Image: iStock
Ovulation is when a mature egg (ovum) is released from the ovary. It is a hormone-mediated process where the follicular stimulating hormone (FSH) stimulates follicular growth, and the luteinizing hormone (LH) triggers ovulation. The released ovum moves from the ovary to the fallopian tube and stays alive for 12 to 24 hours, and it may fertilize during this time. This may occur about 14 days before menstruation in a 28-day menstrual cycle (1).
You can predict ovulation by tracking its signs and symptoms or using ovulation predictor kits. The fertile window is five days before ovulation and the day of ovulation.
Knowing the ovulation time may help a woman conceive or prevent pregnancy accordingly.
Read on to know more about the signs and symptoms of ovulation, tests to detect ovulation, and ways to manage ovulation problems.
Key Pointers
- Ovulation is when a mature egg is released from the ovary and can be predicted to help conceive or prevent pregnancy.
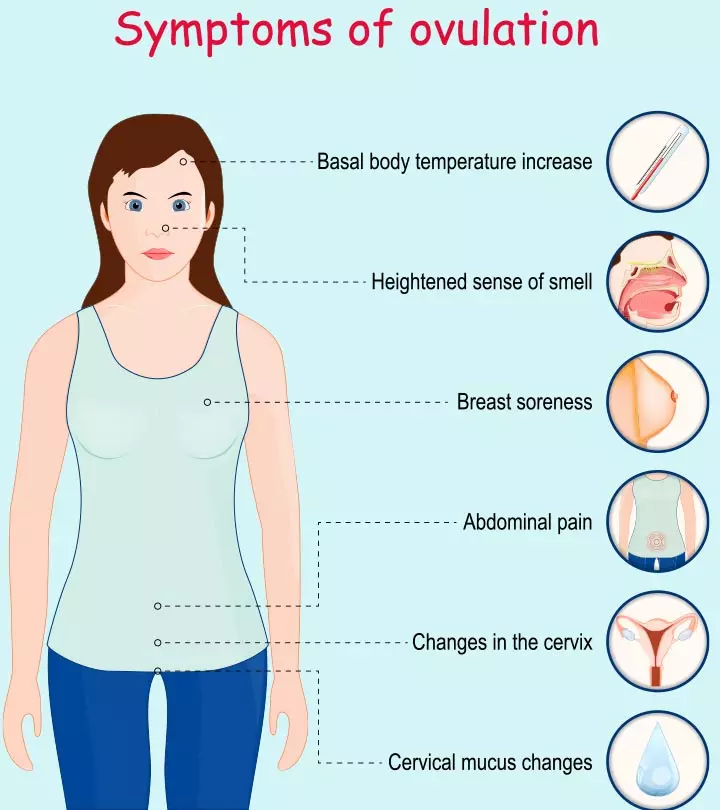
- Symptoms of ovulation include increased basal body temperature, breast soreness, mid-cycle pain, and others.
- To increase the chances of ovulation, maintain a normal BMI, avoid strenuous exercise, sudden dietary changes, and reduce stress.
- Medications such as clomiphene citrate, letrozole, metformin, and gonadotropins can help induce ovulation.
What Are The Signs And Symptoms Of Ovulation?
Ovulation signs and symptoms may not be the same for all women. Some may not notice any symptoms at all. The time of ovulation can also vary; while some ovulate on the same day of their cycle every month, others ovulate on different days in each cycle. If you are unsure about your symptoms and what ovulation feels like, here are some signs and symptoms of the ovulation phase (2):
- Cervical mucus changes: The cervical fluid is similar to egg whites near or during ovulation. There can be an increase in cervical mucus on the day of ovulation.

- Basal body temperature changes: Some women may notice a slight decrease in basal body temperature (BBT) before ovulation and an increase in temperature after ovulation.
- Changes in cervical firmness and position: During ovulation, the cervix is soft, wet, and open. The cervix may also move higher up into the body.
Tracking these changes for a few months may help women understand their body’s unique patterns during ovulation. These are fertility awareness methods that may help achieve or prevent pregnancies.
Erika Moulton, a mother of a two-year-old child, candidly shares her experiences during ovulation, “The first symptom and the strongest of them, and how I know that I’m ovulating, is my libido goes through the roof. I will become super hormonal, and every little thing will either annoy me, upset me, or make me sad. It’s really intense; it’s like this wave of emotion comes through me. The next symptom that I have been experiencing so intensely during ovulation time is cramping – tiny little cramps, like little lightning bolts of cramps in my ovaries. I have noticed little headaches here and there around the times I’m ovulating (i).”
What Are Secondary Signs And Symptoms Of Ovulation?
Ovulation signs and symptoms that are not consistent are called secondary signs.
They may be consistent in some women, but not in all cases.
Secondary signs and symptoms of ovulation may include:
- Light spotting or brown discharge may occur in some women during ovulation. This can be due to the rupture of ovarian follicles to release the ovum (2).
- Slight pain or cramps on one side of the pelvis (ovulation cramps). Release of the ovum causes this pain. Ovulation pain is also called mid-menstrual cycle pain or mittelschmerz. Some women may feel constant discomfort during ovulation, while others may not feel any ovulation pain symptoms or have mild cramps (3).

- Breast tenderness or soreness around the ovulation until menstruation. Some women may have severe breast pain radiating to the underarms, while a few may not notice any breast soreness or have mild discomfort (4).
 Research finds
Research finds- Increased sex drive (libido) is commonly seen around ovulation. Neuroendocrine mechanisms (hormonal changes) are responsible for increased libido during fertile days (5).
- Abdominal bloating. An increase in estrogeniA sex hormone responsible for the development of female sexual characteristics. hormone before the LH surge could be the reason for bloating during ovulation (6).
- Heightened senses of taste, smell, and vision can be noticed by some women in the second half of their menstrual cycle (after ovulation) (2).
It is important to know these body changes and signs since ovulation is related to fertility, reproductive health, and general well-being. In addition, these changes would help you identify and seek early medical care for ovulation problems.
What Are The Signs Of Ovulation Problems?
Keeping track of your menstrual cycles and knowing the signs and symptoms of ovulation can help you understand ovulation problems or not ovulating (anovulation). The following signs and symptoms are often associated with ovulation problems (7):
- Lack of periods (amenorrhea) means missing one or more menstruations without being pregnant.
- Irregular periods are when the time between periods keeps changing. It can be shorter or longer than usual.
- Heavy period is when more than 80ml blood (16 teaspoons) of blood is lost during a period or if the menstruation lasts more than seven days.
- Light periodis characterized by menstrual bleeding that involves the loss of less than 20ml (or less than 4 teaspoons) of blood during menstruation.
- Lack of ovulation signs includes no cervical mucus changes or basal body temperature.
- Negative results on ovulation predictor tests
The absence of ovulation (anovulation) is not always associated with a lack of menstruation (amenorrhea). You may seek medical care if you have problems with menstruation or cannot conceive.
 Be watchful
Be watchfulHow To Increase Your Chances Of Ovulation?
The following ways help increase your chances of ovulation (8):
- Maintain normal BMI: Keeping body weight around the average of your height and weight helps resolve ovulation problems related to obesity and overweight.

- Avoid strenuous exercise: You may seek expert opinion on physical activity levels since excessive exercise can affect ovulation.
- Avoid sudden dietary changes: Fasting, skipping meals, crash diets, and other disordered eating habits may affect ovulation. Eating regularly and properly can regulate ovulation in many women. Seek expert advice if you change eating habits for weight loss or are concerned about eating disorders, such as bulimia nervosaiAn eating disorder characterized by binge eating followed by purging through methods such as vomiting or laxative use. or anorexia nervosaiAn eating disorder characterized by extreme weight loss and an intense fear of gaining weight. .
- Reduce stress: Chronic emotional stress can affect ovulation. You may try relaxation techniques, meditation, etc., to cope with the stress.
 Quick Tip
Quick TipHow To Check Ovulation At Home?

You may use an ovulation home test to determine ovulation. This home urine test detects a rise in luteinizing hormone (LH) in the body. LH surge triggers ovulation, and the test helps to predict it. You may get the ovulation test kits in drug stores.
The test kit may contain several sticks to test for several days near your ovulation time based on the length of the menstrual cycle. For example, a woman with a 28-day cycle interval may begin testing on the 11th day after menstruation to detect ovulation. If ovulation occurs, there can be color change or other positive signs, as mentioned by the manufacturer.
Ovulation can also be tracked by digital handheld devices called home fertility monitors. These devices predict ovulation based on the salivary electrolyte levels, basal body temperature, or urine LH levels. Some monitors can store ovulation details for several cycles.
Sometimes, the test may miss the surge, especially if you have an irregular menstrual cycle. Rarely, false-positive results may occur. You may visit your doctor or see an infertility specialist if you cannot conceive or detect LH surge for several months (9).
How Is Ovulation Detected In The Clinic?
Doctors may ask detailed questions about your cycle length, date, menstruation, ovulation symptoms, and test results. Your doctor may order some of the following tests to detect ovulation problems before prescribing medications (10):
- Ultrasound to visualize the ovaries and uterus
- Blood tests to detect hormone levels
- Hysterosalpingogram (HSG) visualizes the fallopian tube and uterus using a dye.
- Laparoscopy and hysteroscopy use lighted telescopes to look through small incisions into the belly and uterus.
- Endometrial biopsies help identify ovulation and progesterone levels by analyzing endometrial tissue.
Imaging tests help identify structural anomalies, such as a blocked fallopian tube. In such cases, infertility treatment is done after tube repair; otherwise, it may increase the risk of ectopic pregnancy.
How Are Ovulation Problems Treated?
Lifestyle modifications may help some women improve ovulation. However, irregular menstrual cycles and no menstrual cycles (amenorrhea) due to ovulatory dysfunctions require medical treatment.
Commonly prescribed medications for ovulation problems may include (10):
- Clomiphene citrate (CC) is an ovulation-induction drug. This medication stimulates ovulation by making the pituitary gland release more follicular stimulating hormone (FSH). Increased FSH levels can stimulate the maturation of ovarian follicles.
- Aromatase inhibitors such as letrozole and anastrozole decrease the estradioliA form of estrogen hormone that plays a vital role in the development and maintenance of the female reproductive system. levels. A temporary decrease in estradiol stimulates the pituitary gland to make more FSH. This medication is also FDA-approved for treating some types of breast cancer in women after menopause.
- Insulin-sensitizing drugs such as metformin are often prescribed for women with insulin resistance and hyperinsulinemia (high insulin levels in the blood) and associated ovulation problems such as polycystic ovarian syndromeiA condition where the female body produces increased male hormone resulting in multiple cysts on the ovaries. (PCOS). Treating insulin resistance can lead to regular ovulation and menstruation in some women. Insulin sensitizers can also be combined with clomiphene.

However, these drugs are currently not approved by the US FDA to stimulate ovulation, and they are only approved for type 2 diabetes treatment to improve the body’s insulin sensitivity.
- Gonadotropins contain FSH or LH or both and are administered as injections. They can stimulate ovulation in some women. Human chorionic gonadotropin (hCG) can also be given to induce ovulation. Ovulation may happen about 36 hours after hCG since this drug is structurally and functionally similar to LH, which causes the follicle to release the egg (ovulation).
- Bromocriptine and cabergoline are prescribed for women with ovulation disorders due to hyperprolactinemia (high prolactin levels in the blood). Higher than normal prolactin levels inhibit the release of LH and FSH hormones from the pituitary gland and disrupt follicle maturation and ovulation. Prolactin levels can be high due to pituitary adenomas (benign tumor), certain painkillers, alcohol, oral contraceptives, hallucinogens, and thyroid or kidney diseases.
- Gonadotropin-releasing hormone (GnRH) helps release FSH and LH from the pituitary gland. Usually, GnRH is naturally released from the hypothalamusiThe part of the brain that controls hormone secretions, body temperature, hunger, sleep, and electrolyte balance. in small amounts every 90 minutes. When it is not released naturally, replacement is given with synthetic GnRH. This synthetic hormone is delivered in small amounts using a special pump through needles beneath the skin every 60 to 90 minutes.
- GnRH analogs, including agonists and antagonists, are synthetic hormones similar to natural GnRH. But these are chemically modified to change the GnRH function. Leuprolide acetate, goserelin acetate, and nafarelin acetate are GnRH agonists that stimulate the pituitary gland to secrete FSH and LH. GnRH antagonists such as ganirelix and cetrorelix can suppress FSH and LH production.
Frequently Asked Questions
1. At what age does ovulation stop?
Ovulation in reproductive women usually stops by the age of 51 since it is the average age for menopause (11).
2. Can I get pregnant on ovulation day?
Yes. The three days leading to ovulation and the day of ovulation are the most fertile period and the best time to get pregnant (12).
3. Can I ovulate more than once in a given cycle?
These medications can treat infertility or menstrual disorders due to ovulation problems. Doctors may also prescribe them for superovulation (mature two or more ovum) before in vitro fertilization (IVF). Gonadotropins and clomiphene citrate are not associated with congenitaliA condition or trait present at birth. disabilities or increased risk of ovarian cancer.
Ovulation symptoms and signs and ovulation predictor tests help a woman know her fertile days and plan pregnancy accordingly. You may track ovulation for several cycles to know these changes. Keeping track of ovulation using an ovulation calendar or apps can help you identify ovulation problems earlier. Always seek medical advice if you have any concerns about ovulation and fertility.
Infographic: Signs Of Ovulation Problems And Interventions
Ovulation issues may become notable if you tend to have a stressful and unhealthy lifestyle. However, knowing the symptoms will help you seek appropriate intervention. Check out the infographic below to learn about potential symptoms and practical advice that can help you improve your chances of ovulation.
Some thing wrong with infographic shortcode. please verify shortcode syntaxIllustration: Symptoms Of Ovulation To Help Predict Your Most Fertile Time

Image: Stable Diffusion/MomJunction Design Team
Join a medical expert as she breaks down the signs of ovulation. From increased cervical mucus to heightened libido, discover the natural cues your body gives during this crucial phase.
Personal Experience: Source
MomJunction articles include first-hand experiences to provide you with better insights through real-life narratives. Here are the sources of personal accounts referenced in this article.
i. Ovulation symptoms.. my *intense* symptoms!https://www.youtube.com/watch?v=0UecgAvBC2U&feature=youtu.be
References
- Julie E. Holesh, et al; Physiology, Ovulation.
https://www.ncbi.nlm.nih.gov/books/NBK441996/ - Signs You’re Ovulating.
https://www.healthywomen.org/content/article/signs-youre-ovulating-2 - Mid-Menstrual Cycle Pain (Mittelschmerz).
https://www.health.harvard.edu/a_to_z/mid-menstrual-cycle-pain-mittelschmerz-a-to-z - Breast Conditions in Young Women.
https://www.urmc.rochester.edu/encyclopedia/content?contenttypeid=90&contentid=P01589 - Women’s sexual experience during the menstrual cycle: Identification of the sexual phase by noninvasive measurement of luteinizing hormone.
https://www.tandfonline.com/doi/abs/10.1080/00224490409552216 - Ovulation Symptoms: Bloating.
https://nordicalagos.org/ovulation-symptoms-bloating/ - Anovulation.
https://my.clevelandclinic.org/health/diseases/21698-anovulation - Ovulation.
https://www.betterhealth.vic.gov.au/health/conditionsandtreatments/ovulation#increase-your-chances-of-ovulation - Ovulation Home Test.
https://medlineplus.gov/ency/article/007062.htm - Medications For Inducing Ovulation.
https://www.reproductivefacts.org/news-and-publications/patient-fact-sheets-and-booklets/documents/fact-sheets-and-info-booklets/medications-for-inducing-ovulation-booklet/ - Age and Fertility (booklet)
https://www.reproductivefacts.org/news-and-publications/fact-sheets-and-infographics/age-and-fertility-booklet/ - When are you more likely to conceive?
https://wwwyourfertilityorgau/everyone/timing#:~:text=Pregnancy%20is%20technically%20only%20possible - Owen Dyer; Women may ovulate two or three times a month
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC1126506/ - Angela R Baerwald et al; A new model for ovarian follicular development during the human menstrual cycle
https://www.sciencedirect.com/science/article/pii/S0015028203005442 - Breast Pain (Mastalgia).
https://www.hopkinsmedicine.org/health/conditions-and-diseases/mastalgia-breast-pain#:~:text=The%20most%20common%20type%20of,start%20of%20their%20menstrual%20cycle - Ovulation.
https://my.clevelandclinic.org/health/articles/23439-ovulation
Community Experiences
Join the conversation and become a part of our nurturing community! Share your stories, experiences, and insights to connect with fellow parents.
Read full bio of Dr. Mona Hardas
Read full bio of Dr Bisny T. Joseph
Read full bio of Rebecca Malachi
Read full bio of Reshmi Das