Image: Shutterstock
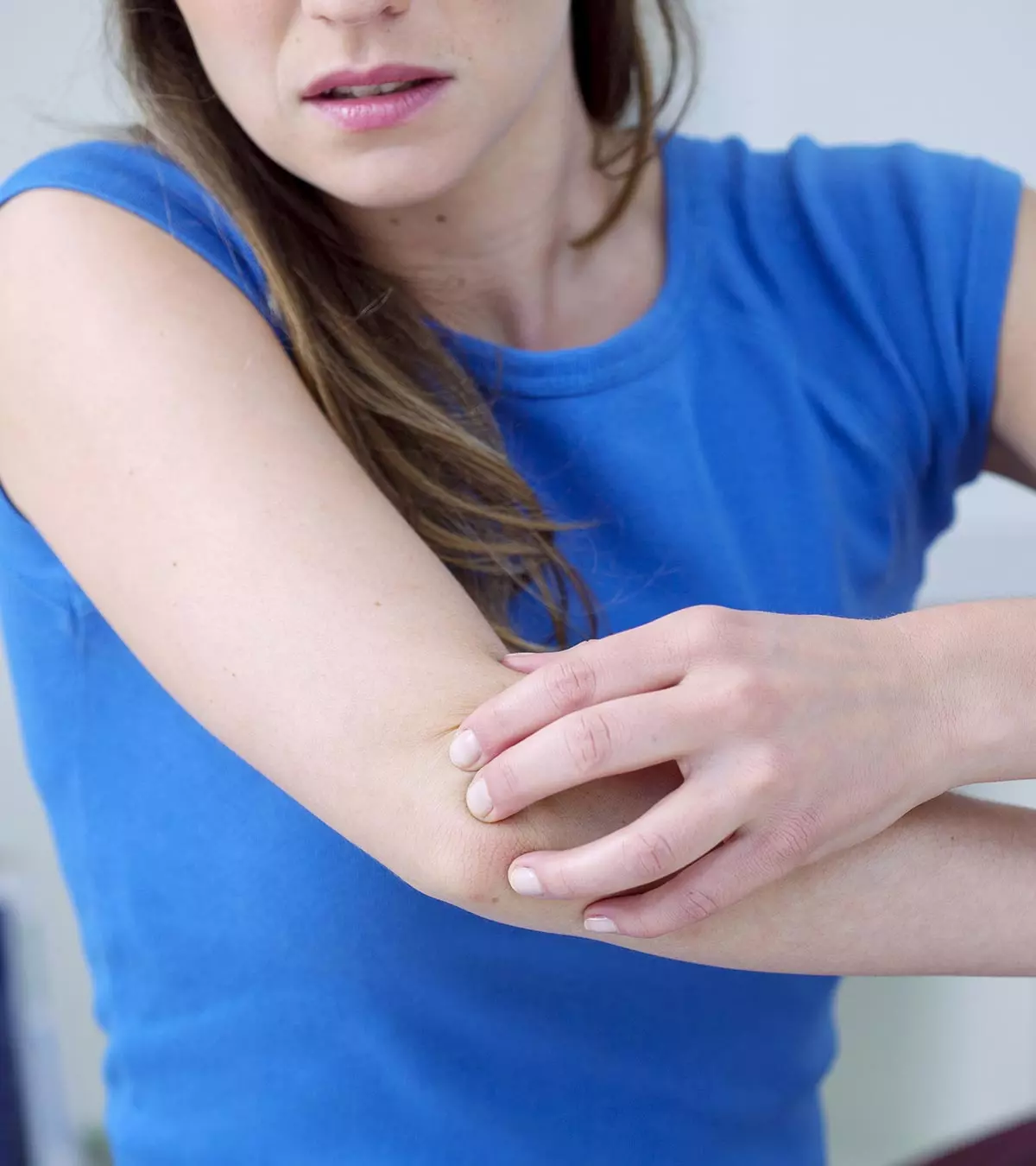
If you are experiencing hives while breastfeeding, you may fear transferring them to your babies. Hives commonly occur as rash-like bumps on the skin that are itchy and reddish in appearance. In addition, they may appear when the body reacts to an allergen.
Hives are mostly treated with antihistamine drugs; however, they may affect your baby since the drug passes into the breast milk. Therefore, it is important to consult your doctor about the safety of antihistamines and the right way of using them before you adopt the treatment.
Read about the causes of hives, their symptoms, diagnosis, and the treatment options for nursing mothers.
Key Pointers
- Hives are commonly caused by insect bites, excessive sweating, or exposure to pollen.
- Common symptoms of hives include redness of the skin and itching.
- Applying a cold compress and wearing loose-fitting clothes can help relieve the symptoms.
- If signs of breathlessness and swelling of lips and eyes occur, consult with the doctor immediately.
What Are Hives?
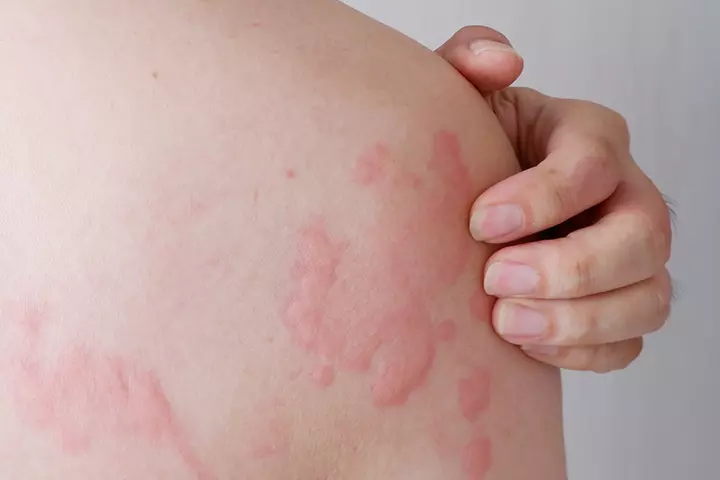
Your body’s reaction to an allergen can trigger hives. Nettle rash and urticaria, are other popular names for hives. It causes skin irritation and makes your skin break out in red and itchy rashes that look like little bumps on your skin. If you have hives, you will experience an itching and stinging or burning sensation.
Hives can appear anywhere on your body, including your face, lips, arms, throat and even ears. The rashes may be as small as a regular eraser to as big as a meal plate. Sometimes, multiple rashes can join to form a big patch or plaque (1).
What Causes Hives?

When your body reacts against an allergen, it produces the protein histamine as well as certain other chemicals. As your body releases histamine, the blood vessels in your skin leak blood plasma. It could cause swelling, itching and rashes.
Here are some of the most common causes of hives during breastfeeding:
- Pollen
- Drugs like aspirin, other nonsteroidal anti-inflammatory medications such as ibuprofen, high blood pressure drugs or painkillers such as codeine may also cause hives.
- Bites by insects and bugs
- Animal dander especially from cats
- A food allergy caused by the consumption of nuts, eggs, fish, chocolate, berries, shellfish, and more. Milk allergy may also cause hives. Foods that contain additives and preservatives may also trigger hives.
In addition to common allergens, hormonal fluctuations during the postpartum period can increase sensitivity to environmental factors and trigger hives in some women.
Sometimes, hives can be caused by the following factors.
- Excessive sweating
- Stress, especially emotional stress
- An infection, especially mononucleosisiA contagious viral infection that typically spreads through the saliva.
- Excessive exercising
- Extreme cold or excessive exposure to sun
- Illness, including lupusiAn autoimmune disease causing inflammation and damage to several organs in the body. , other autoimmune diseases, and leukemiaiA cancer of blood-forming cells and tissues impacting the immune system and normal body functioning.
 Do remember
Do rememberWhat Are The Symptoms Of Hives?

Some common symptoms of hives include the following:
- Itching (pruritus)
- Appearance of red or skin-colored welts with defined edges.
- Plaques that enlarge, spread, and join to form larger areas of flat rashes.
- You know you have hives when you press the center of a plaque, and it turns white.
- Chronic itching that may last longer than the initial rash
- Recurring episodes of hives over weeks or months
 Be watchful
Be watchfulHow To Diagnose Hives?
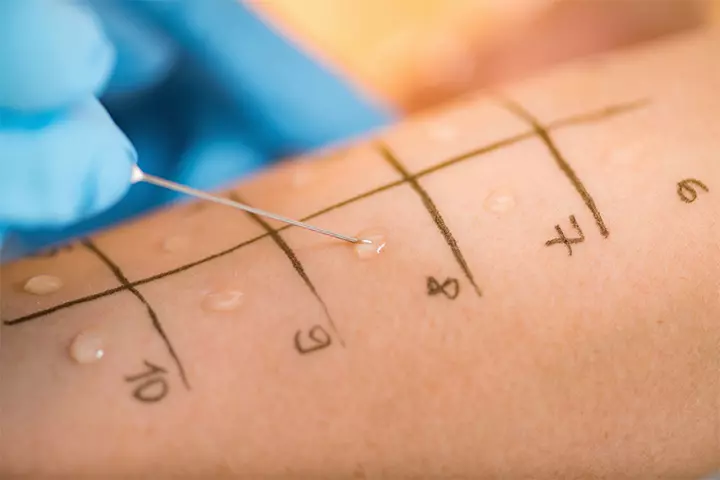
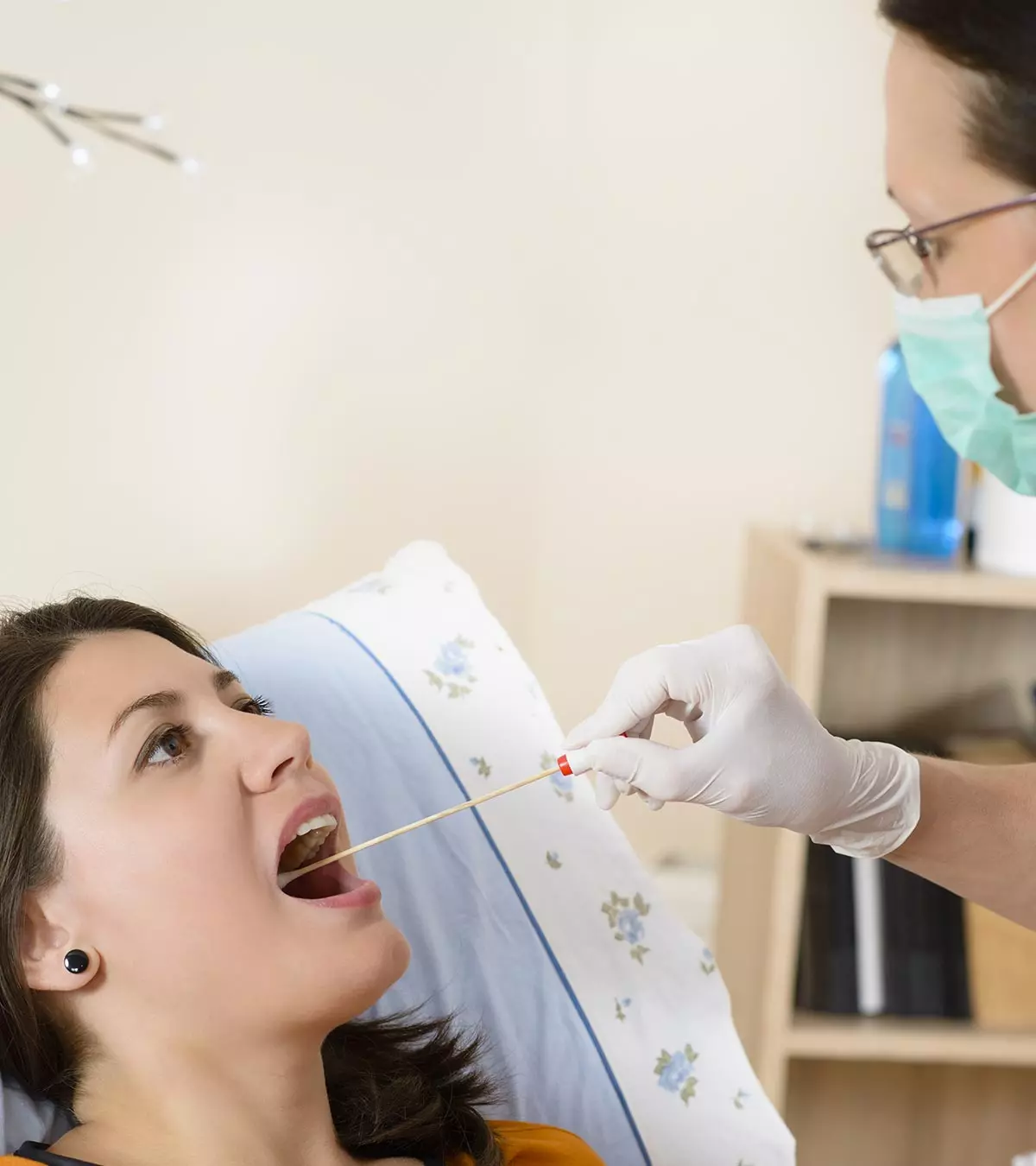
A doctor can diagnose hives during a physical examination. They may enquire about any history of allergies you have had. They may advise a skin and blood test to identify the exact cause of hives. An allergy blood test measures the immunoglobulin E (an antibody) in your body. The more the antibody, the more is the chance for allergy to be diagnosed.
A mother of four who goes by the pen name ‘Arizona Girl’ shares her experiences with allergy testing. The testing became necessary when she developed postpartum hives while breastfeeding. She reveals, “Allergy testing showed that I am allergic to a lot of environmental things. Even if my hives are being caused by hormonal changes, they can be worsened by environmental factors or food allergens. We have used this information to try to limit the effects of my environment. I am now at a point where I can live with my hives (i).”
When To Seek Medical Help?
You should seek immediate medical help if you experience
- Breathlessness
- Inflammation in your throat, face or tongue
- Wheezing
- Infected bumps
- Hives or swelling lasting more than a week
- Swelling in eyes and lips
Treating Hives While Breastfeeding
Antihistamine drugs are one of the most common ways to treat a case of hives, but it is not the choice of treatment when you are breastfeeding. Antihistamines drugs can enter your bloodstream, permeate your breast milk and harm your baby. If you have contracted hives and are also breastfeeding, do not panic yet. Here is how you can start the treatment for hives while breastfeeding (2):
- Speak to your doctor the moment you notice the rashes. Make sure you inform your doctor that you are breastfeeding your baby. Your doctor may prescribe antihistamines that pass in the breast milk in minimal amounts. Discuss the potential effects the medication may cause you or your baby. Take it as soon as you feed your baby, as it will reduce your baby’s chances of exposure to the same.
- Check with your doctor if they can identify a specific allergen that triggered hives. Try and avoid exposure to the same to minimize further risk. If it is a food-related allergy, remove that from the maternal diet.
- Try using a cold compress that will soothe the itching or burning sensation due to hives.

Home Remedies For Treating Hives
For those dealing with mild hives, here are simple home remedies to ease the symptoms (3) (4) (5):
- Take a comfortably cool bath and add substances like baking soda, uncooked oatmeal, or colloidal oatmeal to soothe irritated skin.
- Wash with a fragrance-free cleanser. Ensure it is truly fragrance-free rather than just unscented, which can still irritate the skin.
- Ensure your skin does not get overheated.
- Use fragrance-free moisturizers multiple times daily to prevent dry skin, aiding in alleviating symptoms.
- Tracking your daily activities, meals, and surroundings can unveil the factors causing sudden hives. Identify and avoid these triggers to minimize future episodes.
These easy measures offer relief for minor hives. For persistent or frequent cases, seeking advice from a healthcare expert is vital for accurate diagnosis and treatment.
Frequently Asked Questions
1. How long do postpartum hives last?
Most postpartum hives may resolve in a few hours or a day, but some may continue for weeks or even months (6).
2. Why is my body so itchy after pregnancy?
Skin problems that occur during pregnancy may last for certain periods after childbirth. Pruritic urticarial papules and plaques of pregnancyiA skin condition causing intense itchy, red rashes in the belly area during pregnancy. (PUPPP) rashes may occur either in the later stages of pregnancy or shortly after childbirth. It usually affects the breasts, upper thighs, and arms (7).
3. Can I take Benadryl for hives while breastfeeding?
When you take Benadryl while breastfeeding, it passes into breast milk in small amounts and may not cause any side effects in your baby. However, it is better to see your doctor and make careful choices if there is concern about your or your child’s safety (8) (9).
4. Can I pass hives to my baby?
No, hives are not contagious, so you will not infect your baby or any other family members (10).
5. Can I get hives from a hormone imbalance?
Due to hormonal changes during pregnancy, women who have never had hives or allergies may get them. Hormonal changes may be one of the causes of postpartum hives, a common issue that many women experience after giving birth (10).
6. How can I manage hives long-term while breastfeeding?
Long-term management may involve identifying and avoiding specific triggers, maintaining a diary of symptoms and possible allergens, and regular follow-ups with your healthcare provider for personalized treatment options.
Hives are usually caused by pollen, allergy, or insect bites. The most common treatment option for hives is antihistamine drugs. However, the possibility of the drug components permeating the breastmilk and reaching the baby is high while breastfeeding, and hence you should try alternative remedial measures. Consult your doctor immediately if you are concerned about symptoms such as breathlessness, fainting, or are experiencing discomfort. Also, do not stress yourself during this situation as it might aggravate the condition.
Infographic: When To Seek Medical Help For Hives During Breastfeeding?
The symptoms and rashes caused by hives could make you uncomfortable while nursing and impact your feeding sessions. So, as this infographic explains, if you are experiencing prolonged or additional symptoms of hives during breastfeeding, it is time to talk to your healthcare provider as soon as possible.
Some thing wrong with infographic shortcode. please verify shortcode syntaxIllustration: How To Treat Hives While Breastfeeding?

Image: Dall·E/MomJunction Design Team
Watch this informative video to discover effective strategies for managing hives while breastfeeding. Learn gentle techniques to alleviate your infant’s skin irritation and promote their comfort.
Personal Experience: Source
MomJunction articles include first-hand experiences to provide you with better insights through real-life narratives. Here are the sources of personal accounts referenced in this article.
i. My hives (postpartum hives).https://arizonaforever.blogspot.com/2009/06/my-hives-postpartum-hives.html
References
- What causes hives?
https://www.aad.org/public/diseases/a-z/hives-causes - Hives (Urticaria) and Swelling (Angiodema).
https://my.clevelandclinic.org/health/diseases/8630-hives - Hives: Self-care.
https://www.aad.org/public/diseases/a-z/hives-self-care - 10 Ways To Get Relief From Chronic Hives.
https://www.aad.org/public/diseases/a-z/hives-chronic-relief - Home Remedies: Help with itchy hives.
https://newsnetwork.mayoclinic.org/discussion/home-remedies-help-with-itchy-hives/ - Hives / Urticaria.
https://www.columbiadoctors.org/treatments-conditions/hives-urticaria - Silonie Sachdeva; (2008); THE DERMATOSES OF PREGNANCY.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2763729/ - Miranda So et al.; (2010); Safety of antihistamines during pregnancy and lactation.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2868610/ - Antihistamines: Definition, Types & Side Effects.
https://my.clevelandclinic.org/health/treatments/antihistamines - About Postpartum Hives and Its Management; Revival Research Institute.
https://revivalresearch.org/blogs/postpartum-hives///
Community Experiences
Join the conversation and become a part of our nurturing community! Share your stories, experiences, and insights to connect with fellow parents.
Read full bio of Dr. Ashley Van Putten
Read full bio of Jessica Albert
Read full bio of Rohit Garoo
Read full bio of Shinta Liz Sunny