Image: ShutterStock
With new ideas and innovations taking over our world, we cannot overlook the rise in the number of alternative birthing methods that we are presented with. Of late, the Lotus birth (no, it has nothing to do with a certain political party) is one such postpartum practice that is being both critiqued and welcomed at the same time.
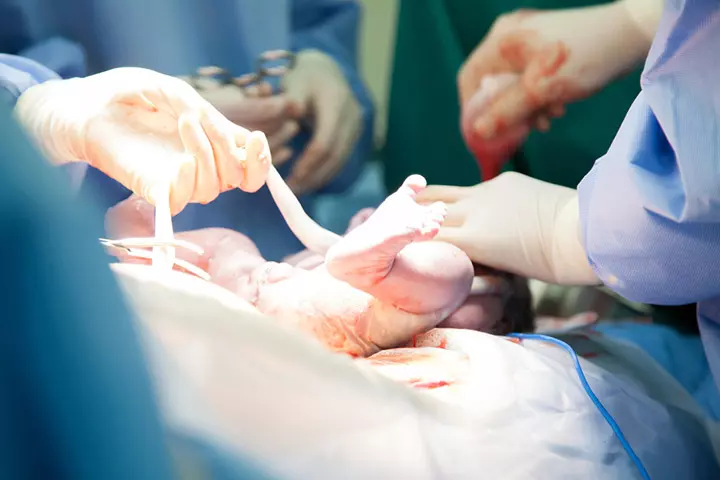
Vanessa Fisher, a new mom, raised eyebrows when she decided to opt for a Lotus birth—that demands the baby’s umbilical cord to fall off naturally, post birth. Unlike the usual norm of clamping the umbilical cord right after birth, Fisher took control of how she would welcome her baby and adopted this method of umbilical non-severance that lets nature take its own course. So, how does a lotus birth, that leaves the placenta connected to the baby for days, benefit the baby? That’s exactly what everyone was wondering. Let’s take you through the details.
What Is Lotus Birth And How Does It Work?
Image: Shutterstock
The moniker, Lotus Birth, comes from the parallels drawn between the significance of the placenta, and the reverence of the lotus in the Hindu and Buddhist cultures. Contrary to the clinical protocol, the cord is left unclamped from the baby’s naval and is instead allowed to dry and wither off on its own. The parents continue to carry the placenta, attached to the baby, in a bowl or a separate pouch even after the placenta has stopped pulsating.
According to a report by the World Health Organization (WHO) Reproductive Health library, substantial amounts of iron are deposited in the placenta and fetus during pregnancy, and this delayed detachment of the umbilical cord nourishes the baby with the transfer of the extra iron by adding the mineral to the newborn’s weight, thereby preventing iron deficiency during infancy (1).
Image: Nick and Vanessa Fisher
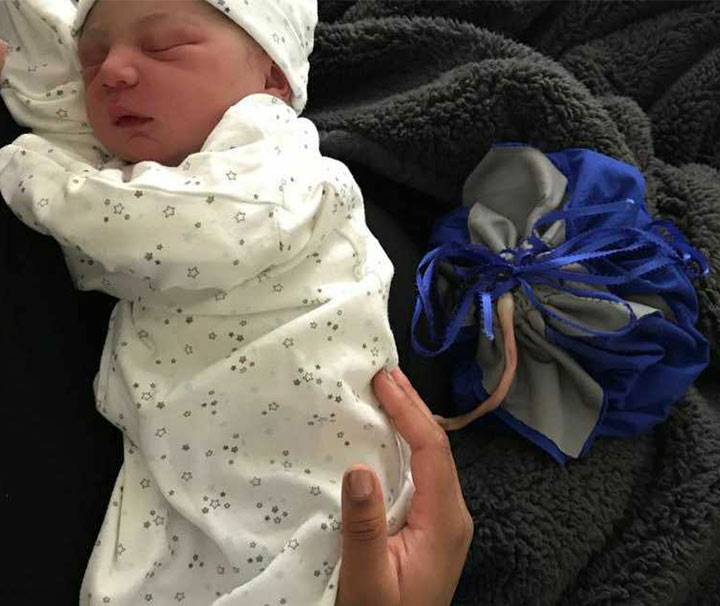
In addition to the multiple health benefits, this allows the newborn’s transition to being more natural and less traumatic, as Fisher explains. She believes that Lotus birth should be considered by new parents because of the health benefits a baby receives from a complete placental blood transfer. It creates a more fluid transition for a newborn baby, encourages bonding, and may result in a more peaceful and serene infant as they are spared the traumatic experience at birth.
Although Fisher faced some flak for her decision by her family members, her husband was supportive. “Most of the reluctance stems from the unconventionality of the procedure,” she says. However, the idea was mostly frowned upon based on the matters of practicality. The arguments included – the placenta is definitely unattractive; the placenta being attached would require that they be even more careful with the baby. Post the delivery, it took five days for the natural detachment of the placenta and the cord. However, on day nine, Fisher saw the complete snapping of the cord.
Image: Nick and Vanessa Fisher
“My son decided he wouldn’t even hold the baby until the placenta was done away with. I read articles that said it was unsanitary, even uncivilized. Online, I found that doctors speculated that infection could occur but I didn’t find any studies to verify that concern,” she said.
But, Is It Medically Recommended?
Image: Shutterstock
According to a study by the American College of Obstetricians and Gynecologists’ Committee, a delay of 30 to 60 seconds in unclamping the cord, post birth, leads to a high hemoglobin count and better iron reserves in the blood (2). But the medical experts remain skeptical about the benefits of a prolonged attachment of the cord and the placenta.
But, are we so accustomed to the limitations of western medicine that we refuse to acknowledge the possibilities of considering any alternatives? That’s something that only time will tell. But, if you are considering this birthing method, then the onus lies on you as parents to go that extra mile and weigh out the pros and cons before you take the big step.
Community Experiences
Join the conversation and become a part of our nurturing community! Share your stories, experiences, and insights to connect with fellow parents.