Image: Midjourney/ MomJunction Design Team
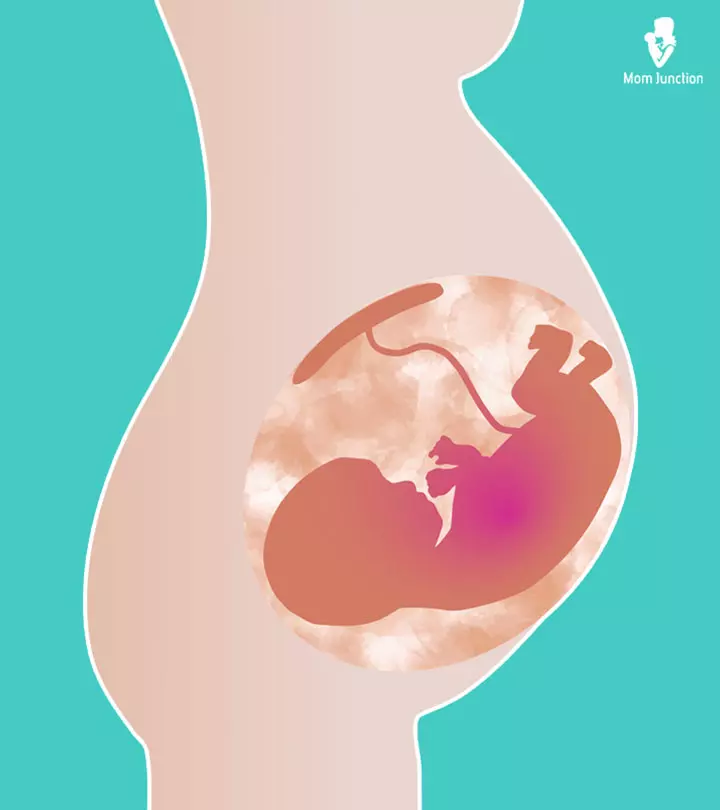
The fetus is surrounded by and cushioned in a clear, yellowish fluid in the womb known as amniotic fluid. Some women may experience leaking amniotic fluid during pregnancy, too much of which may be harmful.
The amniotic fluid comprises hormones, immune cells, nutrients, and urine produced by the fetus. The fetus starts swallowing and excreting this protective fluid at around 20 weeks. The amniotic fluid helps fetal movement and growth. Also, it prevents infections and injuries to the fetus, supports organ development (e.g., kidneys, intestines, and lungs), and protects the umbilical cord from compressing.
Keep reading this post to learn more about amniotic fluid leakage, how to differentiate it from the leakage of other fluids such as urine or vaginal discharge, and what to do in such cases.
Key Pointers
- An amniotic fluid leak (premature rupture of membranes) involves clear or colorless fluid with mucus or blood, with no odor, and either a gush or slow trickle.
- Causes of PROM include smoking, recreational drug use, alcohol use, uterine infection, cervical surgery, or a short cervical length.
- Many women go into labor within 24 hours after membrane rupture, or labor is induced to avoid difficulties. However, there can be problems if the fluid leaks before term.
- Risks of amniotic fluid leak include labor induction, infections, placenta separating from the uterus, umbilical cord problems, and C-section delivery.
What Is Leaking Of Amniotic Fluid Or Premature Rupture Of Membranes (PROM)?

The premature or preterm rupture of the amniotic sac membrane or water bag before the start of labor is called premature rupture of membranes (PROM). If it occurs before 37 weeks, it is called preterm premature rupture of membranes (pPROM). Intrauterine infections and other causes, such as intrauterine bleeding have been recognized to be responsible for about 30% of pPROM cases (1). However, premature rupture of membranes is still rare, and no definite cause is identified despite various etiologies (2).
Normal Levels Of Amniotic Fluid
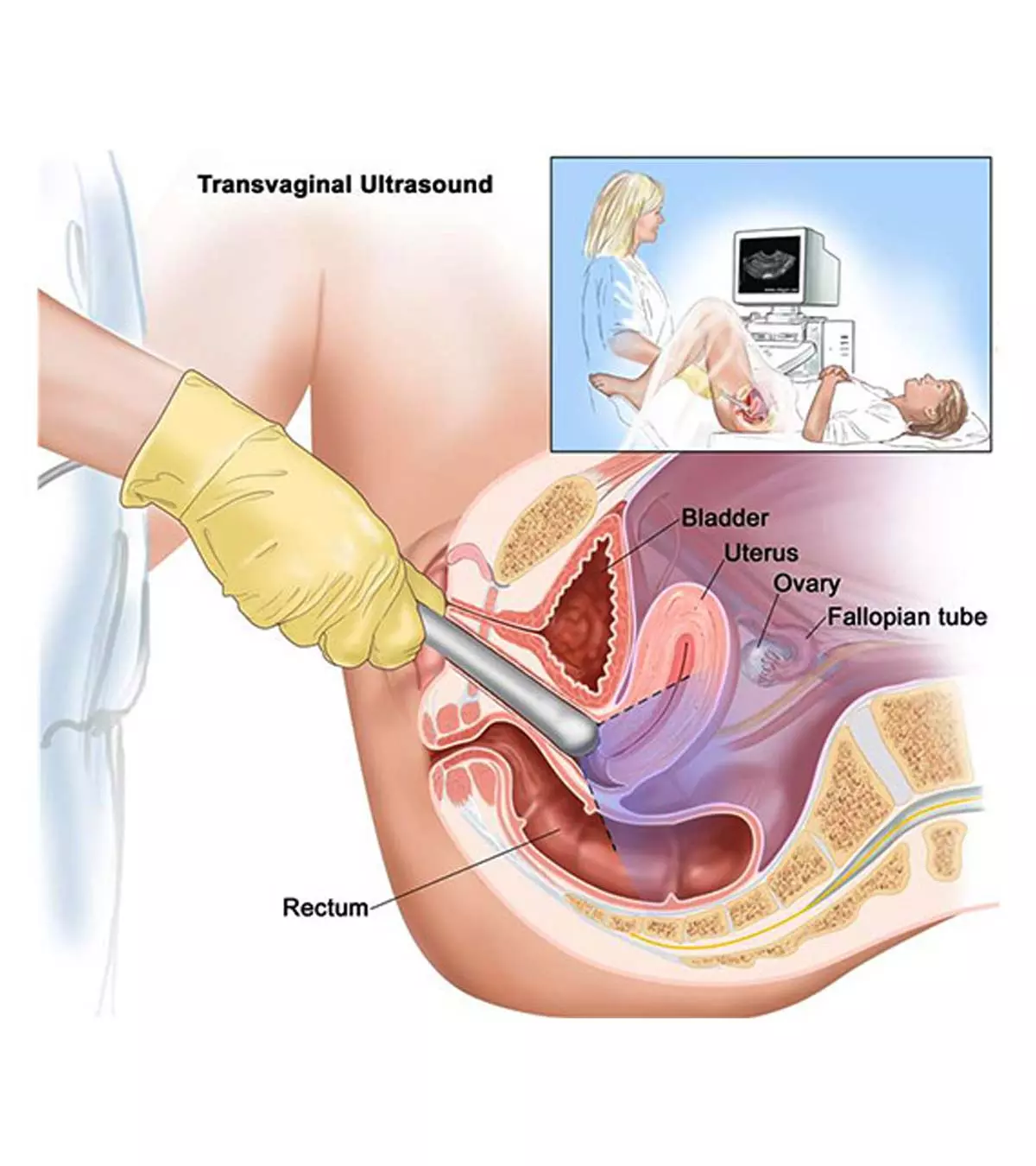
The normal levels of amniotic fluid vary according to gestational age. The amniotic fluid is visible after 12 days of conception, reaching the highest volume at the 36th week of gestation and declining near birth. Your doctor will measure the amount of amniotic fluid through ultrasound during your prenatal visits. An average amniotic fluid index is between 5cm and 25cm (3).
Amniotic fluid levels during your pregnancy can be (4):
- 60ml at 12 weeks
- 175ml at 16 weeks
- Around 400-1200ml between 34 and 38 weeks
The fluid level declines by around 125ml a week at 38 weeks of gestation and decreases to around 800ml by the 40th week.
Leakage could result in too little of the amniotic fluid in the sac, which could be problematic. Hence, you should detect a possible amniotic fluid leak and seek medical help.
Signs And Symptoms Of Amniotic Fluid Leak
Amniotic fluid comes out in a gush when the membrane ruptures. This is also known as a water break, and it usually happens when you enter labor. A small hole in the amniotic sac, it may lead to a slow fluid leak, which feels like the trickle of fluid down to the vagina. First-time mothers might be confused about the difference between amniotic fluid, mucus plug, urine, and vaginal discharge during pregnancy. Dr. Stephanie Langsam, FACOG, a Wynnewood, Pennsylvania-based physician specializing in Obstetrics and Gynecology , says, “It is hard to know that your water broke, and rarely there is a moment with a large gush of fluid. Leaking amniotic fluid typically occurs randomly and feels almost like you are peeing on yourself. It can be a continuous trickle or a few spurts of leaking at random times. If you are concerned your water broke, call your doctor immediately. Amniotic fluid is usually clear and odorless; however, it may be concerning if it is green or mixed with blood.”
The following signs may help you identify amniotic fluid (5):
- Clear or colorless
- Present with mucus or blood
- No odor
- Does not stop leaking
- Soaks pad or underwear often
Jennica Hill, a mother of one, experienced amniotic fluid leakage at around 27 weeks of pregnancy. Reflecting on this incident, she says, “Usually, my discharge was very milky and white. But I noticed that I was getting more of a clear discharge. I wasn’t sure if it was urine, just a completely clear discharge, or amniotic fluid. But leaking amniotic fluid at this stage would mean that my water bag broke, and the baby might need to be born early.” However, after ultrasound, pH test, and microscopic examination of amniotic fluid, it was confirmed that she didn’t have amniotic fluid leakage (i).”
It may not be amniotic fluid if there is:
- Odor
- Light- or pale-yellow color
- Thick mucus or look milky
Urine and vaginal discharge have a peculiar odor and color. You may use a pad or panty liner to check these aspects. Obstetrician and gynecologist Dr. Veena Madhankumar suggests, “If fluid continues to leak when you lie down or change positions, it is more likely amniotic fluid. Place a clean pad in your underwear and look for any leakage. Amniotic fluid will typically soak through slowly and steadily.”
Another way to know is by holding your pelvic floor muscles for a few seconds. If it is urine, the leakage will stop. If it doesn’t stop, it is probably leaking amniotic fluid. These home tests to confirm amniotic fluid may not be helpful for all women. It is advised to get medical help if you are not sure it is not amniotic fluid. If the color of your amniotic fluid appears green or brown, it could indicate fetal distress, and you should seek medical assistance immediately.
 Did you know?
Did you know?Causes Of Premature Rupture Of Membranes

A premature amniotic fluid leak may occur from membrane weakening and uterine contractions. Every one-fourth to one-third of all preterm births are caused by PROM (6). The possible risk factors of PROM include (1):
- Smoking
- Recreational drug use
- Alcohol use
- Uterine infection
- Accidental trauma
- Polyhydramnios or too much amniotic fluid in the sac
- Oligohydramnios or too little amniotic fluid in the sac
- Overstretching of amniotic sac and uterus
- Improper prenatal care
- Cervical surgery or short cervical length
- AmniocentesisiDiagnosis procedure carried out during pregnancy
- Previous preterm birth (premature birth)
- Sexually transmitted infections
- Less than six months after the previous labor
- Twin or multiple pregnancies
- Second and third trimester vaginal bleeding
- Nutritional deficiencies and underweight
- Connective tissue disordersiDisorders resulting from inflammation of connective tissues
The amniotic sac ruptures or water breaks during or at the beginning of labor after 37 weeks of pregnancy. However, the leaking amniotic fluid before 37 weeks is associated with certain risks.
What Happens When Amniotic Fluid Leaks?
Many women enter labor around 24 hours after the rupture of the membrane or leakage of amniotic fluid at term. If it doesn’t begin in 24 hours, labor is induced to prevent any complications (7), and the mother is closely monitored to record cervical dilation rates and labor progression. If the fluid leaks before term, it may lead to the following risks (8):
- Fetal and maternal infection
- Placenta separating from the uterus
- Umbilical cord problems
- C-section delivery
An amniotic fluid leak in the first and second trimesters may be associated with an increased risk for congenital disabilities, miscarriage, stillbirth, or preterm delivery, whereas in the third trimester, it may cause difficulties in delivery.
The risk of complications may be reduced by choosing suitable approaches after a preterm premature rupture of the membranes (PPROM). A retrospective study by the University Emergency Hospital, Bucharest, revealed that waiting 48 hours for delivery following a PPROM can reduce the risk of complications in a baby born after 28 weeks of pregnancy (9). Discuss with your Ob/Gyn the best next step after an amniotic fluid leak to ensure your safety and your baby’s best health.
 Be watchful
Be watchfulWhen To Call The Doctor?

You should also call the doctor if (10):
- Fluid is green-tinged or brownish-yellow or has a foul smell
- You have vaginal bleeding
- You have a fever or flu-like symptoms such as feeling hot and shivery
- Heart rate has increased
- There is abdominal pain or contractions
- You are uncertain and concerned
The doctor will diagnose your condition based on your gestation age and will also give you an internal examination before the treatment. An amniotic fluid leak is diagnosed by a speculumiA device used to look inside the vagina to observe the cervix examination, followed by a pH test and microscopic fluid examination.
Since intrauterine infection is one of the major causes and complications of PROM and pPROM, all pregnant women with ROM should be evaluated for any signs of intrauterine infectioniAn infection inside the uterus , which includes (2):
- Maternal fever
- Fetal tachycardiaiWhen a fetus has a faster heart rate , such as a fetal heart rate of 160 bpm or more for about 10 minutes,
- Uterine tenderness
- Foul-smelling vaginal discharge
While waiting for the doctor, try to stay calm and do not insert anything, such as a tampon or cloth, into the vagina to stop the leakage. Just notice how much fluid has leaked and what the color of the fluid is to let the doctor know.
How Is Amniotic Fluid Leakage Or PROM Treated?
The treatment plan differs for a woman based on the gestational age, cause of fluid leakage, and maternal and fetal health status. If it occurs at term, it is managed with delivery unless there is an indication to wait for spontaneous labor.
If fluid leaks or PROM occurs before term, the next steps could be (11):
- Administers corticosteroidsiMedication used to reduce inflammation and overactive immune system to speed up the maturity of the fetal lung between 24 and 34 weeks of gestation
- Prescribes antibiotics to prevent infection
- TocolyticiProcedure used to delay delivery in women having preterm contractions medicines to prevent preterm labor
- Delivery to manage PROM unless there are benefits from delaying it without any risks.
- Magnesium sulfate to protect the fetus from neurological complications such as cerebral palsyiA medical condition where damage occurs to the developing brain, mostly before or at birth, causing one to lose control of arms and legs. if delivery is expected within 24 hours before 32 weeks of gestation (12).
- Admission to a hospital for observation and fetal monitoring and transfer to a hospital where there are good neonatal intensive care facilities just in case the baby arrives early.
If the PROM causes low amniotic fluid levels (13):
- Amnio-fusion: This may be carried out using an intrauterine catheteriA device placed inside a pregnant woman's uterus to monitor uterine contractions during labor during labor induction. Adding fluid to make up for the loss of amniotic fluid will provide extra support around the umbilical cord and reduce the chances of a cesarean.
- Re-hydration: You may be given fluids orally or intravenously to increase the amniotic fluid level.
 Quick fact
Quick factCan You Prevent Premature Rupture Of Membranes?
PROM is generally not preventable but avoiding the risk factors such as smoking, alcohol, and unprotected sex might reduce the probability of the condition (6).
According to one clinical trial study, intake of vitamin C supplements by pregnant women, with a history of PROM, after the 14th week of pregnancy may help reduce the risk of PROM in the current pregnancy (14). However, consult your doctor about the safety and efficacy of its consumption.
Does Leaking Amniotic Fluid Mean Miscarriage?
Leaking amniotic fluid is not one of the common reasons for a miscarriageiThe sudden loss of pregnancy beor 20th week of pregnancy . However, if it occurs in the second trimester and is accompanied by other symptoms such as abdominal pain, it could be a sign of miscarriage. Nevertheless, you should get it checked by the doctor before concluding anything.
Can Amniotic Fluid Replenish Itself?
The fetus will continue to produce amniotic fluid even if there is a leak, but it may not be enough if there is a heavy leak (15). In a few cases, the amniotic sac may reseal itself and prevent fluid leakage. However, more studies are required to understand the resealing of the sac and replenishing of amniotic fluid after a leak. A study found that the amount of sterile amniotic fluid left when preterm PROM (pPROM) happens might help predict if the fetal membranes can seal on their own. The study involved 38 cases of pPROM at less than 27 weeks of pregnancy, where five cases of pPROM resulted in spontaneous sealing after 14 days of pPROM. Therefore, it is usually suggested that obstetricians wait at least 3-14 days after pPROM to observe if spontaneous sealing occurs (1).
Frequently Asked Questions
1. Why do I experience more discharge in general during pregnancy?
It is normal to experience more vaginal discharge during pregnancy due to the softening of the cervical and vaginal walls and the increased progesteroneiHormone produced in the ovaries that plays a key role in pregnancy levels. The softening causes an increase in the discharge to prevent any infectious agent from entering the uterus through the vagina (20).
2. Can I leak amniotic fluid and not have contractions?
Yes, you may leak amniotic fluid and not have contractions with it. This may indicate a premature delivery or discharge that is not amniotic fluid (21). As mentioned above in the signs and symptoms, you may differentiate between an amniotic fluid discharge and other discharge based on its color, texture, and flow.
3. Can amniotic fluid leak if my cervix is closed?
Yes, the fetal membrane may rupture even when the cervix is closed and cause leaking amniotic fluid. Although its exact cause may not be known, it is believed to occur from the breakage of the weakest membrane point from an infection, trauma, or internal pressure (22).
4. How is amniotic fluid measured?
“There are two ways of measuring amniotic fluid; both are done with an ultrasound. The first way is called the amniotic fluid index (AFI), and the second is the single deepest vertical pocket (MVP). To measure the AFI, the womb is broken down into four quadrants, and each quadrant is measured. The normal levels, when added up, should be between five and 24. To measure the MVP, the largest fluid area is measured in the greatest vertical dimension. The normal level is between 2 and 8 centimeters,” Dr. Langsam observes.
5. Can the baby move after the water breaks?
When the amniotic sac breaks and the water gushes out, the fetal position may change and the baby may slide further down in preparation for labor (19). According to experts, some women may feel reduced fetal activity, but the baby will keep moving until the mother goes into labor (23).
6. How long can I go with amniotic fluid leaking?
If you do not enter labor within 24 hours of the water breaking, you and your baby may be at an increased risk for infection (24). Therefore it is vital to promptly consult a doctor if you notice an amniotic fluid leak.
7. Does drinking water increase amniotic fluid?
A few studies indicate that pregnant women with low amniotic fluid levels (oligohydramnios) experienced a significant increase in fluid volume after drinking an extra two liters of water within two hours (25). However, more studies are needed to prove this hypothesis, and it’s essential to consult your healthcare provider before consuming excessive water during pregnancy.
8. Is the amniotic fluid sticky?
The amniotic fluid is typically clear, not sticky. However, if you spot leakage of a sticky substance, it could indicate that your mucus plug has been released. You may identify the mucus plug by its clear, off-white, or slightly bloody appearance, about one to two tbsp in volume. It also has a stringy, sticky, and jelly-like texture. This jelly like discharge during pregnancy is a normal part of the body’s preparation for labor, but if you have concerns or notice any unusual changes, it’s always best to consult your healthcare provider (26) (27).
The amniotic fluid may gush out as membranes break before delivery. Leaking amniotic fluid before term may occur due to an infection, trauma, nutritional deficiencies, or overstretching of the amniotic sac. The condition may increase the risk of congenital disabilities in early pregnancy. Later it may make the body susceptible to infections and umbilical cord issues and necessitate a C-section delivery. Seek immediate medical help if you suspect any symptoms of leaking amniotic fluid. Treatment depends on the duration of pregnancy, underlying cause, and health status of the mother and fetus.
Infographic: Difference Between Leaking Amniotic Fluid And Urine Leak
Amniotic fluid leak before the due date requires medical evaluation and necessary interventions since it may lead to preterm birth or other complications. However, it is possible to have urine leaks in the last trimesters of pregnancy due to increased pressure on the bladder. Go through the below infographic to know the difference between an amniotic fluid leak and a urine leak during pregnancy that may help you seek medical care if required.
Some thing wrong with infographic shortcode. please verify shortcode syntax
Illustration: How To Recognize Leaking Amniotic Fluid And What To Do?

Image: Dall·E/MomJunction Design Team
Are you worried you might be leaking amniotic fluid? Learn the signs to tell the difference between amniotic fluid and pee. Get the facts now!
Personal Experience: Source
MomJunction articles include first-hand experiences to provide you with better insights through real-life narratives. Here are the sources of personal accounts referenced in this article.
i. Am I Leaking Amniotic Fluid? How Do I Know For Sure?!…A Pregnancy Story.https://www.youtube.com/watch?feature=shared&v=wzZWcYTj_yg
References
- Sae Yu et al.; (2026); Residual amniotic fluid volume predicts the sealing of preterm prelabor rupture of fetal membranes in the pre- and periviable period.
https://www.sciencedirect.com/science/article/pii/S1028455923001286 - Shailja Dayal and Peter L. Hong; (2026); Premature Rupture Of Membranes.
https://www.ncbi.nlm.nih.gov/books/NBK532888/ - Megan Lord et al.; (2026); Amniotic Fluid Index.
https://www.ncbi.nlm.nih.gov/books/NBK441881/ - Amniotic Fluid: Physiology and Assessment.
https://www.glowm.com/section-view/heading/Amniotic%20Fluid:%20Physiology%20and%20Assessment/item/208#.YtZ-tnZBzIU - Premature rupture of membranes.
https://medlineplus.gov/ency/patientinstructions/000512.htm - Premature Rupture of Membranes (PROM)/Preterm Premature Rupture of Membranes (PPROM).
https://www.chop.edu/conditions-diseases/premature-rupture-membranes-prompreterm-premature-rupture-membranes-pprom - Overview of Labor.
https://www.stanfordchildrens.org/en/topic/default?id=overview-of-labor-90-P02896 - Preterm Premature Rupture of Membranes (PPROM).
https://www.urmc.rochester.edu/encyclopedia/content?ContentTypeID=90&ContentID=P02496 - Roxana Elena Bohilțea et al; (2026); Expectant Management of PPROM Improves Neonatal Outcome—A Retrospective Study of 562 Patients.
https://pmc.ncbi.nlm.nih.gov/articles/PMC8745911/ - Artificial Rupture of the Membranes.
https://www.uofmhealth.org/health-library/hw195832 - Preterm Premature Rupture of Membranes: Diagnosis and Management.
https://www.aafp.org/pubs/afp/issues/2006/0215/p659.html - Magnesium Sulphate to Prevent Cerebral Palsy following Preterm Birth.
https://dl.icdst.org/pdfs/files1/31717c87985179a44f35419b907ed05e.pdf - Low Amniotic Fluid Levels: Oligohydramnios.
https://americanpregnancy.org/healthy-pregnancy/pregnancy-complications/oligohydramnios/ - Nayereh Ghomian et al.; (2013); The Role of Vitamin C in Prevention of Preterm Premature Rupture of Membranes.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3652497/ - R. Devlieger et al.; (2007); Fetal membrane healing after spontaneous and iatrogenic membrane rupture: A review of current evidence.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC1665653/ - Shehla Noor et al.; Prevalence Of PPROM And Its Outcome.
https://www.researchgate.net/publication/23162252_Prevalence_of_PPROM_and_its_outcome - A. F. Ray et al.; (2015); Vision Amniotic Leak Detector (ALD) to Eliminate Amniotic Fluid Leakage as a Cause of Vaginal Wetness in Pregnancy: A NICE Medical Technology Guidance.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4575365/ - Amniotic Fluid.
https://www.marchofdimes.org/find-support/topics/pregnancy/amniotic-fluid - What does it feel like when your water breaks.
https://www.lamaze.org/Giving-Birth-with-Confidence/GBWC-Post/what-does-it-feel-like-when-your-water-breaks-1 - Vaginal discharge during pregnancy.
https://www.pregnancybirthbaby.org.au/vaginal-discharge-during-pregnancy - How to know if your water breaks.
https://news.sanfordhealth.org/womens/did-my-water-break/ - Antenatal Care Module: 17. Premature Rupture of Membranes (PROM).
https://www.open.edu/openlearncreate/mod/oucontent/view.php?id=48&printable=1 - What to expect when your waters break.
https://www.tommys.org/pregnancy-information/giving-birth/what-expect-when-your-waters-break - Inducing labor.
https://www.nhs.uk/pregnancy/labour-and-birth/signs-of-labour/inducing-labour/ - Hofmeyr GJ et al. (2002); Maternal hydration for increasing amniotic fluid volume in oligohydramnios and normal amniotic fluid volume.
https://www.cochrane.org/CD000134/PREG_maternal-hydration-for-increasing-amniotic-fluid-volume-in-oligohydramnios-and-normal-amniotic-fluid-volume - Amniotic Fluid.
https://my.clevelandclinic.org/health/body/23310-amniotic-fluid - Mucus Plug.
https://my.clevelandclinic.org/health/symptoms/21606-mucus-plug
Community Experiences
Join the conversation and become a part of our nurturing community! Share your stories, experiences, and insights to connect with fellow parents.
Read full bio of Dr. Sangeeta Agrawal

Dr. Veena Madhankumar is an experienced obstetrician and gynecologist with 25 years of clinical expertise. She completed her MBBS from Coimbatore Medical College, India, in 1999 and pursued her MD in Obstetrics and Gynecology from Sri Ramachandra Medical College, Chennai, India. Dr. Madhankumar has been associated with iCliniq for over a decade, providing expert medical consultations and guidance. She has also established a practical laparoscopy training course.
Dr. Veena Madhankumar is an experienced obstetrician and gynecologist with 25 years of clinical expertise. She completed her MBBS from Coimbatore Medical College, India, in 1999 and pursued her MD in Obstetrics and Gynecology from Sri Ramachandra Medical College, Chennai, India. Dr. Madhankumar has been associated with iCliniq for over a decade, providing expert medical consultations and guidance. She has also established a practical laparoscopy training course.
- Dr. Stephanie Langsam is a board-certified physician specializing in Obstetrics and Gynecology. She received her medical degree from Technion Israel Institute of Technology and completed her residency at Lankenau Medical Center. She is certified by the American Board of Obstetrics and Gynecology.
 Dr. Stephanie Langsam is a board-certified physician specializing in Obstetrics and Gynecology. She received her medical degree from Technion Israel Institute of Technology and completed her residency at Lankenau Medical Center. She is certified by the American Board of Obstetrics and Gynecology.
Dr. Stephanie Langsam is a board-certified physician specializing in Obstetrics and Gynecology. She received her medical degree from Technion Israel Institute of Technology and completed her residency at Lankenau Medical Center. She is certified by the American Board of Obstetrics and Gynecology.
Read full bio of Aneesha Amonz
Read full bio of Rebecca Malachi
Read full bio of Dr. Joyani Das