Image: ShutterStock
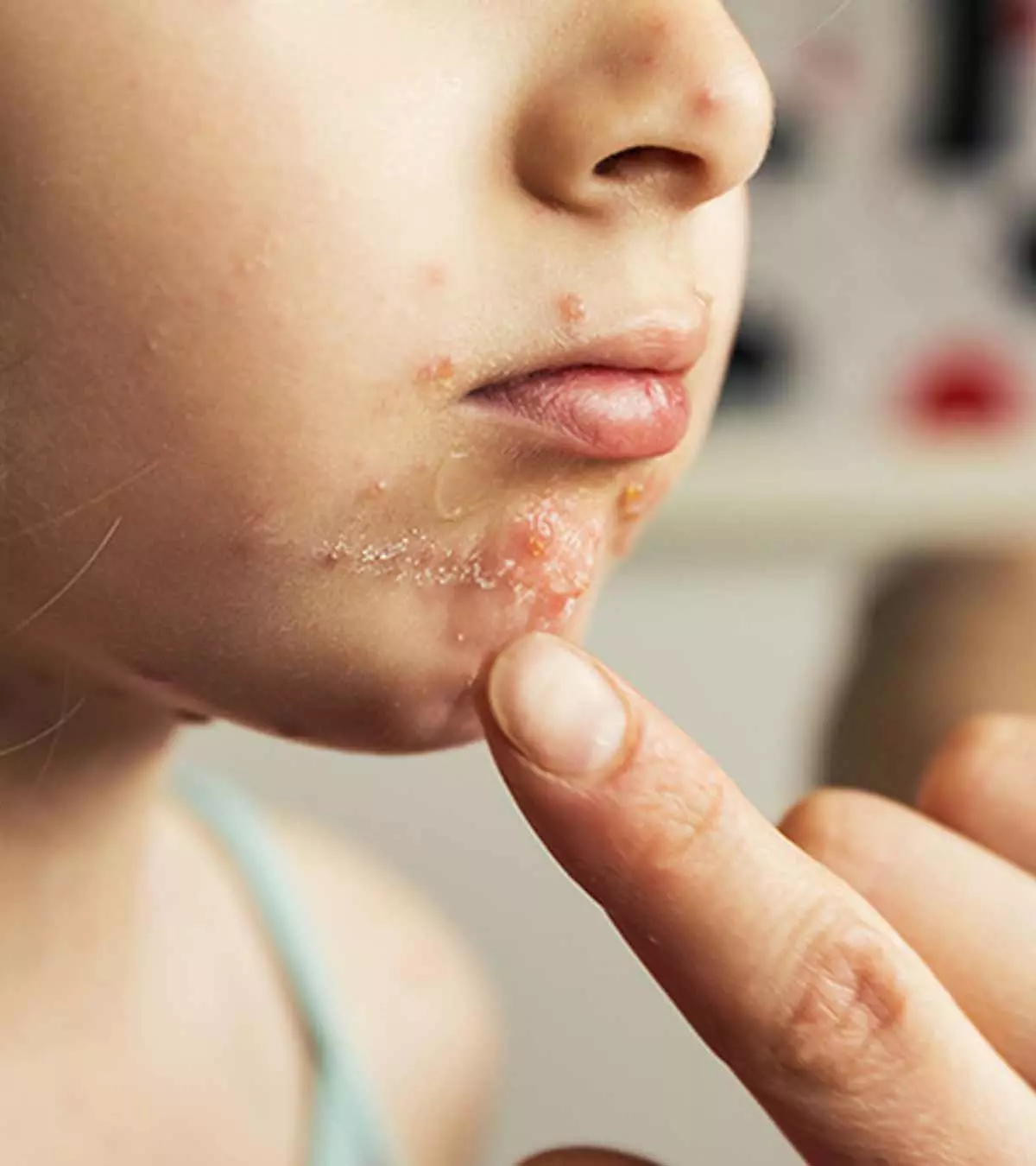
Blocked tear ducts and allergies are a common cause of epiphora or watery eyes in children. Tears fill the eyes and drain onto the face when the ducts are blocked. Although it looks like weeping, there is no emotional trigger for these tears. Watery eyes can be self-resolving, and often no interventions or remedies are needed. However, a few children may need medications, or sometimes even surgical intervention is necessary to get relief from blockage or allergies. Awareness of the signs and symptoms of blocked tear ducts and other eye problems in children can help parents know when to seek medical care. However, if you are unsure of the underlying cause or the child has other symptoms, it is advised to visit the pediatrician or a pediatric ophthalmology specialist. Read on to know the causes, symptoms, and management of watery eyes in children.
Key Pointers
- Children’s watery eyes may result from various conditions, including allergies, pink eye, the common cold, and eye injuries.
- Treatment options might range from utilizing medications to undergoing surgery, depending on what is causing the teary eyes.
- Saline solutions, tea bags, and cold and hot compresses are some home remedies that could be helpful.
- Contact a medical professional right away if the watery eyes are accompanied by swelling, eye discharge, pain, or redness.
Possible Causes And Treatments For Watery Eyes In Children
Most causes of watery eyes in children can be treated or managed. Read on to know more about the reasons.
1. Blocked tear ducts
This common condition in infants is also known as congenitaliA condition present from birth nasolacrimal ductiDuct that transports tears from the ocular surface towards the lacrimal sac and, eventually, the nasal cavity obstruction (NLDO) or dacryostenosis. Statistics show that around six percent of all newborns are born with a blocked tear duct (1). In children with this condition, the opening of the tear duct is not appropriately formed, which might result in watery eyes.
This can occur in one eye or both eyes, may go away on its own, or be intermittent.
Associated Symptoms
Along with watery eyes, other symptoms of blocked tear ducts might include:
- Tear pool at the corner of the eyes.
- Mucus or yellow discharge due to infection because of the stagnant and moist environment in the tear duct; this could also cause sticky eyes in the morning.
- Redness of eyes due to rubbing (2).
Treatment
- The eye doctor would do a physical examination to find out your child’s condition.
- Based on the examination, they might suggest waiting for it to resolve on its own or clearing the duct opening manually using a probe.
- There is conflicting evidence as to when the optimal time is to do the procedure. It is a technically difficult procedure and as with any procedure does not have a 100% outcome.
- Most of these cases resolve spontaneously within the first six to 12 months.
- There is some evidence that a lateral nasal massage can speed up the process. Place your thumb or forefinger on the region where the inside of the eye and nasal bone meet. Stroke downward firmly. This might help the pus or fluid that is trapped in the tear sac, to move downward due to the pressure put by the finger. You may try about five strokes, three to four times a day for several weeks. (3).
 Point to consider
Point to consider2. Allergies

Watery eyes could also be a symptom of allergies (allergic conjunctivitisiInfection or inflammation of the clear membrane that lines the eyelids and eyeball ). The 2026 CDC National Health Interview Survey data reveals that the prevalence rate of seasonal allergies, such as allergic conjunctivitis, allergic rhinitis, and hay fever, among children could be approximately 18.9% (4). The cause of such allergic reactions could be an external factor, such as insect bite or sting, dust, mites, mold spores, pollen, ragweed, grass, foods such as dairy, eggs, soy, nuts, hay fever, and sometimes certain medications.
Associated symptoms
- Runny nose
- Nasal congestion
- Sneezing
- Itchy red and swollen eyes
- Headache
- Itchy nose, mouth, and throat
Treatment
Identifying and avoiding the allergy-causing agent can help in preventing allergic reactions. You may also:
- Keep your home dust-free
- Discourage your children from going out and playing when there is pollen in the air
- Clean and replace the filters in your house regularly
- Use wraparound sunglasses when there is dust in the air
- Avoid second hand smoke
If it is not always possible to avoid an allergen, then take your child to the doctor, and they might prescribe antihistamine eye drops and other medications to relieve the symptoms (5).
3. Dry eye syndrome
Sometimes, watery eyes can be due to dry eye syndrome. It may seem unlikely, but dry eye syndrome can stimulate the tear glands to overproduce tears as a protective response (5).
Associated symptoms
- A sensation that a foreign body is in the eye
- Burning sensation
- Rubbing of eyes and redness (6)
Treatment
Once your child’s doctor confirms the diagnosis of dry eye syndrome, they may prescribe eye drops, gels, and artificial tears.
4. Conjunctivitis (pink eye)
Watering of eyes in children could also be due to an infection called conjunctivitis. Also known as pink eye, this is a common eye infection. Pink eye (conjunctivitis) in kids is likely caused due to allergies, bacterial infections (bacterial conjunctivitis), or viral infections (viral conjunctivitis) (7). Among these, bacterial conjunctivitis tends to occur more frequently. According to studies, it accounts for up to 70% of all conjunctivitis cases in children (8).
Associated symptoms
The symptoms could vary based on what is causing the eye infection, and may include:
- Watery discharge, if the infection is due to viruses
- Pus-filled eye discharge or conjunctival discharge in the case of bacterial infection
- Sometimes, fever and sore throat may also be experienced
- Eyelid swelling or cornealiThe transparent portion of the eye that protects the iris and pupil while allowing light to reach the eye ulcers
Treatment
The treatment options vary according to the causative microorganism; your child’s doctor might prescribe broad-spectrum antibiotics and eye ointments in the case of bacterial infections. There are no specific treatments for certain viral infections in children, and they might get better in a week or two. However, antibiotics and eye ointments could be given to prevent secondary infections (9).
Zibby Owens, a mother of four, shares how she treated her daughter’s pink eye. She says, “The next morning, my daughter woke up and said, perplexed, at the top of the stairs, ‘Mama, my eye feels a little funny.’ Uh-oh. I bounded up the steps only to find her right eye completely encrusted. Pink eye. She was blinking repeatedly and purposefully as if the motion would somehow cause the thick layer of crust to magically disappear… I applied wet compresses to my daughter’s eye and pumped her with Motrin (i).”
5. Common cold
Red eyes, with watery discharge, are a common symptom of a cold. If there is pus in the discharge, then it could indicate a bacterial infection.
Associated symptoms
- Runny nose
- Nasal congestion
- Sneezing
- Coughing
- Sore throat
Treatment
Common cold usually gets better on its own in a week. However, you could try certain home care tips such as using humidifiersiA device used to increase the moisture in the air , clearing the nasal congestion with a suction bulb, or using some over-the-counter cold medications (consult your doctor if your child is below three years) (10).
6. Eye injuries
Children are susceptible to eye injuries while playing. The injury would be on the white part of the eye. If they are using contact lenses, they might have watery eyes.
Associated symptoms
- Eye pain
- Feeling the presence of a foreign body in the eye
- Teary eyes
Treatment
If the pain is mild and the scratch is superficial, then it would resolve on its own. Rinsing your eye with clear water, avoiding rubbing or touching the eye can help speed up the recovery. However, if the pain is unbearable and if you have noticed damage to the pupil, then take your child to the doctor (11). Moreover, if your child complains of their vision blurring or light sensitivity, contact your doctor immediately.
7. Blepharitis
This condition causes inflammation of the eyelids. Although this is not a serious condition, it might cause complications, such as permanent alteration of eyelid structure, if left untreated.
Associated symptoms
- Ocular discomfort
- Watery eyes
- Redness of the eyes
- Eye or eyelid redness
- A sensation of a foreign body in the eye
- Crusting of eyelids
Treatment
Primary care involves massaging and rinsing the eyelids to remove the dead skin debris and crusting. Your child’s doctor might also prescribe antibiotics (12).
 Quick fact
Quick fact8. Other causes

Watery eyes could also be due to bright light, irritation due to a foreign body sensation in the eyes, eye strain due to prolonged exposure to smartphones, excessive laughing, and yawning.
Treatment
These are normal conditions and usually do not need medical intervention. Rinsing the eyes with water to remove the foreign object and restricting your child’s screen time might help.
When To See A Doctor?

Take your child to a doctor if you notice any of the following signs, along with watery eyes.
- Eyes exposed to or come in contact with chemicals
- Inflammation and redness with severe pain
- Suspect a major eye injury
- High amounts of eye discharge
- Child is often rubbing the eyes
- Prolonged watering of eyes
- Change in the color of the eye – especially if only one eye is involved and is red and painful – then see a doctor as soon as possible
 Be watchful
Be watchfulHome Remedies For Watery Eyes In Children
Watery eyes might be a symptom of an underlying cause, so it is always advised to look for other signs and identify the underlying cause. Your child’s doctor would determine the best course of treatment after examining your child’s eye and the additional symptoms.
In addition to the treatment, you may also consider trying some of these home remedies to provide relief to watery eyes. However, try these home remedies only if there is mild pain but no irritation.
- Saline water: In the case of conjunctivitis, you could consider cleaning the eyes with clean water or normal saline solution before applying the eye ointment (13). Saltwater has been traditionally used as a treatment option for an eye infection, as it has antimicrobial properties.
- Teabags: There are no studies to prove if tea bags can help in treating the underlying problem for watery eyes. However, some teas such as Rooibos tea and black tea are said to have anti-inflammatory properties that might help in soothing the eye and providing comfort (14) (15). You can place cold tea bags on your child’s eyes, while they keep their eyes closed for 15 minutes.
- Massage: If your doctor has recommended waiting until your child’s tear ducts open up on their own, then massage might help. To perform the massage,
- Put one drop of the prescribed eye drops in the eye.
- Place your index finger near the side of the nose under the eye to be massaged.
- Move your finger in short downward strokes while pressing firmly.
- Repeat this thrice daily (16).
- Hot compress: For bacterial eye infections, the American Academy of Ophthalmology suggests soaking a clean washcloth in warm water and placing it on the eyes until it becomes cold (17).
According to a Cochrane review, a warm compress is also said to ensure eyelid hygiene (18). Hot compresses are also considered as traditional treatments for dry eye (19).
- Cold compress: According to the American Academy of Ophthalmology, applying cold compress might help in reducing watery eyes due to allergies. Soak a washcloth in cold water and put it on the child’s eyes for a few minutes. You can repeat this several times in a day (17).

Can You Prevent Watery Eyes In Children?

Prevention is possible based on the underlying cause of watery eyes in children. You may try the following measures to prevent watery eyes due to infection, allergies, common cold, or eye injuries.
- Make sure your child does not share towels and bedsheets with people who have conjunctivitis.
- Identify the allergens and try to keep your children away from them.
- Explain the importance of safety and hygiene during playtime and around pets – never touch the eyes immediately after touching something dirty or a pet.
- Include a balanced diet for your children to strengthen their immunity and make them less prone to the common cold.
- If your children are using contact lenses, then make sure they use them properly to avoid infections or injuries to the eye.
- Reduce screen time to prevent eye strain and watery eyes, particularly if they use devices for extended periods. Encourage them to take breaks every 20 minutes to give their eyes a rest.
Frequently Asked Questions
1. What does a bacterial eye infection look like?
The following are the symptoms of a bacterial eye infection (20):
- Deposition of yellow or green colored discharge in the corner of the eyes
- Puffy or swollen lids
- White part of the eyes appears pink
- Eyelashes might stick when asleep
- Dried pus on the eyelashes
2. Can sinusitisiAn infection of the paranasal sinuses cause epiphora in children?
Yes, blocking the tear duct from an eye injury or disease can lead to epiphora (excessive tearing of the eye) in children (21).
3. Are watery eyes and sneezing symptoms of Covid?
Although sneezing is a common symptom of Covid, the combination of watery eyes and sneezing are usually signs of a cold or seasonal allergy (22).
4. Are itchy, watery eyes a symptom of COVID-19 in children?
No, itchy and watery eyes are not a symptom of COVID-19 in children. They could be the symptoms of seasonal allergies (23).
5. What age group is most susceptible to watery eyes?
Infants and toddlers are more prone to watery eyes, often caused by blocked tear ducts and allergies.
Watery eyes in children could be due to benign factors or underlying issues. For example, allergies, common cold, or tear gland malfunctioning could lead to watery eyes. If there is a suspicion of prolonged eye-watering, get your child tested to diagnose the underlying cause. Simultaneously, if you notice other symptoms such as sticky eyes, redness, discharge, or swollen eyelids in children, report to your doctor for prompt medical attention as it could be a sign of an infection. Follow the treatment course as suggested by the ophthalmologistiA physician or osteopathic doctor who specializes in vision and eye care . If you wish to follow any home remedies, consult your doctor before you practice.
Infographic: Does Watery Eyes Mean Bacterial Infection?
Watery eyes are not a specific symptom of bacterial eye infection, and they may not be cured with antibiotics. Blocked tear ducts or viral eye infections can cause watery discharge in children. It resolves as the underlying condition resolves. Go through the infographic to learn to distinguish watery eyes from bacterial eye infections in children.
Some thing wrong with infographic shortcode. please verify shortcode syntax
Illustration: Watery Eyes In Kids Causes Symptoms Treatment & Remedies

Image: Dall·E/MomJunction Design Team
Prior to receiving treatment for watery eyes, children commonly experience discomforting symptoms such as eye redness, itching, and a sensation of burning. Watch our informative video to gain more insights.
Personal Experience: Source
MomJunction articles include first-hand experiences to provide you with better insights through real-life narratives. Here are the sources of personal accounts referenced in this article.
i. The big sick: my daughter’s eye infection taught me that old-fashioned fun is the best of all;https://zibbyowens.medium.com/the-big-sick-my-daughters-eye-infection-taught-me-that-old-fashioned-fun-is-the-best-of-all-f6433e2c618
References
- Blocked Tear Duct (Dacryostenosis); Boston Children’s Hospital
https://www.childrenshospital.org/conditions/blocked-tear-duct-dacryostenosis - Yomayra Perez; Bhupendra C. Patel; Magda D. Mendez; Nasolacrimal Duct Obstruction; NCBI
https://www.ncbi.nlm.nih.gov/books/NBK532873/ - Petris C Liu D; Using a probe to clear a blockage in a child’s tear duct;; Cochrane Review
https://www.cochrane.org/CD011109/EYES_using-probe-clear-blockage-childs-tear-duct - Diagnosed Allergic Conditions in Children Aged 0–17 Years: United States 2026; Centers for Disease Control and Prevention
https://www.cdc.gov/nchs/products/databriefs/db459.htm#:~:text=In%202021%2C%2018.9%25%20of%20children%20had%20a%20seasonal%20allergy%2C%2010.8%25%20had%20eczema%2C%20and%205.8%25%20had%20a%20food%20allergy - Ahmed Elshemy
Mohammed Abobakr; Allergic Reaction: Symptoms - Laura B. Kaufman; Are We Missing Dry Eye in Children?; American Academy of Ophthalmology
https://www.aao.org/eyenet/article/are-we-missing-dry-eye-in-children - Conjunctivitis; American Optometric Association
https://ebiz.aoa.org/sso/login.aspx?vi=7&vt=b3b275436a5ebb4ad8cb5a92209f45b3452190ed20bb376191a12090d65856c60d5acc1e0181130fd2576db7adc26a586bbcc961d7e37dbcdb7ccc0a2fb1ad744541358782fdaa422534bac510230281f96e0a49b49c693530977c86fab8724828f746a999b40d43ed24b83a962aa4c5&DPLF=Y - Mahoney Matthew J.
et al; Pediatric Conjunctivitis: A Review of Clinical Manifestations Diagnosis and Management; Children - Conjunctivitis in Children; Stanford Children’s
https://www.stanfordchildrens.org/en/topic/default?id=conjunctivitis-in-children-90-P02078 - Colds in children; Canadian Paediatric Society
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2722603/pdf/pch10493.pdf - Kierstan Boyd and Dan Gudgel; First Aid for Eye Scratches; American Academy of Ophthalmology
https://www.aao.org/eye-health/tips-prevention/first-aid-eye-scratches - Chirstopher M Putnam; Diagnosis and management of blepharitis: an optometrist’s perspective; Dovepress
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6095371/pdf/opto-8-071.pdf - Isaac Baba; The red eye – first aid at the primary level; Community Eye Health Journal
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC1705661/pdf/jceh_18_53_070.pdf - Baba H et al.; Studies of anti-inflammatory effects of Rooibos tea in rats; NCBI
https://www.ncbi.nlm.nih.gov/pubmed/19419525 - Priyanka Chatterjee Sangita Chandra and Sanjib Bhattacharya; Evaluation of anti-inflammatory effects of green tea and black tea: A comparative in vitro study; Journal of Advanced Pharmaceutical Technology
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3401676/ - Eye: Tear Duct Massage; Nationwide Children’s Hospital
https://www.nationwidechildrens.org/family-resources-education/health-wellness-and-safety-resources/helping-hands/eye-tear-duct-massage - Quick Home Remedies for Pink Eye; American Academy of Ophthalmology
https://www.aao.org/eye-health/diseases/pink-eye-quick-home-remedies - Kristina Lindsley Sueko Matsumura and Esen K Akpek; Interventions for chronic blepharitis; The Cochrane Database of Systematic Reviews
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4270370/ - Jing Qiao and Xiaoming Yan; Emerging treatment options for meibomian gland dysfunction; Clinical Ophthalmology
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3772773/ - Eye – Pus or Discharge; Seattle Children’s Hospital
https://www.seattlechildrens.org/conditions/a-z/eye-pus-or-discharge/ - Sinusitis in Children; Johns Hopkins Medicine
https://www.hopkinsmedicine.org/health/conditions-and-diseases/sinusitis-in-children - Is it coronavirus (COVID-19) the flu a cold or seasonal allergies?; Atrium Health
https://atriumhealth.org/medical-services/prevention-wellness/covid - Allergies and Coronavirus (COVID-19); The Royal Children’s Hospital Melbourne
https://www.rch.org.au/kidsinfo/fact_sheets/Allergies_and_Coronavirus_(COVID-19)/ - Watering eyes; Milford Eye Clinic
https://www.milfordeyeclinic.co.nz/services/childrens-eye-problems/watering-eyes/ - Watering eyes; NHS
https://www.nhs.uk/conditions/watering-eyes/
Community Experiences
Join the conversation and become a part of our nurturing community! Share your stories, experiences, and insights to connect with fellow parents.
Read full bio of Dr. Wayne Hough
Read full bio of Dr Bisny T. Joseph
Read full bio of Swati Patwal
Read full bio of Anindita Ghatak