Image: Shutterstock
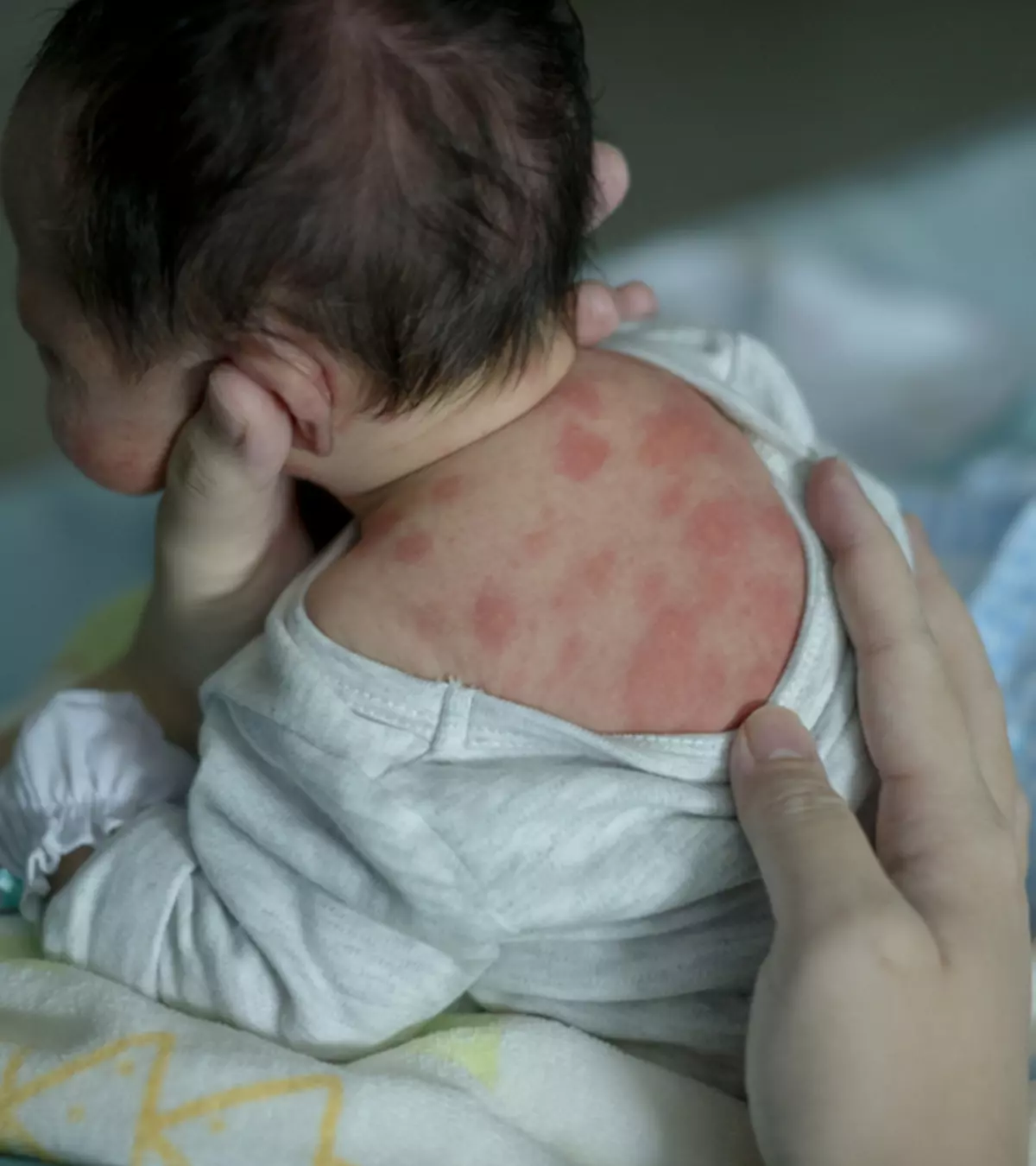
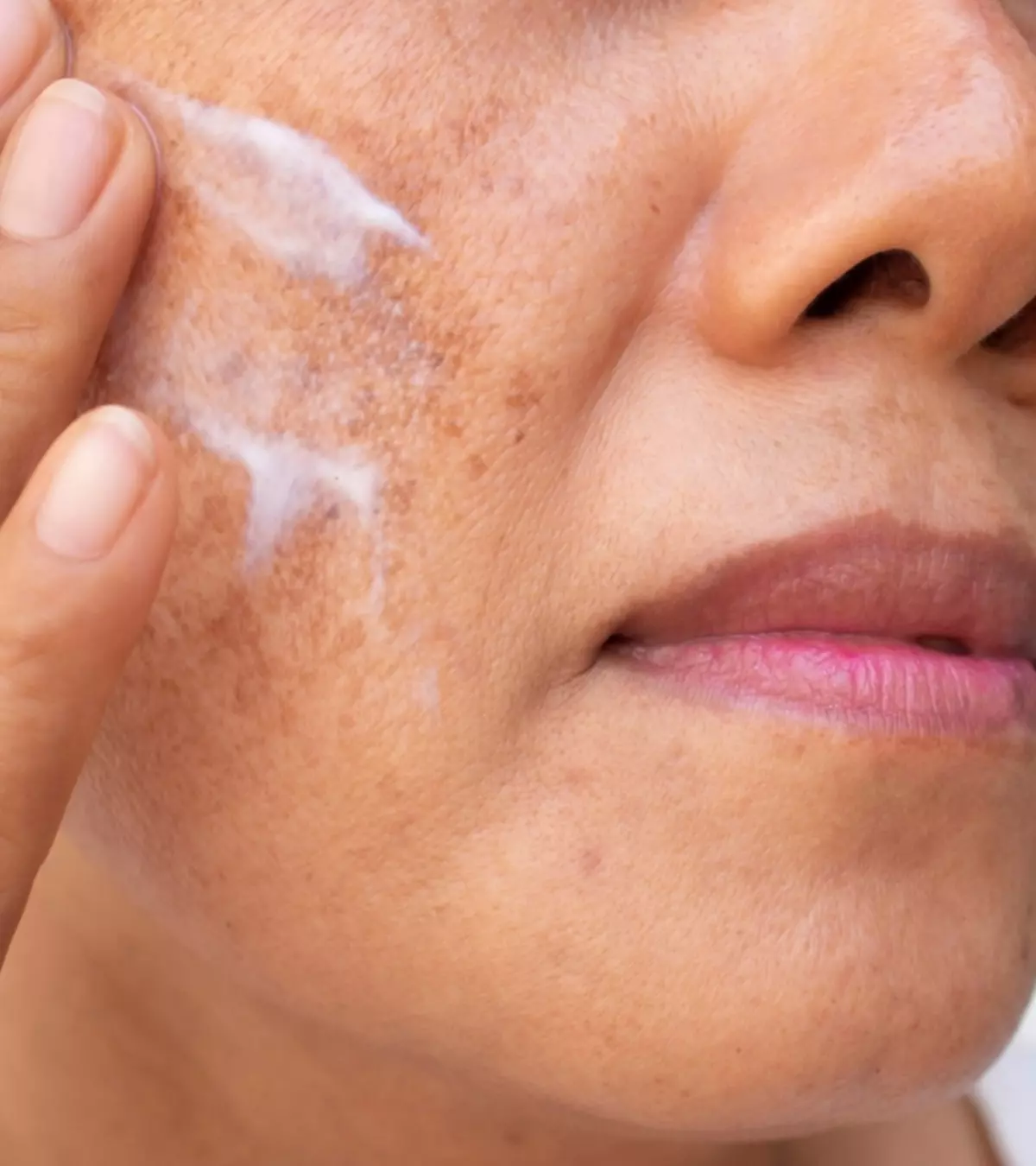
Pregnancy melasma, also known as chloasma, is a condition that causes dark spots or gray-brown patches on the skin. It is also sometimes called the “mask of pregnancy” or “pregnancy mask” because melasma patches generally occur on the nose, forehead, chin, cheeks, and upper lip and appear like patches.
Sometimes, these patches also appear on the neck, chest, forearms, and other body parts exposed to the sun (1).Maternal health is generally unaffected by the condition and poses no harm to the baby. Although the patches can be treated with topical medicines, they fade with time in most women.
Read this post to learn more about melasma, including its causes and treatment options.
Key Pointers
- Melasma causes dark or gray-brown patches on the skin during pregnancy.
- It can be triggered by increased hormonal levels, genetic history, sun exposure, skin care products, drugs, older maternal age, or other factors.
- The patches usually disappear a few months post-delivery when hormonal fluctuation stabilizes.
- To reduce melasma patches, it is advised to avoid sun exposure, certain skincare products, and waxing due to limited safety studies for topical treatments.
- Plant-based products, such as vitamin C, glycolic acid, licorice extract, or soybean extract, may also be helpful.
Is It Normal To Have Melasma During Pregnancy?
According to a research paper published in the Croatian journal Collegium Antropologicum, melasma affects around 50% to 70% of pregnant women.
The National Institutes of Health state that its prevalence fluctuates between 1.5% and 33%, contingent upon the population studied. The increased levels of estrogeniA sex hormone responsible for the development of female sexual characteristics , progesterone, and the melanocyte-stimulating hormone (MSH) in the third trimester could trigger melasma (2). Melasma is not a painful condition and does not lead to any pregnancy complications. But what might cause it?
Causes Of Melasma During Pregnancy
- The exact cause of melasma is unclear. It is likely to develop when the melanocytesiCells that create the melanin pigments that give hair, eyes, and skin their color of the skin produce extra color. Those with darker complexion are likely to develop melasma as they have active melanocytes than those with a lighter complexion (3).
Some of the common melasma triggers include
- Exposure to Ultraviolet light (UV rays) from the sun stimulates melanocytes, leading to melasma. The condition might worsen during summers (4).

- Hormonal changes are another reason for pregnancy melasma. The symptoms of melasma are likely to be triggered in pregnant women during gestation by increased levels of hormones such as estrogen, progesterone, and MSH in the third trimester (5) (6).
- Other factors include genetic history (if someone else in the family has been suffering from it), skincare products, drugs, multiple pregnancies, and older maternal age.
Melasma that occurs during pregnancy tends to go away after a few months postpartum when the hormonal activity stabilizes (7).
 Quick fact
Quick factWays To Reduce The Melasma Patches
Although melasma disappears with time, certain things might help in minimizing the flare-ups on your skin.
- Stay out of the sun: The foremost step is to avoid sun exposure as much as possible, to prevent skin damage and the consequent skin discoloration. If your work forces you to go out in the sun, apply a broad-spectrum sunblock. Choose sunscreens or blocks with SPF 25 or higher that may help to prevent exacerbating chloasma (8). Also, wear a wide-brimmed hat, long-sleeved dress, and sunglasses, and avoid tanning salons.
- Avoid skincare products or cosmetics: Facial cleansers, skin creams, and make-up during pregnancy may irritate your skin, making melasma worse. Avoid them until you have given birth, or the melasma disappears.

- Do not wax: Waxing for removing hair might worsen melasma as it could cause skin inflammation. The effect may be high, especially in the areas affected by hyperpigmentation (uneven skin tone).
Although no specific diet or prenatal vitamin can help prevent melasma. A well-balanced diet with adequate vitamin D may help keep the skin healthy.
 Quick tip
Quick tipCan Pregnancy Melasma Be Treated?
Besides taking precautions to prevent flare-ups, you could talk to a dermatology expert about the treatment options to minimize the patches. However, the treatment options are limited for pregnant women.
- Topical medications such as retinoids and hydroquinone are usually prescribed for melasma, but their safety during pregnancy is not studied (9).
- Plant products with vitamin C, glycolic acid, arbutiniA substance extracted from the bearberry plant that is considered to be a skin-lightening agent , azelaic acidiA natural compound found in grains, rye, barley, and animal products and synthetically used to treat certain skin issues , licorice extractiA flowering herb known for aiding digestive problems and infections , or soybean extract help protect the pregnancy glow. Again, you may only use them when their benefits outweigh their risks (8).

Most women see a natural improvement in their skin tone postpartum, as the hormones return to normal levels. However, it is better to talk to an obstetric for the right treatment, especially if you are on birth control pills after pregnancy.
Can You Prevent Melasma Or Chloasma In Pregnancy?
Preventing melasma during pregnancy may not be possible if the condition is due to hormonal changes or genetics. You might, however, take the precautions discussed above to prevent the patches from darkening further.
Does Melasma During Pregnancy Tell Something About The Baby’s Gender?
No. It is just folklore that pigmentation in a pregnant woman could indicate the gender of the fetus. There is no scientific evidence to support this.

Frequently Asked Questions
1. Does melasma from pregnancy go away?
Usually, melasma fades away on its own three months after pregnancy. However, you may check with your dermatologist on tips to make the fading away effortless (10).
2. What foods make melasma during pregnancy worse?
Currently, there is limited evidence on foods that could trigger melasma (10). If you notice flaring up of the skin after eating food, restrict its intake and consult your doctor to understand the trigger.
3. Can pregnancy melasma be treated with laser therapy?
The use of lasers to treat any disease during pregnancy is highly controversial and not advised. Before undergoing such a procedure, consult your doctor (13).
4. Can stress worsen pregnancy melasma?
Though this theory is controversial, the American Academy of Dermatology research suggests that stress triggers the formation of more cortisol, which may trigger melasma (11).
5. Does breastfeeding affect pregnancy melasma?
No studies have been dedicated to this association but pregnancy melasma is not permanent and usually fades after birth or breastfeeding.
6. How is pregnancy melasma diagnosed?
Pregnancy melasma can be diagnosed with the help of a Wood’s lamp, this is used to accentuate the hyperpigmentation, which is epidermal. This disease can also be detected on a cellular level with the help of reflectance confocal microscopy (RCM)(14).
Pregnancy melasma is a temporary condition caused due to hormonal changes and UV radiations. The skin usually returns to its normal complexion after the baby’s delivery. However, if the patchy skin is uncomfortable, you may take a few preventive measures, such as applying dermatologically-approved sunscreen or wearing protective clothing. In addition, use skin products approved by a doctor. Also, check with your medical advisor before practicing any home remedies to treat melasma. Also, consult them if you notice any uncommon symptoms or if the discomfort increases.
Infographic: Triggers Of Pregnancy Melasma
Melasma is a skin condition that could occur in pregnant women and may resolve after childbirth. However, some factors could trigger the condition. Check out the infographic below to learn about these factors and ways to reduce flare-ups during pregnancy. Illustration: Momjunction Design Team
Illustration: Pregnancy Melasma (Chloasma): What It Is Causes & Treatment
_what_it_is_causes__treatment_illustration.jpg.webp)
Image: Stable Diffusion/MomJunction Design Team
References
1. Melasma; U.S. Department of Health and Human Services National Institutes of Health (2018)
2. Bolanca I et al.; Chloasma–the mask of pregnancy; Collegium Antropologicum (2008)
3. David J. Leffell; Melasma (Chloasma); Harvard Health Publishing (2019); Yale School of Medicine
4. ajira Basit et al.; Melasma; StatPearls Publishing (2019)
5. Jp Ortonne et al.; A global survey of the role of ultraviolet radiation and hormonal influences in the development of melasma; University of Texas Southwestern Medical Center
6. Gertrude-Emilia Costin and Stanca-Ariana Birlea; What is the mechanism for melasma that so commonly accompanies human pregnancy; IUBMB Journal – Wiley Online Library
7. Melasma; British Association of Dermatologists; The British Skin Foundation
8. Debabrata Bandyopadhyay; Topical Treatment of Melasma; Indian J Dermatol (2009)
9. Pina Bozzo et al.; Safety of skin care products during pregnancy; Can Fam Physician (2011)
10. Melasma; Cleveland Clinic
11. Melasma: Causes; American Academy of Dermatology Association
12. What to Know About Melasma and Other Skin Changes During Pregnancy; WFMC Health
13. Farzad Allameh et al.; (2026);A Systematic Review of Elective Laser Therapy during Pregnancy;; NCBI
14. Oluwatobi A. Ogbechie-Godec and Nada Elbuluk; (2017);Melasma: an Up-to-Date Comprehensive Review;; NCBI
Community Experiences
Join the conversation and become a part of our nurturing community! Share your stories, experiences, and insights to connect with fellow parents.
Read full bio of Dr. Christian Pope
Read full bio of Rebecca Malachi
Read full bio of Swati Patwal
Read full bio of Aneesha Amonz