Image: ShutterStock
Ringworm in kids is highly contagious and can cause discomfort and pain as well as affect a child’s self esteem. Ringworm, also known as tinea or dermatophytosis, is a common fungal skin infection that causes itchy, ring-shaped rashes and affects the skin, scalp, and nails. It commonly occurs in hot and humid climates and affects people of all ages, including children. There are several types of ringworms that are caused by dermophytes, fungi types that inhibit the skin, hair, and nailbeds. Timely identification and treatment of ringworm can help relieve itching. Keep reading this post to know about the symptoms, treatment, and prevention of ringworm in children.

Key Pointers
- Ringworm can affect various body parts including the scalp, hair, feet, torso, limbs, groin area, hands, palm area, face, and nails.
- Common symptoms of ringworm include itchy rashes, circular rings, hair loss, nail thickening and discoloration, and blisters.
- Ringworm infection may occur through playing with soil and animals, poor hygiene, sharing of personal items, weakened immune system, and direct contact.
- It may take 3-4 weeks to completely cure ringworm.
- Preventive measures such as maintaining good hygiene, avoiding direct contact, regular checkups, and keeping skin clean and dry can help prevent ringworm infections.
What Causes Ringworm In Children?
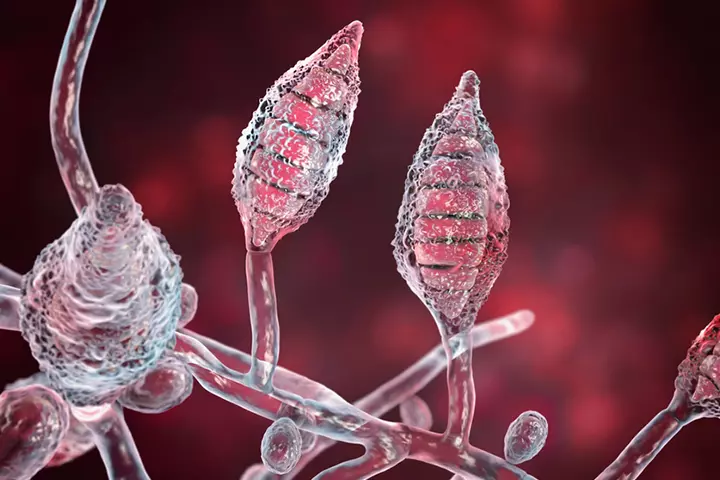
Ringworm is caused by any fungus from a group called dermatophytes (1). The most common fungi that cause the infection are from the genera Trichophyton, Microsporum, and Epidermophyton. These fungi are found almost everywhere in the environment.
Once a fungus gets on to the skin, it spreads on the outer keratinous/hard layer of the skin, nails, and the scalp. It propagates in a circular, ring-like pattern, thus giving its name.
Dermatophyte fungi cannot invade layers of skin beyond the dry, hard outer one. Therefore, ringworms are never found in mucus-rich regions like inside the nose, mouth, and the genitals. The medical term for ringworm is tinea. The name gets a suffix depending on the part of the body affected by the infection.
What Are The Types Of Ringworm?
The type of ringworm depends on the part of the body affected. Here are the kinds of tinea infection and the part of the body affected (2) (3):
- Tinea capitis: Scalp and hair
- Tinea pedis: Feet; it is also called Athlete’s foot
- Tinea corporis: Torso and limbs
- Tinea cruris: Groin area and the area around the genitals
- Tinea manuum: Hands and the palm area
- Tinea faciei: Face
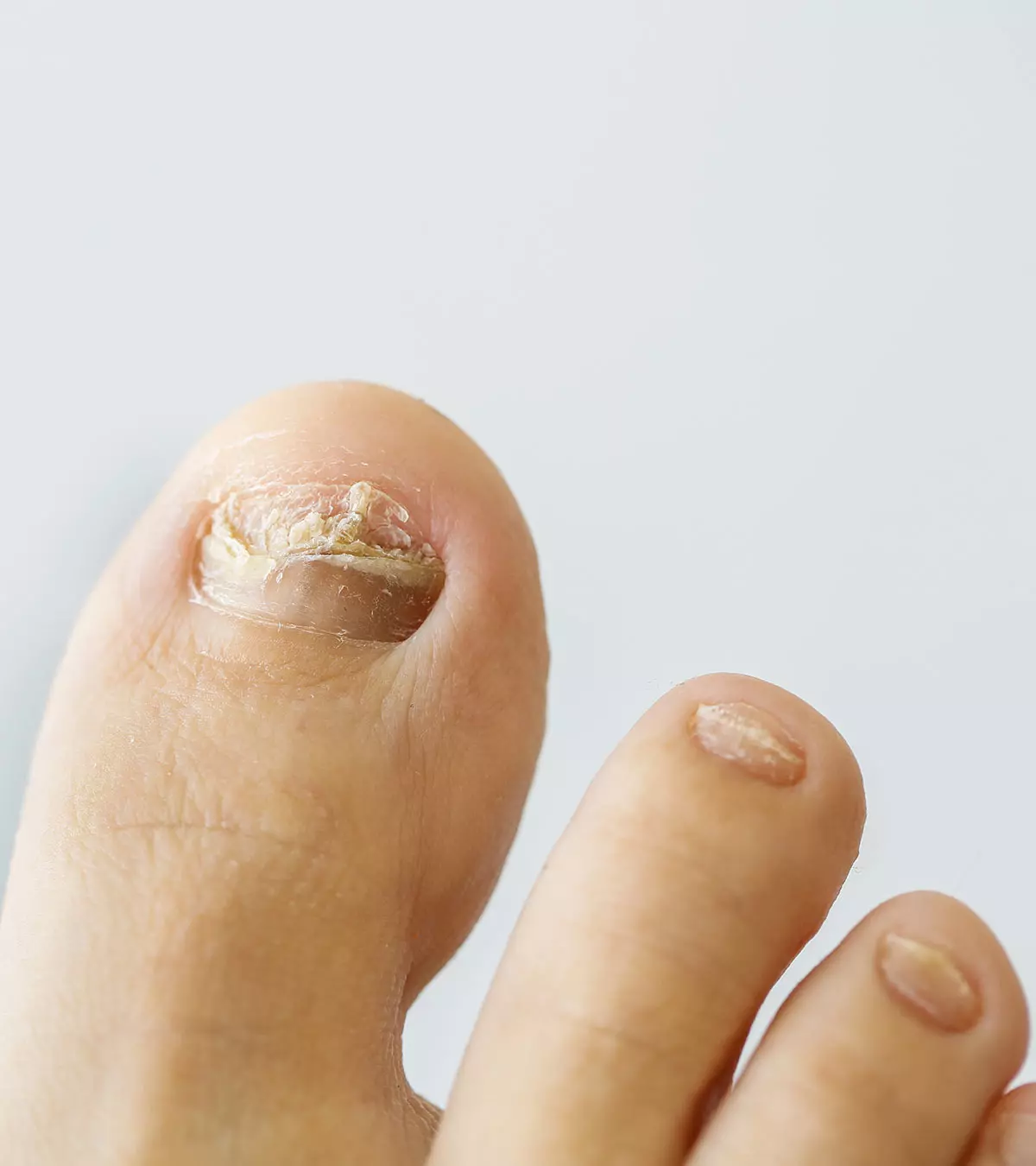
- Tinea unguium: When the nails are affected by a nail fungus.
- Tinea versicolor: Skin infection, often on the chest and back (4)
Each type of ringworm has different symptoms. Let’s see what they are.
 Quick fact
Quick factWhat Are The Symptoms Of Ringworm In Kids?
The symptoms of ringworm vary depending on the part of the body affected (5) :
1. Tinea capitis
- The scalp infection may begin as a small, red, scaly rash on the scalp and starts itching.
- The itching intensifies as the rash increases in size and becomes embossed in a ring-like pattern.
- You will notice hair loss at the spot of the ringworm. If there are several ringworms on the head, then you will see multiple circular bald areas on the scalp.
- Sometimes, due to severe inflammatory response, elevated boggyiMushy or wet surface granulomatousiA small area of cells that aggregate in response to an inflammation masses studded with pustulesiSmall reddish pus-filled bumps on the skin surface appear on the scalp (Kerion).
- It is the most common type of ringworm to occur in children.
2. Tinea pedis and tinea manuum
- Most commonly, the lateral toe webs (third to fourth and fourth to fifth interdigital space) are affected.
- The first symptoms are the development of reddish-white, moist, and itchy patches of the skin usually between the toes/fingers.
- Scales develop on parts of the feet/hand.
- The scales and red patches become itchy.
- You may eventually see itchy blisters on the sole of the feet in the case of tinea pedis.
- Sometimes, the infection begins from the sole of the feet instead of between the toes. Tinea pedis is more common in adolescents than in prepubertal children.
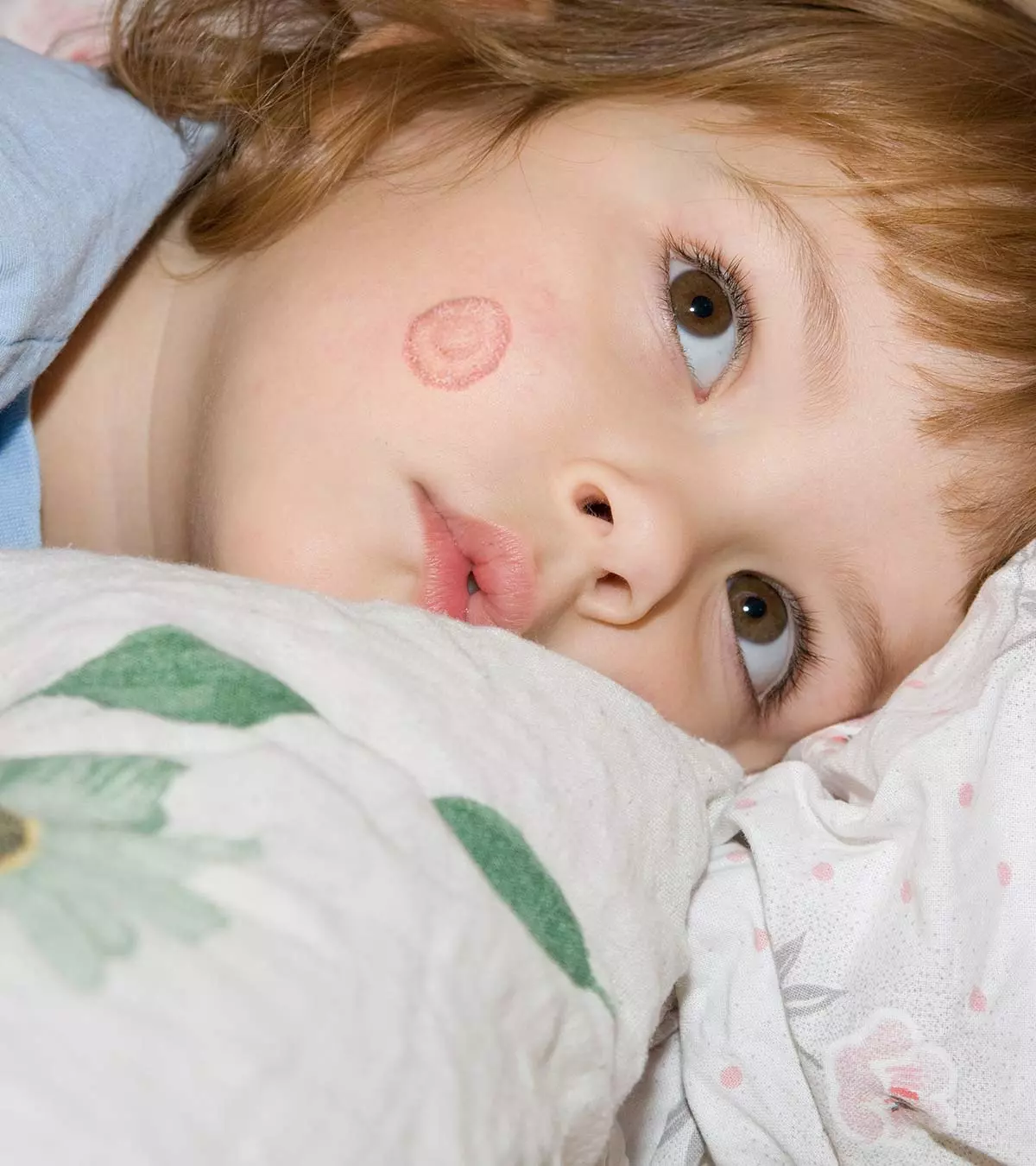
3. Tinea corporis and tinea faciei
- It usually has circular, ring-like lesions with clear skin at the center.
- In the case of tinea faciei, the fungus may show around the eyes, eyelids, and below the ear.
- The diameter of the lesion may appear to grow as the fungus spreads. The spreading fungus usually leaves the area in the center clear.
- The ring feels itchy and you may also notice white, flaky skin along the seam of the ring.
4. Tinea cruris
- Small, reddened patches of skin gradually expand to a larger lesion that flanks the genitals. The lesions are mostly concentrated around the folds of skin in the groin.
- The red patch expands and gets itchy. The fungus extends with a well-marked, scaly, red border.
- The fungus causing the groin infection does not occur on genitals. In boys, tinea cruris is seldom seen on the skin of the scrotum.
- Tinea cruris is also called jock’s itchiA fungal infection occurring in the moist regions of the body, especially the inner thighs, and genitals . It is most common in adolescent boys.
- It is more common in hot weather conditions.
5. Tinea unguium
- The nail ringworm has a different manifestation than other types of tinea.
- Nails thicken and have yellow patches. They may become brittle and flake.
- The patches expand and spread to the nail bed. The yellow patches darken to become grayish in color.
- Tinea unguium is less common in prepubertal children and mostly seen in adolescents.
- Nail ringworm is more likely to affect the toenails than the fingernails.
6. Tinea versicolor
- It is a fungal skin infection caused by yeast that affects only the top layer of the skin.
- The infection results in lighter or darker (white, pink, or light brown) patches or rashes on the skin, which commonly appear on the back and chest.
- The infection causes uneven tanning of the skin and worsens in hot and humid environments, thus, occurs more frequently in summer.
- Tinea versicolor is more common in teenagers and young adults than in children.
- Steroid medications and the weakened immune system of affected children can exacerbate skin rashes in children, making these patches and rashes worse (4).
How Do Kids Get Ringworm?
Children get the infection when the microscopic dermatophyte fungi settle on the skin and the conditions are right for it to spread and cause ringworm. Certain factors increase the risk of getting the infection (6) (7) (8):
- Living in a hot and humid environment: Hot and humid weather provides favorable conditions for a fungus to grow. Under these conditions, the child might sweat more than usual, which can cause the fungus to spread especially in moist parts like the groins and underarms.
- Playing in soil: Soil may contain the spores of the fungus. Children who spend a lot of time playing in the soil are susceptible to ringworm.
Recalling a moment when she observed possible signs of ringworm in one of her children, Dawn Gray, a mother and agriculturist, says, “My kids have been playing in a bunch of dirt we just brought in as we are expanding our Christmas tree farm parking lot. They’ve been digging, making forts, moving dirt, and just having a grand old time! Who knows if this could be the culprit or not (i).”

- Contact with animals: The infection might spread from pets like cats and dogs to your child on contact or through the sharing of their bed.
- Poor hygiene: Not washing hands after coming from play and touching/ scratching the skin with those dirty hands can transfer the fungus from the hands to the skin.
- Daycare centers and swimming pools: A child comes in contact with several other children at a daycare center. In such scenarios, the infection can spread from one child to another. Swimming in public pools also puts the child at a risk of contracting fungal infections.
- Playing contact sports: Children who play wrestling or any other sport that involves a lot of skin contact are at a higher risk of getting ringworm.
- Weakened immune system and health problems: Children who have a weak immune system are vulnerable to a host of fungal infections including ringworm. Diabetes can also increase the risk of skin infections including fungal infections.
- Sharing personal items: Scalp ringworm can spread from sharing combs while ringworm of the hand can spread through sharing of gloves.
- Some types of attire: Wearing tight socks for too long can cause feet to become sweaty and vulnerable to fungal infection. Staying in wet clothes for long, like after getting wet in the rain, may also increase the risk of ringworm.
- Direct contact: A child can catch the ringworm from an infected person or sibling, but only with direct skin-to-skin contact.

 Quick fact
Quick fact If your child has any of these risk factors and displays symptoms as mentioned in the previous section, you may take them to a doctor for a diagnosis.
How Is Ringworm In Children Diagnosed?
Early diagnosis of ringworm is crucial to prevent the spread of infection to others and reduce the risk of more severe complications, especially in vulnerable populations, such as children. A doctor uses the following diagnostic methods.
- Visual inspection: In most cases, doctors can diagnose ringworm by looking at the shape of the skin rash or lesion and its location on the body. The doctor will ask about the symptoms and any previous instances of skin infection. They may also want to know if you have any pets at home or if the child plays any contact sport like wrestling.
- Testing of the scraping: The symptoms of ringworm often overlap with other skin conditions like eczemaiA skin condition that causes itchy, red, and scaly patches on the skin due to various factors such as allergies, genetics, or stress and fungal infection such as candidaiA yeast genus capable of causing infections in the skin and genital regions . Therefore, the doctor may scrap and collect a tiny amount of the skin from the crusty lesions for laboratory testing. The scraping of the skin is painless. A microscopic examination and culture of the sample in a lab will determine the presence of fungus and also the type of it.
How Is Ringworm In Kids Treated?
Here are some medications commonly used to treat ringworm (9):
- Topical antifungal: Most cases of ringworm are treatable with the use of topical antifungals. It can either be a topical antifungal cream or powder. Common antifungal compounds are miconazole, clotrimazole, and tolnaftate. Your child will have to apply the ointment/powder two to three times a day for several weeks. Scalp ringworm will require a medicated shampoo that contains antifungal compounds.
- Oral antifungal: Oral antifungal drugs are specially used in tinea infection of scalp, hair, and nails. chosen when there are too many fungal lesions on the body or when the fungus is too stubborn like when on the nails. Oral antifungal medicines usually have stronger potency than topical antifungal and may cause side effects on overdose. They can have side effects such as nausea, liver toxicity, and allergic reactions. Therefore, oral antifungals should only be given as per the doctor’s prescription. Common oral antifungal compounds are griseofulvin, terbinafine, fluconazole, and itraconazole.
The doctor may also prescribe additional items like an antifungal soap and a medicated skin lotion to reduce the spread of the ringworm further.
How Long Does Ringworm Last In Kids?
Ringworms can take a week to 3-4 weeks after the initiation of medication to cure completely. In most cases, ringworm does not last for more than a month since the beginning of the treatment.
Children with immunity problems like those with AIDS and cancer may have the infection for longer. There are no complications of ringworm and once the infection is treated, the child will have healthy skin.
What Are The Home Remedies For Ringworm In Kids?
There is no effective home remedy against ringworm in children. Some items are quite popularly used as a home cure for ringworm, but most do not cure the condition completely.
A few home remedies for ringworm are apple cider vinegar, tea tree oil, coconut oil, and garlic paste. These are often applied to the infected area using a cotton ball. Evidence suggests that these items contain antifungal properties (10) (11) (12), but there is no reliable proof that these agents can eliminate the fungi entirely.
Nevertheless, it is best to avoid home remedies if the child is on medication since home remedies could interfere with the effective action of drug compounds.
Prevention is the best thing you can do at home to protect your child from ringworm.
How To Prevent Ringworm In Kids?
Preventing ringworm in children is easier than you think. Here is what you can do:
- Maintain good hygiene: In most cases, children get ringworm because of poor personal hygiene. For instance, not washing hands after playing in soil or touching stray animals can cause the child to contract an infection. Also, change your child’s bed sheets once a week to prevent fungal spores from settling into it.
- Teach the child not to share personal items: Tell your child that they must always keep things like clothes, towels, and combs private and not share them with anyone.
- Avoid contact with ringworm on others: If they see another child with blotches, blistering or a strange lesion on their skin, they should not touch it. This instruction is particularly crucial for children going to daycare centers and schools.
- Regularly check pets for ringworms: Even if you maintain hygiene at home, pets can bring ringworm from outside. Check your pet’s skin periodically for any signs of ringworm. If you see a strange blister/lesion and suspect it to be a fungal infection, then take your pet to a veterinarian.
- Dress your child appropriately: During hot and humid weather, keep your child dressed in loose, comfortable clothing made from natural fibers like cotton that allow ventilation. Make sure the undergarments are not too tight or ill-fitting. If your child gets drenched in the rain, then ask them to change to dry clothes soon to prevent providing a moist environment for body fungal infection.

Frequently Asked Questions
1. Is ringworm infection serious in children?
Untreated or inadequately treated ringworm infection may become serious and spread all over the body. It may also affect the nails, making them brittle, and the scalp, leading to bald patches (13).
2. How long is a child contagious with ringworm after treatment?
The ringworm infection is no longer contagious 48 hours after treatment (14).
3. Can ringworm in kids lead to permanent scarring or hair loss?
In children, scalp ringworm can result in a serious condition known as kerion. Kerion can lead to scarring and permanent hair loss by damaging the hair follicles (15). Seeking immediate medical attention is crucial, particularly when kerion is present, to ensure accurate diagnosis, and treatment, and minimize complications.
Ringworm in kids is a contagious fungal infection that resolves in three to four weeks after treatment initiation. It spreads from contact with an infected person or pet, sharing an infected person’s things, and not maintaining proper hygiene. Depending on the body part they affect, ringworm can be of various types. Since ringworm causes itchy rashes and may even turn into skin peeling, its timely diagnosis and treatment are essential for prompt relief. Ensuring proper personal hygiene, teaching children not to share personal things, and avoiding contact with an infected person or pet will help prevent ringworm infection.
Infographic: Ringworm Infections And Schools
When your child has a ringworm infection, or you hear somebody in their school contracted one, you start contemplating whether to send them to school or not. This infographic will clear your confusion and provide you with the steps to be taken in such a situation. Illustration: Momjunction Design Team
Illustration: Ringworm In Kids: Types Causes Symptoms Treatment & Care

Image: Dall·E/MomJunction Design Team
Discover practical and safe methods for quickly eliminating ringworm in children in this informative video, which provides essential help for quick resolution.
Personal Experience: Source
MomJunction articles include first-hand experiences to provide you with better insights through real-life narratives. Here are the sources of personal accounts referenced in this article.
i. Say goodbye to ringworm;https://sonshineinthewildwood.blogspot.com/2014/09/say-goodbye-to-ringworm.html
References
1. M.D. Andrews & M. Burns, Common Tinea Infections in Children; American Academy of Family Physicians
2. Tinea Infections (Ringworm); University of Rochester
3. Tinea (Ringworm); American Skin Association
4. Stanford Medicine Children’s Health; American Skin Association
5. Tinea Infections (Ringworm) in Children;Children’s Hospital of Philadelphia
6. Abhineetha Hosthota, Trupthi Gowda, Rajini Manikonda; Clinical profile and risk factors of dermatophytoses: a hospital based study; International Journal of Research in Dermatology (2018)
7. Olaide Oke Olutoyin, Olaniyi Onayemi, and Akinlolu Omisore Gabriel; Risk factors associated with acquiring superficial fungal infections in school children in South Western Nigeria: a comparative study; African health Sciences (2017)
8. Nourchène Toukabri, Cyrine Dhieb, Dalenda El Euch, Mustapha Rouissi, Mourad Mokni, and Najla Sadfi-Zouaoui; Prevalence, Etiology, and Risk Factors of Tinea Pedis and Tinea Unguium in Tunisia; Canadian Journal of Infectious Diseases and Medical Microbiology (2017)7. A.C. Mota et al., Antifungal Activity of Apple Cider Vinegar on Candida Species Involved in Denture Stomatitis; National Center for Biotechnology Information
9. A.C. Mota et al., Antifungal Activity of Apple Cider Vinegar on Candida Species Involved in Denture Stomatitis: National Center for Biotechnology Information
11. B. Shino et al., Comparison of Antimicrobial Activity of Chlorhexidine, Coconut Oil, Probiotics, and Ketoconazole on Candida albicans Isolated in Children with Early Childhood Caries: An In Vitro Study; National Center for Biotechnology Information
12. Pai & Platt, Antifungal effects of Allium sativum (garlic) extract against the Aspergillus species involved in otomycosis; National Center for Biotechnology Information
13. Ringworm; The Royal Children’s Hospital Melbourne
14. Ringworm; Seattle Children’s
15. Ringworm (scalp) – Symptoms and causes; Mayo Clinic
16. Ringworm and Fungal Nail Infections Basics; Centers For Disease Control And Prevention
17. Tinea (Ringworm); Government Of Queensland
Community Experiences
Join the conversation and become a part of our nurturing community! Share your stories, experiences, and insights to connect with fellow parents.
Read full bio of Dr. Saroj Kumar
Read full bio of Dr. Ritika Shah
Read full bio of Swati Patwal
Read full bio of Ghazia Shah