Image: Midjourney/ MomJunction Design Team
Babies have sensitive skin, making them more susceptible to infections and allergies that may cause rashes in babies, a common condition during infancy. Understanding the causes of rashes is crucial for parents, as early identification can lead to effective treatment and prevention measures. Sometimes rashes could be due to an underlying illness and require prompt medical care. Timely diagnosis and treatment of rashes are important since it could be a simple heat rash or an allergic reaction. Read on to know more about rashes, their causes, symptoms, treatment, and ways to deal with them in babies.
 Did you know?
Did you know?Key Pointers
- Rashes are a common occurrence during infancy, and timely identification and diagnosis are necessary to prevent adverse outcomes.
- Some viral diseases that may cause rashes include Chicken pox, measles, hand, foot, and mouth disease, molluscum contagiosum, warts, fifth disease, and dengue.
- Scarlet fever, folliculitis, and impetigo are some bacterial diseases that can cause rashes in children.
- Rashes can also occur due to infections caused by worms, fungus, and skin parasites.
- Maintaining good hygiene, ensuring immunization, monitoring allergies, and dressing the baby comfortably can help reduce the incidence of skin rashes in babies.
What Are The Different Causes Of Rashes In Babies?
Rashes can be categorized based on what causes them. The following is a list of the most common illnesses that cause skin rashes among infants (1) (2) (3):
1. Heat rash
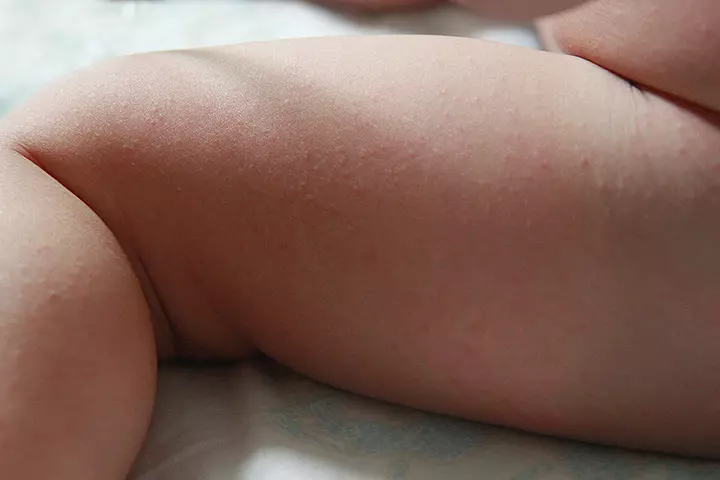
Heat rash is medicinally called miliaria, and results due to the accumulation of sweat within the pores of the sweat gland, due to excess perspiration. Tiny red bumps cluster together to form heat rash in babies, also called prickly heat.
Symptoms: Fine red and pink rashes around skin folds like underarms, between the joints, and under the thighs. Rashes also appear around the neck, face, and the groin area.
Treatment: A baby prickly heat powder can provide relief to the baby. Keep the affected area exposed to air and do not apply creams or ointments on it. Since heat rashes mostly happen during hot and humid weather, it is okay to leave the baby bare to provide relief from the rash.
2. Skin hives
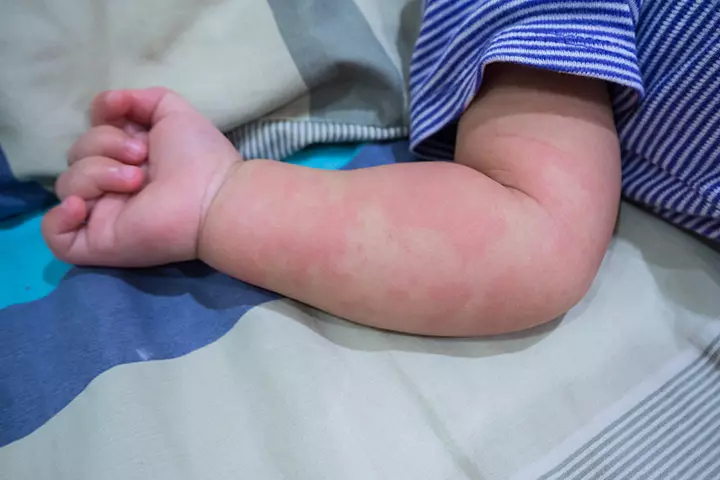
Allergies stimulate the release of a compound called histamine, which causes blood plasma to leak into the skin and form skin hives (4). Skin hives are medically called urticaria (5). Papular urticaria, which is similar to regular skin hives, is mostly a result of insect bites (6).
A mild skin rash may occur when the baby is teething, although it is not always the case. Teething may cause a rash around the mouth due to the excessive drooling caused by teething.
Symptoms: Tiny, reddish to pink bumps that appear in clusters or scattered around the body. The rash may ooze liquid when scratched.
Treatment: Treating the rash involves treating the underlying cause of skin hives, which is an allergy. Avoiding the allergen, use of corticosteroid cream and antihistamine medicines can help subdue the allergy, which in turn cures the skin hives. See a doctor before administering medicines to an infant.
3. Eczema
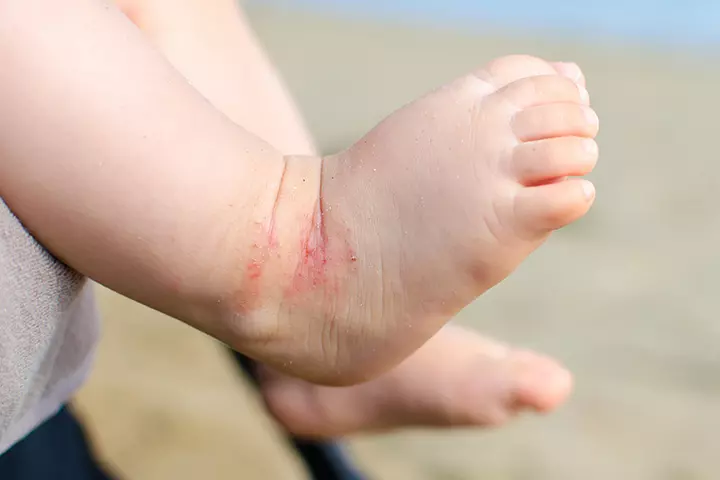
There is no single cause for the condition, and it is often induced by external factors such as overheating, sweating, and friction of the skin. There are several types of eczema. Eczema due to general reasons is called atopic dermatitis. Eczema caused by friction and contact with a substance is called contact and irritant dermatitis respectively (7). According to a population-based global survey by multiple institutions comprising 65,661 participants, the overall pediatric prevalence of atopic dermatitis among the pediatric population in the US is estimated to be 9.8%.
Symptoms: Dry, scaly, or crusty skin with very fine rashes that often appear as clusters. Eczema rash can appear anywhere, but it most commonly affects the limbs, face, folds of the skin, and areas that may have friction with clothing, such as the diaper area and waist.
 Quick fact
Quick factTreatment: There is no single cure for eczema. Topical treatment may ameliorate symptoms but are unlikely to address the underlying cause. These include, corticosteroid creams, skin moisturization with eczema-specific moisturizing lotions, calamine lotion, and use of natural, soft fibers for clothing. Also, discourage scratching, which exacerbates eczema.
Wet wraps are also recommended for managing the symptoms of eczema in babies and children, typically overnight.
4. Fungal infections
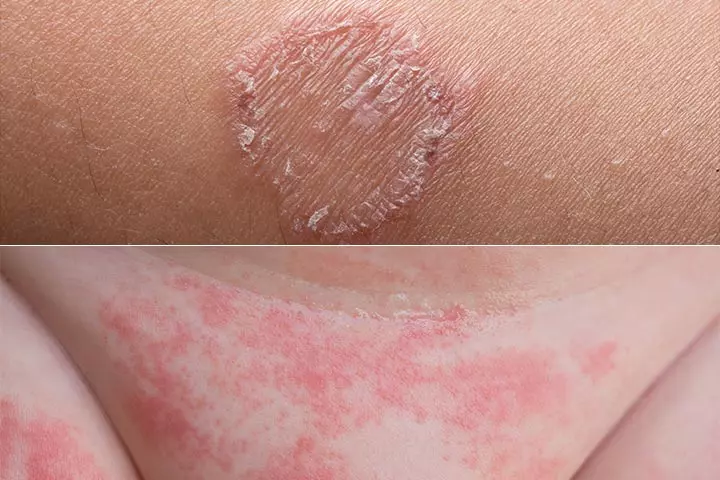
The most common fungal infections to affect infants are tinea (ringworm) and candidiasis (yeast infection). Ringworm is caused by any fungus belonging to a group of fungi called dermatophytes. Candidiasis is caused by a fungus belonging to the Candida genus, which is commonly called yeast responsible for diaper rash. Restrictive clothing, trapped moisture, and skin-to-skin contact with an infected individual or even a pet cause the spread of the infection.
Yeast infections could indicate a disruption in microbiome health internally as well as externally and indication for probiotic therapy.
Symptoms: Tinea infection appears as a round circular lesion, made of fine red rashes, presented at multiple parts of the body. The lesion can be of any diameter and resembles a coiled worm, which gives it the name. Candidiasis appears as reddish, scaly rashes mostly around skin folds such as the groin and underarms. The rashes may have whitish bumps in between or a white, semi-liquid substance attached to it.
Treatment: Usually, topical antifungal creams are enough to cure fungal infections. In very severe cases of infection, the baby may need oral antifungal medication. Treatment often lasts for several weeks to even months. Keeping the affected area dry, washing the baby’s clothes and towels in warm water will prevent the fungus from spreading.
Bridget Teyler speaks about what helped with her daughter’s diaper rash in her YouTube video. She says, “With my own daughter, when we experienced the yeast infection, we did the baking soda bath, we aired it out, we used lanolin, and we gave her the probiotic every day, and it cleared out quickly and only with natural products on her sensitive skin and in her body (i).”
5. Skin parasites
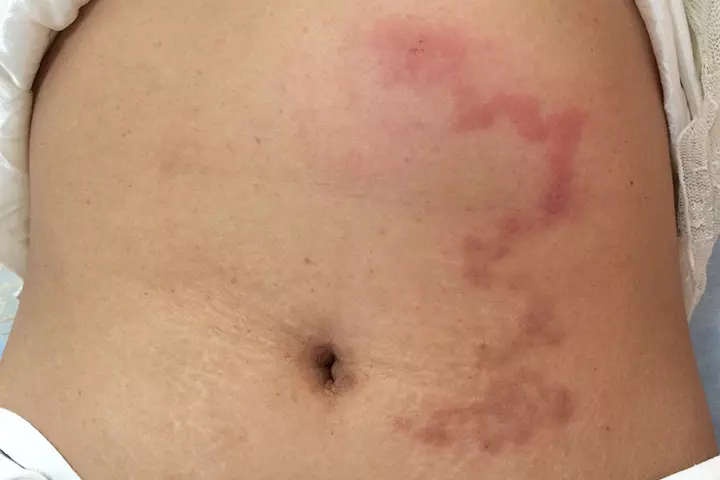
Examples of some skin parasites that can cause rashes are sandworm and microscopic parasites from snails. Infants are most likely to acquire these by playing in contaminated soil or seawater at the beach.
Symptoms: Rashes appear as raised bumps scattered across one region. Some parasites tend to migrate within the skin, thus leaving rashes and a raised trail behind them.
Treatment: The treatment is systemic with the use of anti-helminth (antiparasitic) topical creams and oral medicines. Discouraging itching and application of calamine lotion are ways to tackle the irritation caused by the skin rashes.
6. Chickenpox
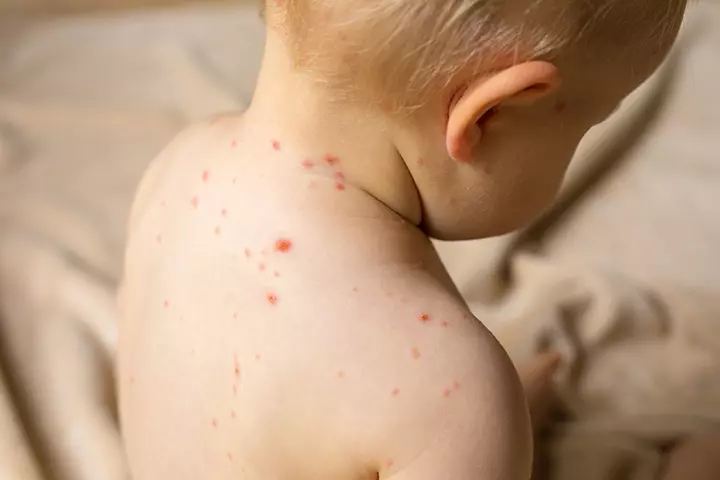
The varicella-zoster is a herpes virus that causes chickenpox. The virus transmits through inhalation of saliva and mucus droplets expelled by an infected person. It may also spread through contact with a chickenpox blister when it is in the contagious stage.
Symptoms: Chickenpox rash has a characteristic puffiness and is fluid-filled. The rash also has an inconsistent shape and can randomly appear on any part of the body. The rash gradually dries to form a scab in a week and falls off.
Treatment: The disease does not have any medication and clears on its own in a week or two. Most infants do not require medical attention for chickenpox. Adequate home care will do (8). Monitor temperature and attend a doctor or accident and emergency if an infant sustains a high fever and/or is unresponsive.
7. Measles
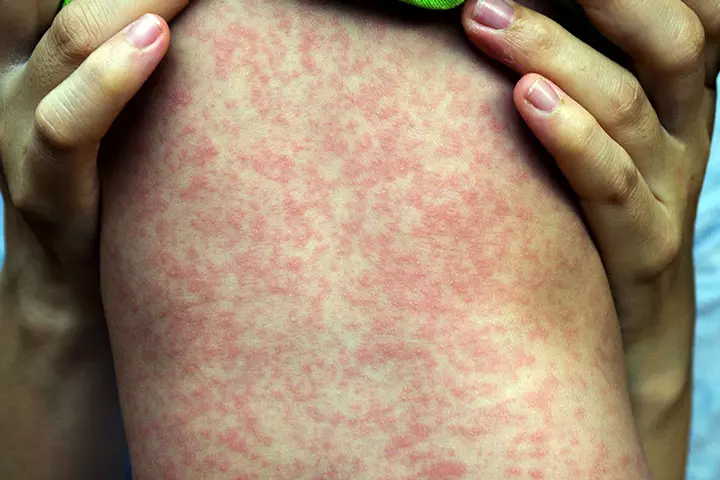
The measles virus spreads through the inhalation of mucus and saliva expelled by an infected person.
Symptoms: Measles rash is bright pink to red and is mostly flat, arranged in clusters. If a group of small rashes breaks at a part of the body, then they are quite likely to merge to eventually spread to other parts of the body (9).
Treatment: You need to wait for the immune system to fight and remove the virus on its own. The illness usually resolves in a couple of weeks with proper rest and home care. If you think your baby has measles, see a doctor immediately.
 Quick tip
Quick tip8. Hand, foot, & mouth disease

This disease is caused by the virus Enterovirus coxsackie, which spreads more often during summer. A baby can get the virus in multiple ways, including skin-to-skin contact with an infected person, inhaling the virus, and consuming contaminated food and water.
Symptoms: Rashes are flat, irregularly-shaped, and pink to reddish. You will notice the rash on the skin around the mouth, on the face, hands, soles of the feet, and the buttocks.
Treatment: The body can get rid of the virus on its own. Itching and irritation can be discouraged with the use of calamine lotion. The baby will start feeling better within a week and the rashes should be gone by the end of two weeks.
9. Molluscum contagiosum
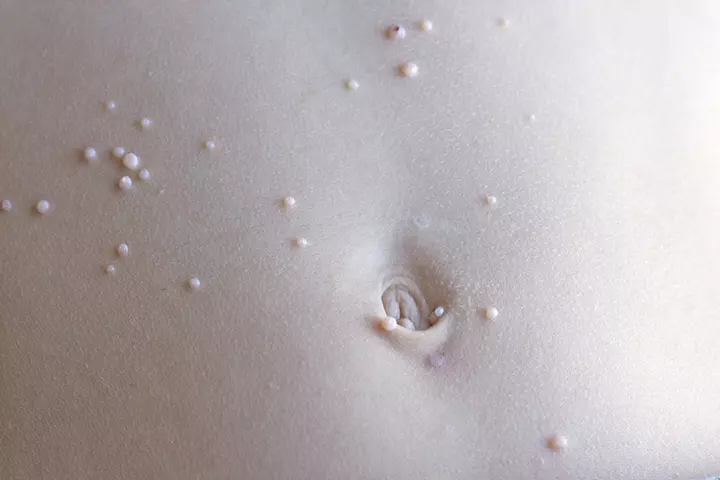
It is caused by the poxvirus (not the same as the Chickenpox virus). A baby contracts the disease through skin-to-skin contact with an infected person.
Symptoms: The tell-tale sign of the condition is the presence of pearl-like, fluid-filled vesicles or blisters on different areas of the body. The density of the rashes varies as per the severity of the infection. The outbreaks tend to be itchy, swollen, and reddish.
Treatment: Oral medication aims at ridding the body of the lesions. These medications and the efforts of the immune system together help overpower the virus and cure the illness. In most cases, the immune system alone will clear the infection within a year. Molluscum contagiosum may take a long time to cure and could persist for a couple of years. Opportunistic infections can be an indicator that a child is depleted. Consider seeing a naturopathic physician to assess nutritional status required to support a healthy immune response.
10. Impetigo
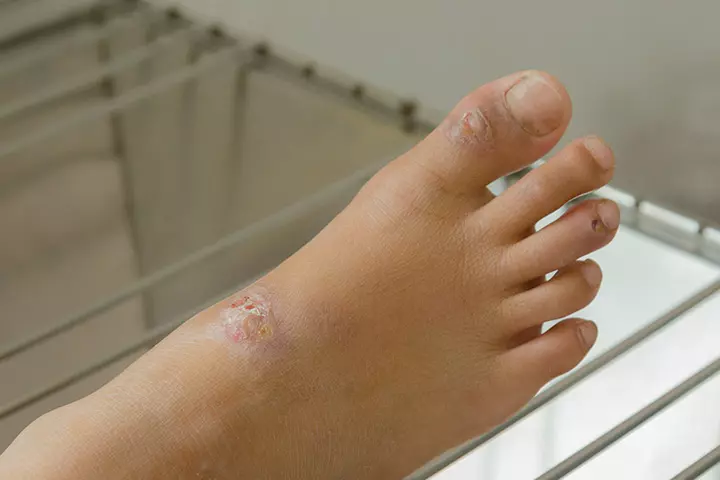
Impetigo is a bacterial infection that causes fluid-filled blisters that burst to form yellowish-red rashes, which eventually dry and fall off. This condition often develops during hot and humid weather. An impetigo rash is most likely to appear around cuts or breaks on the skin, such as an insect bite or an injury.
Symptoms: Impetigo starts with red sores around the mouth and torso. These sores gradually turn into fluid-filled blisters, which burst and dry to form yellowish rash. The rash subsequently dries to form a scab.
Treatment: Topical antibiotic cream and oral antibiotic medicines are necessary to cure the condition. The irritation from the rashes will subside within a few days of commencing the treatment and the disease will be gone in a few weeks.
11. Neonatal and infantile acne
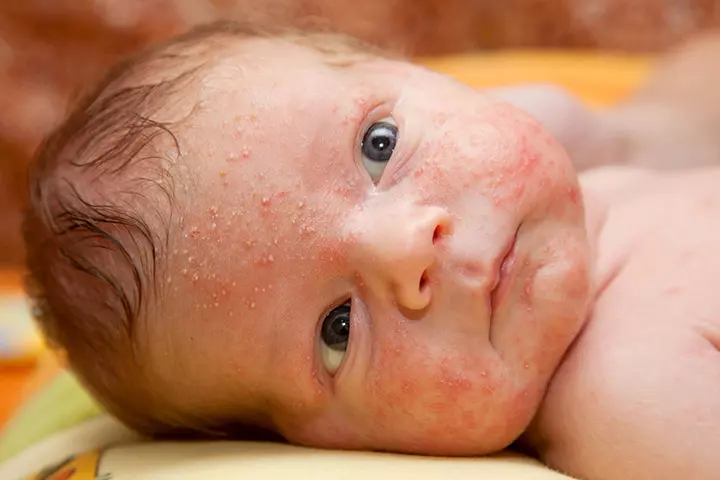
Neonatal acne appears during the first three months of a baby’s life while infantile acne occurs after the age of three months. The causes of this acne are unknown. Overactive sebaceous glands (oil glands), due to maternal hormones transmission through breast milk is suspected to be the leading cause. Sometimes, a bacterial infection of the skin may cause excessive oil production and formation of acne.
Symptoms: The acne looks like a cluster of fine, reddish-pink rashes that mostly appear around the cheeks and the forehead. Infantile acne can be similar to adolescent acne with the presence of pus.
Treatment: Treatment is seldom needed because the acne subsides on its own as the baby grows older. In rare instances, the acne could be irritable and lasts for several years. A doctor can prescribe topical ointments in such cases.
12. Folliculitis
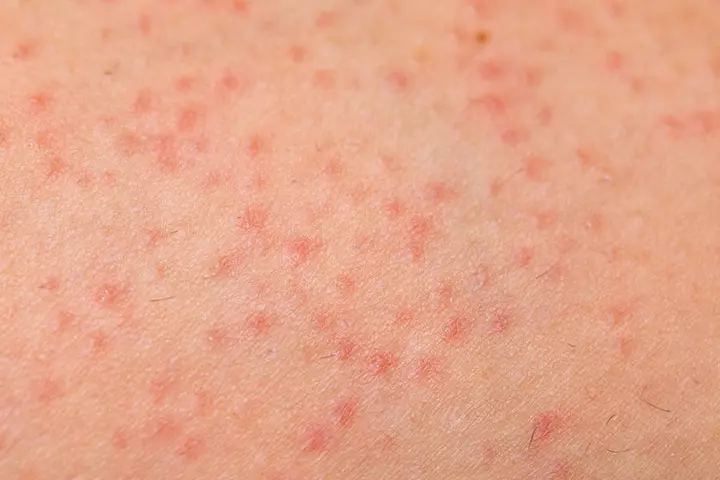
Folliculitis occurs when bacteria from unclean water enter the hair follicles and cause inflammation. A baby can get it when bathed in an unclean bathtub or wearing soiled, wet clothes for too long.
Symptoms: Yellow, pus-filled rashes on any part of the body that could have come in contact with the pathogen.
Treatment: Topical antibiotic and antiseptic ointments are usually sufficient to treat the condition. The condition does not last very long and the rashes will dry and fall eventually.
13. Juvenile plantar dermatosis

It occurs when the feet get sweaty and dry repeatedly, several times during the day. It can happen when you put the baby’s shoes on and off multiple times in a day.
Symptoms: The affected skin becomes pinkish to red with a scaly appearance. The scales develop a white color and begin to peel as the feet get drier.
Treatment: Treatment through the application of moisturizer is usually all that is needed. Preventive care by keeping the feet dry also helps in subsiding the condition (10). If symptoms are very severe, then a doctor can prescribe ointments to subdue inflammation of the skin.
14. Cradle cap
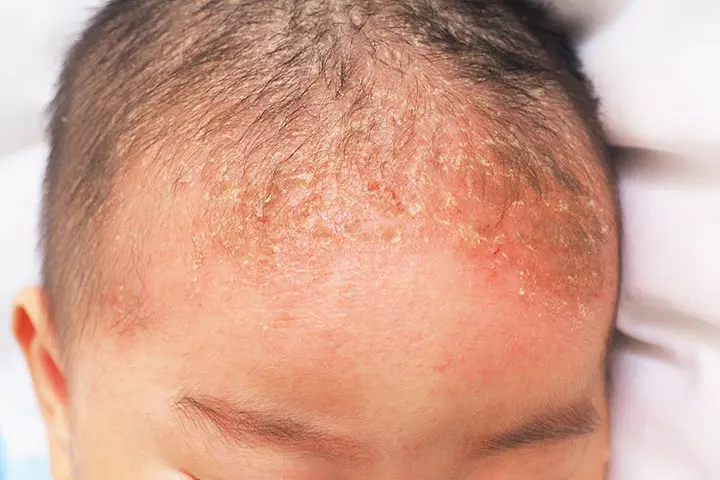
Also called seborrheic dermatitis, CC is a common occurrence in infants up until three months of age, of unknown cause. Red to yellowish scales form on the top of the baby’s head. The scales are easily visible on top of the head. Excessive production of oil by the sebaceous gland quite likely causes cradle cap (11).
 Did you know?
Did you know?Symptoms: Reddish yellow scales form on the top of the head. Rubbing the scales can cause them to flake and fall away from the head. The scales become dry and deep yellow before falling away on their accord.
Treatment: Washing the baby’s hair with a regular baby shampoo every day can help loosen the scales and cure the condition. If there are signs of infection, then the pediatrician can prescribe a medicated shampoo to prevent the likelihood of an infection.
15. Erythema toxicum
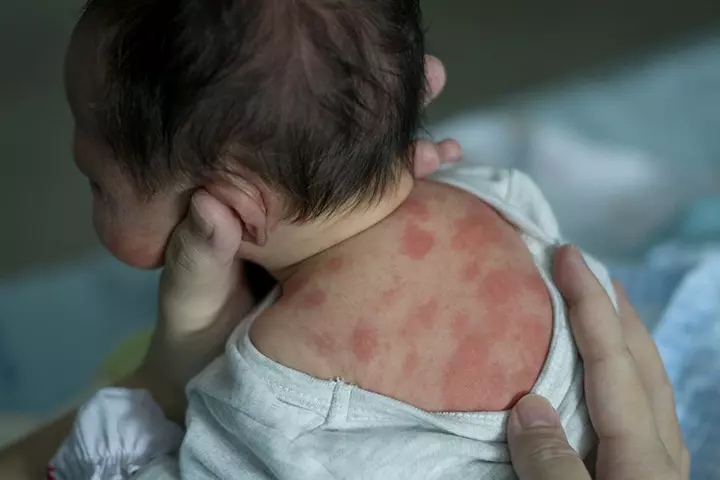
The cause of the condition is unknown, but it is quite likely due to an excessive response of the immune system to the air and substances in the environment. Erythema toxicum in newborns is painless and seldom causes any complications to the baby. The rashes mostly appear within a day after birth and disappear in a week (12).
Symptoms: Yellow-white pustule rashes on the chest, face, torso, and the limbs. The number of rashes peaks on the second day of appearance.
Treatment: Treatment is not needed as the condition is benign and resolves in about seven days with no lasting effect on the baby’s health.
16. Milia

Milia occur due to the retention of the protein named keratin and sebum (oil) from the sebaceous gland within the skin. It is most common among newborns, especially those in their first month.
Symptoms: White bumps that range in size from being fine to large in diameter. The rashes mostly appear on the face, particularly on the nose.
Treatment: No treatment is required and the rashes disappear within a month of their appearance.
17. Dengue
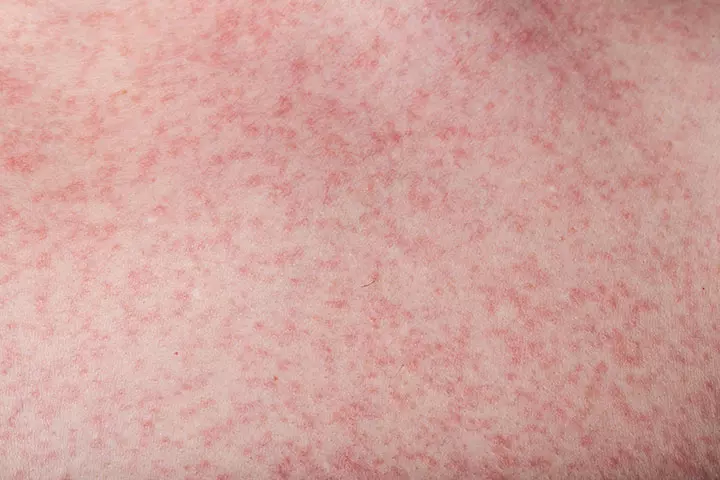
It is caused by the dengue virus that spreads through mosquito bites. The virus does not spread directly from person to person, but is passed by mosquitoes that had earlier bitten someone infected with the dengue virus. The disease is most common in the warm and wet regions in the world (13). The World Health Organization reports that approximately 50% of the global population faces the risk of dengue, with an estimated annual occurrence of 100-400 million infections.
Symptoms: One of the symptoms of the condition is the development of rashes on the body. The rash is reddish-pink and flat.
Treatment: There is no specific medication for the disease. The body clears the virus on its own and supportive care through adequate hydration is vital for the speedy recovery of the baby. Doctors may recommend the use of analgesics, acetaminophen and other drugs containing aspirin for relief from symptoms (14).
18. Fifth disease

The medical term for the fifth disease is erythema infectiosum. The parvovirus B19 causes the condition. The pathogen spreads through the air when an infected person releases them while sneezing and coughing. A newborn baby may also get the virus in case the mother had the infection before delivery (15).
Symptoms: The disease causes a fine rash on the cheeks, making it look like a slapped cheek. The rashes are very fine and appear-disappear for several weeks.
Treatment: One needs to wait for the immune system to clear the virus on its own. The baby can have acetaminophen (paracetamol) in case they have a fever.
19. Scabies
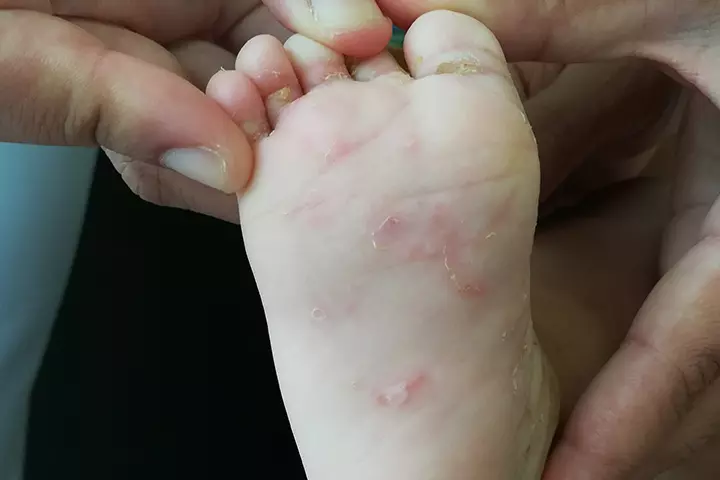
Scientifically called Sarcoptes scabiei, it is a parasitic infection caused by the scabies mite. Babies can get the mite from skin-to-skin contact with an infected person or when they come into contact with bedding contaminated with the scabies mite.
Symptoms: The female scabies mite burrows into the skin to deposit its eggs, causing deep red rash marks at the point of entry. The redness is usually caused by the body’s reaction to the mites, their waste, and their eggs.
Since the mite crawls under the skin, it leaves very fine trails that often connect two rashes. The rashes are itchy and may get inflamed too. The body will also mount an allergic reaction towards the mite thus causing pinkish-red sores all over.
Treatment: Treatment is a combination of creams and ointments containing compounds that kill the mites. The prognosis varies by the intensity of the condition. Typically scabies in babies is cured within four weeks (16).
20. Scarlet fever
It is caused by the A Streptococcus bacteria, which transmits through direct contact or inhalation of infected mucus/saliva of an infected person (17).
Symptoms: The pathogen causes a bright red, flat rash all across the body. The outbreak is severe at the folds of the skin like the underarm, crease of the elbow, and the groin.
Treatment: Oral antibiotics along with topical antibiotics are used to cure the condition.
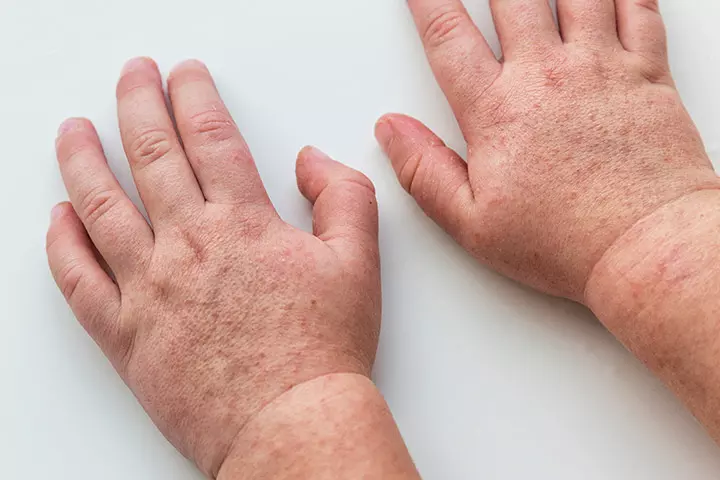
21. Warts
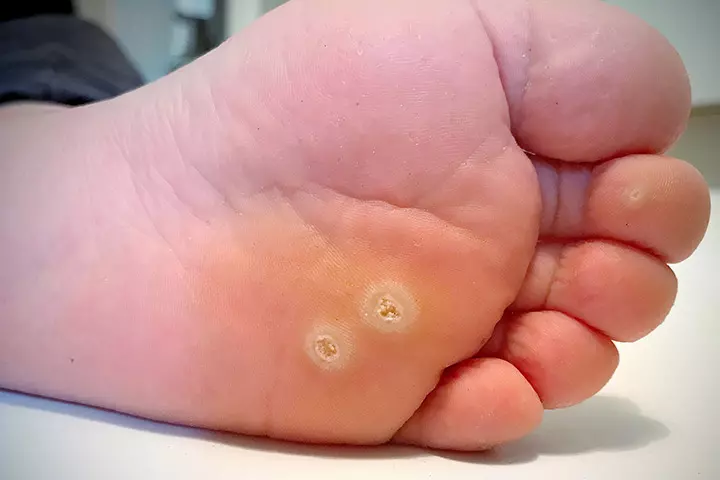
Warts is the thickening of the skin due to the human Papillomavirus (HPV) that enters through cracks and breaks in the skin (18). Warts are benign and do not usually cause any discomfort. A baby can pick the virus through direct contact with a person who has warts, using unclean bedding, and bathing in contaminated swimming pools or bathtubs.
Symptoms: Warts appear as reddish-gray or brownish bumps on any part of the body. They are seldom flat and mostly extend out way beyond the skin surface.
Treatment: Warts in adults are often treated with the use of liquid nitrogen. However, it can be painful for a baby thus the doctor may use topical ointments containing compounds that can gradually disintegrate the wart. The doctor may then manually extract warts for their complete removal (18).
22. Roseola
Roseola, also known as the sixth disease or roseola infantum, is a viral infection caused by human herpesvirus (HHV) types 6 and 7. It mainly affects children aged six months to two years. It spreads through respiratory droplets released when an infected child talks, coughs, or sneezes. It is most contagious in the fever phase, but even asymptomatic carriers can transmit the virus. Once the fever subsides and the rash appears, it is considered safe for the child to return to childcare or preschool (19).
Symptoms: Babies with roseola may exhibit irritability, reduced appetite, sore throat, and swollen lymph nodes during the fever phase. In addition, symptoms such as runny nose, cough, diarrhea, or vomiting may also be present. The fever often concludes abruptly, sometimes triggering febrile seizures in 10–15% of cases. Subsequently, a non-itchy rash emerges on the trunk, spreading to the neck, face, arms, or legs, appearing as pink or red spots on light skin.
Treatment: For roseola, medical treatment is usually not needed. The goal is to provide symptomatic relief by using medicines such as acetaminophen or ibuprofen to ease the symptoms. Keeping the child hydrated is important, so encourage fluids like breast milk, formula, oral rehydration solutions, and water. Avoid lukewarm sponge baths and alcohol rubs. The main focus is on providing comfort and keeping an eye on the child’s well-being (19).
More often than not, these skin rashes can be prevented by reducing the risk of the conditions that cause them.
How To Prevent Skin Rashes In Babies?
Prevention methods help mitigate the reasons that lead to rashes in babies. Here is what you can do to prevent skin rashes in infants:
- Immunize: Conditions like chickenpox and measles can be prevented through immunization. Most vaccines will be a part of the baby’s regular vaccination schedule. You can ask the baby’s doctor about the relevant vaccines.
- Maintain good hygiene: The viruses that cause rashes in babies can be kept at bay by maintaining good hygiene. Wash the baby’s hands after outdoor play and wash your hands before handling the infant. If someone in the family is ill, do not let them hold the baby until they are cured. Wash the baby’s clothes separately and do not allow a sibling to use them.
- Be watchful of allergies: Babies who eat solid food are susceptible to several allergies. Be cautious, especially when feeding a new food item to the baby. Some conditions such as eczema and cradle cap may begin as a minor rash. But they become severe quickly, so it is best to contain them sooner. If you suspect a rash to be a result of allergy or eczema, then consult a doctor right away. Quick intervention reduces the chances of complications.
- Take extra care during hot and humid weather: Hot and humid weather can further several conditions that cause rashes. During the summer months, keep the baby cool and let them stay without diapers for some time every day. It helps keep the skin dry and inhibits the accumulation of sweat.
Home Care Tips For Rashes In Babies
Here are some practical home care tips to help manage and prevent skin rashes in babies.
- Keep the baby’s skin clean and dry: Regularly clean your baby’s skin, especially in areas prone to moisture, to prevent irritation.
- Use fragrance-free products: Choose fragrance-free soaps, lotions, and wipes to reduce the risk of skin irritation.
- Apply a barrier cream: Use a barrier cream to protect against diaper rash and create a shield between your baby’s skin and moisture (30).
When To Seek Help?
Reach out to your child’s healthcare provider if your child
- has a rash that goes beyond the diaper region.
- has blisters.
- shows no improvement after three days of home care.
- has a fever or other unexplained symptoms related to the rash.
- has wet, oozing, or red areas that may signal an infection.
- has a rash that worsens in the skin folds.
- experiences severe itching (31)
Frequently Asked Questions
1. What rashes are common in babies?
Diaper rash is the most common skin problem in babies since urine, feces, and dampness can irritate babies’ skin. You may notice various types of diaper rash in babies who wear diapers (20).
2. What does a food allergy look like in a baby?
Skin rashes may appear after the intake of foods that cause allergies. They may present as hives on some areas of the body. Sometimes, individual tiny bumps can cluster and make a more prominent rash. However, some babies may only develop red and inflamed skin without raised lesions (21).
3. How can I tell if a rash is serious?
Skin rashes associated with a stiff neck, confusion, high fever, and light sensitivity are considered severe and require prompt medical care. Breathing problems and appearing ill are signs of serious underlying causes (22).
4. What are babies most allergic to?
Babies are most allergic to cow’s milk, eggs, and peanuts. Soy, wheat, and tree nut allergies are also common in babies. Peanut, shellfish, and fish allergies may trigger severe allergic reactions in babies (23).
5. What does a viral rash look like on a baby?
Viral rashes are tiny pink spots. They may appear on both sides of the stomach, back, and abdominal area. Viral rashes can be associated with fever, cold symptoms, and diarrhea, often lasting for two to three days (24).
6. How can I treat my baby’s rash naturally?
Homecare measures as per the doctor’s recommendations can help manage some self-resolving skin rashes. For instance, you may use a cold compress to reduce itchy skin and thus soothe the feeling of pruritus. Moisturizing the skin with ointments and creams can also be beneficial. In addition, colloidal oatmeal baths may help reduce the severity of symptoms (25).
Rashes in babies are common and treatable. Although they are generally not concerning and do not threaten the baby’s health, they may cause discomforts such as pain, itchiness, and irritation. Therefore awareness about their cause can help prevent them from occurring and stay prepared with management tips. Do not panic if you notice symptoms of any of the above rashes, and consult your child’s doctor for prompt and effective treatment.
Infographic: Rare Infant Diseases Causing A Typical Rash
Rashes on the skin and body are common and may not always indicate a severe problem in infants. Nevertheless, some rare diseases may manifest as characteristic rashes in babies, some of which are stated in the infographic below. Illustration: Momjunction Design Team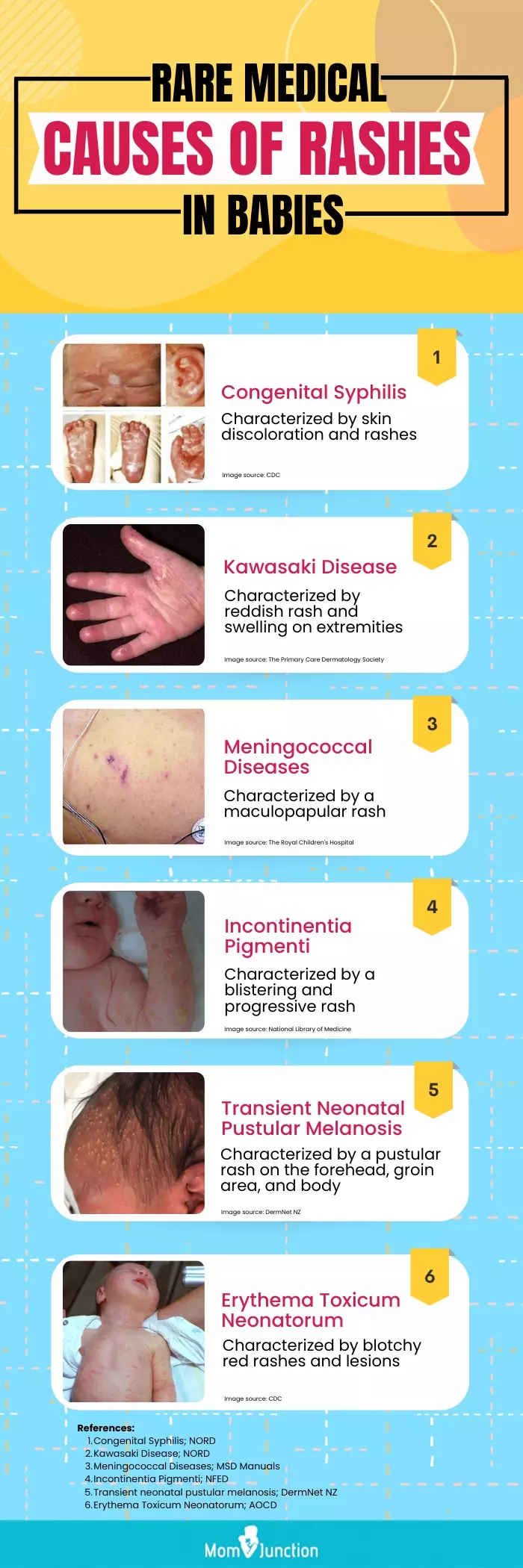
Discover efficient methods for promptly and efficiently addressing skin rashes in children. Acquire valuable advice on optimal approaches and solutions for their well-being.
Personal Experience: Source
MomJunction articles include first-hand experiences to provide you with better insights through real-life narratives. Here are the sources of personal accounts referenced in this article.
i. Fast + natural diaper rash treatment every parent should know;https://www.youtube.com/watch?v=K4Pw6qVsMVU
References
- 12 Common Summertime Skin Rashes in Children; AAP (2017)
https://www.healthychildren.org/English/health-issues/conditions/skin/Pages/Common-Summertime-Skin-Rashes-in-Children.aspx - Neonatal and Infantile Common Skin Lesions; The University of Chicago Pediatrics Clerkship
https://pedclerk.uchicago.edu/ - Newborn Rashes and Skin Conditions; Michigan Medicine (2017)
https://www.mottchildren.org/health-library/zx1747 - Hives; Children’s Hospital Of Philadelphia (2003)
https://www.chop.edu/conditions-diseases/hives - Urticaria; The University of Chicago Pediatrics Clerkship
https://pedclerk.uchicago.edu/ - Urticaria Papular; National Organization for Rare Disorders (Last updated in 2006)
https://rarediseases.org/rare-diseases/urticaria-papular/ - Contact Dermatitis; The University of Chicago Pediatrics Clerkship
https://pedclerk.uchicago.edu/ - Chickenpox; NHS Inform (2018)
https://www.nhsinform.scot/illnesses-and-conditions/infections-and-poisoning/chickenpox - Measles Symptoms and Complications; CDC (2026)
https://www.cdc.gov/measles/signs-symptoms/?CDC_AAref_Val=https://www.cdc.gov/measles/symptoms/signs-symptoms.html - Juvenile Plantar Dermatosis; AOCD
https://www.aocd.org/page/JuvenilePlantarDerm - Cradle Cap; AAP (2009)
https://www.healthychildren.org/English/ages-stages/baby/bathing-skin-care/Pages/Cradle-Cap.aspx - E. Roques; M. D. Mendez; Erythema Toxicum; StatPearls Publishing (2017)
https://www.ncbi.nlm.nih.gov/books/NBK470222/ - Dengue; Medline Plus
https://medlineplus.gov/dengue.html - Clinical Care of Dengue; CDC
https://www.cdc.gov/dengue/hcp/clinical-care/index.html - Fifth Disease (Parvovirus B19); AAP (2006)
https://www.healthychildren.org/English/health-issues/conditions/skin/Pages/Fifth-Disease-Parvovirus-B19.aspx - Scabies; American Academy of Dermatology (AAD)
https://www.aad.org/diseases/a-z/scabies-treatment#treatment - About Scarlet Fever; CDC
https://www.cdc.gov/group-a-strep/about/scarlet-fever.html?CDC_AAref_Val=https://www.cdc.gov/groupastrep/diseases-public/scarlet-fever.html - Warts; University Of Michigan
https://uhs.umich.edu/warts - Roseola; Nemours KidsHealth
https://kidshealth.org/en/parents/roseola.html#:~:text=Roseola%20(roe%2Dzee%2DOH,just%20as%20the%20fever%20breaks. - Rash – child under 2 years.
https://medlineplus.gov/ency/article/003259.htm - Does My Baby Have a Food Allergy Rash?.
https://www.preventallergies.org/blog/baby-food-allergy-rash - Rashes in babies and children.
https://www.nhs.uk/conditions/rashes-babies-and-children/ - Food Allergies in Children.
https://www.hopkinsmedicine.org/health/conditions-and-diseases/food-allergies-in-children - Rash or Redness – Widespread.
https://www.seattlechildrens.org/conditions/a-z/rash-or-redness-widespread/#:~:text=Viral%20rashes%20usually%20have%20small - Home Remedies: What Can Relieve Itchy Eczema?.
https://www.aad.org/public/diseases/eczema/childhood/itch-relief/home-remedies - Zekayi KUTLUBAY et al.; Newborn Skin: Common Skin Problems; Maedica (2017)
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5574071/ - National Collaborating Centre for Women’s and Children’s Health (UK); Atopic Eczema in Children: Management of Atopic Eczema in Children from Birth up to the Age of 12 Years; RCOG Press (2007)
https://pubmed.ncbi.nlm.nih.gov/21204322/ - Measles in babies and children; Pregnancy Birth and Baby’s information
https://www.pregnancybirthbaby.org.au/measles-in-babies-and-children - Timothy Nobles et al.; Cradle Cap; StatPearls Publishing (2026)
https://www.ncbi.nlm.nih.gov/books/NBK531463/ - Diapers and Diaper Rash.
https://www.nationwidechildrens.org/conditions/health-library/diapers-and-diaper-rash - Rash – child under 2 years
https://www.mountsinai.org/health-library/symptoms/rash-child-under-2-years
Community Experiences
Join the conversation and become a part of our nurturing community! Share your stories, experiences, and insights to connect with fellow parents.
Read full bio of Rebecca Hughes
Read full bio of Rohit Garoo
Read full bio of Dr. Ritika Shah
Read full bio of Anindita Ghatak

















