
Image: Midjourney/ MomJunction Design Team
Preterm or premature birth occurs when a woman delivers her baby before the 37th week of pregnancy. Various factors can cause preterm birth, but one of the most serious concerns is the babies’ low birth weightiA term used to describe a baby who is born weighing less than 5 pounds, 8 ounces or 2500 grams regardless of their gestational age (LBW). According to the American Academy of Pediatrics (AAP), “development is not a race, and babies develop at their own pace” (1). Therefore, even premature babies who experience developmental delays will gradually reach developmental milestones, including weight gain, if proper conditions are offered. This post discusses premature babies’ weight gain and growth and provides a premature baby growth chart.
Key Pointers
- Preterm babies typically weigh five pounds or less, though this might vary based on the child’s gestational age.
- Premature infants in the Neonatal Intensive Care Unit (NICU) normally begin gaining weight within a few days of birth.
- A healthy preterm baby may first show an increase in head circumference before showing gains in weight and height.
- The Fenton development chart is a popular method for assessing the growth milestones of premature infants, taking into account weight, height, and head size.
Understanding The Weight Of Premature Babies
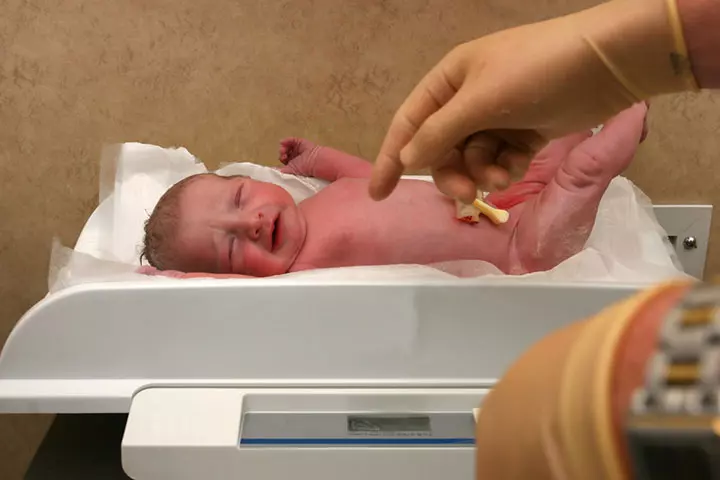
The average weight of a newborn is seven pounds (3.17 kilograms). But the average weight of a preterm infant is about five pounds (2.26 kilograms) or less. The exact weight depends on how early the baby is delivered, with infants born after 28 weeks of pregnancy weighing 2.3 pounds (one kilogram) (2).
There is a difference in premature babies with low birth weight compared to babies with intra uterine growth retardation or “Small for gestational age” babies. Medical expert Dr. Po-Chang Hsu says, “A baby’s weight gain is influenced by several key factors, with genetics playing a foundational role. Some babies are naturally smaller or larger at birth due to their parent’s genetic makeup, which can shape their growth patterns in the first year of life.”
In the United States, the preterm birth rate for non-Hispanic White mothers decreased by 1% from 7.44% in 2019 to 7.36% in 2026, while there were no significant changes for non-Hispanic Asian and Hispanic mothers. However, there were insignificant increases for non-Hispanic Black and non-Hispanic American Indian or Alaska Native mothers. In 2026, the singleton preterm birth rate was significantly higher for non-Hispanic Black mothers by about 65% compared to non-Hispanic White and non-Hispanic Asian mothers.

Preterm singleton birth rates in the US, based on the mother's race
Source: Exploring the Decline in the Singleton Preterm Birth Rate in the United StatesSymptoms Of Premature Birth
Premature birth results from preterm labor. While premature birth might be unforeseen in many and cannot be prevented, knowing the signs of preterm labor might help you take necessary precautions and make timely intervention. Here are some possible signs and symptoms of preterm labor you should be aware of (3).
- Frequent or regular feeling of contractions
- Constant lower back pain
- Mild abdominal cramps
- Pressure in the lower abdomen or pelvic area
- Light bleeding or vaginal spotting
- Watery, mucusy, or bloody vaginal discharge
- Preterm rupture of membranesiA condition where the amniotic sac ruptures before the 37th week and leaks fluid indicating the onset of labor (PROM)
Weight, Height, And Head Circumference Growth In Premature Babies
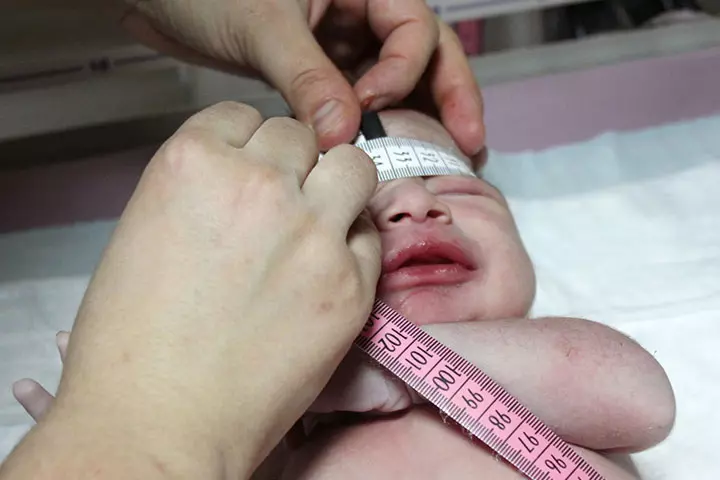
The weight, height, and head circumference of a premature infant will vary depending on the gestational week of their birth and their overall health at birth. The following are some key points about the weight, height, and head circumference of premature babies:
Note that these are the average figures while the actual figures may differ from one baby to another.
- Premature infants are put in the neonatal intensive care unit (NICU) and ideally start gaining weight within a few days after birth.
- The weight gained can significantly differ among babies. A baby with a gestational age of 24 weeks (born after the 24th week of pregnancy) may attain five grams per day while those born at 33 weeks or later can put on as much as 30 grams per day (4).
- The desirable weight gain in kids who are born with a birth weight of more than two kilograms is 20-30 grams per day (5).
- The height of preterm babies increases by about 1.1 centimeters every week until the completion of the ideal gestational age, which is about 40 weeks (5).
- The chronological age of the baby is the absolute age, which is the time from the birth of a premature baby to the present. This age is also called postnatal age.
- A healthy premature infant is likely to show improvement first in the head circumference, followed by weight and height.
- Following premature birth, the head circumference of babies increases by about 0.5 centimeters per week until the age of three months, beyond which the growth slows down to about 0.25 centimeters per week until six months of age (5). Studies indicate that this weekly growth further slows beyond six months, with a two-centimeter increase in head circumference between six and nine months and a one-centimeter increase between nine and twelve months of age (6).
In the next section, we give you a detailed growth chart for premature infants.
 Trivia
TriviaPremature Baby Growth Chart
The Fenton growth chart for preterm infants is most commonly used for assessing the growth milestones of a premature baby. The Fenton chart was created in 2003 by Dr. Tannis Fenton, who revised it in 2013 to accommodate the new standards suggested by the World Health Organization (7).
In the next section, we list the approximate values for height, weight, and head circumferences for both preterm infant girls and boys. The value given is the 50th percentile, which is a median number (8).
Growth charts for premature infants

Weight, height, and head circumference of premature infant girls
| Gestational Age In Weeks | Weight In Kilograms | Height In Centimeters | Head Circumference In Centimeters |
|---|---|---|---|
| 24 | 0.6kg | 30cm | 21.1cm |
| 26 | 0.8kg | 33cm | 23cm |
| 28 | 1kg | 35.6cm | 25cm |
| 30 | 1.3kg | 38.5cm | 27cm |
| 32 | 1.7kg | 41.1cm | 29cm |
| 34 | 2.1kg | 44cm | 30.5cm |
| 36 | 2.6kg | 46.5cm | 32.1cm |
| 38 | 3.1kg | 48.5cm | 33.5cm |
| 40 | 3.4kg | 50.5cm | 34.9cm |
Weight, height, and head circumference of premature infant boys
| Gestational Age In Weeks | Weight In Kilograms | Height In Centimeters | Head Circumference In Centimeters |
|---|---|---|---|
| 24 | 0.65kg | 31cm | 22cm |
| 26 | 0.83kg | 34cm | 23.5cm |
| 28 | 1.1kg | 36.5cm | 25.8cm |
| 30 | 1.4kg | 39cm | 27.5cm |
| 32 | 1.8kg | 42cm | 29.5cm |
| 34 | 2.25kg | 44.9cm | 31cm |
| 36 | 2.7kg | 47cm | 32.8cm |
| 38 | 3.2kg | 49.5cm | 34cm |
| 40 | 3.6kg | 51cm | 35cm |
Source
: Fenton Preterm Growth Chart Site, University of Calgary (9)
Not all babies develop the same way or at the same pace, as the growth at this stage depends on multiple factors. Doctors periodically assess a preterm baby in the NICU.
Note that the growth figures indicated by the doctor could be less or more than those mentioned in the chart. But as long as your doctor states that your baby is doing well, you can relax and look forward to taking your baby home from the NICU.
However, one thing you may still worry about is the baby’s nutrition as it can affect their weight significantly.
 Trivia
TriviaNutrition For A Premature Baby
Premature babies often experience feeding difficulties and the doctors in the NICU will determine a premature baby’s feed after considering the gestational age and their overall health condition. Below are the sources of nourishment for a preterm infant:
- Intravenous fluids: Early preterm babies will not be able to breastfeed and will require an intravenous delivery of nutrients and other fluids. The IV solution will be a mix of all the proteins, carbohydrates, and lipid compounds that the baby will need to thrive and grow stronger(10).
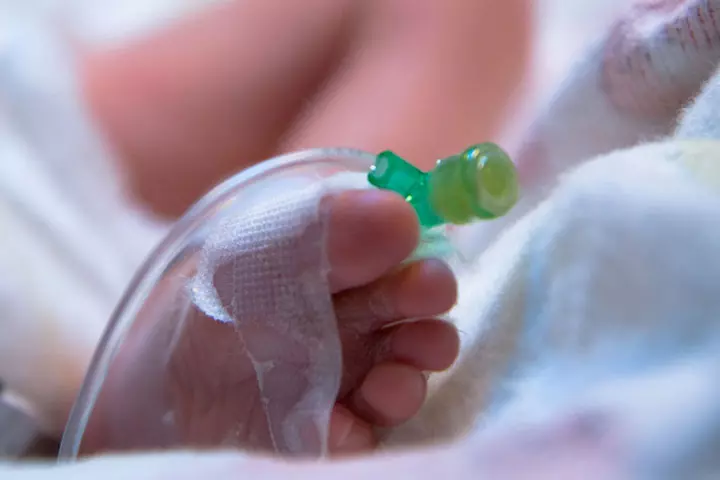
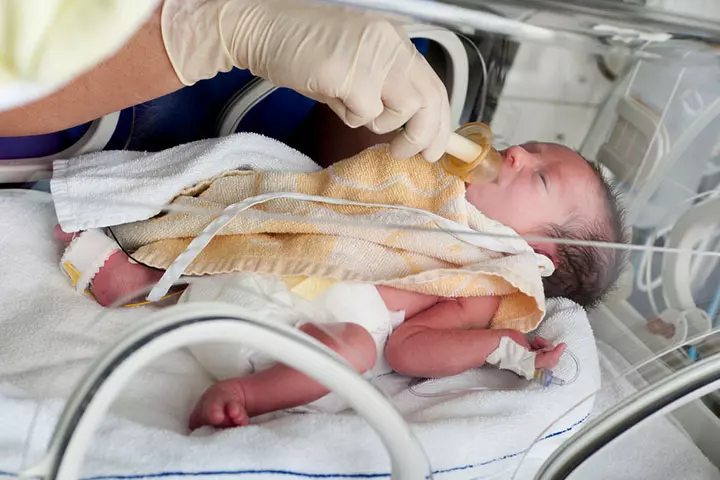
- Formula or breast milk through tube feeding: Once your baby’s digestive system is a bit strong, they can receive breast milk or formula directly into their stomach through a sterile tube that goes through their nose or mouth. This form of feeding is called nasogastric or orogastric tube feeding (10).
The doctor will determine the nature of the feed. If the mother is lactating sufficiently, then she can express breast milk, which would be then given to the baby through tube feeding. The quantity of breast milk or formula increases gradually in this method.
Teena, a mother from India, speaks at length about the methods she used to help her premature baby girl Olive gain weight. She says, “I fed my baby every two hours. This speeds up digestion and allows them to accept new nutrients… Olive’s doctor also suggested we give her coconut oil which contains healthy fats… Kangaroo mother or skin to skin contact also helped Olive with her weight gain… Giving Olive formula also helped her gain weight consistently… Tracking her feeding until four months and letting her sleep and rest also helped in her weight gain (i).”
- Breastfeeding: If your baby is a late preterm infant (born between 34-37 weeks), then they may be able to breastfeed. Both the mother and baby will require some initial practice. It is advisable for mothers to work with lactation consultants to develop effective breastfeeding strategies. Once the baby understands how to latch to the nipple, you can breastfeed the premature baby just like you would a full-term baby.
If the baby has trouble latching, you can provide expressed breast milk through a feeding bottle. Breastmilk has protein, minerals, and fat that the baby can easily digest (11). Breastmilk will also reduce the risk of intestinal infection. Additionally, breastfeeding will promote bonding between you and your baby through skin-to-skin contact, thus helping them recover quickly (12).
- Fortified formula: Breastmilk alone may not provide the nutrition that premature babies need to grow. They have a higher caloric requirement, usually around 120-kilocalories per kilogram of body weight per day (13). Fortified formula milk can provide the extra nutrition that preemies need, along with the right mix of vitamins and minerals for healthy growth. If required, the doctor may recommend this.
Frequently Asked Questions
1. What is premature birth?
A birth that occurs before three weeks of the expected due date or before 37 weeks of gestation is called preterm birth or premature delivery. A baby born before 25 weeks of gestation is considered highly preterm, and before 32 weeks is very preterm (14).
2. Why does premature birth happen?
Premature birth may happen due to various reasons. Some can be induced or early cesarean section due to medical reasons. Premature rupture of membranes, multiple pregnancies, prenatal infections, and chronic conditions such as hypertension and diabetes can result in premature birth. However, there can be cases of premature birth with no apparent causes (15).
3. What factors increase the chances of premature birth?
A positive personal or family history of preterm birth can increase the chances of preterm birth. There are also increased chances in women under age 20 or above 40 and among African Americans. Being underweight and smoking during pregnancy can also increase the risk (14).
4. How does premature birth affect a child’s development?
Preterm birth is the leading cause of mortality in children under age five in most countries. While some preemies may thrive and grow as term infants without significant problems, a few might face disabilities (15).
5. How can premature birth be prevented?
There is no sure way to prevent premature birth. Eating healthy, reducing stress, and taking adequate prenatal care may reduce the risk. A minimum of an 18-month gap between subsequent pregnancies is also recommended to reduce the chance of preterm delivery. Avoiding alcohol, tobacco, and other drugs may also reduce the risk of premature birth in some cases (14).
6. How does premature birth affect the mother?
Mothers of preterm babies are more likely to experience postpartum anxiety and depression. They may also develop post-traumatic stress disorder (PTSD) and find it difficult to bond with their preemies (14).
7. How is premature birth diagnosed?
If you feel any signs of labor before 37 weeks, your doctor will perform a pelvic exam to see if your cervix has started to dilate or open to prepare for birthing. Your doctor will also suggest a transvaginal ultrasound, urine test, fetal fibronectin screening, and will monitor your contractions for the diagnosis of premature birth (16).
8. What is the long-term outcome for premature babies?
The long-term health problems for premature babies may include the risk of chronic illnesses and limited abilities (17). However, advancement in preemie care has reduced the risk of these conditions, and several premature babies grow fine, without any problems, like full-term babies.
9. What are some management strategies for preterm infants?
Preterm babies are at high risk of developing hypothermia soon after delivery. Therefore, they must be wrapped in warm towels, dried, and transferred to a NICU incubator for regulating body temperature. Other management strategies for preterm infants include monitoring their vital signs regularly, ensuring enough fluid intake through feeding tubes, giving blood transfusions, and helping them breathe (18).
You may give premature birth to your baby if they’re born before 37 weeks of gestation. Your baby could be in the low birth weight index if born prematurely. Also, some babies may need NICU to facilitate their proper growth and improve premature baby survival rates. Though it may be disheartening to see your newborn in an incubator, it is essential for their growth. This phase is temporary, and your baby will eventually gain weight with appropriate nourishment and care. As your baby initiates feeding well, has normal body functioning, and develops at the right pace, you may take them home.
Infographic: What Are The Health Challenges Of Extremely Preterm Babies?
Extremely premature babies are born before the 28th week. Chances of survival are rare if born before 23 weeks. Babies born at 23 to 25 weeks have a better chance of survival with medical care. However, it is not possible to rule out the risk of lifelong disabilities. Go through the infographic to know the health challenges of extremely preterm babies. Illustration: Momjunction Design Team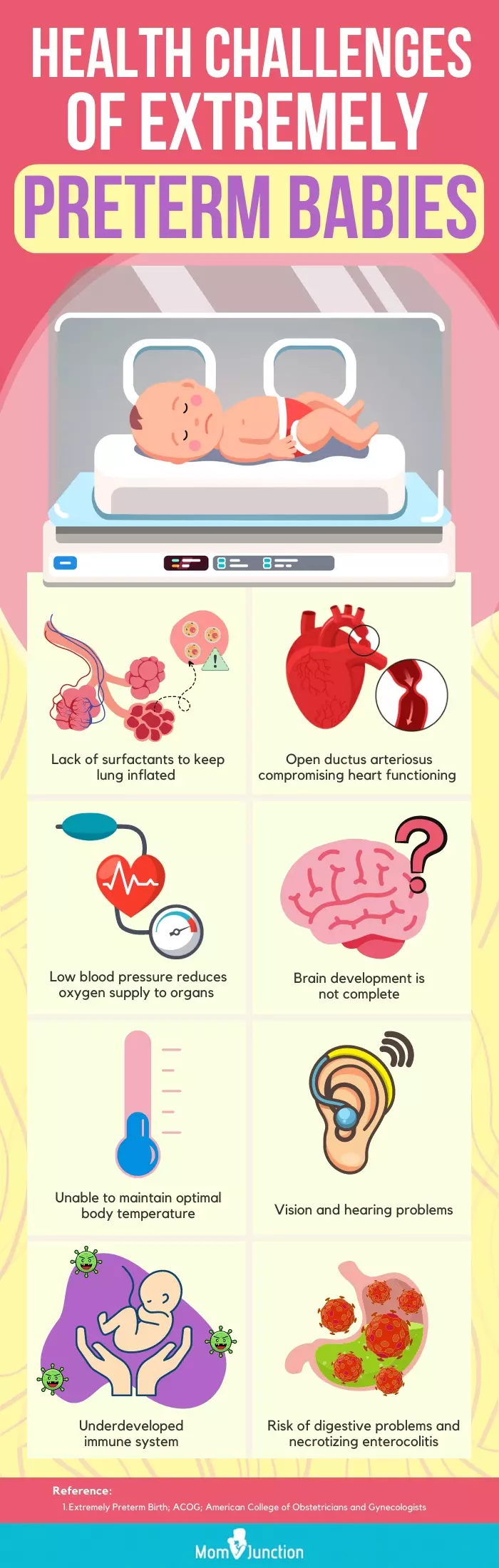
Illustration: Height And Weight Gain Growth Chart For Premature Babies

Image: Dall·E/MomJunction Design Team
Learn about preterm birth in this informative video. Understand its causes, recognize the signs and symptoms, and explore diagnosis and treatment options. A must-watch for expectant parents.
Personal Experience: Source
MomJunction articles include first-hand experiences to provide you with better insights through real-life narratives. Here are the sources of personal accounts referenced in this article.
i. Weight gain tips for premature babies I How to improve weight in preterm babies? Increase weight;https://www.youtube.com/watch?v=zApoXvYdiVg
References
1. Preemie Milestones; American Academy of Pediatrics
2. Caring for a Premature Baby: What Parents Need to Know; American Academy of Pediatrics
3. Preterm Labor; Mayo Clinic
4. Neonatal weight gain and nutrition; U.S. National Library of Medicine
5. NICU Family Information Packet; Agency for Healthcare Research and Quality
6. E. Rivers; Children: Stages of Growth and Development; Encyclopedia of Forensic and Legal Medicine (Second Edition); (2016); Science Direct
7. Fenton and Kim, A systematic review and meta-analysis to revise the Fenton growth chart for preterm infants; National Center for Biotechnology Information
8. Growth chart; U.S. National Library of Medicine
9. Fenton Preterm Growth Charts; University of Calgary
10. Moriam Mustapha, Kate Adele Wilson, and Sybil Barr; Optimising nutrition of preterm and term infants in the neonatal intensive care unit; Pediatrics and Child Health Journal
11. Providing Breastmilk for Premature and Ill Newborns; American Academy of Pediatrics
12. Your Role In Caring For Your Premature Baby; Tommy’s
13. Care of the Premature Infant: Part I. Monitoring Growth and Development; American Academy of Family Physicians
14. Preterm Birth; World Health Organization
15. Premature Birth; Cleveland Clinic
16. Preterm Birth; NYU Langone Health
17. Short and Long-Term Effects of Preterm Birth; UK HealthCare; University of Kentucky
18. Premature Birth; Mayo Clinic
Community Experiences
Join the conversation and become a part of our nurturing community! Share your stories, experiences, and insights to connect with fellow parents.
Read full bio of Dr. Elna Gibson

Dr. Po-Chang Hsu is a medical doctor and medical content expert. He received his medical degree from Tufts University School of Medicine in Boston in 2016. Previously, he did a master’s degree at Harvard University and wrote a thesis on neuroimaging in schizophrenia patients at Brigham and Women’s Hospital. He currently works at Alpas Wellness.
Dr. Po-Chang Hsu is a medical doctor and medical content expert. He received his medical degree from Tufts University School of Medicine in Boston in 2016. Previously, he did a master’s degree at Harvard University and wrote a thesis on neuroimaging in schizophrenia patients at Brigham and Women’s Hospital. He currently works at Alpas Wellness.
Read full bio of Rohit Garoo
Read full bio of Dr. Ritika Shah
Read full bio of Vidya Tadapatri
















