmit through the fecal-oral route. So, if kids touch soiled diapers or come in contact with a soil or surface contaminated with feces of an infected person, they may catch the virus.
- Skin contact with an infected person. A close physical contact, such as a handshake or a hug, can be a source of infection.
- Contact with any object that is infected. Viruses can survive on inanimate objects; therefore, touching an object used by an infected person can transmit the virus.
If somebody in your family, close neighborhood or the child’s daycare is having the disease, then your child is likely to get it. It commonly spreads in day care centers, schools, playgroups, close contact sports, families living in congested quarters. Therefore, keep an eye on the symptoms.
What Are The Symptoms Of Hand, Foot, And Mouth Disease?
Symptoms begin to show three to six days after contracting the infection. This period is known as the incubation period.
Your child may show some or all of these symptoms:
- Mild fever of around 102oF

- A sore throat and a scratchy feeling in the throat that is often painful due to lesions
- Poor appetite
- A headache
- Painful red sores or ulcers inside the mouth, affecting the roof of the mouth, gums, and inner walls
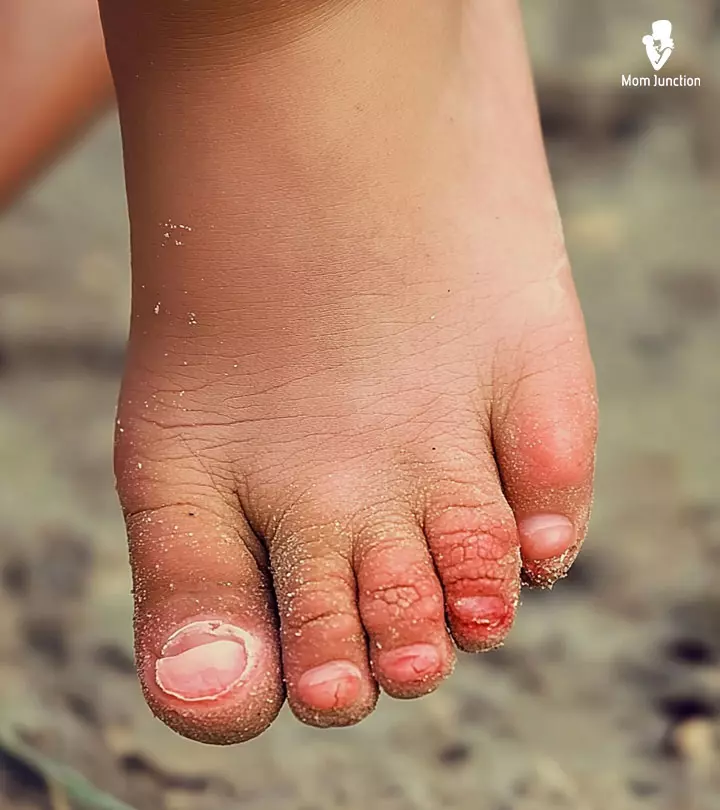
- Red rashes on the palms, soles, and in the buttocks
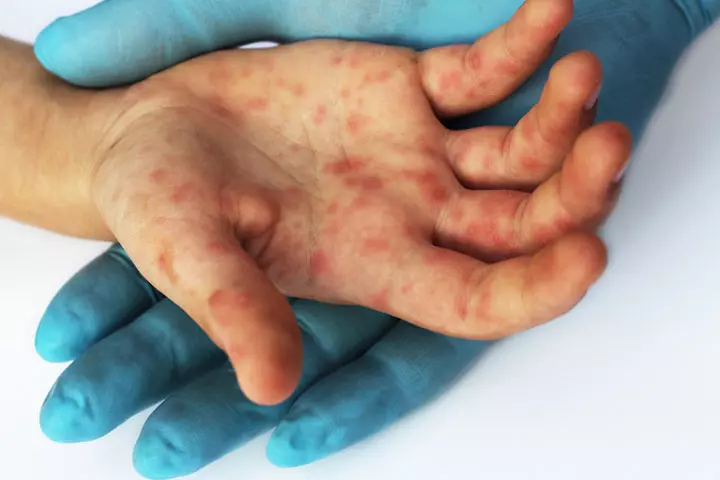
The first symptoms are usually a fever followed by a sore throat and loss of appetite in children in a day or two. The rashes appear one to two days after the fever starts. Painful blisters may appear inside the mouth (herpangina) within a day or two. This makes it difficult for the child to swallow.
Tiffany Lim Baura, a mother of two, shares her experience dealing with her children’s symptoms when they had hand, foot, and mouth disease. She says, “My two-year-old daughter developed a fever for two days. On the second day, I noticed that she started to develop some red rash around her mouth. I initially thought this was just some sort of allergy. I later noticed that the rash looked like chicken pox sores. It sort of had blisters, and she kept on scratching them, so I knew they were a little bit itchy. She also started complaining of ‘ouchy’ inside her mouth the same day. When I checked, I saw one sore on her palate. This caused her to cry each time she was fed solid food (i).”
 Point to consider
Point to considerWho Is At The Risk Of Getting HFMD?
Young children below ten years, often below five years, are at the highest risk of contracting the disease.
Those attending a daycare or school can contract the infection as viruses spread quickly at places where there are several children. Also, children living in closed and crowded neighborhoods are at increased risk.
What Are The Complications Of HFMD?

Usually, HFMD runs its course and the affected child recovers on their own without any complications.
The greatest and most common complication is dehydration. The sores inside the mouth and throat make swallowing difficult, making the children reluctant to drink water. The mother needs to make sure the child has an adequate intake.
Any other serious complications are rare but children with low immunity are likely to have:
- Viral meningitis. This causes inflammation of the meninges or the membranes that surround the brain and spinal cord. Viral meningitis in children results in a headache, a fever, and a stiff neck.
- Encephalitis. The inflammation of the brain can be potentially fatal but is very rare.
As mentioned above, HFMD subsides on its own and doesn’t require a visit to a pediatric doctor. However, in some cases, you may have to.
When To See A Doctor?

You need to visit a doctor if:
The symptoms in your child exacerbate after a few days
- The mouth sores are too painful and prevent the child from drinking fluids
- Severe dehydration as the child doesn’t pass urine for more than eight hours or their mouth becomes very dry
- The symptoms are persisting even after ten days
The doctor will do a diagnosis to confirm if it is HFMD or any other infection.
How Is HFMD Diagnosed?
The diagnosis is mainly clinical. The doctor will ask the age of the child and about the symptoms; they will check for the body and mouth sores.
If the disease has been there for long or the symptoms are confusing, the doctor may also conduct a throat swab culture and take a stool sample for laboratory testing to identify HFMD and the virus that caused it.
Treatment For Hand, Foot, And Mouth Disease
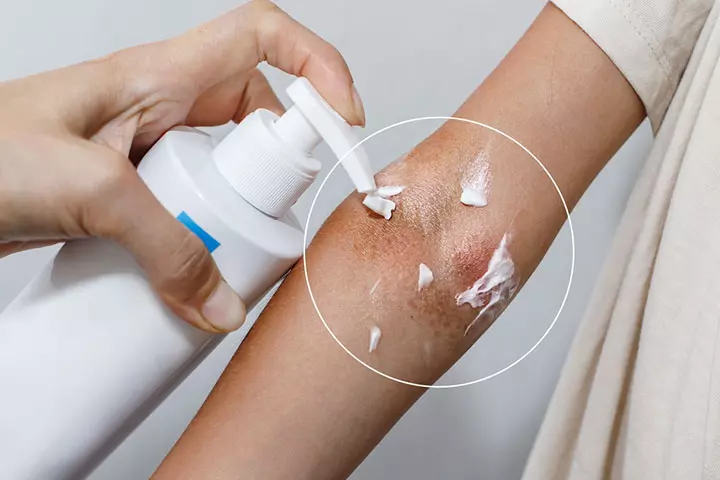
Treatment is not required as the infection goes away on its own in seven to ten days. However, your child’s doctor may prescribe a few medicines to reduce the fever or relieve the pain from the sores:
- Topical ointments and oral anesthetics to soothe the rashes and blisters
- Acetaminophen or ibuprofen for kids to relieve general discomfort, pain and headaches
- Medicated syrups for soothing sore throat pain.
- Anti allergics to relieve itching.
If you are not keen to use painkillers and soothers, you may try some relief methods at home.
Maddison Miller, a mother, emphasizes a crucial point about treating HFMD in children, “You want to administer all types of gels with Q-tips and not your fingers; the reason is because it is extremely contagious with skin-to-skin contact (ii).”
Home Remedies For HFMD
Certain at-home remedies can improve the symptoms of hand, foot, and mouth disease:
- Give your child popsicles to suck when the mouth blisters become very painful. They soothe the sores as well as hydrate the body.
- Have your child gargle with lukewarm water and salt to alleviate the mouth and throat sores.
- Offer cold and soft foods like ice cream and juices instead of solid foods.
Based on her experience with her children’s hand, foot, and mouth disease, Baura adds, “Ice is a soother! When the kids were crying from sores in the mouth or throat, I gave them ice. That relieved them of the pain somehow. I also made a lot of ice candies for them so that it’s more fun to eat. This also helps to keep them hydrated since my children found it painful to drink water on the first two days.”
- Have your child drink water and other fluids to prevent dehydration.
- Do not give citrus fruits, soda or carbonated drinks.
- Avoid spicy and salty foods as they may irritate the mouth sores.
If you do not want any of this trouble for the child or you, you may take these childcare measures to prevent the infection.
How To Prevent Hand, Foot, And Mouth Disease?
You may take the below steps to prevent HFMD:
- The best means to prevent this illness is to practice good hygiene. Have your children wash hands with soap and water after using the washroom, and before and after eating.
- Teach young kids not to put their hands or any object in their mouth.
- Make sure your child does not share stationary or other objects with other kids in school or daycare.
 Experts say
Experts say- Separate towels and bed sheets if someone in the family develops the disease.
- Disinfect common areas in your home, especially shared areas and surfaces, regularly. Disinfect your kid’s toys and other commonly used objects.
- If your child is suffering from fever or rashes, have him or her stay at home until they get better. This will avoid spreading the infection to others.
- Teach them to cover their mouth before sneezing or coughing; this will contain the spread when they have the infection.
- If someone in your family is having HFMD, keep your child away from them.
Below we answer some of the most commonly asked questions on HFMD.
Frequently Asked Questions
1. If my child had HFMD previously, can he or she get it again?
Your child can get hand, foot, and mouth disease for the second time but it is rare. Kids do develop immunity against the virus that has caused it; however other strains of the virus can cause it.
2. How long is an infected person contagious?
If you or a family member contracts HFMD, you are the most contagious in the first week. They can still be contagious (although to a lesser extent) for a few weeks even after the symptoms go away.
3. Is HFMD and foot and mouth disease the same?
Hand, foot, and mouth disease is not related to foot and mouth disease (also known as hoof and mouth disease), which is an infection caused by viruses in cattle and farm animals. A human being can neither contract it, nor can they transmit hand, foot, and mouth disease to animals.
4. Can siblings go to school if one has a hand, foot, and mouth disease?
According to the American Academy of Pediatrics, if a child has been diagnosed with HFMD and they do not have fever, open blisters, and are not experiencing uncontrolled drooling with mouth sores, they can go to school. Therefore, if the siblings are asymptomatic, there is no reason for them to miss school (4).
5. How can I prevent the spread of hand, foot, and mouth disease between siblings?
Hand, foot, and mouth disease in children is a transmissible viral infection they often contract in schools or daycares. The infection first starts as a mild fever. Then, rashes and painful blisters may appear. Children may experience headaches or poor appetite during this time. Consult a doctor if the mouth sores are painful, and children cannot swallow properly. They may suggest topical ointments and anti-allergics for relief. You may help soothe the rashes at home by giving them enough water, offering soft and cold foods, and avoiding citrus fruits. HFMD, although uncomfortable, rarely leads to any complications. The infection clears out in a few days.
Infographic Topic: What Are Atypical Symptoms Of Hand, Foot, And Mouth Disease In Children?
Hand, foot, and mouth disease may occur with atypical clinical features such as neurological symptoms and severe skin lesions. There is a higher possibility of delay in identification and treatment in atypical HFMD. Go through the infographic to know the atypical symptoms of hand, foot, and mouth disease. Illustration: Momjunction Design Team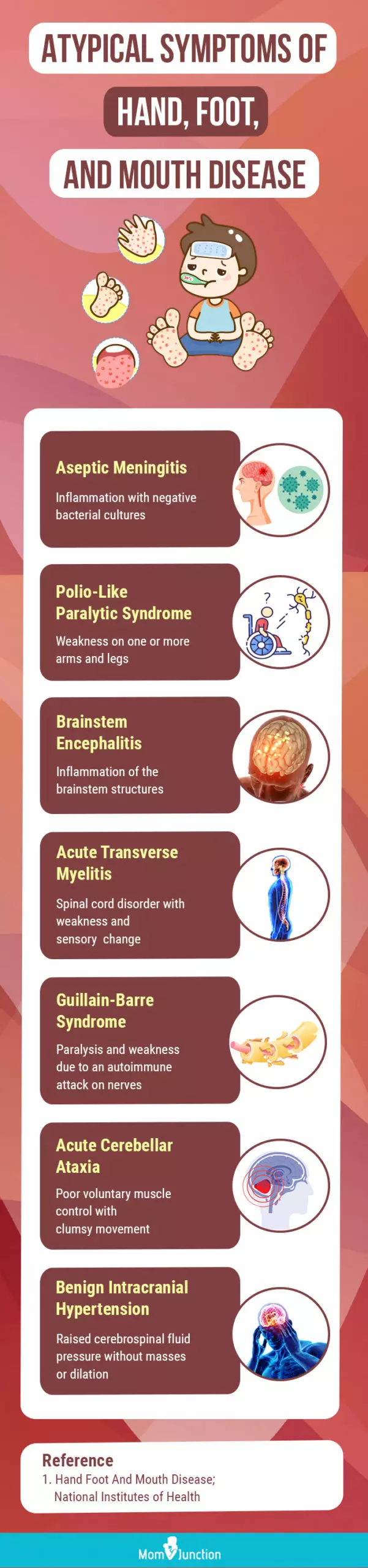
In this informative video, learn about the rash associated with hand, foot, and mouth disease and discover helpful tips for parents to alleviate their child’s discomfort.
Illustration: Hand Foot & Mouth Disease In Children: Symptoms & Treatment
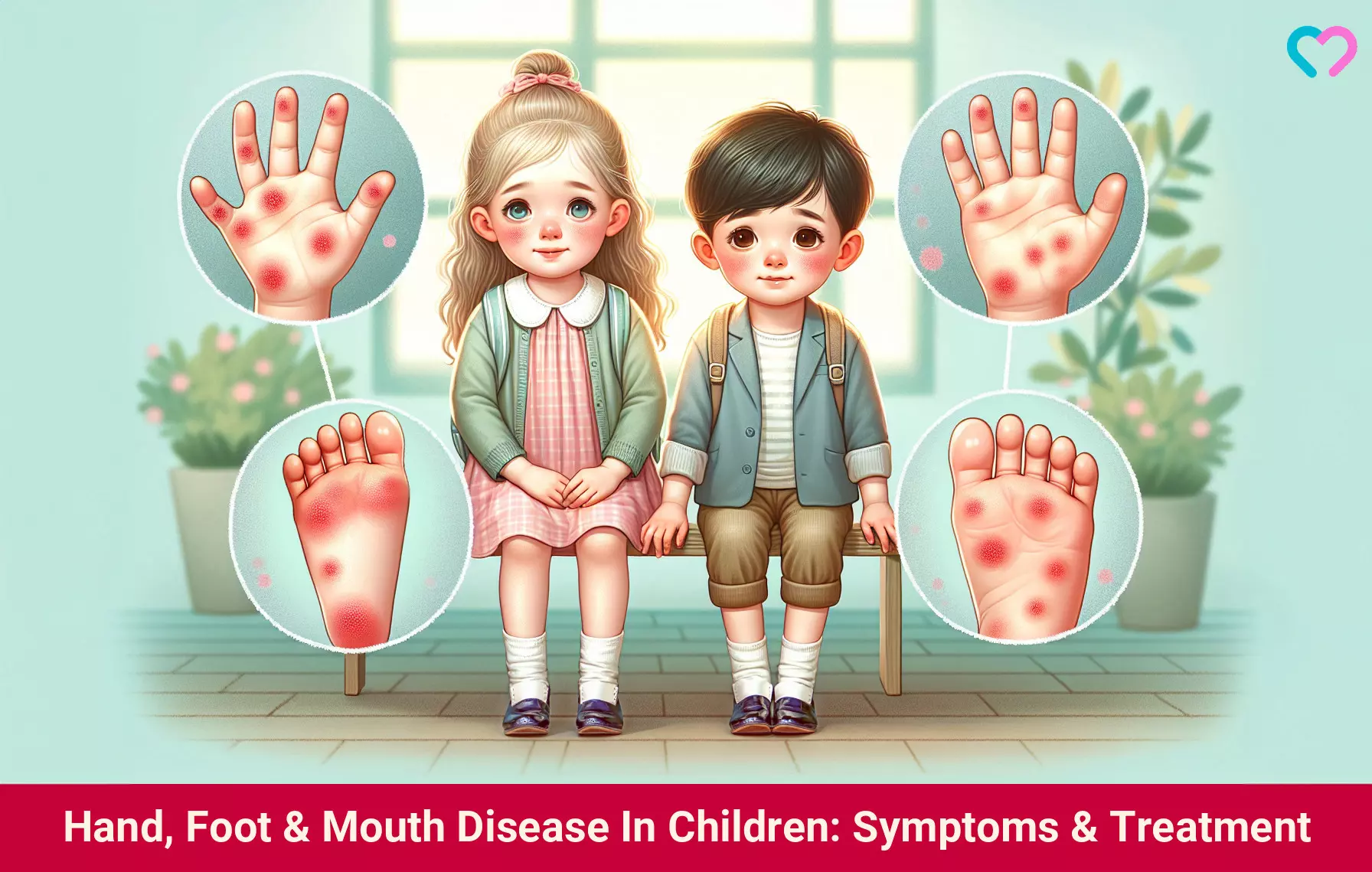
Image: Dall·E/MomJunction Design Team
Personal Experience: Sources
MomJunction articles include first-hand experiences to provide you with better insights through real-life narratives. Here are the sources of personal accounts referenced in this article.
i. Our experience with Hand, Foot, and Mouth Disease (HFMD).https://densandfan.blogspot.com/2013/07/our-experience-with-hand-foot-and-mouth.html
ii. Treating hand foot mouth disease & impetigo! | hardest week ever!.
https://www.youtube.com/watch?v=Pos8l-RjIJo
References
- Hand foot and mouth disease.
https://www.nhs.uk/conditions/hand-foot-mouth-disease/ - HFMD: Causes and How It Spreads.
https://www.cdc.gov/hand-foot-mouth/causes/?CDC_AAref_Val=https://www.cdc.gov/hand-foot-mouth/about/transmission.html - HFMD Symptoms and Complications.
https://www.cdc.gov/hand-foot-mouth/signs-symptoms/?CDC_AAref_Val=https://www.cdc.gov/hand-foot-mouth/about/complications.html - Hand Foot & Mouth Disease: Parent FAQs.
https://www.healthychildren.org/English/health-issues/conditions/infections/Pages/Hand-Foot-and-Mouth-Disease.aspx - About Hand Foot and Mouth Disease.
https://www.cdc.gov/hand-foot-mouth/about/index.html#:~:text=
Community Experiences
Join the conversation and become a part of our nurturing community! Share your stories, experiences, and insights to connect with fellow parents.
Read full bio of Dr. Mubina Agboatwalla
Read full bio of Dr Bisny T. Joseph
Read full bio of Swati Patwal
Read full bio of Anindita Ghatak