Image: iStock
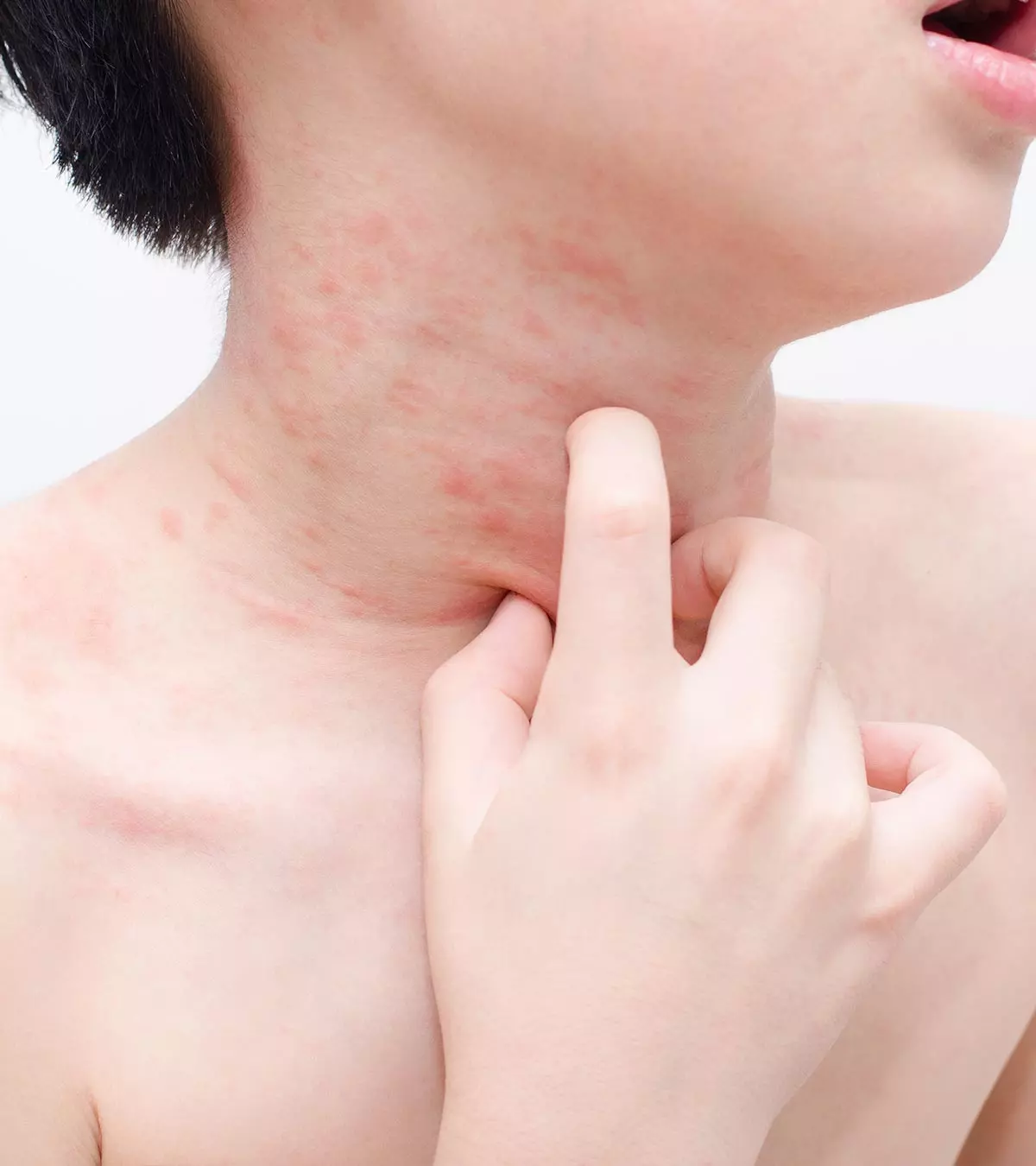
Skin rashes in children are not uncommon and may occur due to an infection or autoimmune diseaseiA group of medical conditions where the body’s immune system mistakenly attacks the healthy body cells . They may also be triggered by an allergic reaction. Your pediatrician may help you diagnose the exact cause of your child’s skin rash. A prompt and accurate diagnosis enables timely treatment and helps prevent complications. It is suggested to seek the pediatrician’s suggestion instead of trying any over-the-counter (OTC) drugs or home remedies for your child. Read this post to know more about the causes and management of this condition in children.
Key Pointers
- Skin rashes are a common problem in children and can have various causes, such as infections, allergies, autoimmune disorders, etc.
- Symptoms of skin rashes in children can include redness, itching, blistering, and skin scaling.
- Some common skin rashes in children include eczema, chickenpox, and impetigo.
- Using water and soap for washing the body can help prevent the spread of skin infections.
- If the rash is severe or accompanied by other symptoms, it is essential to consult a doctor for proper evaluation and treatment.
When Should You Take Your Child To The Doctor For A Rash?
Skin rashes could be common in children, but if your child is showing the signs that we mention next, then you need to consult your child’s doctor.
- The rashes are interfering with the child’s day-to-day activities.
- The child has difficulty in sleeping, or the rashes are causing pain.
- The rashes have not subsided or did not decrease after two days.
- Your child has a fever.
- The rashes have developed after your child has consumed a new food or a medication.
- The rashes appear like bruises.
Should you find any or more of these symptoms, take the child to a doctor soon.
A child could develop a rash due to viral, bacterial, or other infections. Next, we list down the causes and symptoms of various rashes in children.
Rashes Caused By A Virus
- Chickenpox
- Measles
- Rubella
- Slapped cheek disease
- Hand, foot, and mouth disease
- Molluscum contagiosum
1. Chickenpox
Chickenpox is a highly contagious viral disease caused by the varicella-zoster virus.
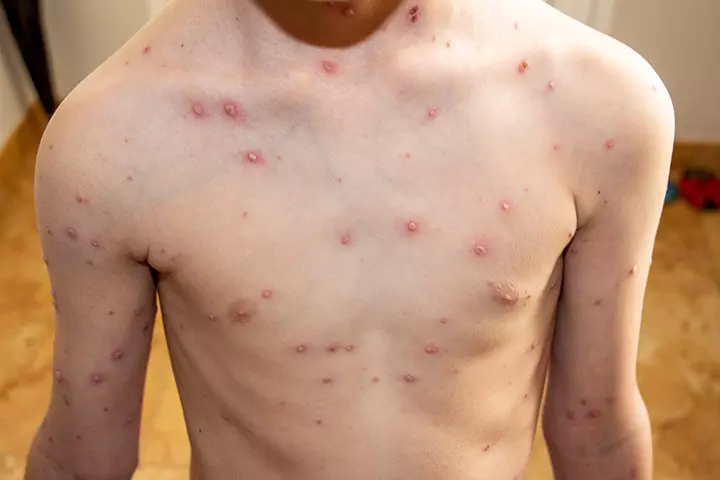
Symptoms:
- The main signs of chickenpox are rashes, headache, fever for two to three days, followed by a vesicular rash, and loss of appetite.
- The rashes are itchy and form blisters filled with fluid. They blister and scab over after another five to six days after the onset of rash.
- They can appear anywhere on the body, even inside the mouth and around the genitals (1).
Treatment:
Although there is no specific treatment for chickenpox, you can follow some tips to relieve the symptoms.
Calamine lotion and a cool bath in water mixed with baking soda and uncooked oatmeal may help relieve the itching. Discourage your child from itching as it may spread to others and may also cause potential bacterial infection.
Your doctor might prescribe over-the-counter medications to relieve fever. Make your child drink plenty of fluids to keep the body hydrated (1).
Prevention: According to the CDC, two doses of chickenpox vaccine is recommended as a preventive. For children under the age of 13, the first dose should be given at 12 to 15 months and the second dose between four and six years. Children above 13 years, who have not received any chickenpox vaccine earlier, should be given two doses 28 days apart (2). The CDC also notes that the chickenpox vaccination program has effectively decreased its prevalence, with annual reported cases below 150,000. This success underscores the vaccine’s efficacy and highlights the importance of following the vaccination schedule.
 Quick fact
Quick fact2. Measles
Measles is an infectious viral respiratory disease, it could be dangerous in babies and young children, if you find any of the below symptoms in your child, then make an appointment with your pediatrician.
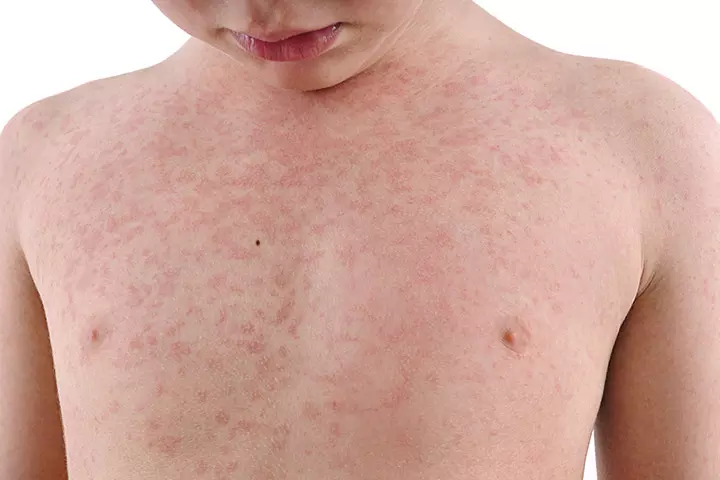
Symptoms: It could spread via droplets from the nose, mouth, or throat of an infected person, the initial symptoms which will appear 10-12 days after the infection include.
- High fever
- Runny nose
- bloodshot eyes
- Two to three days after the above symptoms, tiny white spots are formed on the inside of the mouth
- Three to five days later, a rash develops which starts on the face and upper neck and gradually spreads downwards (3)
Treatment:
Usually, no medicines are prescribed for measles, and the symptoms typically go away within seven to ten days. However, your doctor might ask to keep your child away from school for at least four days from when the rash appears. Your child’s doctor may prescribe acetaminophen to relieve the fever and aches and suggest vitamin supplements as well (4).
Prevention: You can prevent measles by giving the MMR (measles, mumps, rubella) vaccine to your child. One dose of this vaccine is given to children when they are 12 to 13 months old, and a second dose is given at three years and four months (4).
3. Rubella or German measles
Rubella is a contagious viral disease in children. It is also known as three-day measles and German measles.

Symptoms: A red rash on the face, which later spreads to the rest of the body, is one of the first signs of German or Rubella in children. Other symptoms that may occur one to five days before the rash appears are:
- A low-grade fever
- Headache
- Mild pink eye
- General discomfort
- Swollen and enlarged lymph nodes
- Cough
- Runny nose (5)
Treatment:
Treatment cannot prevent rubella from living its course. So, the therapy tries to relieve the symptoms effectively. Doctors advise rest and prescribe acetaminophen to reduce fever and aches (5).
Prevention: Rubella can be successfully prevented by the MMR vaccine. The CDC recommends one dose between 12- 15 months of age and the second dose between four to six years of age (6). There is another vaccine known as MMRV vaccine (measles, mumps, rubella and varicella), but it is licensed for use in children aged 12 months to 12 years (5).
4. Slapped cheek disease
Slapped cheek disease or the fifth disease in kids is a viral infection common in children during early summer, winter, and spring.

Symptoms: The first sign is usually not feeling well for a few days. Some of the symptoms might include.
- A high temperature of 100℉ or more
- Runny nose, sore throat and headache
- The bright red rashes begin on the cheeks and spread to the torso, arms, and legs in a few days, which will go away within two weeks (7).
Treatment:
This condition runs its course; you may do the following to help your child ease the symptoms.
- Let the child rest and have plenty of fluids
- Your child’s doctor might prescribe paracetamol for high temperatures and headache
- You can also apply moisturizer for itchy skin
Prevention:
As this is an airborne virus, maintaining proper hygiene can help in preventing it to an extent. To reduce the spread of infection:
- Instruct your child to wash their hands with warm water and soap frequently
- Use a tissue to cover your child’s mouth while sneezing and coughing (7)
5. Hand, foot, and mouth disease
Hand, foot, and mouth disease (also known as HFMD) is a contagious viral infection usually affecting children younger than five years of age. It mostly occurs during summer and fall.
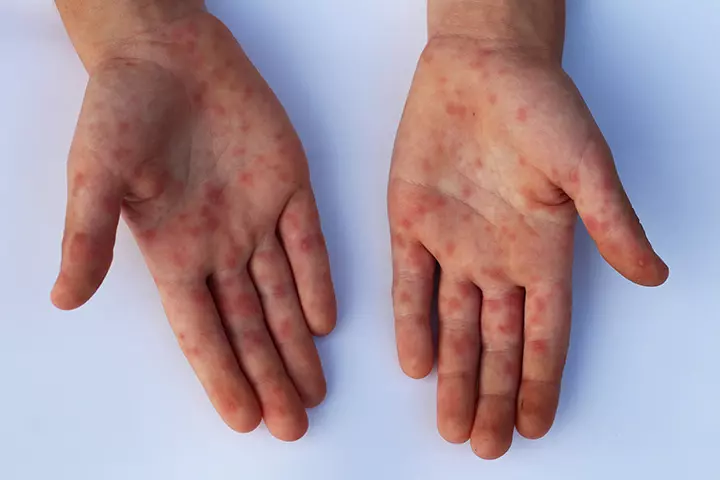
Symptoms:
- Multiple ulcers in the mouth and throat, and a rash on the hands and feet.
- It is generally mild and goes away on its own in a few days.
- Besides mild fever, your child may have painful red sores inside the mouth, affecting the roof of the mouth, gums, and inner walls. They are also likely to have red rashes on the palms, soles, and buttocks.
- Usually, it runs its course, and the affected child recovers without any complications.
Treatment:
There is no specific treatment to cure this disease. It usually gets better within 7 to 10 days. However, you can do the following to help your child recover
- Make your child drink plenty of fluids to avoid dehydration; avoid acidic drinks
- Give mild and soft foods, and keep them away from eating hot and spicy foods
- Consult your doctor if you could give paracetamol or ibuprofen to ease the fever (8).
Prevention:
The best means to prevent this illness from spreading is by practicing good hygiene. Make sure that your children wash their hands with soap and water thoroughly. Also, do not share your child’s bed and towels; wash their bedclothes, towels, and clothes in hot water (8).
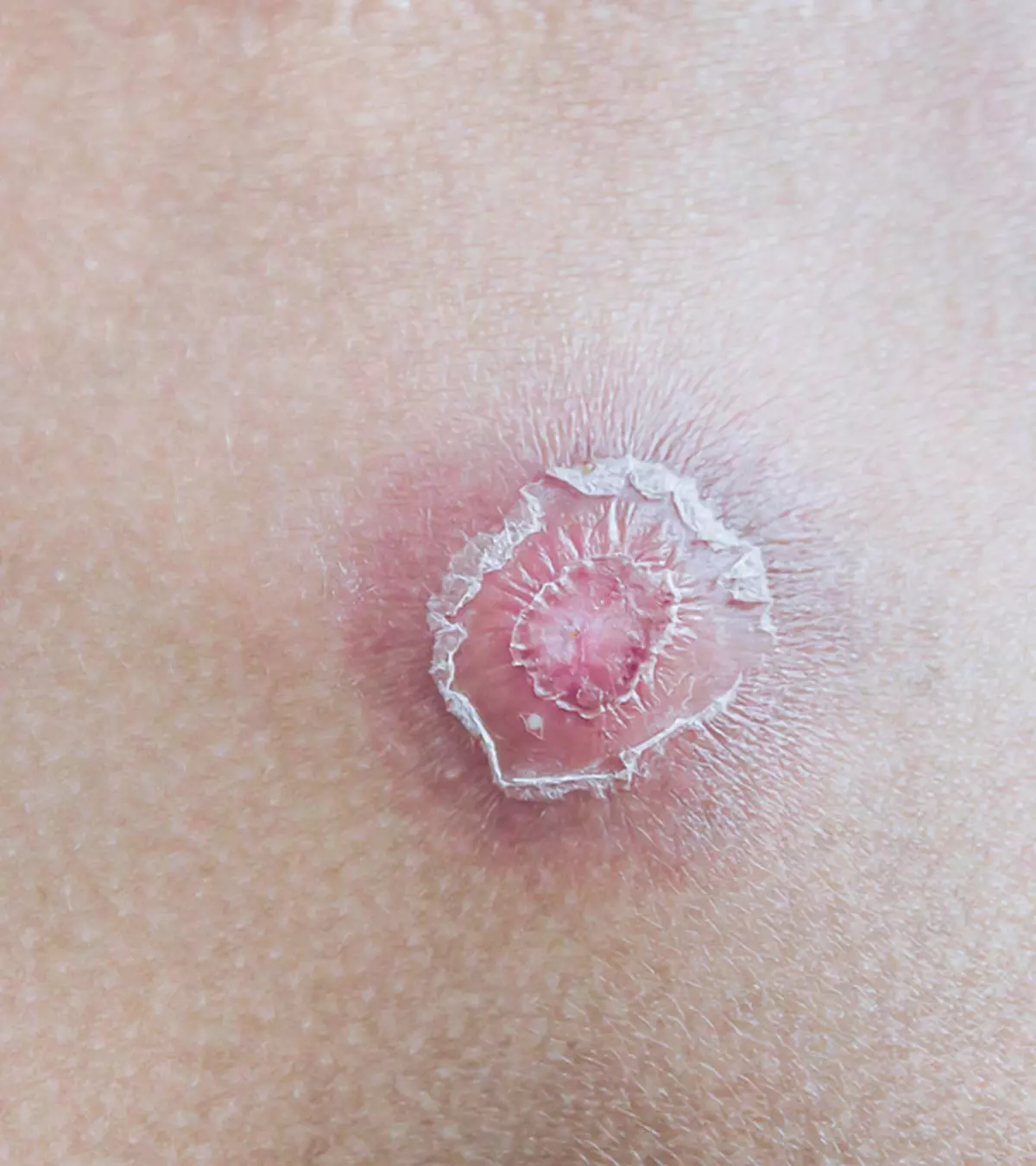
6. Molluscum contagiosum
Molluscum contagiosum is a viral skin infection.
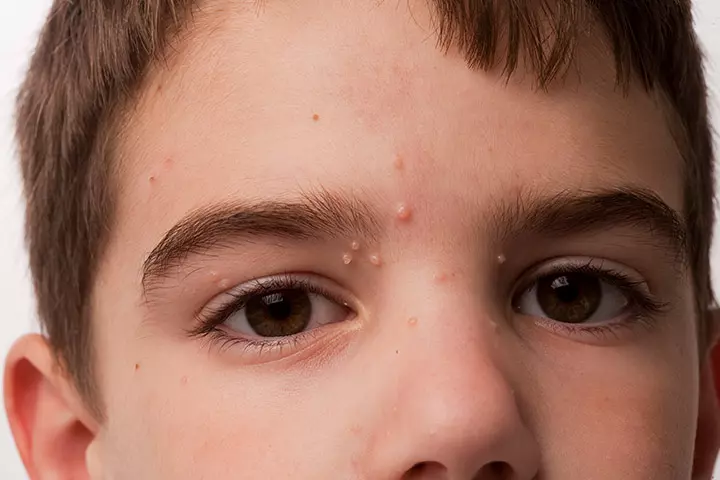
Symptoms:
- It causes small, painless raised lesions on the skin.
- They are commonly smooth and shiny pink or white in color, with a dent in between.
- The rashes mostly appear on the face, torso, thighs, abdomen, and genitals.
- The rashes may last from six months to four years. In most cases, treatment is not required (9).
Treatment:
Normally, the lesions caused by molluscum contagiosum do not require treatment. But in some extreme situations, the doctor may suggest topical creams and ointments.
In very rare cases, the doctor may recommend treatments like topical therapy, laser therapy, and cryotherapyiA treatment intervention that involves the use of frigid temperatures to freeze and destroy abnormal tissues . These treatments cure each lesion separately and may need a couple of sessions to finish (10).
Prevention: It spreads through skin contact, and therefore practicing good hygiene helps. Also, control the spread of rashes by keeping them covered to avoid direct contact, not scratching them, and not sharing personal items (10). Read more on this infection here.
Rashes Caused By Bacteria
- Scarlet fever
- Impetigo
Some diseases caused by bacteria also come with skin rashes or lesions. Here are the most common ones.
7. Scarlet fever
Scarlet fever is strep throat (bacterial infection causing a scratchy sore throat) with an accompanying rash. It usually affects children in the age group of five to 15 years and is unusual for children under two years.
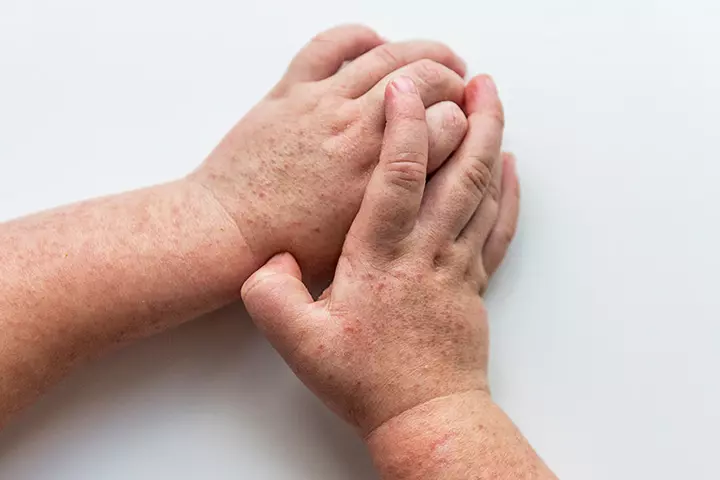
Symptoms:
- It is caused by ‘type A’ Streptococcal bacteria that also cause strep throat.
- Also known as scarlatina, scarlet fever comes with a characteristic red rash, along with high fever and sore throat.
- The most common symptoms are a red rash that appears all over the face, neck, torso, arms, and legs. Sometimes, the rashes leave a white, clear area around the mouth.
- Red streaks or scars appear around the creases like armpits, elbows, knees, groin, and neck. This condition is known as Pastia’s lines.
- The tonsils and the back of the throat may appear red, swollen, and marked by several rashes with little white specks of pus.
Treatment:
It was once a severe and fatal disease in children but is now treatable with antibiotics. Besides antibiotics, your child’s doctor may also prescribe topical ointments for rashes or medicines to ease a sore throat.
Scarlet fever might last for a week, and the child will be infectious up to seven days after the appearance of the first symptom, and until 24 hours after they take the first antibiotic.
Prevention: The bacteria are contagious and spread quickly. If a child contracts the disease, keep him or her at home, as their cough and sneeze can infect others.
If somebody in the family has the infection, prevent your child from having skin contact with the patient. Wash hands thoroughly, and keep utensils, cups, and belongings of an infected person separate (11) (12).
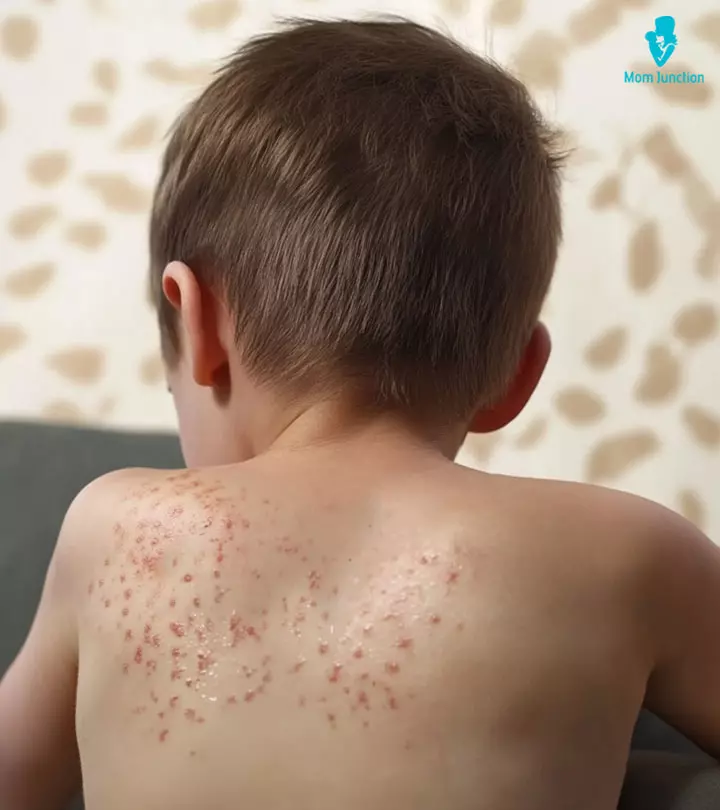
8. Impetigo
Impetigo is a bacterial infection common in children but is not a serious one. It mostly occurs during hot and humid weather and is highly contagious.
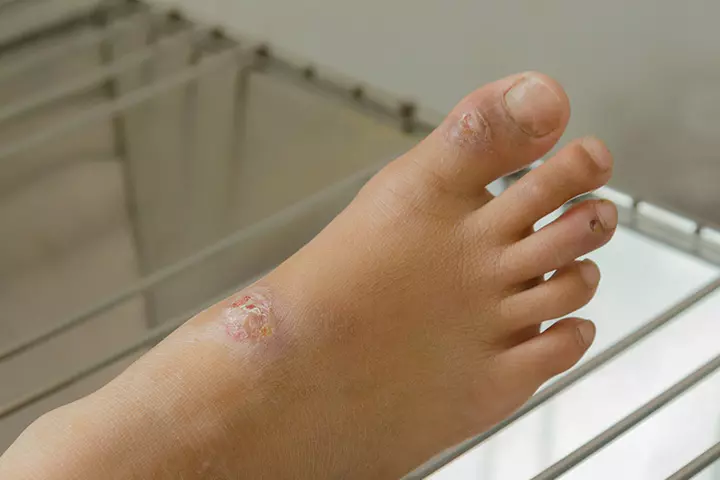
Symptoms:
- Bright red spots, appearing in clusters around the nose and the lips.
- The sores form fluid-filled blisters that may ooze and then crust over.
- The sores are itchy and sometimes painful. After crusting, it may leave red marks on the skin (12).
Treatment:
Doctors usually give antibiotics to heal the rashes. With the treatment, your child will recover in a week’s time.
You may clean your child’s impetigo sores with clean, warm water and soap, and use topical antibiotic ointments to relieve the sores. Topical antibiotics can cure impetigo in seven days.
This disease stops being contagious after 48 hours of starting the medications, if your child is not under treatment, then when the patches start to dry out and crust over (13).
Prevention: Maintaining good hygiene is the best way to prevent impetigo. Give baths regularly, wash their hands, cover any skin wounds, cut the nails, and disinfect the rooms and objects (13). You can find more information about it here.
Other Rashes
Sometimes rashes may be caused by heat, allergic reaction, or other infections.
- Eczema
- Prickly heat rash
- Erythema multiforme
- Psoriasis
- Scabies
- Hives
- Tinea corporis
9. Eczema
Eczema is another name for Allergic Contact Dermatitis and is an inflammatory skin condition.
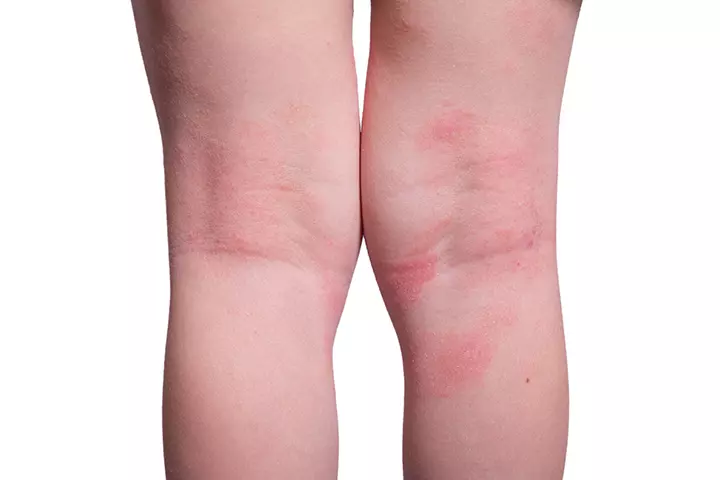
Symptoms:
- The exact cause of eczema is not known, but sometimes the combined factors of genes and environmental factors can trigger eczema.
- The skin becomes dry, cracked, red, and itchy.
- The most common type of eczema is atopic dermatitisiA skin condition characterized by redness, swelling, and the appearance of scaly, itchy rashes , which commonly affects children.
- The rashes usually appear behind the creases of the knees and elbows. They may also appear on the wrists, ankles, legs, and neck.
- The rashes are red, bumpy, and very itchy. But they are non-contagious.
- Eczema usually goes away as the child gets older, but some may continue to have it even in their adulthood (14).
A mom and blogger who goes by the name ‘Bionicwoman’ experienced eczema during childhood. Recounting her ordeal, she says, “I remember one scorching German summer day at the age of three (it’s crazy, but I do remember this distinctly) ripping off my Pampers and pulling myself up onto the cool stone top of our living room’s coffee table, viciously digging my nails into the skin that has been insanely itchy through a combination of active eczema and a hot, moist environment. That sweet relief of answering the itch was short-lived, however, and instantly replaced by burning, screaming, inflamed pain (i).”
Treatment: There is no cure for eczema, and the treatment aims to recover the skin and prevent any flare-ups by using topical medications. Doctors commonly prescribe biologic drugs and immunosuppressants.
Prevention: Recognize and avoid aggravating factors like some foods, dust mites or pollen, chemicals, detergents, smoke, and certain fabrics that can aggravate the rash. Hydrate your child’s skin with a moisturizer and prevent him/her from scratching. Keep a humidifier in the room, especially during the winter when the weather is dry.
The American Academy of Allergy Asthma and Immunology (AAAAI) recommends wet-wrap therapy for severe and unmanageable eczema, in which the skin is soaked in warm water for about 15-20 minutes and then patted dry. Then topical medication is applied on the rashes, and a wet towel is placed on the rash areas, followed by the dry wrapping with a soft and smooth cloth, such as pajamas or socks over the wet gauze or towel. This method should be followed under the guidance of your child’s doctor (15).
 Research finds
Research finds10. Prickly heat rash
Prickly heat rashes in children, also known as miliaria, happens when the sweat ducts of the epidermis or the outer layer of the skin become clogged. This does not spread from one person to another.
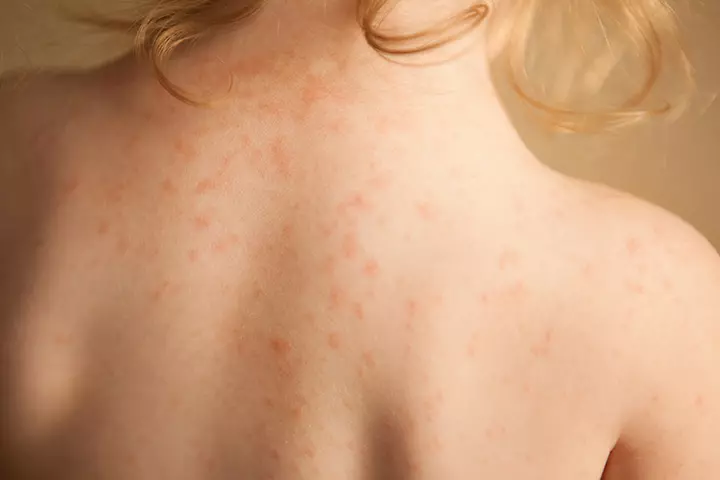
Symptoms:
- Small red spots that appear anywhere on the body and spread
- These spots are itchy and prickly to feel
- Redness and mild swelling (16)
Treatment:
It is not a serious condition and does not require any specific treatment. Apply heat rash lotions like calamine lotions, or over-the-counter topical steroids such as hydrocortisone cream.
Prevention: Keep your child in a cool, dry atmosphere and prevent overdressing in a hot climate. Know more on heat rash here.
 Quick tip
Quick tip11. Erythema multiforme
This is not a disease, but a reaction to some infection (bacterial, fungal, or viral), which makes the body’s immune system destroy its skin cells. It can happen as a reaction to medicine too.
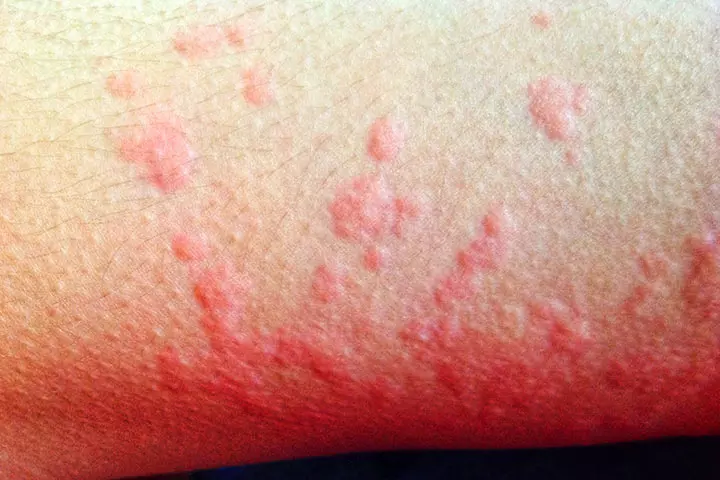
Symptoms:
- Erythema multiforme comes with target-shaped, ring-like red sores.
- The rashes begin like pink blotches and then turn red and form rings. They may also form blisters or scabs.
- They may appear on the face, neck, torso, arms, and legs too. And in some severe cases, the rashes appear inside the mouth.
- If you are not able to identify the rashes, then it is best to seek a doctor’s advice.
Treatment:
There is no treatment as the mild infection goes away on its own. However, cold compresses and paracetamol can be used to relieve symptoms like sore rashes and fever (17). The rash usually goes away in one to two weeks or can last as long as four weeks too.
Prevention: Erythema is not contagious. Environmental factors (pollen, smoke) and foods like dairy can trigger the rashes. Know your child’s triggers and prevent exposure to them.
12. Psoriasis
Psoriasis is a common skin infection that is long-lasting. However, it can get better or worse, almost randomly. It may suddenly disappear and reappear.
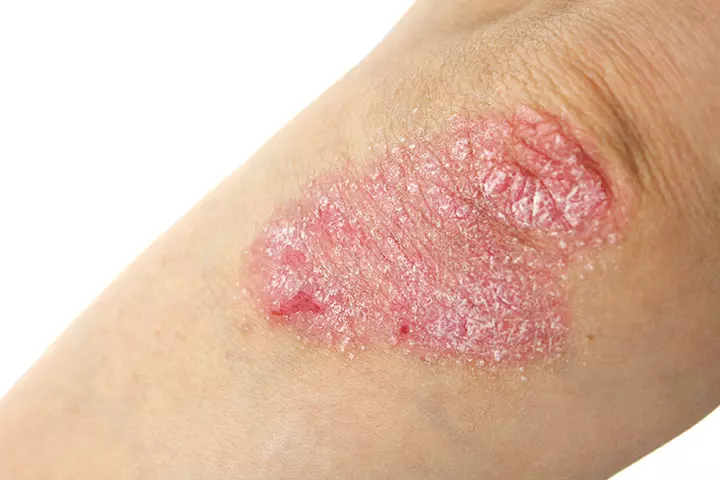
Symptoms:
- This condition causes skin cells to accumulate on the skin’s surface. They form thick whitish scales and raised bumps (known as plaques).
- The plaques are red and itchy. These bumpy rashes appear all over the body – scalp, torso, legs, elbows, and knees.
- Psoriasis is genetic. Research says that children of parents, who have psoriasis, have chances of getting it.
- Psoriasis is non-contagious. But its severity varies. For some, it will be a mild distraction, while for some others, it can adversely affect their quality of life. Plaques may cover large areas on the face or body, and the children may feel uncomfortable.
- Common symptoms are dry and cracked skin that bleeds, and itching and burning sensation around the flaky and affected areas (18).
Treatment:
There is no cure for psoriasis, but medications like topical ointments and creams can be used for the rashes. Sometimes, doctors can come up with combined therapies to effectively relieve the symptoms (19).
Prevention: There is no way to prevent psoriasis (20). You can avoid flare-ups by using moisturizing lotions to prevent the skin from getting dry, topical treatment shampoos for the scalp, a humidifier to keep the atmosphere moist, and avoid freezing, dry weather.
13. Scabies
Scabies is a skin infestation by mites that burrow in the skin.
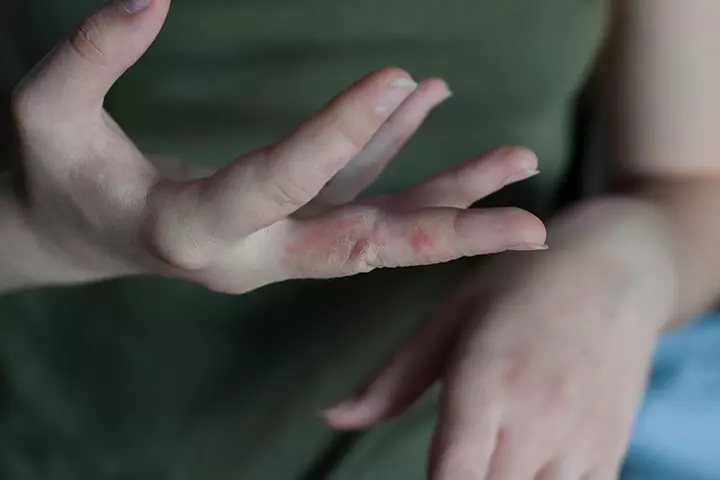
Symptoms:
- They burrow the skin and lay eggs, which could trigger the body’s immune system causing small red bumpy rashes and blisters. The bumps are often filled with pus.
- The rashes are itchy, and the skin may become thick and scaly.
- The areas most affected by scabies are the hands, in between the fingers and toes, the inner sides of the wrist, underarm folds, elbows, and buttocks.
Treatment:
Scabies infection needs medical treatment. Take your child for a diagnosis if such symptoms show up. Doctors usually give medicated ointments or creams to kill the mite. They may also prescribe antihistamines for relieving itching. After the treatment begins, the itching stops in about two days’ time.
Prevention: It is highly contagious and can spread by contact. Therefore, if one person in the house is affected, the whole family should be treated (21).
14. Hives
Hives can happen as an allergic reaction to a drug, for example, a penicillin rash, or to foods, which usually resolve within a few hours.
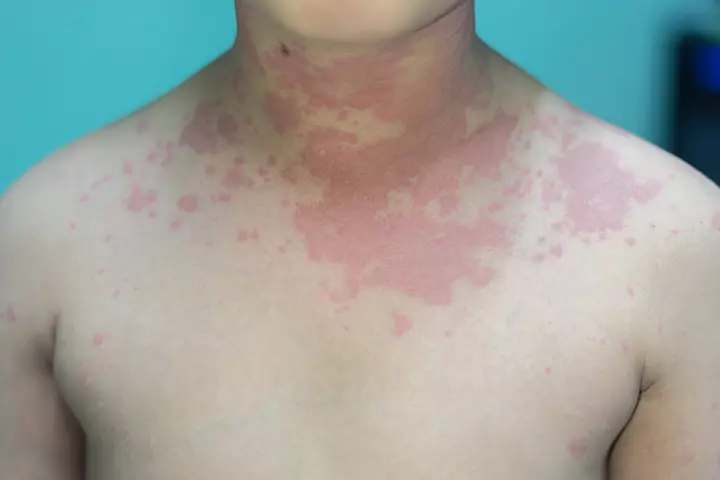
- Hives are raised pink spots or bumps affecting the skin. It is also known as urticaria.
- The most common reason for hives is a viral infection with symptoms like cough, fever, and diarrhea. Sometimes, it can also happen due to bacterial infections like UTI.
- The rashes are very itchy and may look like small insect bites.
- Sometimes, hives may appear all over after a bee sting, or as an anaphylactic reaction, which involves the sudden onset of widespread hives as a severe reaction to some allergic food within two hours of consumption.
- The rashes usually remain for three to four days. Children do not usually get hives more than once (22).
Treatment:
The treatment focuses on relieving the symptoms. Doctors usually recommend topical medicines like corticosteroid tablets and antihistamines. Give your child a cold shower to ease the itching, rub ice cubes on itchy spots.
Prevention: Washing the hands and body with water and soap can help avoid hives. Also, avoiding things that can trigger the reaction can also help prevent hives in children.
15. Tinea corporis
Tinea corporis, commonly known as ringworm, is a fungal infection that is not caused by a worm but by various dermatophyte fungi (23).
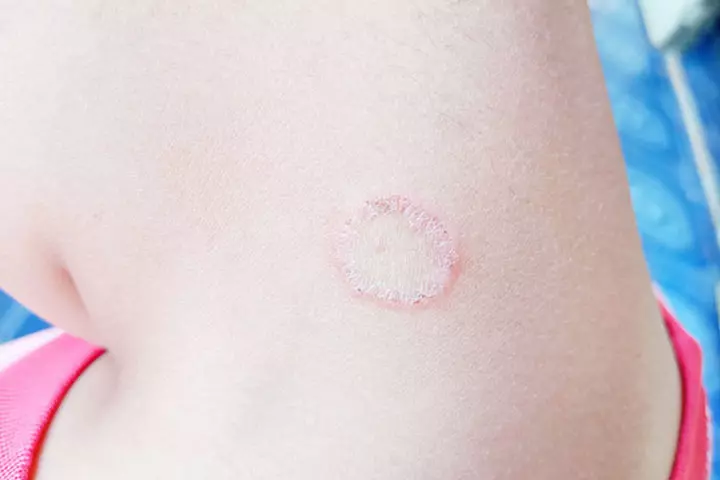
Symptoms:
- The infection appears on the skin as a rash consisting of small red pimples. The rashes may not be generalized and can occur anywhere on the body.
- Gradually, the pimples slowly spread and coalesce, forming a distinctive circular or oval ring that is about a half to one inch in diameter.
- The edges of the ring may remain red, raised, or exhibit scaliness. Within the ring, the skin may appear pink or nearly normal.
- Affected children often experience itching, which can be moderate to severe. Scratching the rash can lead to further spread of the infection.
Treatment:
For only one or a few patches of the infection, topical antifungal creams are commonly prescribed. Oral antifungal medications may be necessary in more severe cases or when the infection is widespread. It is essential to complete the entire course of treatment, even if symptoms improve before the medication is finished, to prevent the infection from recurring. The rashes typically take four weeks to go. However, children can resume school after they begin the treatment.
Prevention: Keeping the body clean and dry, wearing fresh and clean clothes and socks, and wearing shoes or flip-flops in locker rooms and public shower areas can help prevent contracting the infection. Encouraging regular handwashing, avoiding close skin-to-skin contact with infected individuals, and discouraging sharing personal items like towels and clothing can help reduce the risk of transmission. In addition, ensuring that children wear breathable clothing and promoting good overall hygiene practices can prevent the onset of tinea corporis (24).
What To Do If Your Child Develops Skin Rashes?
Here are a few things you can do immediately after noticing the rashes on your child’s skin, before taking them to the doctor. Maintaining a journal of your child’s symptoms, along with their dates and severity, can help create a thorough medical history for your doctor. Check with the doctor and continue these home care practices alongside the medications prescribed. Note that these tips may only alleviate the suffering caused by the rash (15):
- Use mild soap and take care not to scrub – consult your child’s doctor on this.
- Cut your child’s nails short or cover them with gloves to avoid them from scratching the rash.
- Wash their clothes with a disinfectant and sun-dry them.
- If your child’s rashes have pus oozing, then wipe it gently with a damp cloth.
Frequently Asked Questions
1. How long do viral rashes last?
Each viral infection is different; the duration depends mainly on the virus. Most viral rashes last between a few days and weeks (25).
2. How do I know if my rash is viral?
Some viral infections, such as chicken pox and roseola, cause a characteristic rash that makes them prominent. However, most viral rash symptoms might seem familiar and hence require the attention of a medical advisor.
3. How can I tell if a rash is serious?
It is advisable to get the rashes checked by a doctor and identify their cause, even if there are no accompanying symptoms. However, if the rash is accompanied by a fever, neck or back pain, or headache, it is recommended to seek prompt medical attention (26).
4. Is a rash a symptom of COVID-19 in children?
A mild COVID infection could cause a rash in the toes known as COVID toes. Red or purple fingers, pus, and swelling of the toes are a few signs of rash caused by COVID. Sometimes, in children, this rash could be the only sign of COVID infection (27).
5. What does it mean if a rash is spreading?
Syeda Amna Husain, a New York-based pediatrician, says, “It is typical and anticipated for a viral rash to spread. However, in the case of an allergic or irritant rash, it could be due to the continued presence of the triggering factor. For instance, if a particular detergent is causing a rash on the extremities, using it on a piece of clothing could lead to the spreading of the rash to the trunk.”
6. What viruses cause full-body rashes?
According to Dr. Anna H. Chacon, a board-certified dermatologist from Miami, Florida, “Many diseases, including mononucleosis, chickenpox, sixth disease, and measles result in a viral rash. In different body areas, a rash may manifest as tiny pimples, blisters, or patches. Once the sickness has passed its peak, the rash usually disappears.”
Skin rashes in children are usually caused by microbes, such as bacteria and viruses, or allergies. You may encourage your child to follow proper hygiene practices to reduce microbial exposure. Nevertheless, most rashes resolve quickly with appropriate care and topical ointments. Although they do not cause any harm to a child’s overall health, you must know the origin of the outbreak to avoid further complications. Also, if the rashes persist for more than 24 hours or your child is in pain or discomfort due to rashes, you should get them evaluated by a doctor promptly.
Infographic: Home Remedies For Children’s Skin Rashes
Skin rashes are common in children, probably because their immune system is still developing, and they are exposed to different environmental conditions and people at schools and playdates. So if your child has developed a rash, don’t panic and follow the steps below to take care of them. Illustration: Momjunction Design Team
Illustration: Skin Rashes In Children: Causes And Treatment

Image: Dalle E/MomJunction Design Team
Discover quick and easy ways to treat and relieve your child’s skin rashes. Learn about the best treatments and therapies for children.
Personal Experience: Source
MomJunction articles include first-hand experiences to provide you with better insights through real-life narratives. Here are the sources of personal accounts referenced in this article.
i. Me, my eczema, and I;https://bionicwoman.medium.com/food-is-medicine-84d5fb8c78a0
References
- Chickenpox; National Health Service
- Chickenpox Vaccination: What Everyone Should Know; Centers for Disease Control and Prevention
- Measles Symptoms and Complications; Centers for Disease Control and Prevention
- Measles-; National Health Service
- Rubella (German Measles); Cleveland Clinic
- About Rubella; Centers for Disease Control and Prevention
- Slapped Cheek Syndrome; Centers for Disease Control and Prevention
- Hand, foot and mouth disease; National Health Service
- Molluscum Contagiosum; Centers for Disease Control and Prevention
- Molluscum Contagiosum; Cleveland Clinic
- Preventing Group A Strep Infection; Centers for Disease Control and Prevention
- Scarlet Fever; National Health Service
- Impetigo; Medline Plus; US National Library of Medicine
- Eczema; Medline Plus; US National Library of Medicine
- Eczema (Atopic Dermatitis) Overview; American Academy of Allergy Asthma and Immunology
- Heat Rash; National Health Service
- Erythema Multiforme; Johns Hopkins All Children’s Hospital
- Psoriasis; Great Ormond Street Hospital for Children
- Psoriasis: Diagnosis, Treatment, and Steps to Take; National Institute of Arthritis and Musculoskeletal and Skin Diseases
- Can you prevent psoriasis?; Stanford Health Care
- Preventing Scabies; Centers For Disease Control And Prevention
- Urticaria; National Health Portal
- Ringworm of the Body (Tinea Corporis); Nationwide Children’s Hospital
- Ringworm; Nemours KidsHealth
- Viral Exanthem Rash; Cleveland Clinic
- Rashes; The Royal Children’s Hospital Melbourne
- Rash: Sign Of Coronavirus In Kids; American Academy of Dermatology Association
- About Chickenpox; Centers For Disease Control And Prevention
- Sandeep R.Varma et al.; (2019);In vitro anti-inflammatory and skin protective properties of Virgin coconut oil; Science Direct
- Heat rash (prickly heat); NHS
Community Experiences
Join the conversation and become a part of our nurturing community! Share your stories, experiences, and insights to connect with fellow parents.
Read full bio of Dr. Vineet Kwatra
- Dr. Syeda Amna Husain is a board-certified pediatrician, spokesperson for the American Academy of Pediatrics (AAP), a board-certified lactation consultant, and private practice owner. Dr. Husain lives in NJ. She did her MD at The Brody School of Medicine at East Carolina University and Pediatric Residency at Georgetown University.
 Dr. Syeda Amna Husain is a board-certified pediatrician, spokesperson for the American Academy of Pediatrics (AAP), a board-certified lactation consultant, and private practice owner. Dr. Husain lives in NJ. She did her MD at The Brody School of Medicine at East Carolina University and Pediatric Residency at Georgetown University.
Dr. Syeda Amna Husain is a board-certified pediatrician, spokesperson for the American Academy of Pediatrics (AAP), a board-certified lactation consultant, and private practice owner. Dr. Husain lives in NJ. She did her MD at The Brody School of Medicine at East Carolina University and Pediatric Residency at Georgetown University. 
Dr. Anna H. Chacon is a board-certified dermatologist and author originally from Miami, Florida. She has authored over a dozen peer-reviewed articles, book chapters and has been published in JAAD, Archives of Dermatology, British Journal of Dermatology, Cosmetic Dermatology, and Cutis. An alumnus of Brown University, Dr. Chacon has over 7 years of experience and works as a tele dermatologist.
Dr. Anna H. Chacon is a board-certified dermatologist and author originally from Miami, Florida. She has authored over a dozen peer-reviewed articles, book chapters and has been published in JAAD, Archives of Dermatology, British Journal of Dermatology, Cosmetic Dermatology, and Cutis. An alumnus of Brown University, Dr. Chacon has over 7 years of experience and works as a tele dermatologist.
Read full bio of Dr. Ritika Shah
Read full bio of Swati Patwal
Read full bio of Ghazia Shah