Image: iStock
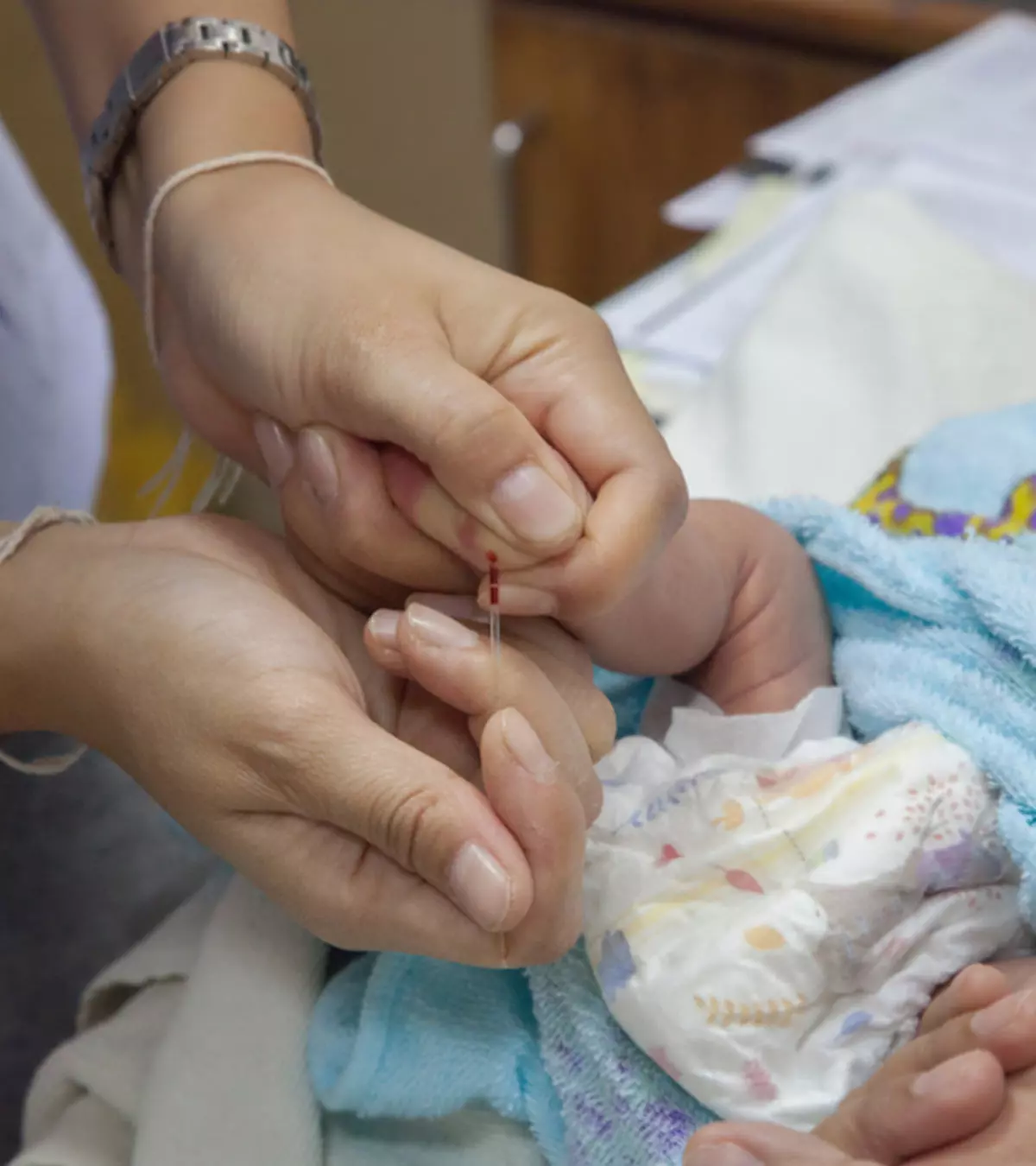
Thrombocytopenia in pregnancy is characterized by low platelets in pregnancy. Platelets are called thrombocytes, and hence the condition is called thrombocytopenia. A normal blood platelet count in healthy individuals ranges from 150,000 to 450,000 per microliter of blood. When the count falls below 150,000 platelets per microliter, it results in thrombocytopenia.
Thrombocytopenia is a common blood disorder during pregnancy. Although a slight decrease in platelet count is usually not concerning, a drastic fall may indicate a serious pregnancy complication (1).
Read on to learn the causes, symptoms, complications, treatment, and more on thrombocytopenia in pregnancy.
Key Pointers
- Thrombocytopenia is a common blood disorder in pregnancy marked by low platelet count.
- Available treatments include prednisone, immunoglobulins, transfusions, and plasma exchange.
- Pregnancy-induced hypertension, autoimmune and bone marrow diseases, viral infections, and fatty liver are among the causes of thrombocytopenia in pregnancy.
- Symptoms of thrombocytopenia in pregnancy are fatigue, frequent bruising, blood in urine/stool, round spots under skin, and excessive bleeding.
- Foods that may help increase platelet count are leafy greens, fortified cereals, nuts, seeds, and omega-3-rich foods.
Occurrence Of Thrombocytopenia During Pregnancy
During normal pregnancy, there is a physiological drop in platelet counts due to changes in blood composition in pregnancy. This drop is found in about 10% of all pregnancies, as reported by a doctor from the Massachusetts General Hospital. Although usually mild and benign, thrombocytopenia is the second most common blood disorder in pregnancy, the first being anemia (1). The condition affects about 6-15% of pregnant women and is mostly seen in later trimesters or towards the end of gestation (2).
Classification Of Thrombocytopenia
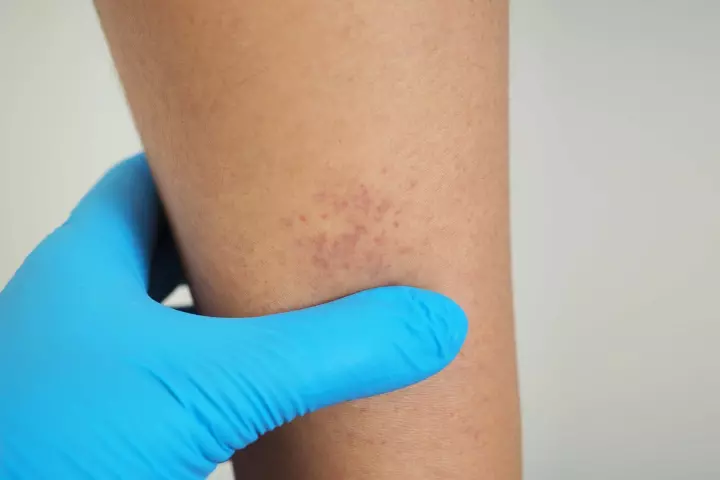
Image: Shutterstock
Thrombocytopenia may be classified into three types based on the number of platelets per microliter of blood (3).
- Mild: 100,000 to 150,000 platelets per microliter of blood
- Moderate: 50,000 to 100,000 platelets per microliter of blood
- Severe: Less than 50,000 platelets per microliter of blood
The platelet count usually drops during pregnancy for various reasons. However, in women who have platelet counts below moderate (around 100,000 per microliter of blood), other underlying health conditions and non-pregnancy-related etiologies must be evaluated.
Causes Of Low Platelets In Pregnancy
Some of the common causes of thrombocytopenia in pregnancy are (1):
- Gestational thrombocytopenia (GT): This is a benign condition in which platelet levels drop to moderate range and accounts for 70-80% of the cases of thrombocytopenia in pregnancy. It is currently unknown why there is a low count of platelets. GT usually develops in the third trimester and is mostly asymptomatic, resolving spontaneously. A frequent monitoring of platelet count is recommended to ensure that the condition is not progressing.
- Hypertensive disorders: Thrombocytopenia associated with hypertensive disorders, such as preeclampsia, eclampsiaiA severe complication of high blood pressure characterized by seizures and unconsciousness in pregnant women. , and HELLP syndrome, is the second leading cause of thrombocytopenia in pregnancy, accounting for approximately 20% of the cases.
- Immune thrombocytopenic purpura: Immune thrombocytopenic purpura (ITP) is an autoimmune disorder stimulated due to platelet destruction in the spleen. However, it is not a frequent cause of thrombocytopenia in pregnancy.
 Quick fact
Quick fact- Fatty liver: Acute fatty liver of pregnancy (AFLP) is a rare but serious condition, where the platelet count may drop below 20,000 per microliter of blood.

Image: Shutterstock
- Other causes: Nutritional deficiencies (most importantly vitamin B12 and folate), autoimmune diseasesiA group of medical conditions where the body’s immune system erroneously attacks healthy cells. , thrombotic thrombocytopenic purpura, certain medications, viral infections (HIV and CMV), and bone marrow diseases may be some of the other causes of thrombocytopenia in pregnancy.
Symptoms Of Thrombocytopenia In Pregnancy
In most cases, pregnant women with thrombocytopenia may be asymptomatic. Some women may show the following common signs of thrombocytopenia (4).
- Bleeding from a cut, the gums, or nose that won’t stop
- Tiny round spots (petechiae) that are caused due to bleeding under the skin
- Presence of blood in the urine or stool
- Red or brown bruises (purpura)
- Frequent bruising
- Fatigue
Complications Of Thrombocytopenia During Pregnancy
If the platelet count falls extremely during pregnancy and continues to remain low until delivery, it might increase the chances of the following complications (1):
- Epidural hematoma and inability to have epidural anesthesia before delivery
- Increased blood loss/postpartum hemorrhage at the time of or following delivery
- Recurrent gestational thrombocytopenia if the woman has a history of thrombocytopenia
- Fetal or neonatal thrombocytopenia (depending on the cause of maternal thrombocytopenia) and increased risk of intracranial hemorrhage
- Other potential complications such as disseminated intravascular coagulationiA serious condition in which blood clots form throughout the body, potentially leading to multiple organ damage. (DIC) and hemolytic and uremic syndromeiA rare but severe condition leading to the breakdown of red blood cells and improper functioning of kidneys and blood vessels. (5)
Treatment For Thrombocytopenia During Pregnancy
Depending on the cause of thrombocytopenia, women with thrombocytopenia during pregnancy may not require treatment until the condition is severe. Your healthcare provider would suggest a CBC test during pregnancy for regular monitoring of the platelet count. Multidisciplinary care in conjunction with a hematologist is usually needed in pregnant women requiring treatment. In the management of thrombocytopenia, addressing maternal mortality and morbidity is crucial for fetal health. Some of the treatment options for thrombocytopenia in pregnancy may include the following (1) (6).
- Oral prednisone: The first-line treatment for pregnant women with thrombocytopenia is with the drug prednisone. Although it is considered pregnancy-safe, a few studies have shown its association with certain adverse effects, such as gestational diabetes (1).

Image: Shutterstock
- Intravenous immunoglobulinsiDefensive proteins produced by the immune system in response to foreign invaders such as bacteria and viruses. (IVIg) and other corticosteroidsiA class of drugs that mimic the effects of cortisol, a hormone produced by the adrenal gland to alleviate inflammation. : Studies have shown that corticosteroids and intravenous immunoglobulin therapy are acceptable in pregnant women with ITP (7).
- Platelet or blood transfusions: Platelet and blood transfusion is indicated in case of emergency cesarean delivery and when the platelet count falls below 50,000 per microliter.
- Plasma exchange: Research suggests that plasma exchange therapy might be used in cases of severe HELLP syndromeiA severe complication of high blood pressure, marked by hemolysis, elevated liver enzymes, and low platelet count in pregnant women. and AFLP.
 Quick fact
Quick factPrecautions For Thrombocytopenia In Pregnancy
Taking certain measures in pregnancy may help in the management of thrombocytopenia in pregnancy (8) (9).
- If you have a history of thrombocytopenia or a family history of blood disorders, you must disclose this to your doctor as there may be certain medications that you need to avoid taking, such as aspirin.

Image: IStock
- Avoid taking any additional medicines, supplements, or herbal remedies without consulting your doctor. These may affect the platelet counts and increase your risk of bleeding.
 Things to know
Things to know- Do not indulge in contact sports and strenuous activities, which may put you at risk of injuries and bruises.
- It is wise to avoid exposure to any toxic and household chemicals, such as pesticides, as they may lead to a drop in platelet counts in some cases.
- Avoid alcohol intake to mitigate the risk of lowered platelet production and liver damage.
- Be gentle while brushing your teeth, shaving, and blowing your nose to avoid potential bleeding risks.
Natural Remedies To Increase Low Platelet Count
The consumption of certain foods during pregnancy may help improve platelet count and improve overall blood health; take note that this does not replace the need to see your doctor regularly and/or medical treatments if necessary (10).
- Fresh green leafy vegetables such as spinach and kale

Image: IStock
- Fruits and veggies such as oranges, berries, beetroots, carrots, and tomatoes
- Foods rich in vitamin C, such as lemon, red bell pepper, sprouts, and broccoli
- Enriched dairy items, peanuts, walnuts, and dark chocolate
- Fortified cereals, lentils, black-eyed peas, eggs, and beef liver
- Foods rich in omega-3 fatty acids such as flaxseeds and fortified cereals
Lena H, a mother and Adult Nurse Practitioner, shares the natural solutions recommended by her midwife to prevent a significant drop in her platelet levels. She says, “My midwife gave me a mixture of dry herbs to drink daily for the rest of my pregnancy. I had ITP, or idiopathic thrombocytopenia purpura, with both of my pregnancies…So needless to say, if I hope to have my dream home birth, my platelets must stay in a healthy range. My midwife advised drinking nettle tea for this purpose. However, the herbal pregnancy blend I received from her also included red raspberry leaf, alfalfa & oat straw (i).”
Combining these dietary choices with medical guidance in a holistic approach may help maintain a healthy platelet level during pregnancy.
Note: Pregnant women are advised to avoid intake of fish that potentially contain high mercury levels, such as swordfish, tilefish, king mackerel, and shark. You may contact your doctor if you are unsure about including any new foods in your diet during pregnancy.
Effect Of Thrombocytopenia On The Baby
Mild thrombocytopenia is common in normal pregnancy and has no adverse effects on the mother and fetus. Conversely, severe thrombocytopenia, along with other underlying medical conditions, may lead to adverse fetal-maternal outcomes (1). Several research studies suggest that low maternal platelet counts during the first trimester of pregnancy can result in pregnancy complications, including miscarriage (11). However, no research studies prove that thrombocytopenia in pregnancy alone can cause any birth defects in babies (12).
Frequently Asked Questions
1. How long does it take for platelets to increase after pregnancy?
After childbirth, it generally takes a few weeks for the platelet count to return to normal levels as in nonpregnant women (12).
2. Does banana increase platelet count in pregnancy?
No. Foods containing folate, iron, and vitamins B-12, C, D, and K help increase platelet count (13). However, bananas do not contain vitamins B-12, D, and K and contain low amounts of folate, iron, and vitamin C, which are not enough to promote platelet count (14).
3. Can low platelets cause early labor?
A high drop in platelet counts during pregnancy may lead to maternal health complications, such as preterm labor (10).
Mild thrombocytopenia is relatively common in most pregnancies, but several studies have shown no serious consequences for the mother and the child. Nevertheless, if you have a low platelet count during pregnancy, you must make sure to keep a watch on your symptoms, such as red and brown bruises, blood in urine and stool, or nose bleed during pregnancy. Take good care and have regular follow-up visits with your healthcare provider so that your thrombocytopenia can be closely monitored.
Infographic: Symptoms Of Thrombocytopenia In Pregnancy
In mild cases, pregnant women may not exhibit symptoms, but severe thrombocytopenia can reduce platelet count significantly and cause specific symptoms during pregnancy, as depicted in the infographic below.
Some thing wrong with infographic shortcode. please verify shortcode syntaxIllustration: Low Platelets In Pregnancy: Symptoms Causes And Treatment
Image: Dalle E/MomJunction Design Team
Pregnancy can be a joyous time, but you also need to be careful of several pregnancy-related risks and complications. Learn about thrombotic thrombocytopenic purpura and how it can affect pregnant women.
Personal Experience: Source
MomJunction articles include first-hand experiences to provide you with better insights through real-life narratives. Here are the sources of personal accounts referenced in this article.
i. 17 weeks.https://reflectingtheheart.blogspot.com/2011/06/pregnancy-update-17-weeks.html
References
- Anca Marina Ciobanu; (2016); Thrombocytopenia in Pregnancy.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5394486/ - F. Boehlen; (2006); Thrombocytopenia during pregnancy. Importance diagnosis and management.
https://pubmed.ncbi.nlm.nih.gov/16444327/ - Thrombocytopenia in Pregnancy.
https://thejh.org/index.php/jh/article/view/28/20 - Low Platelet Count (Bleeding); American Cancer Society
https://www.cancer.org/cancer/managing-cancer/side-effects/low-blood-counts/bleeding.html - Laure Federici, et al.; (2008); Thrombocytopenia during pregnancy: from etiologic diagnosis to therapeutic management.
https://pubmed.ncbi.nlm.nih.gov/18621503/ - Terry Gernsheimer, et al.; (2013); How I treat thrombocytopenia in pregnancy.
https://ashpublications.org/blood/article/121/1/38/31058/How-I-treat-thrombocytopenia-in-pregnancy - Dongmei Sun, et al.; (2016); Corticosteroids compared with intravenous immunoglobulin for the treatment of immune thrombocytopenia in pregnancy.
https://ashpublications.org/blood/article/128/10/1329/35306/Corticosteroids-compared-with-intravenous - Thrombocytopenia.
https://my.clevelandclinic.org/health/diseases/14430-thrombocytopenia - Important Outside Influences: Understanding What Impacts Your Platelets.
https://pdsa.org/about-itp/warnings - How can having low platelets affect my pregnancy and birth plan?
https://utswmed.org/medblog/low-platelets-pregnancy/ - Piazze Juan, et al.; (2011); Platelets in pregnancy.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3399052/ - Jessica A. Reese, et al.; (2019); Platelet Counts during Pregnancy
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6049077/ - Swati Burungale; Natural remedies to increase platelet count.
https://www.thepharmajournal.com/archives/2016/vol5issue12/PartA/5-12-1-648.pdf - Bananas ripe and slightly ripe raw.
https://fdc.nal.usda.gov/fdc-app.html#/food-details/1105314/nutrients - Ankit Mangla and Hussein Hamad; (2026); Thrombocytopenia in Pregnancy.
https://www.ncbi.nlm.nih.gov/books/NBK547705/
Community Experiences
Join the conversation and become a part of our nurturing community! Share your stories, experiences, and insights to connect with fellow parents.
Read full bio of Dr. Ng Kai Lyn
Read full bio of Vidya Tadapatri
Read full bio of Rebecca Malachi
Read full bio of Dr. Joyani Das