Image: ShutterStock
Moles, or melanocytic nevi (MN), are harmless patches or spots on the skin that may be present at birth or develop over time (1). Women may sometimes notice a change in moles during pregnancy (2). These changes may be influenced by the physical and hormonal changes in the body. As a result, women may notice new moles or old moles may disappear. Some may even notice that their moles are growing bigger or darker than usual. Fortunately, these changes do not indicate any risk. However, if you notice some worrying changes in your mole’s color, size, and texture during pregnancy, it is important to consult a doctor (3). On the other hand, brown or black moles could be a type of birthmark that is known as congenital moles or congenital melanocytic nevi (4). They are usually caused by an overgrowth of pigment cells and could have become hairy and darker during puberty. Read this post to know more about the changes moles undergo during pregnancy, the reasons behind it, and the symptoms you should not ignore.
Key Pointers
- Pregnancy can cause hormonal changes that make existing moles more prominent or darker, and increase their number.
- Moles with even pigmentation, distinct edges, and smooth surface are considered normal.
- It is important to check for any changes or warning signs of skin cancer with a dermatologist.
- In most cases, pregnancy-related moles will disappear after childbirth.
- However, if there are any malignant instances, they need to be treated immediately.
- Melanoma, a type of skin cancer, may appear as a new or changing mole, but it is unlikely to spread to the baby.
Is It Normal For Moles To Change During Pregnancy?

During pregnancy, the moles you already have may undergo minor changes. Some, especially those present on the abdomen and breasts, may become larger and darker. These are benign changes that could happen due to the stretching of the skin or fluctuating hormone levels or hormonal imbalance (5) (6).
A study investigated dermoscopic changes in melanocytic nevi in 2,799 pregnant women, shedding light on how pregnancy can influence the appearance of moles. The study report states, “In pregnant women, diameter, number of colors, shape asymmetry, and border sharpness increased, while ellipseness decreased from the first trimester to postpartum. These changes occurred mainly during the third trimester to postpartum (7).”
However, in rare cases, moles that change asymmetrically could become malignant (cancerous) and may require dermatological care. You should get it checked by a specialist for care before they could negatively impact maternal health or fetus development.
What Causes Moles To Develop During Pregnancy?
New moles may develop due to hormonal changes in pregnancy (8). The increasing hormonal levels of estrogeniA sex hormone responsible for the development of female sexual characteristics and progesteroneiA female reproductive hormone that plays an important role in menstruation, pregnancy, and breastfeeding stimulate the melanocytes (cells producing melanin pigment) to produce more pigment (9). Melanin is a natural pigment that gives your skin its natural color and is also known for causing skin pigmentation. Moles thereby appear where there is a concentration of pigment-making cells in the skin (10).
Do Moles Get Itchy When Pregnant?

Moles may get itchy when the nerves of the skin get irritated or experience changes. The irritation may be from the chemicals that you apply to the skin, peeling of the skin from sunburn, or dry skin (11). In some cases, a mole could turn itchy solely due to the changes it undergoes (stretching skin or hormonal surge). Using fragrance-free cleansers and moisturizers may help minimize itchiness or irritation. Always consult your doctor before using any topical treatments.
When Do Moles Get Harmful?
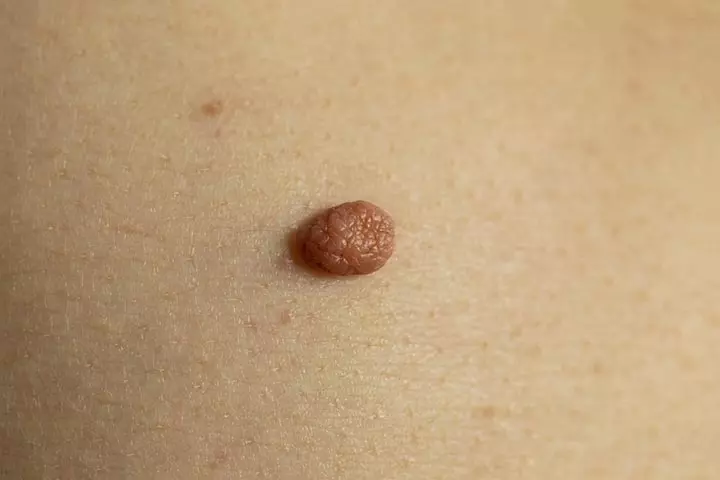
In general, moles have even pigmentation, distinct edges, and a smooth surface. Checking the changing moles and also examining the emerging moles for the warning signs and symptoms is important to determine if they need medical attention. Talk to your doctor or a dermatologist for the right diagnosis if the moles (12) (13):
- Have uneven or ragged borders
- Have uneven color tone, either become darker or have varied colors
- Form flakes and crusts
- Are itchy
- Bleed and cause pain
- Are raised from the skin surface
- Is larger than 6mm
These changes could happen over weeks and months. In some cases, these could be signs of melanoma, a type of skin cancer (3).
Is Mole Removal Safe During Pregnancy?
There is limited study on the safety of mole removal in pregnant women. The local anesthetics, such as lidocaine, used to numb the area for a mole excision are relatively safe to use in pregnancy, but in small doses (14). However, higher doses and exposure during the first trimester could have teratogenic effects on the fetus.
Do Pregnancy Moles Go Away After Childbirth?
Pregnancy moles are likely to go away after delivery, unless they are malignant, in which case they warrant medical intervention (5). While most pregnancy-related moles are benign, it’s important to monitor them postpartum. In some cases, persistent moles can be removed for cosmetic reasons or if medically necessary.
What Is Melanoma And How To Look For It During Pregnancy?
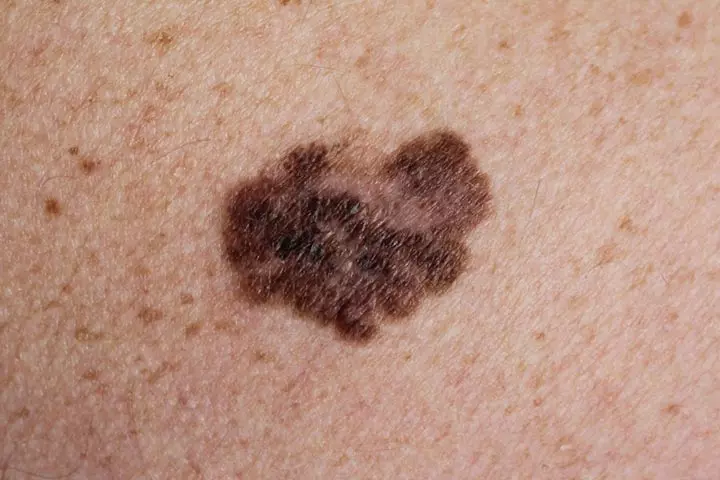
Melanoma is a type of skin cancer that develops from pigment-producing cells (melanocytes). It either appears as a new mole or changes an existing mole into a cancerous one. According to the National Cancer Institute, there were an estimated 1,449,916 people living with melanoma of the skin in the US, in the year 2026 (15). The specific genetic factor that contributes to acquired melanocytic moles remains unknown but developing large numbers of moles may be an autosomal dominant traitiA trait or characteristic that shows up when you get just one copy of that gene from either your mom or dad . It is also likely to occur from exposure to UV rays from the sun and also tanning beds (16).
The signs and symptoms of melanoma in pregnant women are the same as those in non-pregnant women. To evaluate the changes, you can follow the ABCDE rule. This rule for self-examination of the skin was introduced by a group of dermatologists as ABCD in 1985 and was later expanded to ABCDE in 2004 (17).
- A is for Asymmetry, which means that half of the mole looks different from the other half in color, shape, or texture.
- B is for Border irregularity, which implies that the border is irregular or ragged with no defined edges.
- C is for Color variation, meaning the color is not uniform throughout the mole and has shades of brown, tan, black, red, or even blue and white.
- D is for Diameter, which suggests that moles greater than six millimeters could be malignant.
- E is for Evolving; this is also known as ‘the ugly duckling sign,’ where some moles look different from other moles. They change or enlarge with time, and that can be a cause for concern.
If you have a mole that meets one or more of the above criteria, you should consult a doctor immediately.
 Experts say
Experts sayIs Melanoma Treatment Recommended During Pregnancy?
Treatment for pregnant melanoma patients is usually the same as it is for anyone else. Also, the treatment depends on the stage of melanoma (18).
- For early-stage melanoma, treatment may involve a surgery where the melanoma is removed after the administration of a local anesthetic. Also, a section of healthy skin that surrounds the melanoma is removed, and the surgery is usually considered safe to undergo while pregnant.
Leah, a mother of four, shares her story about dealing with skin cancer while pregnant, “I noticed a beauty mark on my forehead that I hadn’t noticed before. It was right above my eyebrow. I was pregnant at the time. So, I went to the dermatologist, who ordered a biopsy. He scraped it off with a razor or something similar. To make a long story short, I had basal cell carcinoma! My doctor quickly introduced me to a plastic surgeon. Surgery was scheduled for one month after my due date.
“Delivered my baby and then two weeks later, the dreaded appointment. Basically, the doctor cuts around the spot, sends that sample down the hall for the pathologist to look at, and then decides if any more needs to be removed. The incision was vertical, so the skin could be pulled closed easily. The pathologist found cancer at the top of the incision as well as in the original place. I’m not sure how many stitches there were, but my face was swollen for a couple of days, but in the end, it healed well (i).”
- For advanced-stage melanoma that has spread, chemotherapy and immunotherapy may be the options. Both are not recommended during pregnancy as they pose serious side effects, such as risks of birth defects and spontaneous abortion (5).
Can Melanoma Spread To The Baby?
Melanoma is not likely to spread to the baby. In late-stage cancer, when the internal organs are affected, there might be a risk of cancer spreading to the placenta and the baby. In this case, the placenta needs a thorough examination, and the baby should be under a dermatologist’s supervision (18).
 Things to know
Things to knowFrequently Asked Questions
1. Can changes in moles during pregnancy be hereditary?
Moles are benign aggregations of melanocytes caused by an alteration in the proteins that manage these cells. Research has been done to determine the genetic influence of BRAFiA gene that produces a protein involved in cell growth signaling, and when mutated, it can lead to uncontrolled cell growth and other similar genes on changing melanocyte cell aggregations. However, little evidence exists to establish the relationship between pregnancy mole changes and these genetic factors (8).
2. What can pregnant women do to protect themselves from changes in moles?
Changes in moles during pregnancy are quite common due to hormonal changes and do not require remedies or preventive measures. But staying hydrated and maintaining a balanced diet may help maintain overall health during pregnancy. However, do speak to a doctor if you notice sudden changes in existing moles or the appearance of new moles (19).
3. How can pregnant women protect their skin from sun exposure and prevent the formation of new moles?
One of the best ways for pregnant women to protect their skin is to stay indoors as much as possible. You can also opt for protective measures against harsh direct sunlight and harmful UV rays by using sunscreen and protective clothing when you venture out in the sun (20).
4. Is it safe to use topical treatments for existing moles during pregnancy?
The fluctuations in hormone levels may lead to change in moles during pregnancy. The mole changes brought by the pregnancy-related conditions usually diminish on their own after the delivery. However, if they have taken an irregular shape or if they worry you, it is safe to get them checked by a dermatologist. The medical team would perform a proper diagnosis of the mole to determine its state of normalcy. A malignant mole would be treated promptly.
Alternatively, follow a good skin care routine and avoid sun exposure. Always use dermatologically-approved sunscreens based on your skin type. Visit a dermatologist regularly to identify any skin issues in their early stages.
Infographic: When To Inform Your Doctor About Your Moles During Pregnancy?
Pregnancy can sometimes cause moles to change in size, shape, or color due to hormonal fluctuations. However, if a mole appears suddenly or undergoes significant changes during pregnancy, it is essential to have it evaluated by a healthcare provider. Scroll through the following infographic for a list of other signs you should be aware of. Illustration: Momjunction Design Team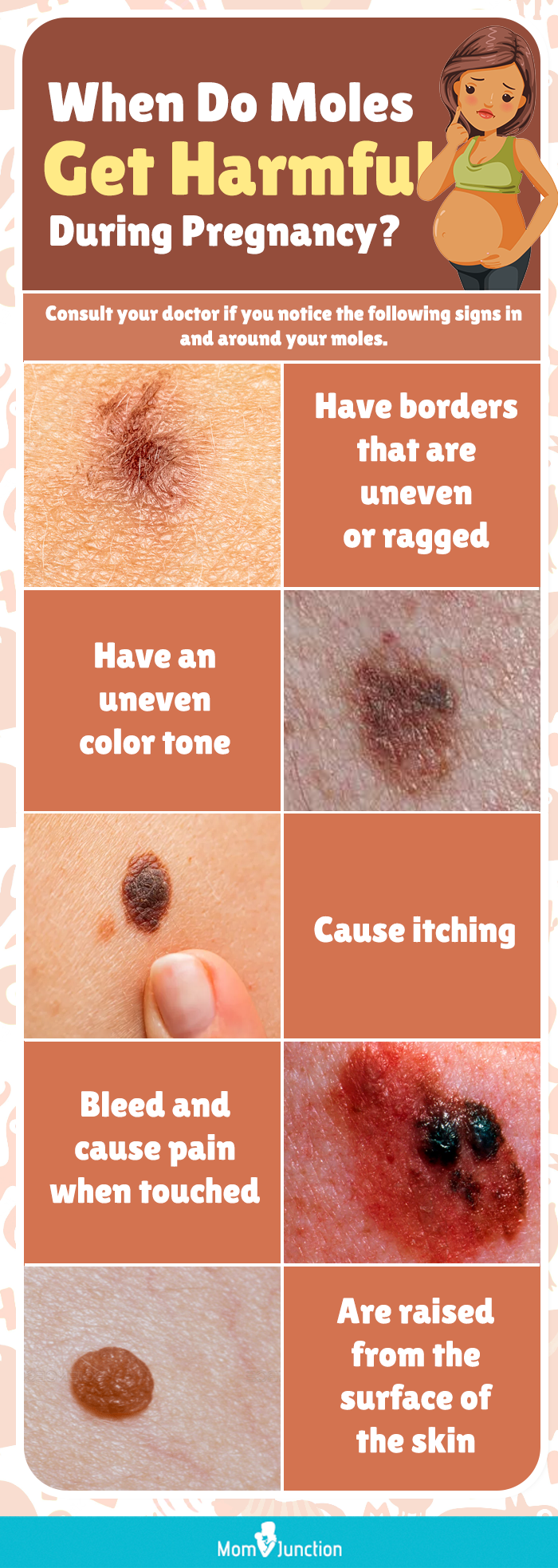
Personal Experience: Source
MomJunction articles include first-hand experiences to provide you with better insights through real-life narratives. Here are the sources of personal accounts referenced in this article.
i. My skin cancer; here’s my story;https://damagedskin.blogspot.com/2008/08/heres-my-story_9135.html
References
- Melanocytic Nevi (Moles).
https://www.yalemedicine.org/conditions/melanocytic-nevi-moles#:~:text=Melanocytic%20nevus%20is%20the%20medicaltypically%20do%20not%20require%20treatment. - Melanocytic naevi and melanoma in pregnancy.
https://dermnetnz.org/topics/melanocytic-naevi-and-melanoma-in-pregnancy#:~:text=Melanocytic%20naevi%20(moles)%20may%20changeto%20stretching%20of%20the%20skin. - Moles.
https://www.nhs.uk/conditions/moles/ - Moles (Congenital Melanocytic Nevi).
https://www.cincinnatichildrens.org/health/m/moles-congenital-melanocytic-nevi#:~:text=If%20they%20are%20seen%20atbrown%20spots%20on%20the%20skin. - Christopher A Natale et al.; Sex steroids regulate skin pigmentation through nonclassical membrane-bound receptors; eLife (2016)
https://elifesciences.org/articles/15104 - Pregnancy-related skin changes or skin cancer? How to tell the difference.
https://www.mdanderson.org/cancerwise/pregnancy-related-skin-changes-or-skin-cancer–how-to-tell-the-difference.h00-159616278.html - Jelissa K Peter et.al; (2026); AI-assisted Total Body Dermoscopic Evaluation of Changes in Melanocytic Nevi during Pregnancy: A Prospective Comparative Study of 2799 Nevi.
https://pmc.ncbi.nlm.nih.gov/articles/PMC11697141/ - Are moles determined by genetics?
https://medlineplus.gov/genetics/understanding/traits/moles/#:~:text=Moles%20are%20overgrowths%20of%20skindevelopment%20are%20not%20well%20understood. - Gilvan Ferreira Alves et.al; (2005); Dermatology and pregnancy.
https://www.scielo.br/j/abd/a/6tGxsbZmjFF6ckJ7JVHfnHy/?format=pdf&lang=en - Biochemistry Melanin.
https://www.ncbi.nlm.nih.gov/books/NBK459156/ - My Mole Itches But Doesn’t Hurt What Does This Mean?
https://www.skincenterofsouthmiami.com/2018/08/my-mole-itches-but-is-not-painful-what-does-this-mean/ - Are moles cancerous?
https://www.mdanderson.org/cancerwise/are-moles-cancerous.h00-159463212.html - Moles.
https://www.cancer.org.au/cancer-information/causes-and-prevention/moles - Ji Min Lee and Teo Jeon Shin; (2017); Use of local anesthetics for dental treatment during pregnancy; safety for parturient.
https://pmc.ncbi.nlm.nih.gov/articles/PMC5564152/ - Cancer Stat Facts: Melanoma of the Skin.
https://seer.cancer.gov/statfacts/html/melan.html - What is melanoma skin cancer?
https://www.nhs.uk/conditions/melanoma-skin-cancer/ - J Daniel Jensen and Boni E Elewski; (2015); The ABCDEF Rule: Combining the “ABCDE Rule” and the “Ugly Duckling Sign” in an Effort to Improve Patient Self-Screening Examinations.
https://pmc.ncbi.nlm.nih.gov/articles/PMC4345927/ - Melanoma during pregnancy: What it means for you and your baby.
https://www.aad.org/public/diseases/skin-cancer/types/common/melanoma/during-pregnancy - Skin Changes During Pregnancy.
https://americanpregnancy.org/healthy-pregnancy/pregnancy-health-wellness/skin-changes/ - Sun-damaged Skin (Photoaging).
https://my.clevelandclinic.org/health/diseases/5240-sun-damage-protecting-yourself - Pina Bozzo et.al; (2011); Safety of skin care products during pregnancy.
https://pmc.ncbi.nlm.nih.gov/articles/PMC3114665/ - Karen Konkel et.al; (2026); Serious Skin Injuries Following Exposure to Unapproved Mole and Skin Tag Removers.
https://pmc.ncbi.nlm.nih.gov/articles/PMC9891211/
Community Experiences
Join the conversation and become a part of our nurturing community! Share your stories, experiences, and insights to connect with fellow parents.
Read full bio of Dr. Irene (Eirini) Orfanoudaki
Read full bio of Rebecca Malachi
Read full bio of Swati Patwal
Read full bio of Aneesha Amonz