Image: Shutterstock
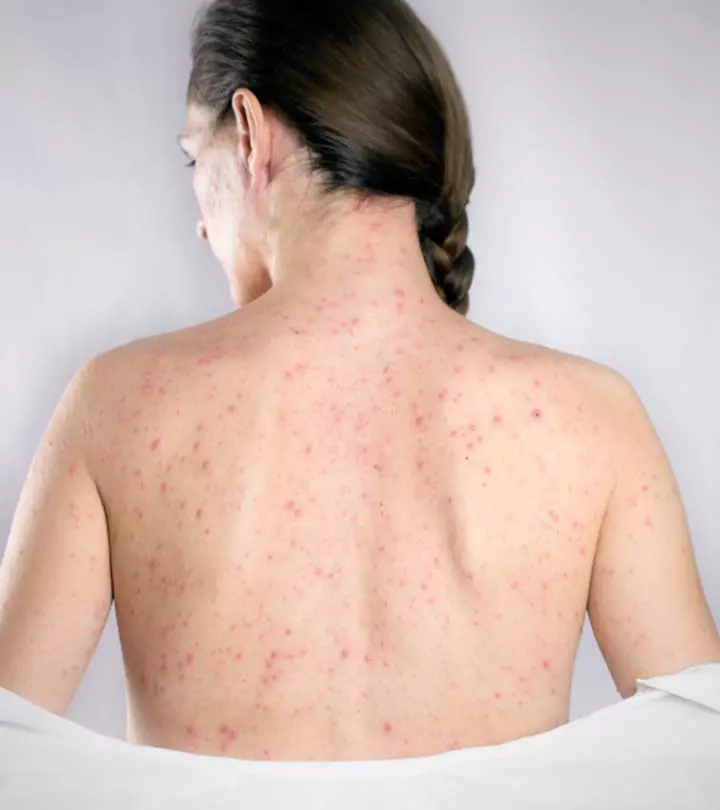
Shingles is a viral infection that manifests as painful rashes or blisters, often on one side of the body or face (1) (2). Shingles or herpes zoster and chickenpox share a common causative agent, varicella zoster virus. If you are affected with shingles in pregnancy, it is not known to cause fetal complications. Although rare, the availability of different pregnancy-safe treatments can help alleviate the symptoms of shingles and discomfort. In general, around one in every three people in the US develop shingles and are mostly above 50 years (3).
The below post discusses shingles in pregnancy, including its causes, symptoms, and treatments.
Key Pointers
- Shingles is an infection caused by the varicella zoster virus, which may result in symptoms such as high fever, malaise, rash, and fluid-filled itchy blisters.
- Stress, fatigue, underlying health conditions, exposure to radiation, poor nutrition, and the use of immunosuppressants can increase the risk of developing shingles.
- While shingles usually does not pose a threat to pregnancy, the mother may experience complications if the infection persists for more than four weeks.
- Treatment for shingles involves the use of prescription antiviral drugs, painkillers, and measures to soothe the rashes and blisters.
What Are The Causes Of Shingles?

Shingles is a secondary infection of chickenpox contracted from another person containing the virus. It remains dormant in the posterior root ganglioniA group of nerve cells in the dorsal root of a spinal nerve after the primary infection (chickenpox) and travels to the skin upon reactivation, resulting in shingles (4).
Besides the advancing age and the body’s natural changes, a person who has had chickenpox may develop shingles later in life from other factors as follows (4) (5):
- Underlying health conditions, such as HIV or cancer that compromise the immune system
- Exposure to radiation or chemotherapy
- Lack of nutrition
- Stress and fatigue
- Intake of immunosuppressantsiDrugs that reduce the body’s immune responses , including cyclosporin or corticosteroids
- Exertion of pressure on the nerve root
 Things to know
Things to knowWhat Are The Symptoms Of Shingles In Pregnancy?
The manifestation of shingles usually proceeds in stages. These are (2) (6):
Early symptoms:
- Pain or tingling sensation in the affected area
- MalaiseiA state of weakness, general discomfort, disease, or just not feeling well or headache
- High temperature

- Sensitivity in the area of the skin before the rash occurs
Later symptoms:
- Development of painful rash in the tingling area of the skin about one to five days after the early symptoms
- Formation of fluid-filled itchy blisters over the rash after seven to ten days
Symptoms can appear anywhere in the body— around the stomach, the chest, and the eyes. However, they typically occur only on one side of the body and are expected to subside within two to four weeks without posing any threat to the baby or the pregnancy. However, it is still better to recognize the symptoms early on for timely intervention and to minimize any severe and painful rashes.
Celine, a mother and a dancer, was six and a half months pregnant when she contracted Shingles infection. She says, “I have shingles currently on the left side of my face. There are blisters on the chin, and some under the chin as well. I have some on my head, on my ear, and inside my ear as well (i).” She was prescribed antiviral medication acyclovir, and her condition improved thereafter.
 Quick fact
Quick factWhen To See A Doctor?

If you have contacted an infected patient, you should consult a healthcare provider immediately for timely treatment. This might help shorten the disease’s duration and reduce the severity. A prolonged manifestation may cause pregnancy complications if not addressed in time.
How Is Shingles In Pregnancy Diagnosed?
Upon manifestation, the healthcare provider may want to know if you’ve had chickenpox in the past and any direct contact with an infected person. Diagnosis involves a lab test, where a small portion of the rash is scraped and examined. Upon confirmation, the healthcare provider will proceed with effective and pregnancy-safe treatment (2).
How Is Shingles In Pregnancy Treated?
Below are some medications and home measures you can follow only after consultation with a healthcare provider (7) (8):
- Antiviral drugs: Acyclovir during pregnancy is considered a safe and effective option, especially when treating shingles in the early stages. Classified as a category B antiviral medication, acyclovir, valacyclovir, and famciclovir are recommended for use during pregnancy. The medicines are likely to be effective when taken within 72 hours of blister eruption.
- Painkillers: Analgesics include category B drugs, such as acetaminophen and short-term opioid medicinesiA kind of medication obtained from the opium poppy plant and is used to manage moderate to severe pain . Most opioid medicines except for codeine are safe for pregnancy with proper monitoring. Acetaminophen is usually prescribed for relief from severe neuritisiA condition that causes inflammation of one or more nerves of the peripheral nervous system, primarily because of infection or injury pain.
- Self-care measures: Some recommended home measures include:
- Cold compresses on the rashes or blisters for pain relief
- Lukewarm baths
- Application of calamine lotion and other creams (pramoxine or menthol) for relief from itchiness
Note: Some medications are not suitable for pregnant people, and the over-the-counter medicines should not be taken without a doctor’s prescription.
Can You Prevent Shingles?
Prevention of shingles can be achieved only by taking the Herpes zoster vaccine or the shingles vaccine, Shingrix. CDC recommends it for people of 50 years and above. The vaccine is given in two doses, with the second dose administered after two to six months of the first one. Shingrix is more than 90% effective, and you will be immune at least for about seven years from the time of vaccination (9).
If pregnant women contract the disease, they should not get the vaccination until post-delivery. Women who have had Shingrix vaccination are recommended to wait for at least one month to get pregnant (10). Since the virus can be transferred from a person with shingles to another person, it is better to stay away from infected people and maintain good hygiene for the safety of yourself and your fetus.
What Are The Complications Of Shingles During Pregnancy?
Complications may arise if the symptoms of shingles persist for longer than four weeks. They can include (2) (7):
- Postherpetic neuralgia (PHN): Patients with severe pain or compromised senses during the infection can be at a higher risk of PHN. It is characterized by acute pain that can last for 30 to 90 days even after the blisters subside. Early treatment can help prevent further problems with category B opioids as it is the common and safe treatment choice.
- Secondary bacterial infection: The rash may be further infected by a bacterial agent, which is not commonly seen in pregnant women. The healthcare provider may prescribe oral antibiotics for the bacterial infection, mostly for staphylococcal or streptococcal infections, for the baby’s safety.
- Vision impairment: If the rash develops around the eyes, it can compromise the vision of the infected person through an infection in the cornea. This can further lead to temporary or permanent loss of sight.
Can Shingles Cause Miscarriage?
According to experts, miscarriage is common and can occur due to different reasons. However, no studies have been done to see if shingles can raise the risk of pregnancy loss (11). Shingles itself can’t cause miscarriage. However, the herpes zoster virus that causes shingles also causes chickenpox. If contracted at the 20th week, chickenpox can pose a risk to the developing fetus. Besides, it raises the risk of congenital varicella syndrome or other complications, including a higher miscarriage risk (3). Therefore, if you observe symptoms of shingles, consult your doctor. They will evaluate the situation, assess the risk, and initiate suitable treatment to ensure your and your unborn baby’s safety.
Frequently Asked Questions
1. I’m pregnant, and I have shingles. Will this harm my baby?
Shingles do not cause fetal complications or increase the chance of birth defects. However, if an unvaccinated pregnant woman contracts the virus for the first time during pregnancy, it can lead to chickenpox. Chickenpox during pregnancy, unlike shingles, can pose a threat to the baby in the form of congenitaliPhysical anomaly that exists since birth varicella syndrome orneonatal varicellaiA rare disorder where babies have issues because their mothers got infected by chickenpox during the last three weeks of pregnancy depending on the time of exposure (11) (3).
2. What if my husband has shingles when I am pregnant?
If a pregnant woman has been vaccinated against chickenpox or exposed before, she is not at risk of contracting the disease from her infected husband. However, if an unvaccinated pregnant woman’s intimate partner has shingles, she may be infected (11).
3. How can I protect my newborn if I have shingles?
Shingles are non-contagious and also cannot spread through breast milk. A few steps such as not feeding from the breast that has lesions and using a pump, and washing hands often are some of the steps you should follow. If the newborn comes in contact with shingles lesion, check with the pediatrician if they think the baby should receive Varicella Zoster Immune Globulins (13).
Shingles will not raise concerns for the mother or the baby. The best way to prevent shingles is by getting vaccinated before pregnancy and maintaining distance from the infected people. It is important to be aware about the symptoms to seek appropriate and timely treatment to prevent further complications.
Infographic: Identification And Treatment Of Shingles During Pregnancy
Although shingles does not affect the fetus and typically goes away on its own, their blisters can cause pain and discomfort in pregnant women. Knowing the early symptoms and safe treatments can help subside the infection sooner. Read the infographic below to learn about the early symptoms of shingles and how to treat it safely during pregnancy.
Some thing wrong with infographic shortcode. please verify shortcode syntax
Illustration: Shingles In Pregnancy: Causes Symptoms And Treatment

Image: Dall·E/MomJunction Design Team
Personal Experience: Source
MomJunction articles include first-hand experiences to provide you with better insights through real-life narratives. Here are the sources of personal accounts referenced in this article.
i. Shingles after a root canal while 6 months pregnant.https://www.youtube.com/watch?v=XLWZ0OB2xRM
References
- About Shingles (Herpes Zoster).
https://www.cdc.gov/shingles/about/index.html - Shingles.
https://myhealth.ucsd.edu/Conditions/Pregnancy/85,P00328 - Shingles exposure during pregnancy.
https://www.marchofdimes.org/find-support/blog - Herpes zoster.
https://dermnetnz.org/topics/herpes-zoster - What is shingles?
https://www.aao.org/eye-health/diseases/herpes-zoster-shingles - Shingles.
https://www.nhs.uk/conditions/shingles/ - Svidal Kimberly Rn (2026). Herpes Zoster in Pregnancy.
https://commons.und.edu/cgi/viewcontent.cgi?article=1306&context=nurs-capstones - Am Fam Physician
(2011). Acyclovir Safe for Treating Herpes Infection in Early Pregnancy. - Shingles Vaccination.
https://www.cdc.gov/shingles/vaccines/index.html - Shingles and pregnant women.
https://jamaicahospital.org/newsletter/shingles-and-pregnant-women/ - Herpes zoster (Shingles).
https://mothertobaby.org/fact-sheets/herpes-zoster-shingles/ - Shingles.
https://my.clevelandclinic.org/health/diseases/11036-shingles - Shingles
https://www.cdc.gov/breastfeeding/breastfeeding-special-circumstances/maternal-or-infant-illnesses/shingles.html
Community Experiences
Join the conversation and become a part of our nurturing community! Share your stories, experiences, and insights to connect with fellow parents.
Read full bio of Dr. Kritika Shashank Verma
Read full bio of Aneesha Amonz
Read full bio of Rebecca Malachi
Read full bio of Dr. Joyani Das

 Quick tip
Quick tip