Image: iStock
Hypothyroidism in children, just as in adults, is a condition in which the thyroid gland produces insufficient thyroid hormone. The thyroid gland is a butterfly-shaped endocrine gland located below the larynx (voice box) in the front of the neck. It produces thyroid hormones, including thyroxine (T4) and triiodothyronine (T3), which are secreted into the bloodstream. The thyroid-stimulating hormone (TSH) which is produced in the brain causes the release of thyroid hormones.
These hormones regulate your child’s metabolism and energy utilization and ensure the brain, heart, kidney, and other organs function properly (1). Therefore, thyroid dysfunction or disorders can have profound detrimental effects (2) (3).
This post discusses the types, causes, symptoms, diagnosis, and treatment of hypothyroidism in children.
Key Pointers
- The symptoms of hypothyroidism in children may vary from adults and include puffy appearance, fatigue, and sore muscles.
- A family history of thyroid or autoimmune disorders could increase the risk of hypothyroidism in kids.
- The main treatment involves taking thyroid hormone replacement pills lifelong or until puberty is complete.
Hypothyroidism In Children
The main thyroid disorders are hyperthyroidism or excessive thyroid hormone production (overactive thyroid gland) and hypothyroidism or insufficient hormone production (underactive gland). Adults are more likely to have hypothyroidism, but it is the most common thyroid condition in children and teenagers (4).
The clinical presentation of hypothyroidism may vary among different children, and they may have different symptoms than adults. Many of these clinical manifestations are non-specific and may be overlooked as routine aspects of daily life (5) (6). Early detection of hypothyroidism is crucial, as it can lead to long-term health issues in children and significantly impact treatment outcomes.
Symptoms Of Hypothyroidism In Children
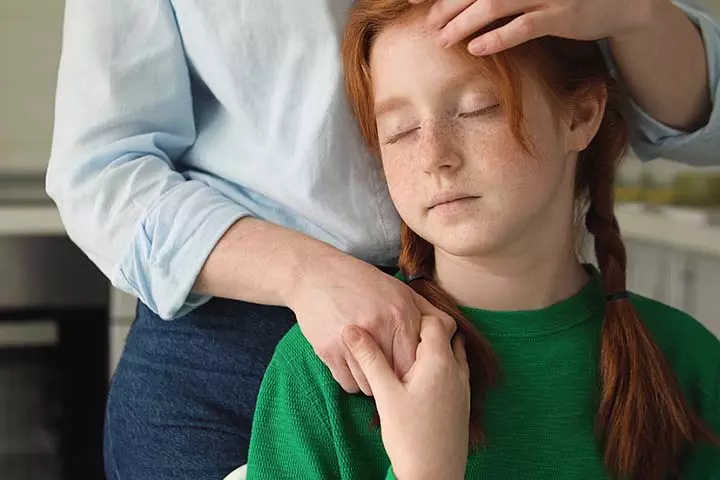
Hypothyroidism may go unnoticed since its symptoms develop slowly and resemble those of other diseases or medical conditions (5) (6).
However, according to the American Diabetes Association and the Pediatric Endocrine Society, children may exhibit the following hypothyroidism symptoms (2):
- Tiredness and decreased energy
- Swollen or puffy appearance
- Weight gain without increased appetite
- Slower growth rate
- Sore muscles
- Constipation
- Dry skin
- Brittle and dry hair
- Depression
Younger children may have delayed tooth development and short limbs (owing to a slower growth rate) (7)
. Meanwhile, older children may have delayed pubertal development and irregular or heavy menstrual periods. Children may also have increased sensitivity to cold (8).
 Quick fact
Quick factTypes Of Hypothyroidism In Children
Hypothyroidism is mainly of three types (9) (10)
- Primary hypothyroidism occurs when the thyroid gland cannot produce enough thyroid hormone on its own.
- Secondary (central) hypothyroidism occurs when the thyroid gland is normal, but the pituitary gland in the brain, which regulates growth and sexual development, functions abnormally.
- Tertiary hypothyroidism occurs due to a dysfunctional hypothalamus in the brain, which maintains the homeostasisiAbility of an organism to retain stable internal conditions in accordance with the external changes. of the body.
Hypothyroidism in children can be further subdivided as
- Hypothyroidism present at birth, which includes:
- Congenital hypothyroidism (CH): It is caused by fetal thyroid gland underdevelopment or dysfunction. It is a common illness that affects one in 4,000 to 5,000 babies born in the US. Due to its high prevalence, CH testing is included in newborn screening programs in all the US states (6) (11).
Recalling her daughter’s diagnosis of congenital hypothyroidism, Mandi, a mother of three, says, “He (the pediatric endocrinologist) walked in and explained that based on Margot’s (her nine-day-old daughter) newborn screen, she was being diagnosed with congenital hypothyroidism. A normal THL number for her thyroid would be 0.8, and hers was about 178. He didn’t even repeat blood work to make sure; he immediately started her on a daily thyroid medication that she would require for the rest of her life. He also explained that this occurs in 1 of 4,000 babies and predominantly in females, and how nothing I did or did not do during my pregnancy caused this to happen; it just occurs during fetal development (i).” - Transient hypothyroidism: It is caused by exposure to thyroid medication or the mother’s antibodies because of maternal hypothyroidism. It normally resolves on its own without requiring long-term therapy (1).
- Acquired hypothyroidism develops after birth, usually during late childhood or adolescence. Depending on the underlying cause, it can be further divided into autoimmune hypothyroidism and iatrogenic hypothyroidismiA thyroid gland dysfunction induced by a medication or a surgical treatment. (6).
- Subclinical hypothyroidism is hypothyroidism discovered at an early stage when the TSH is slightly higher than usual but the T3 and T4 levels are normal. Subclinical hypothyroidism is characterized by the absence of symptoms and major health consequences. It could be identified if your child experiences goiter or weight gain or has a significant family history of thyroid disease. It often resolves without medication (8)
Risk Factors For Hypothyroidism In Children

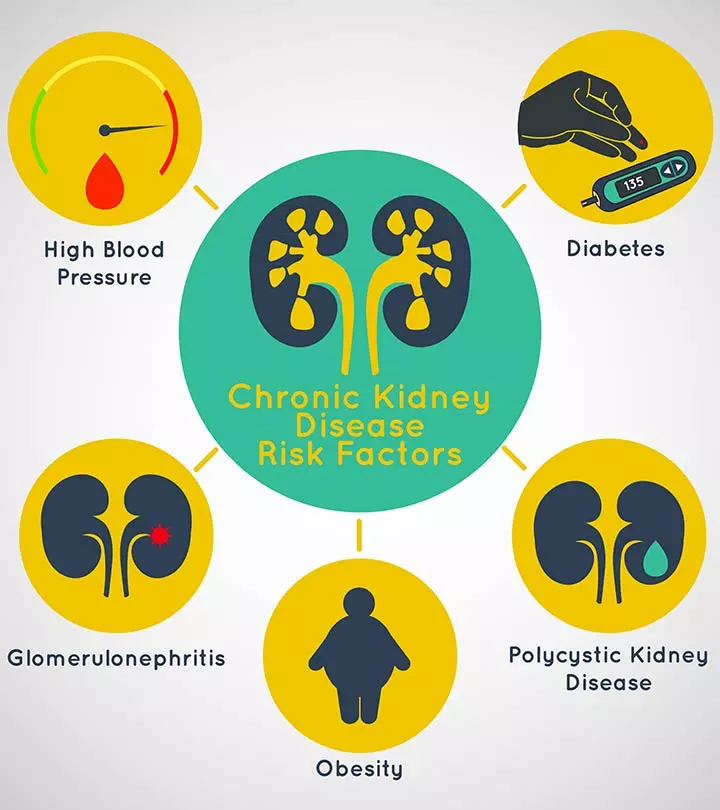
The following are some risk factors that may predispose your child to develop hypothyroidism (4) (12):
- History of thyroid problems, such as goiter (caused by insufficient iodine intake)
- An autoimmune disorder, such as type 1 diabetes or celiac disease
- History of surgery to correct a thyroid problem
- History of radiation treatment to the thyroid gland, head, neck, or chest
- Family history of thyroid disorders
- A chromosomal disorder such as Williams syndromeiA genetic condition caused by the deletion of specific regions on chromosome 7, leading to various physical and cognitive defects. , Down syndrome, or Turner syndromeiA chromosomal abnormality characterized by a single X chromosome in females.
- Thyroid gland injury
- Premature birth (7)
Causes Of Hypothyroidism In Children
The cause of hypothyroidism decides the type of hypothyroidism your child may be diagnosed with. Some causes of hypothyroidism in children include (6) (8):
- Autoimmune diseases in children, such as chronic lymphocytic thyroiditis (CLT) or Hashimoto’s thyroiditis, may cause autoimmune hypothyroidism, where the immune system attacks the thyroid gland, causing impaired thyroid function. CLT affects girls and teenagers more than boys and pre-adolescents. According to a meta-analysis published in Frontiers in Public Health, the prevalence of Hashimoto’s thyroiditis in North America was found to be 7.8%.
- Surgical removal or medical ablation of your child’s thyroid gland (or part of it) can cause iatrogenic hypothyroidism as their body can no longer produce thyroid hormones.
- Thyroiditis (inflammation of the thyroid gland) due to a viral infection can leak stored thyroid hormones, causing hyperthyroidism for a short time before the thyroid gland becomes underactive (hypothyroidism).
- Radiation treatment to the neck or head for conditions such as Graves disease in children can destroy or injure the thyroid gland, causing thyroid hormone dysfunction.
- Medicines such as Amiodarone, Lithium, Interferon-alpha, and Interleukin-2 can decrease thyroid hormone production.

- Damage to the pituitary gland may lead to insufficient TSH production, subsequently causing hypothyroidism.
Diagnosis Of Hypothyroidism In Children
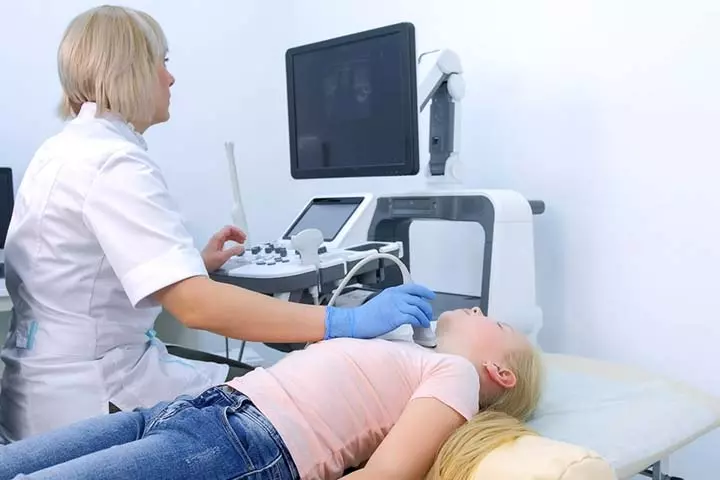
To diagnose hypothyroidism in children, your doctor may require (6) (13)
- Your child’s symptoms
- Your child’s medical and family history
- A physical examination
- Blood tests or thyroid function tests to check the TSH and T4 levels in the blood
- Thyroid imaging tests, such as a thyroid scan, ultrasound, or radioactive iodine uptake test
Children with a family history of thyroid disorders and those with autoimmune conditions need regular screenings for early detection of thyroid issues and prompt management.
 Point to consider
Point to considerTreatment For Hypothyroidism In Children

The purpose of hypothyroidism treatment is to restore the hormone levels to normal and support your child’s normal growth and development, depending on their age, overall health, and other factors. Your child may be referred to a pediatric endocrinologist, who treats children with hormonal problems (4).
The treatment mainly includes taking thyroid hormone replacement pills, such as Levothyroxine (T4 only) pills once daily, to boost the level of thyroid hormones in the body, also known as replacement therapy. Levothyroxine may be taken in the morning before food.
Your child may need to take these synthetic thyroid hormone pills lifelong (such as for iatrogenic hypothyroidism) or until their growth and puberty are complete. During the treatment, your healthcare provider will regularly check your child’s blood to see if the treatment is working, and their growth and development will be tracked over time (7).
Additionally, supplements such as calcium, iron, and vitamins are contraindicated with Levothyroxine and should be avoided during thyroid replacement therapy (8).
Complications Of Hypothyroidism In Children
Although hypothyroidism can be effectively managed with medication, if left undiagnosed or untreated, it can lead to various complications in children, including (5) (7) (10)
- Low levels of red blood cells (RBCs) (anemia)
- Low body temperature
- Heart failure or slower heart rate (bradycardia)
- Nervous system issues, such as lower IQ, speech delay, and impaired motor skills
- High cholesterol (hypercholesterolemia)
- Stunted physical growth or short stature
- Mental retardation
- Myxedema coma, where the body’s activities slow down to a point where it becomes life-threatening (rare)
- Cognitive impairment
- Hearing loss and eye problems
Frequently Asked Questions
1. At what age do thyroid problems begin in children?
Thyroid problems in children may be congenital, presenting themselves at birth, or acquired, developing between the ages of two and 18 (14).
2. Can a child outgrow hypothyroidism?
No, children may not outgrow hypothyroidism; however, they can lead a healthy life with the help of treatments. Doctors advise taking synthetic hormones that help children to grow normally and reach puberty on time (14). The child will need long-term management, including regular follow-ups to monitor thyroid hormone levels, adjust medication dosages, and assess growth.
3. Can hypothyroidism cause behavior problems in children?
Yes, hypothyroidism may cause behavior problems in kids because thyroid hormones influence metabolism. So, children with hypothyroidism may look passive and lack energy if they are not treated for the condition (14).
4. What lifestyle changes can support a child with hypothyroidism?
If your child is detected with hypothyroidism, it is vital to stick to their medication schedule and attend regular follow-ups. Additionally, you may make some lifestyle changes for your child, such as ensuring a well-balanced diet, maintaining stable blood sugar levels, reducing inflammation, and managing stress.
Hypothyroidism is one of the most common endocrine disorders of childhood. Hypothyroidism in children results from an underactive thyroid gland and thereby reduced production of thyroid hormones. The symptoms of hypothyroidism may be similar to many other childhood conditions. If you have a family history of or are concerned about your child’s symptoms, you should consult their routine pediatrician. If your child is diagnosed with hypothyroidism, it is important to give them the prescribed medication regularly and in an appropriate dosage.
Infographic: Can A Specific Diet Cure Hypothyroidism In Children?
There are no specific foods or dietary supplements to cure hypothyroidism and other thyroid disorders in children. Limiting excess calorie intake and changing a sedentary lifestyle could benefit maintaining a healthy weight. Go through the infographic to learn facts about the hypothyroidism diet to maintain a healthy weight.
Some thing wrong with infographic shortcode. please verify shortcode syntax
Illustration: Symptoms Of Hypothyroidism In Children Causes And Treatment

Image: Stable Diffusion/MomJunction Design Team
Learn about hypothyroidism in children and its causes, symptoms, and treatments. Get the facts to help your child live a healthy life.
Personal Experience: Source
MomJunction articles include first-hand experiences to provide you with better insights through real-life narratives. Here are the sources of personal accounts referenced in this article.
i. Congenital hypothyroidism.https://2tikesunder2.blogspot.com/2010/09/congential-hypothyroidism.html
References
- Hypothyroidism.
https://www.nationwidechildrens.org/conditions/hypothyroidism - Common Signs of Thyroid Disease in Children.
https://www.childrensdmc.org/parents/patient-and-family-resources/patient-and-family-resources/common-signs-of-thyroid-disease-in-children - Thyroid Function Anatomy and Hormones.
https://www.chop.edu/conditions-diseases/pediatric-thyroid-disorders - Hypothyroidism In Children.
https://www.cedars-sinai.org/health-library/diseases-and-conditions—pediatrics/a/hypothyroidism-in-children.html - Hypothyroidism (Underactive Thyroid).
https://www.niddk.nih.gov/health-information/endocrine-diseases/hypothyroidism - Hypothyroidism.
https://www.chop.edu/conditions-diseases/hypothyroidism - Acquired Hypothyroidism in Children.
https://www.urmc.rochester.edu/encyclopedia/content?contenttypeid=160&contentid=4 - Hypothyroidism in Children and Adolescents.
https://www.thyroid.org/hypothyroidism-children-adolescents/ - Nikita Patil et al.; (2026); Hypothyroidism.
https://www.ncbi.nlm.nih.gov/books/NBK519536/ - Vishal Gupta and Marilyn Lee; (2011); Central hypothyroidism.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3169862/ - Hypothyroidism In Children.
https://www.hopkinsmedicine.org/health/conditions-and-diseases/hypothyroidism-in-children - Thyroid Diseases.
https://medlineplus.gov/hypothyroidism.html - Hypothyroidism (Underactive).
https://www.thyroid.org/hypothyroidism/ - Could My Child Have Hypothyroidism (and Will It Go Away)?
https://health.clevelandclinic.org/could-my-child-have-hypothyroidism-and-will-it-go-away
Community Experiences
Join the conversation and become a part of our nurturing community! Share your stories, experiences, and insights to connect with fellow parents.
Read full bio of Dr. Arva M Bhavnagarwala
Read full bio of Reshmi Das
Read full bio of Dr. Ritika Shah
Read full bio of Dr. Joyani Das