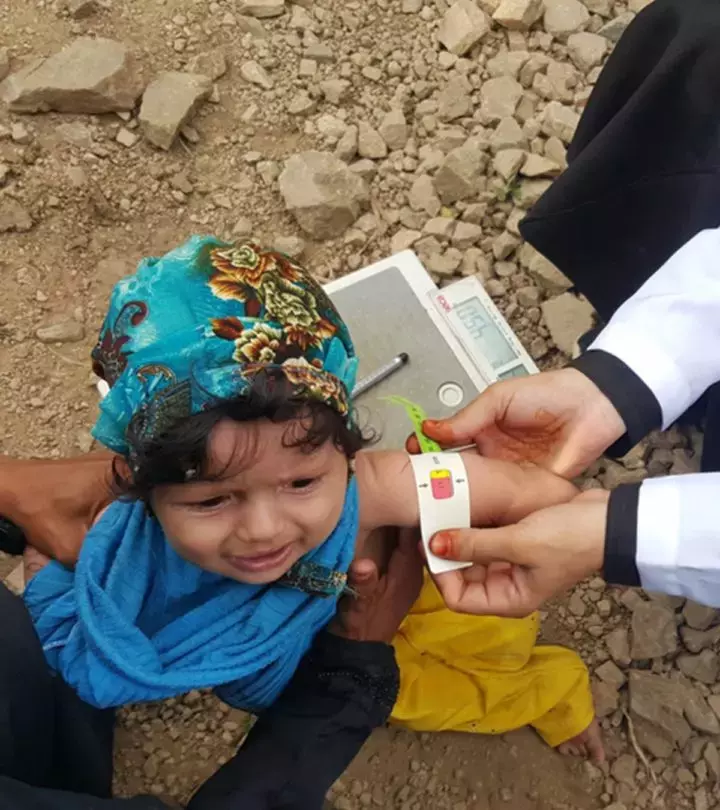
Image: Shutterstock
Malnutrition in children is defined as an imbalance in nutrient intake and utilization. Statistics suggest that 155 million children under five had stunted growth, while 41 million were overweight or obese in 2016 (1) (2). Growth stunting results from inadequate energy and nutrient intake, whereas overweight or obesity results from excessive intake.
Poor eating habits, nutritional malabsorption, and genetic predisposition are common causes of child malnutrition (3). Malnutrition also impacts a child’s growth, development, and general health. However, it can be mitigated by identifying and treating the exact cause and effects of the condition.
Read on to learn more about the causes and symptoms of malnutrition and how it can be treated and prevented in children.
Key Pointers
- Both undernutrition and overnutrition come under malnutrition.
- Poverty, underlying digestive issues, and poor mental health conditions may cause malnutrition.
- It is diagnosed through physical examination and anthropometric assessment.
- Supplementation and dietary changes are the primary sources of treatment for malnutrition.
Types Of Malnutrition
There are two types of malnutrition (1) (3).
1. Undernutrition
Undernutrition can be of many types depending on the deficient nutrient in the child’s diet
. A type of undernutrition that significantly affects a child’s growth is protein-energy undernutrition or malnutrition. It is associated with the insufficiency or deficiency of protein and energy in a child’s diet, hence protein-energy malnutrition.
This type of undernutrition can be acute or chronic, depending on the period of deficiency (4).
i. Acute malnutrition is a state in which a child has a below-average weight-for-height for a given age. It is caused by a sudden insufficiency of protein and energy, most commonly caused by an illness. Based on the severity of insufficiency or deficiency, the condition is further divided into:
- Kwashiorkor: In this condition, there is severely deficient protein intake. A child with kwashiorkor develops bilateral pitting pedal edema (accumulation of fluid in the feet and lower legs) and ascites (abnormal fluid retention in the abdomen). It is often called edematous malnutrition.
- Marasmus: It is a condition associated with insufficient intake of both total energy and protein, leading to wasting. Wasting is known as an excessive loss of adipose tissue and muscle due to protein and energy deficiency. It is also referred to as wasting syndrome.
 Quick fact
Quick factii. Chronic malnutrition, also known as stunting, is low height for age caused by prolonged or recurrent protein and energy deficiency. Stunting affects the physical and mental development of a child, affecting their overall quality of life. A malnourished child can be stunted, wasted, or both.
According to a joint report by WHO/UNICEF/WB, stunting has gradually declined since 2000, although the pace has been slow. However, wasting continues to be a persistent problem at an alarming rate, and there is a gradual increase in the trend of excessive weight gain (overweight), emphasizing the dual challenge of malnutrition.

Stunting, wasting, and overweight in children under five worldwide
Source: The UNICEF/WHO/WB Joint Child Malnutrition Estimates (JME) group released new data for 2026; WHO; UNICEF/WHO/World Bank Group Joint Child Malnutrition Estimates2. Overnutrition

Overnutrition is a state where the child gets more energy and nutrients than required. It is a chronic condition that results in excess weight gain when calorie consumption is more than calorie expenditure. Abnormal or excessive weight gain increases the risk of chronic health conditions, such as type-2 diabetes and cardiovascular diseases (CVD). Consumption of calorie-rich foods and less exercise put a child at the risk of overnutrition, which can ultimately lead to overweight/obesity. According to the National Institutes of Health (NIH), nearly one in five children in the US is obese, and they are more likely to develop adverse health issues.
Both undernutrition and overnutrition can lead to micronutrient deficiencies making the child prone to infections and illnesses. Iodine, vitamin A, iron, and zinc deficiency are some of the common deficiencies that affect malnourished children. Micronutrient excess has also been recognized as a cause of malnutrition in recent years.
 Quick fact
Quick factSigns And Symptoms Of Malnutrition
Signs and symptoms of malnutrition depend on its cause. They can be mild or severe based on the extent of malnourishment. Some of the common malnutrition symptoms warranting attention are the following (5) (6).
Signs and symptoms of undernutrition
- Lack of energy and lethargy
- Loss of appetite
- Unintentional weight loss
- Excessive loss of fat and muscle mass
- Changes in nail, hair, and skin quality and color
- Sunken eyes and hollow cheeks
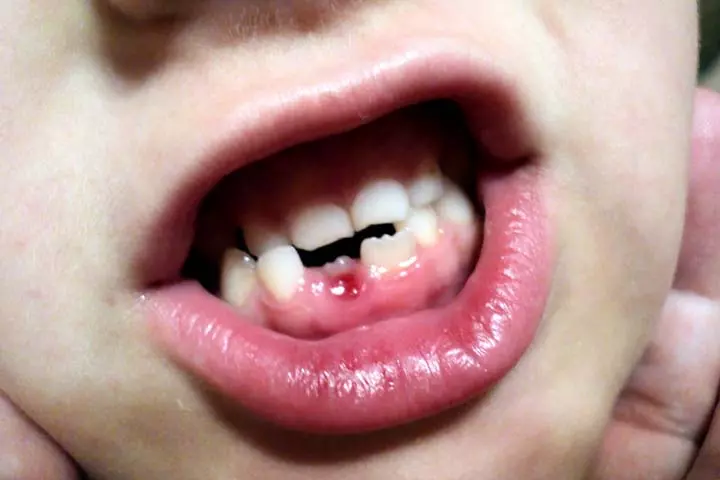
- Swollen bleeding gums and decaying teeth
- Mood swings and behavioral changes, such as irritability and anxiety
- Frequent illnesses and delayed recovery
- Failure to thrive, i.e., failure to grow (height and weight) as expected
- Poor mental development affecting learning
Signs and symptoms of overnutrition
- Unintentional weight gain in kids, which is often abnormal or excessive
- Changes in hair, nail, and skin quality and color due to micronutrient deficiencies
- Behavioral problems, such as social isolation and depression, due to excessive weight gain
- Development of chronic health conditions, such as type-2 diabetes
Malnutrition is a leading cause of fatality among children under the age of five years, especially in low- and middle-income countries (1). Evaluating the signs and symptoms can help identify the cause of malnutrition and mitigate its adverse effects. Delayed diagnosis can result in severe health problems and longer treatments. Thus, you should routinely check your child’s growth and development using growth charts and consult healthcare providers if any concerns arise.
Causes Of Malnutrition
A child could be at risk of undernutrition or overnutrition due to the following factors (7).
- Poverty: Unfortunately, even today, inadequate access to healthcare and poverty-induced starvation leading to insufficient access to nutritious food remain among the major causes of malnutrition globally.
- Poor dietary habits: Children with poor or erratic food habits are at risk of malnutrition. For instance, picky eaters are at risk of undernutrition in the long-term. On the other hand, if they overeat or eat foods high in calories regularly, they are at risk of overnutrition. In both cases, consuming a well-balanced diet and maintaining regular physical activity can help resolve the condition.
- Digestive conditions: Digestive health conditions, such as Crohn’s disease, inflammatory bowel disease, cystic fibrosis, and ulcerative colitis, affect the digestion and absorption of food, exposing the child to the risk of undernutrition. Similarly, some other conditions, such as dysphagia, pose difficulty in chewing and swallowing food, leading to undernutrition over time.
 Point to consider
Point to consider- Mental conditions: Depression and anxiety are mental health conditions that can either cause overeating or cause loss of appetite in children. Eating disorders affecting the eating pattern of an individual can lead to malnutrition. For instance, anorexia nervosa can restrict a child’s food intake, causing severe malnutrition over time. On the other hand, binge eating disorder can cause uncontrolled eating, resulting in overnutrition.

- Poor hygiene: Poor sanitation and hygiene practices cause the development of infectious diseases, such as diarrhea. Recurrent infections expose children to the risk of macro and micronutrient deficiencies, causing malnutrition (8).
- Chronic disorders: They commonly lead to loss of appetite with or without increased calorie and protein requirement to fight the disorder. Some common examples are tuberculosis, cancers, and liver and kidney diseases.
 Quick fact
Quick factBesides the above reasons, some medicines may suppress or increase appetite, resulting in under or overeating. All these factors take time to affect health, and malnutrition does not happen overnight. A timely diagnosis can thus prevent any long-term consequences.
Diagnosis Of Malnutrition
A doctor will collect the child’s family, medical, and diet history and have a detailed discussion of the child’s signs and symptoms. Based on the evaluation, the doctor will conduct the following tests (9).
- Physical examination: During physical examinations, the doctor will evaluate the child’s skin, nails, and hair. Changes in the skin, hair, and nail texture and color are signs of underlying nutrient deficiencies caused by malnutrition. They will also check for your child’s vital parameters, such as blood pressure and pulse rate.
- Anthropometric assessment: The anthropometric evaluation includes quantitative measurement of the height, weight, body mass index (BMI), body circumferences (waist, hip, and limbs), and skinfold thickness to determine the child’s growth and development.
Pediatricians use standardized growth charts to compare a child’s anthropometry against other children of the same age. This is one of the best ways to assess the nutritional status of a child.
- Blood tests: If there are signs of malnutrition, the doctor may order blood tests to determine the nutrient deficiencies and functions of the organs. Complete blood count (CBC), lipid profile, total protein, and albumin tests, along with specific tests for nutrition deficiencies, will help determine the causes of malnutrition and its adverse effects on the body, if any.
- Imaging tests: In some cases, the doctor may also recommend imaging tests, such as X-ray, CT scan, and MRI, to evaluate the internal organs’ health. These tests could also help assess the growth and development of muscles and bones.
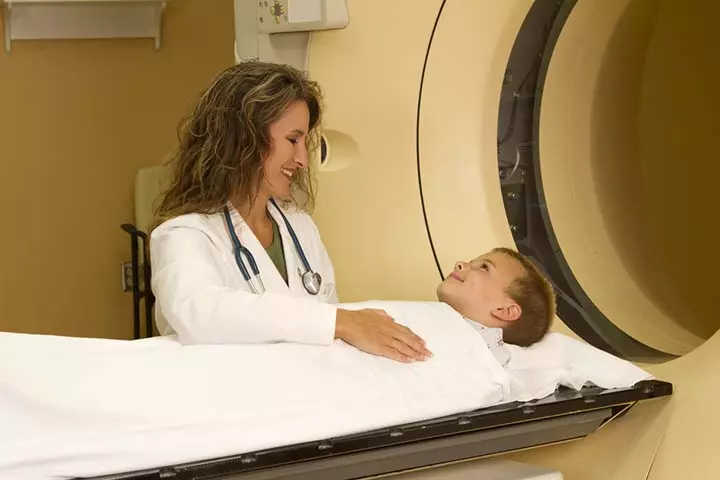
Based on the evaluation and test results, the doctor will chart a suitable treatment plan for the child.
Treatment For Malnutrition In Children
The treatment for malnutrition depends on its cause and severity. A team of health professionals, such as a pediatrician and certified nutritionist, will draft the treatment plan. In most cases, appropriate home care can help reverse malnutrition (10).
- Dietary changes: Feeding energy-dense, nutritious food is most often the first line of treatment for undernourished or mild undernutrition children. On the other hand, a child with overnutrition needs a well-balanced, calorie-restricted diet. These dietary changes are necessary for a child to gain/lose weight and maintain a healthy weight-for-age. Severely malnourished children may require hospitalization for special care. In case a child isn’t able to eat or drink, they would be given intravenous or tube-feeds for some time and then gradually shifted to a normal diet under medical supervision.
- Supplementation: Nutrient deficiencies are a common feature of malnutrition. The doctor might recommend high-energy protein, vitamin, and mineral supplements when dietary changes alone are insufficient. These supplements should be taken as per prescribed dosages under medical supervision. Depending on the child’s improvement, the doctor will change doses and either stop supplements or suggest a few more.
- Treatment of underlying health issues: The treatment of health disorders and infections (if any) may help improve the child’s health. These health conditions may be the cause of malnutrition or the effect of being malnourished. Treatment of the condition is likely to help the body respond to treatment better and reverse malnutrition gradually.
During treatment, regular monitoring of the child’s height, weight, and other growth and development parameters is important. It will determine the efficacy of the treatment for the child. The child may be referred to a specialist if there is no improvement.
Nutrition rehabilitation is typically a time consuming process. It needs involvement of a knowledgeable pediatrician, skilled nutritionist, and dedicated parents along with a supportive family. But once good dietary habits become a way of life, it pays rich dividends.
Prevention Of Malnutrition In Children
Preventing malnutrition is possible with appropriate dietary and lifestyle practices. You could try the following tips to balance your child’s nutritional intake.
- Encourage your child to eat a healthy, well-balanced diet. To ensure the child follows healthy eating, start early in life. Children fed healthy foods from infancy are more likely to adapt to healthy eating practices later in life. Healthy foods for kids include home-cooked balanced meals.
- Ensure their diet contains food from different food groups. Fresh seasonal fruits and vegetables, whole grains, nuts and seeds, dairy products, lean meat, and fish are foods that a child should consume regularly.

- Limit intake of processed foods high in fat and refined sugar. This practice will help avert overnutrition and associated health risks.
- Do not hesitate to make special dietary changes, such as adding supplements to your child’s diet if they are at risk of malnutrition due to an underlying health condition, such as an eating disorder. However, consult a pediatrician and certified nutritionist before adding or removing food from the diet or starting a supplement.
Frequently Asked Questions
1. What are the long-term effects of childhood malnutrition?
Malnourishment may cause irreversible damage to the child’s physical and cognitive development in the first two years of life. Long-term effects of these issues include poor school performance, increased vulnerability to diseases, developmental delays, and an increased risk of developing obesity, diabetes, and cardiovascular diseases (11).
2. How does malnutrition affect a child emotionally?
Malnutrition may lead to psychological changes such as irritability, anxiety, depression, apathy, a lack of concentration, and a poor sleep pattern (12).
3. How does malnutrition affect a child’s intellectual development?
Malnutrition may lead to poor development of verbal and cognitive abilities. It may also cause poorer verbal, spatial, and full-scale IQ. As the child grows older, their reading abilities and neuropsychological performance may also be affected (13).
Malnutrition in children is a serious cause for concern as it interferes with their growth and development. But, it does not develop within a day. Thus, parents and caretakers are advised to take proper care of the child’s food habits and ensure that they are getting adequate amounts of the required nutrients for their proper growth. If you are unsure about the right amount or quantities of nutrients required for your child, speak to your child’s pediatrician and ask for a food chart to be used as a reference.
Infographic: What Are The Signs Of Malnutrition In Children?
Malnutrition is still a concerning issue in various countries; however, early detection can help in effective management. Look at the infographic below for different types of malnutrition and their possible signs. Knowing these signs will ensure prompt treatment and prevent associated complications.
Some thing wrong with infographic shortcode. please verify shortcode syntaxIllustration: Malnutrition In Children: Causes Symptoms And Treatment

Image: Dall·E/MomJunction Design Team
References
1. Fact Sheets, Malnutrition; WHO
2. Malnutrition; WHO
3. Malnutrition; CHOP
4. Marasmus; NCBI
5. Symptoms of Malnutrition; NHS Inform
6. Hunger and Malnutrition; Johns Hopkins Medicine
7. Causes of malnutrition; NHS Inform
8. The-Impact-of-Poor-Sanitation-on-Nutrition; Thousanddays
9. Diagnosing malnutrition; NHS Inform
10. Treating malnutrition; NHS Inform
11. Malnutrition; UNICEF
12. Zeno Stanga et al.; The effect of nutritional management on the mood of malnourished patients; National Library of Medicine
13. Jianghong Liu et al.; Malnutrition at Age 3 Years and Lower Cognitive Ability at Age 11 Years; JAMA Pediatrics.
14. Jianghong Liu et al.; The UNICEF/WHO/WB Joint Child Malnutrition Estimates (JME) group released new data for 2026; WHO.
Community Experiences
Join the conversation and become a part of our nurturing community! Share your stories, experiences, and insights to connect with fellow parents.
Read full bio of Dr. Pooja Parikh
Read full bio of Swati Patwal
Read full bio of Rohit Garoo
Read full bio of Shinta Liz Sunny