
Image: ShutterStock
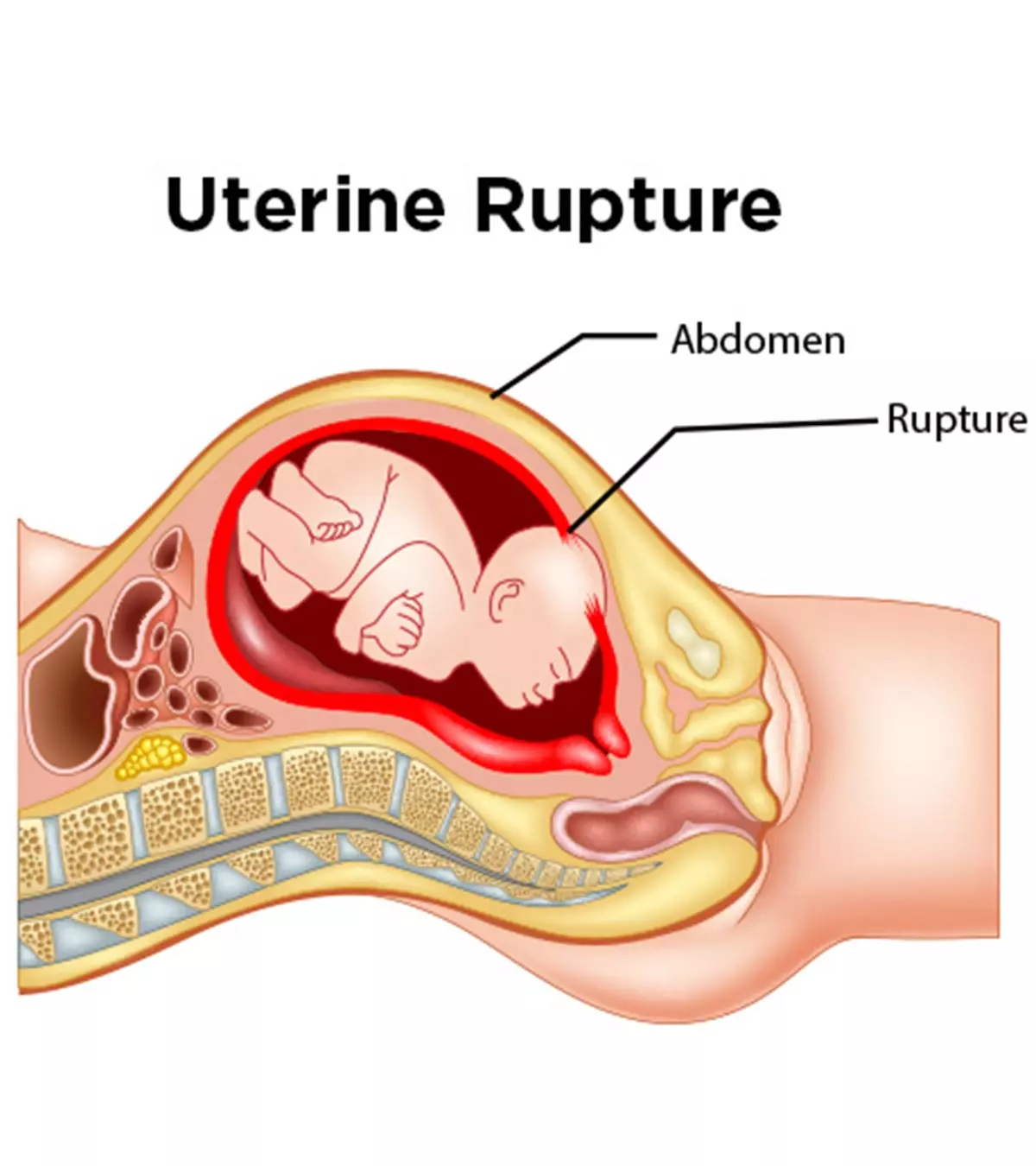
Uterine rupture is the spontaneous tearing of the womb or uterus. Although it can occur in any woman, pregnant women are at higher risk. It is a rare but serious childbirth complication affecting less than one percent of pregnant women (1). Rupture of the womb during pregnancy or labor can be life-threatening for both mother and the baby.

Emergency interventions are recommended to improve the chances of the baby’s survival. Therefore, it is important to know the initial signs and seek immediate medical care. Read on to learn more about the causes, signs, symptoms, and management of uterine rupture and ways to prevent it.
What Causes Uterine Rupture?
Uterine rupture usually occurs along the healed scar of the previous C-section, most commonly among the women who may undergo vaginal birth after cesarean delivery (VBAC). It can be caused by increased pressure in the birth canal, as the baby moves through it during labor.
When the pressure is too intense, it stresses the scar tissue that had formed during the previous surgery. This could lead to a tearing inside the womb and result in internal bleeding, umbilical cord compromise, and placental injury.
Factors that increase the risk of a ruptured womb include:
- A previous C-section
- Vaginal birth after a C-section
- Fibroid surgery, also known as myomectomy
- Uterine repair surgery (removal of a portion of the uterus, removal of the uterine septum or repair of a badly injured uterus)
- Having a body mass index (BMI) of above 30
- Medically induced labor
A ruptured uterus can pose health risks for the baby. Once your healthcare provider diagnoses a uterine rupture, an emergency cesarean section is necessary to pull out the baby from the womb (1).
What Are The Signs and Symptoms Of Uterine Rupture During Pregnancy or Labor?
Uterine rupture can be an incomplete rupture, where the peritoneum overlying the uterus is intact, or a complete rupture where the uterine contents are disrupted (2). The severity of the signs and symptoms may vary based on the type and duration of rupture.
The signs and symptoms associated with uterine rupture during pregnancy or labor include (1) (3):
- Rapid heart rate
- Low blood pressure
- Severe abdominal pain
- Excessive vaginal bleeding
- A sharp pain between contractions
- A recession of fetal head into the birth canal
- A bulge beneath the pubic bone
- Sudden pain in your previous uterine scar
- Loss of uterine muscle tone
- Abnormal fetal heart rate
- Labor fails to progress naturally
If you notice any of these symptoms, call your doctor immediately for further diagnosis and treatment.
How Is Uterine Rupture Diagnosed?
Most of the symptoms discussed above are non-specific, which makes it difficult to diagnose the condition. Diagnosis is confirmed only after laparotomy, which is a surgery to open the abdominal wall. Usually, if there are signs and symptoms of fetal distress, and there is a suspicion of uterine rupture, immediate laparotomy is done.
Abnormal fetal heart rate and reduced movement on the biophysical profile indicate fetal distress. Some may use intrauterine pressure monitoring. However, it is recommended to do emergency surgery and delivery to avoid complications (1).
How Is Uterine Rupture Treated During Pregnancy or Labor?
Emergency C-section is indicated in the case of uterine rupture. If there are signs of fetal distress, such as abnormal fetal heart rate and decreased fetal movement, a c-section delivery may be recommended.
The mother will receive fluid and blood transfusion as required. Confirmation and surgical repair of the uterus rupture are done during the delivery. However, some women may require a hysterectomy (removal of the uterus) if there is life-threatening hemorrhage (1) (4).
Doctors may transfer the baby to neonatal care based on status, and the mother will undergo surgery for the uterus repair or removal.
Can You Prevent Uterine Rupture During Pregnancy?
Uterine rupture can be through a planned cesarean section. It cannot be avoided if you go for a vaginal birth.
Next, we answer a few commonly asked questions by our readers.
Frequently Asked Questions
1. Can you predict uterine rupture during pregnancy?
The strength of the scar can be assessed in the later stages of pregnancy when an ultrasound or MRI is performed to measure the womb’s thickness. However, scans are usually performed to check for abnormalities such as low-lying placenta and not to diagnose or predict a possible uterine rupture.
2. Does uterine rupture harm the mother and the baby?
Uterine rupture is unlikely to cause harm to the mother if treated on time. But it could cause serious complications, such as oxygen deprivation in the fetus (1). This risk is less in the case of a planned C-section.
3. What are the chances of pregnancy after a uterine rupture?
It is possible to be pregnant after uterine rupture. However, this may carry an increased risk for rupture of the uterus again, and chances of pregnancy may vary based on the extent of damage the rupture has caused. Though the physician may recommend vaginal delivery after C- section, it is not recommended if you have a history of uterine rupture during the previous pregnancy.
4. What is a uterine window?
A uterine window is an incomplete rupture where the uterine wall becomes so thin that the baby is visible through the thinned uterine muscle (5). It develops when the covering of the uterine wall called perimetrium is not damaged, but the inner layers (myometrium and endometrium) are torn
This eventually progresses to uterine rupture upon stress. With this condition, the risk of uterine rupture increases in subsequent pregnancies, and therefore doctors suggest a tubal ligation to prevent uterine complications.
Uterine rupture is usually seen along the uterine scar made during previous C-section delivery. The rupture occurs when the woman has subsequent pregnancy and tries natural childbirth. If you had a previous C-section delivery and intend to have a natural delivery, speak to an expert about your health status and learn the risks of experiencing uterine rupture. If your doctor thinks it is safe, you may have a vaginal birth. However, an emergency C-section is recommended in women who have other complications or signs of fetal distress.
Do you have any experiences to share? Tell us about them in the comments section below.
References
- Kevin S. Toppenberg and William A. Block; Uterine Rupture: What Family Physicians Need to Know; The American Academy of Family Physicians
https://www.aafp.org/pubs/afp/issues/2002/0901/p823.html - Ishraq Dhaifalah, et al.; Uterine Rupture During Pregnancy And Delivery Among Women Attending The Al-tthawra Hospital In Sana’a City Yemen Republic
https://citeseerx.ist.psu.edu/viewdoc/download?doi=10.1.1.483.9972&rep=rep1&type=pdf - Uterine rupture; Médecins Sans Frontières (MSF); medical guidelines
https://medicalguidelines.msf.org/en/viewport/ONC/english/3-3-uterine-rupture-51416296.html - Maruti Sinha, et al.; Uterine rupture: A seven year review at a tertiary care hospital in New Delhi, India
https://www.ijcm.org.in/article.asp?issn=0970-0218;year=2016;volume=41;issue=1;spage=45;epage=49;aulast=Sinha - Lim AC, et al.; Pregnancy after uterine rupture: a report of 5 cases and a review of the literature.
https://www.ncbi.nlm.nih.gov/pubmed/16121116 - N. KOK, et al.; Sonographic measurement of lower uterine segment thickness to predict uterine rupture during a trial of labor in women with previous Cesarean section: a meta-analysis
https://obgyn.onlinelibrary.wiley.com/doi/pdf/10.1002/uog.12479
Community Experiences
Join the conversation and become a part of our nurturing community! Share your stories, experiences, and insights to connect with fellow parents.
Read full bio of Dr. Surakshith Battina
Read full bio of Rebecca Malachi